The common dermatophyte genera Trichophyton, Microsporum, and Epidermophyton are major causes of superficial fungal infections in children. These infections (e.g., tinea corporis, pedis, cruris, and unguium) are typically acquired directly from contact with infected humans or animals or indirectly from exposure to contaminated soil or fomites. A diagnosis usually can be made with a focused history, physical examination, and potassium hydroxide microscopy. Occasionally, Wood's lamp examination, fungal culture, or histologic tissue examination is required. Most tinea infections can be managed with topical therapies; oral treatment is reserved for tinea capitis, severe tinea pedis, and tinea unguium. Topical therapy with fungicidal allylamines may have slightly higher cure rates and shorter treatment courses than with fungistatic azoles. Although oral griseofulvin has been the standard treatment for tinea capitis, newer oral antifungal agents such as terbinafine, itraconazole, and fluconazole are effective, safe, and have shorter treatment courses.
Tinea refers to dermatophyte infections, which are generally classified by anatomic location: tinea capitis is located on the scalp, tinea pedis on the feet, tinea corporis on the body, tinea cruris on the groin, and tinea unguium on the nails. Tinea is also called ringworm, especially when located on the body, and is caused by a group of fungi that infect only the outer keratinous layer of skin, hair, and nails. These fungi cannot survive on mucosal surfaces, such as the mouth or vaginal area. Superficial tinea infections are some of the most common dermatologic conditions in children.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Direct visualization of hyphae with potassium hydroxide microscopy is the mainstay for the office-based diagnosis of tinea. | C | 1, 2, 4, 5 |
| Griseofulvin (Grifulvin) and terbinafine (Lamisil; approved by the U.S. Food and Drug Administration for use in children two years and older) are effective therapies in the treatment of tinea capitis. | B | 8–12 |
| Topical fungicidal allylamines such as terbinafine and butenafine (Mentax) are usually sufficient to treat tinea corporis, tinea cruris, and tinea pedis and are superior to the older fungistatic azoles clotrimazole (Lotrimin AF) and miconazole (Micatin). | A | 17, 18 |
| Oral and topical treatment regimens for tinea unguium have low sustained clinical success rates. | B | 24–26 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1360 or https://www.aafp.org/afpsort.xml.
Dermatophytes are aerobic fungi that are divided into three genera (i.e., Trichophyton, Microsporum, and Epidermophyton). Tinea infection is acquired directly from contact with infected humans (anthropophilic organisms) or animals (zoophilic organisms) or indirectly from exposure to contaminated soil or fomites (geophilic organisms). The clinical manifestations of dermatophyte infections varies by the infection site and the patient's immunologic response; genetic susceptibility may play a role in vulnerability to infection.2
Table 1 presents the differential diagnosis of tinea infections,3 and Table 2 summarizes common therapies.
Table 1 Differential Diagnosis of Tinea Infections
| Infection | Common causative species | Differential diagnosis |
|---|---|---|
| Tinea capitis | Trichophyton tonsurans Microsporum audouinii* Zoophilic Microsporum canis* | Alopecia areata Impetigo Pediculosis Psoriasis Seborrheic dermatitis Traction alopecia Trichotillomania |
| Tinea corporis | Trichophyton rubrum Epidermophyton floccosum | Cutaneous lupus erythematous Drug eruption Eczema Erythema multiforme Granuloma annulare Nummular eczematous dermatitis Pityriasis rosea Psoriasis Secondary syphilis Tinea (pityriasis) versicolor* |
| Tinea cruris | T. rubrum E. floccosum Trichophyton mentagrophytes | Candidal intertrigo Contact dermatitis Erythrasma* Psoriasis Seborrhea |
| Tinea manuum | T. rubrum | Same as with tinea pedis |
| Tinea pedis | T. rubrum T. mentagrophytes E. floccosum | Bacterial or candidal infection Contact or atopic dermatitis Dyshidrosis Eczema Pitted keratolysis Psoriasis |
| Tinea unguium | T. rubrum T. mentagrophytes | Contact dermatitis Lichen planus Onychodystrophy Psoriasis |
*— Fluoresces under a Wood's lamp: M. audouinii and M. canis fluoresce blue-green; Malassezia furfur, the fungus that causes tinea (pityriasis) versicolor, fluoresces pale yellow to white, and Corynebacterium minutissimum, the bacterium that causes erythrasma, fluoresces bright coral red.
