Trigeminal neuralgia is an uncommon disorder characterized by recurrent attacks of lancinating pain in the trigeminal nerve distribution. Typically, brief attacks are triggered by talking, chewing, teeth brushing, shaving, a light touch, or even a cool breeze. The pain is nearly always unilateral, and it may occur repeatedly throughout the day. The diagnosis is typically determined clinically, although imaging studies or referral for specialized testing may be necessary to rule out other diseases. Accurate and prompt diagnosis is important because the pain of trigeminal neuralgia can be severe. Carbamazepine is the drug of choice for the initial treatment of trigeminal neuralgia; however, baclofen, gabapentin, and other drugs may provide relief in refractory cases. Neurosurgical treatments may help patients in whom medical therapy is unsuccessful or poorly tolerated.
Trigeminal neuralgia was first described at the end of the first century and was later given the name “tic douloureux” because of the distinctive facial spasms that often accompany the attacks. The International Headache Society has published criteria for the diagnosis of classical and symptomatic trigeminal neuralgia (Table 1).1 In classical trigeminal neuralgia, no cause of the symptoms can be identified other than vascular compression. Symptomatic trigeminal neuralgia has the same clinical criteria, but another underlying cause is responsible for the symptoms. Trigeminal neuralgia may involve one or more branches of the trigeminal nerve (Figure 1), with the maxillary branch involved the most often and the ophthalmic branch the least.2,3 The right side of the face is affected more commonly than the left (ratio of 1.5:1), which may be because of the narrower foramen rotundum and foramen ovale on the right side.2–4
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence Rating | References |
|---|---|---|
| Physicians should obtain magnetic resonance imaging in all patients with suspected trigeminal neuralgia. | C | 3, 11–13 |
| Carbamazepine (Tegretol) should be the initial treatment for patients with classical trigeminal neuralgia because it has been found to be successful in most cases and no other medication has been shown to be superior in large studies. | A | 15, 16, 41 |
| Surgical options should be considered for patients who have persistent pain after trials with several medications or who have a relapse after initial success with medical treatment. | C | 12–14 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1205 or https://www.aafp.org/afpsort.xml.
The annual incidence of trigeminal neuralgia has been reported as 4.3 per 100,000 population, with a slight female predominance (age-adjusted ratio of 1.74:1).2 Primary care physicians might expect to encounter this condition two to four times over the course of a 35-year career. The peak incidence is at 60 to 70 years of age, and classical trigeminal neuralgia is unusual before age 40 years.2,3
The incidence of trigeminal neuralgia in patients with multiple sclerosis is between 1 and 2 percent, making it the most common associated disease.2 Patients with hypertension have a slightly higher incidence of trigeminal neuralgia than does the general population.2 There is no racial predilection.2 Trigeminal neuralgia is generally sporadic, although there have been reports of the disease occurring in several members of the same family. Spontaneous remission is possible, but most patients have episodic attacks over many years.
Table 1 IHS Diagnostic Criteria for Trigeminal Neuralgia
| Classical | |
| A. Paroxysmal attacks of pain lasting from a fraction of a second to two minutes, affecting one or more divisions of the trigeminal nerve, and fulfilling criteria B and C | |
| B. Pain has at least one of the following characteristics: | |
| 1. Intense, sharp, superficial, or stabbing | |
| 2. Precipitated from trigger zones or by trigger factors | |
| C. Attacks are stereotyped in the individual patient | |
| D. There is no clinically evident neurologic deficit | |
| E. Not attributed to another disorder | |
| Symptomatic | |
| A. Paroxysmal attacks of pain lasting from a fraction of a second to two minutes, with or without persistence of aching between paroxysms, affecting one or more divisions of the trigeminal nerve, and fulfilling criteria B and C | |
| B. Pain has at least one of the following characteristics: | |
| 1. Intense, sharp, superficial, or stabbing | |
| 2. Precipitated from trigger zones or by trigger factors | |
| C. Attacks are stereotyped in the individual patient | |
| D. A causative lesion, other than vascular compression, has been demonstrated by special investigations and/or posterior fossa exploration | |
IHS = International Headache Society.
Information from reference 1.
Figure 1.
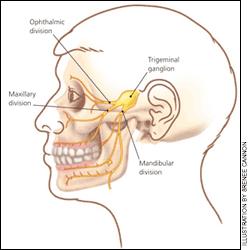
Trigeminal nerve.