Adapted from Noble SL, Forbes RC, Stamm PL. Diagnosis and management of common tinea infections. Am Fam Physician. 1998;58(1):163–174.
Table 2 Antifungal Agents for the Treatment of Tinea Infections
| Agent | Dosage | Cost (generic)* | |
|---|---|---|---|
| Tinea unguium | |||
| Terbinafine (Lamisil) | 250 mg orally every day for 12 weeks† or | $1,171 ($1,047 to $1,080) | |
| 500 mg orally every day during the first week of each month for four months | $780 ($696 to $720) | ||
| Itraconazole (Sporanox) | 200 mg orally every day for 12 weeks or | $1,838 ($1,241 to $1,713) | |
| 400 mg orally every day during the first week of each month for four months‡ | $1,225 ($828 to $1,142) | ||
| Tinea capitis | |||
| Griseofulvin, micronized (Grifulvin) | 20 mg per kg per day for eight weeks | $467 ($467 to $578) for a child weighing 30 kg | |
| Terbinafine | 62.5 mg per day for four weeks§ | $105 (—) for a child older than two years weighing 20 kg | |
| Tinea corporis, pedis, cruris | |||
| Butenafine (Mentax) | Applied to the lesion and a 2-cm area surrounding the lesion once daily for approximately 14 days | 30 g: $84 (—) | |
| Terbinafine | Applied to the lesion and a 2-cm area surrounding the lesion twice daily for approximately 14 days | 15 g: — ($32 to $38) | |
| Miconazole (Micatin) | Applied to the lesion and a 2-cm area surrounding the lesion twice daily for approximately 14 days | 30 g, 2%: — ($3.20 to $3.30) | |
| Clotrimazole (Lotrimin AF) | Applied to the lesion and a 2-cm area surrounding the lesion twice daily for approximately 14 days | 24 g: $9.77 ($6.42 to $8.60) | |
*— Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, N.J.: Medical Economics Data; 2008. Cost to the patient will be higher, depending on prescription filling fee.
†— Higher cure rate among nail regimens.
‡— Lowest cost among nail regimens.
§— Lower cost among scalp regimens.
Diagnostic Tests
MICROSCOPY
Potassium hydroxide (KOH) microscopy is essential for the office-based diagnosis of tinea infections.1,2,4,5 This technique directly shows hyphae and confirms infection. The specimen is examined under the microscope after a drop of 10 to 20 percent KOH solution is added to the scraping from the active border of the lesion. KOH microscopy has good sensitivity and is more sensitive than a fungal culture. A positive test result justifies initiation of treatment. KOH microscopy has a 76.5 percent sensitivity and an 81.6 percent negative predictive value for the diagnosis of tinea unguium compared with a 53.2 percent sensitivity and 69.0 percent negative predictive value with culture.4
CULTURE
Culture techniques have a limited role in the evaluation and treatment of suspected tinea infection because of the expense and time requirement. However, when the need for long-term oral therapy is anticipated, the infection seems resistant to standard topical therapy, or the diagnosis is unclear, a culture is an appropriate approach for laboratory confirmation.
WOOD'S LAMP EXAMINATION
Wood's lamp examination for the diagnosis of tinea infection has decreased to near disuse because of the gradually declining number of dermatophytes that fluoresce under ultraviolet light.2,5 Exceptions include tinea capitis caused by zoophilic Microsporum canis and Microsporum audouinii, which fluoresce blue-green; tinea (pityriasis) versicolor caused by Malassezia furfur, which fluoresces pale yellow to white; and erythrasma caused by Corynebacterium minutissimum, which fluoresces bright coral red. Candida infection and tinea cruris do not fluoresce.
Tinea Capitis
DIAGNOSIS
Tinea capitis is the most common fungal infection in children. In the United States, more than 90 percent of tinea capitis cases are caused by Trichophyton tonsurans, and fewer than 5 percent are caused by Microsporum species. Both of these species go beyond superficial infection and invade hair shafts. Patients typically present with scaling of the scalp or circumscribed alopecia with broken hair at the scalp (Figure 1). The differential diagnosis of tinea capitis includes alopecia areata, trichotillomania, traction alopecia, and seborrheic dermatitis.