Pathophysiology
It has been proposed that the symptoms of trigeminal neuralgia are caused by demyelination of the nerve leading to ephaptic transmission of impulses. Surgical specimens have demonstrated this demyelination and close apposition of demyelinated axons in the trigeminal root of patients with trigeminal neuralgia.5 Results from experimental studies suggest that demyelinated axons are prone to ectopic impulses, which may transfer from light touch to pain fibers in close proximity (ephaptic conduction).5
Current theories regarding the cause of this demyelination center on vascular compression of the nerve root by aberrant or tortuous vessels. Pathologic and radiologic studies have demonstrated proximity of the nerve root to such vessels, usually the superior cerebellar artery.5 Relief of symptoms by surgical techniques that separate the offending vessels from the nerve further strengthens this hypothesis. Demyelination has also been demonstrated in cases of trigeminal neuralgia associated with multiple sclerosis or tumors affecting the nerve root.
Multiple other causes of trigeminal neuralgia have been described, including amyloid infiltration, arteriovenous malformations, bony compression, and small infarcts in the pons and medulla. In most of these situations, demyelination may also be an underlying cause. Most investigators now accept the theory that classical trigeminal neuralgia results from vascular compression of the nerve root. This leads to demyelination of the nerve and the generation of ectopic impulses that are spread ephaptically to precipitate the typical attack.
Diagnosis
The diagnosis of trigeminal neuralgia should be considered in all patients with unilateral facial pain. Accurate and prompt diagnosis is important because the pain of trigeminal neuralgia can be severe. Other diagnoses must also be considered, particularly in patients with atypical features of the disease or “red flags” in the history or physical examination (Table 2). In addition, it is important to distinguish classical from symptomatic trigeminal neuralgia for the purpose of treatment. Symptomatic trigeminal neuralgia is always secondary to another disorder, and treatment should focus on the underlying condition.
Table 2 Atypical Features Suggesting Symptomatic Trigeminal Neuralgia or an Alternative Diagnosis
| Abnormal neurologic examination |
| Abnormal oral, dental, or ear examination |
| Age younger than 40 years |
| Bilateral symptoms |
| Dizziness or vertigo |
| Hearing loss or abnormality |
| Numbness |
| Pain episodes persisting longer than two minutes |
| Pain outside of trigeminal nerve distribution |
| Visual changes |
HISTORY
Because trigeminal neuralgia is a clinical diagnosis, the patient's history is critical in the evaluation. Patients with trigeminal neuralgia present with a primary description of recurrent episodes of unilateral facial pain. Attacks last only seconds and may recur infrequently or as often as hundreds of times each day; they rarely occur during sleep. The pain is generally severe, and is described as a stabbing, sharp, shock-like, or superficial pain in the distribution of one or more of the trigeminal nerve divisions. Patients generally are asymptomatic between episodes, although some patients with long-standing trigeminal neuralgia have a persistent dull ache in the same area.
Talking, smiling, chewing, teeth brushing, and shaving have all been implicated as triggers for the pain. Even a breeze touching the face may cause a paroxysm of pain in some patients. In trigger zones—small areas near the nose or mouth in patients with trigeminal neuralgia—minimal stimulation initiates a painful attack. Patients with trigeminal neuralgia can pinpoint these areas and will assiduously avoid any stimulation of them. Not all patients with trigeminal neuralgia have trigger zones, but trigger zones are nearly pathognomonic for this disorder.
The patient's history is also important for ruling out other causes of facial pain. Because of the association between trigeminal neuralgia and multiple sclerosis, patients should be asked about other neurologic symptoms, particularly those common in multiple sclerosis (e.g., ataxia, dizziness, focal weakness, unilateral vision changes). An evaluation for other diagnoses is indicated in younger patients, because classical trigeminal neuralgia is unusual in persons younger than 40 years.3
Trigeminal neuralgia pain is nearly always unilateral. In rare cases of bilateral trigeminal neuralgia, individual attacks are usually unilateral, with distinct episodes involving each side of the face at separate times. Symptoms are always confined to the trigeminal nerve distribution, with most cases involving the second or third division, or both. The asymptomatic period between attacks is important to distinguish classical trigeminal neuralgia from other causes of facial pain, as well as from symptomatic trigeminal neuralgia. Patients with trigeminal neuralgia have stereotyped attacks; a change in the location, severity, or quality of the pain should alert the physician to the possibility of an alternative diagnosis.
PHYSICAL EXAMINATION
The physical examination in patients with trigeminal neuralgia is generally normal. Therefore, physical examination in patients with facial pain is most useful for identifying abnormalities that point to other diagnoses. The physician should perform a careful examination of the head and neck, with an emphasis on the neurologic examination. The ears, mouth, teeth, and temporomandibular joint (TMJ) should be examined for problems that might cause facial pain.
The finding of typical trigger zones verifies the diagnosis of trigeminal neuralgia. Patients with classical trigeminal neuralgia have a normal neurologic examination. Sensory abnormalities in the trigeminal area, loss of corneal reflex, or evidence of any weakness in the facial muscles should prompt the physician to consider symptomatic trigeminal neuralgia or another cause of the patient's symptoms.
ANCILLARY TESTING
Laboratory studies generally are not helpful in patients with typical symptoms of trigeminal neuralgia. Occasionally, TMJ or dental radiographs may be useful when TMJ syndrome or dental pain is in the differential diagnosis.
Magnetic resonance imaging (MRI) of the brain is useful to look for multiple sclerosis, tumors, or other causes of symptomatic trigeminal neuralgia, and it should be performed in the initial evaluation of all patients presenting with trigeminal neuralgia symptoms. One study found that specific clinical variables may be helpful in determining the likely utility of MRI, which may be useful in prioritizing MRI studies when there is limited MRI capacity.6 Some studies have indicated that MRI may predict surgery outcomes based on findings of neurovascular contact or the volume of the affected trigeminal nerve.7–9
One recent study demonstrated that trigeminal reflex testing could distinguish classical from symptomatic trigeminal neuralgia with a sensitivity of 96 percent and a specificity of 93 percent.10 Trigeminal reflex testing involves electrical stimulation of the divisions of the trigeminal nerve and measurement of the response with standard electromyography apparatus. This testing is not readily available to most physicians, and its indications and clinical utility are still unclear.
DIFFERENTIAL DIAGNOSIS
Some disorders that might be included in the differential diagnosis of trigeminal neuralgia are listed in Table 3.11 A careful examination may disclose local findings indicative of otitis, sinusitis, dental disorders, or TMJ dysfunction. A history of persistent pain or pain that occurs episodically in attacks lasting longer than two minutes eliminates classical trigeminal neuralgia and should lead to a search for other diagnoses. The pain of glossopharyngeal neuralgia, which may be triggered by talking or swallowing, is located in the tongue and pharynx.
Table 3 Differential Diagnosis of Trigeminal Neuralgia
| Diagnosis | Features that differentiate from trigeminal neuralgia |
|---|---|
| Cluster headache | Longer-lasting pain; orbital or supraorbital; may cause patient to wake from sleep; autonomic symptoms |
| Dental pain (e.g., caries, cracked tooth, pulpitis) | Localized; related to biting or hot or cold foods; visible abnormalities on oral examination |
| Giant cell arteritis | Persistent pain; temporal; often bilateral; jaw claudication |
| Glossopharyngeal neuralgia | Pain in tongue, mouth, or throat; brought on by swallowing, talking, or chewing |
| Intracranial tumors | May have other neurologic symptoms or signs |
| Migraine | Longer-lasting pain; associated with photophobia and phonophobia; family history |
| Multiple sclerosis | Eye symptoms; other neurologic symptoms |
| Otitis media | Pain localized to ear; abnormalities on examination and tympanogram |
| Paroxysmal hemicrania | Pain in forehead or eye; autonomic symptoms; responds to treatment with indomethacin (Indocin) |
| Postherpetic neuralgia | Continuous pain; tingling; history of zoster; often first division |
| Sinusitis | Persistent pain; associated nasal symptoms |
| SUNCT | Ocular or periocular; autonomic symptoms |
| Temporomandibularjoint syndrome | Persistent pain; localized tenderness; jaw abnormalities |
| Trigeminal neuropathy | Persistent pain; associated sensory loss |
SUNCT = shorter lasting, unilateral neuralgiform, conjunctival injection, and tearing.
Information from reference 11.
Symptomatic trigeminal neuralgia is usually caused by multiple sclerosis or by tumors arising near the trigeminal nerve root. A history of previous neurologic symptoms and typical findings on MRI assist with the diagnosis of multiple sclerosis. Tumors involving the trigeminal nerve usually cause additional symptoms or examination findings that suggest the diagnosis, and these tumors are generally visible on MRI.
Figure 2. Diagnosis and Treatment of Trigeminal Neuralgia
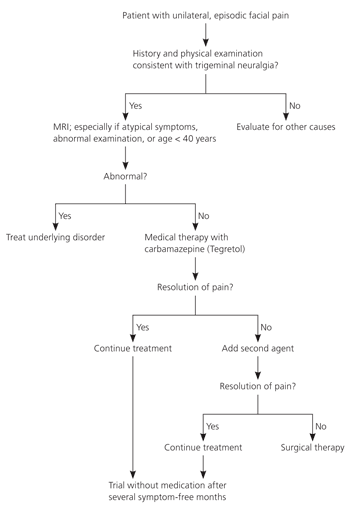
Algorithm for the diagnosis and treatment of trigeminal neuralgia. (MRI = magnetic resonance imaging.)
Information from reference 12.
Treatment
The initial treatment of choice for trigeminal neuralgia is medical therapy, and most patients have at least temporary relief with the use of selected agents. Patients who have no response to or who relapse with medical therapy should be considered for surgical treatment.12–14 Surgery may also be considered for patients who are intolerant of medical treatment.
MEDICAL TREATMENT
Carbamazepine (Tegretol) has been studied extensively in trigeminal neuralgia, with one meta-analysis finding good evidence for its effectiveness.15 A Cochrane review confirmed that carbamazepine is effective for the treatment of trigeminal neuralgia.16 The number needed to treat has been calculated at 2.5 for trigeminal neuralgia. The number needed to harm for minor adverse events is 3.7, which was calculated using data for all conditions.16
Some authors have suggested that carbamazepine is useful as a diagnostic trial for classical trigeminal neuralgia. Lack of response would suggest symptomatic trigeminal neuralgia or another diagnosis, both of which are less likely to respond to the drug. Dosages used have ranged from 100 to 2,400 mg per day, with most patients responding to 200 to 800 mg per day in two or three divided doses.
Carbamazepine should be the initial treatment for patients with classical trigeminal neuralgia. Other medications may be tried if carbamazepine is unsuccessful or provides only partial relief. These may be substituted or added to carbamazepine as necessary. Baclofen (Lioresal) in dosages of 10 to 80 mg daily has been shown to be useful.17 Additional medications with reported success in smaller studies or case reports include phenytoin (Dilantin), lamotrigine (Lamictal), gabapentin (Neurontin), topiramate (Topamax), clonazepam (Klonopin), pimozide (Orap), and valproic acid (Depakene).13,18–23 Most patients will respond, at least temporarily, to single or combination therapy with these agents.
A variety of other medications and modalities have been tried for treatment of trigeminal neuralgia. There are small studies reporting success with botulinum toxin type A (Botox) in some patients,24 and one case report of relief being experienced after an accidentally high discharge from a transcutaneous electrical nerve stimulation unit.25 Topical capsaicin (Zostrix) was helpful for trigeminal neuralgia pain in one open-label trial,26 and intramuscular sumatriptan (Imitrex) was beneficial in one small, single-dose study.27 One recent study found that intranasal lidocaine (Xylocaine) significantly decreased second-division trigeminal neuralgia pain for more than four hours.28 Acupuncture, high-dose dextromethorphan (Delsym), and topical ophthalmic anesthetic have been tried unsuccessfully in small trials.29–31 A recent Cochrane review concluded that there was insufficient evidence from randomized controlled trials to show significant benefit from non-antiepileptic drugs in patients with trigeminal neuralgia.32
SURGICAL TREATMENT
Surgical procedures may be percutaneous or open. The choice of procedure should be made after patient preference and the experience of the surgeon have been considered and the potential risks and benefits of each procedure have been evaluated. Most procedures provide effective short-term relief, but studies suggest that recurrence is likely within several years for many patients.33–40
Percutaneous techniques include glycerol injection, balloon compression, radiofrequency rhizotomy, and gamma knife stereotactic radiosurgery. These techniques offer the advantage of being relatively noninvasive, being outpatient procedures or requiring only a short hospital stay, and lacking life-threatening adverse effects. However, they may provide less long-lasting relief than the more invasive techniques and have a higher incidence of sensory loss, which may cause the patient significant discomfort and can be extremely difficult to treat.
Open techniques include partial trigeminal rhizotomy and microvascular decompression. These procedures involve posterior fossa exploration with its attendant risks, including stroke, meningitis, and death, although the reported incidence of these complications with microvascular decompression is less than 2 percent. Microvascular decompression appears to provide the longest lasting relief, with persistent relief at 10 years in more than 70 percent of patients.36,41,42 It has low risks of symptom recurrence and sensory loss, and is therefore a good choice for young, healthy patients, who have lower risks of adverse outcomes with the invasive surgery involved.