Figure 1.
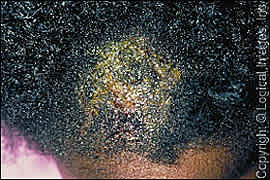
Tinea capitis. Note the hair loss and marked crusting.
Copyright © Logical Images, Inc.
A tinea capitis diagnosis is usually based on physical findings.6 One study showed that children presenting with adenopathy, alopecia, pruritus, and scaling invariably had positive culture results, whereas children who lacked adenopathy and scaling did not have positive culture results (Table 3).6
Table 3 Accuracy of Signs and Symptoms in the Diagnosis of Tinea Capitis
| Sign or symptom | Positive likelihood ratio | Sensitivity (%) | Specificity (%) |
|---|---|---|---|
| Adenopathy | 7.5 | 94 | 87 |
| Alopecia | 3.3 | 84 | 75 |
| Pruritus | 1.4 | 75 | 46 |
| Scaling | 1.1 | 71 | 35 |
Adapted with permission from Hubbard TW. The predictive value of symptoms in diagnosing childhood tinea capitis. Arch Pediatr Adolesc Med. 1999;153(11):1152.
Direct KOH microscopy of the skin scraping and hair shafts can confirm infection when positive, but false negatives are common even with experienced examiners. Wood's lamp examination can help identify Microsporum species, but Trichophyton species, which are increasingly common in the United States, do not fluoresce under a Wood's lamp. If necessary, fungal culture can be obtained (using a toothbrush or cotton swab) and then inoculated onto a fungal culture medium. The cotton-swab method is performed by moistening a sterile cotton swab and vigorously rubbing it over the affected areas of the scalp.7
TREATMENT
Tinea capitis must be treated with oral agents to penetrate the affected hair shafts. Although griseofulvin (Grifulvin) is often considered the treatment of choice for children, other agents are increasingly more cost-effective and may be more convenient.8 If griseofulvin is used, micronized oral griseofulvin is recommended at a dosage of 20 mg per kg per day for at least eight weeks. The long duration of treatment and the adverse effects of nausea, vomiting, and photosensitivity often negatively affect patient compliance.
Four weeks of terbinafine (Lamisil) therapy is as effective as eight weeks of griseofulvin therapy for the treatment of Trichophyton infections.9,10 Terbinafine is not as effective against Microsporum infections, which are much less common.11 A recent meta-analysis showed no significant difference in tolerability or adverse effects between griseofulvin and terbinafine.11
The recommended dosage of terbinafine is based on patient weight (62.5 mg per day in children weighing less than 20 kg [44 lb]; 125 mg per day in children weighing 20 to 40 kg [44 to 88 lb, 3 oz]; and 250 mg per day in children weighing more than 40 kg). Terbinafine is approved for use in children two years or older.12 The cost of a complete regimen of terbinafine is less than that of griseofulvin because of the shorter duration of therapy.13 The shorter regimen may also help increase patient compliance and decrease resistance secondary to early termination of therapy. Adverse effects from terbinafine are uncommon, although there are concerns about liver toxicity. Liver function testing (e.g., aspartate and alanine transaminase) is advised in all patients taking terbinafine at baseline and at follow-up in patients with baseline abnormalities or in those who experience gastrointestinal symptoms.14
Ketoconazole (Nizoral) and itraconazole (Sporanox) are not recommended for treating tinea capitis because of the limited data on their effectiveness and safety. Adjunctive selenium sulfide should be used to decrease the spread of tinea capitis.15 Selenium sulfide 2.5% shampoo is most effective and should be applied at least two to three times per week and should remain on the scalp for at least five minutes per application.16
Tinea Corporis
DIAGNOSIS
Tinea corporis is most commonly caused by Trichophyton species. Patients typically present with an annular patch or plaque with an advancing, raised, scaling border and central clearing (Figure 2). The differential diagnosis includes other annular skin lesions. Most patients with tinea corporis are diagnosed clinically. KOH microscopy of a skin scraping can determine if hyphae are present. Culture confirmation is usually not required.
Figure 2.
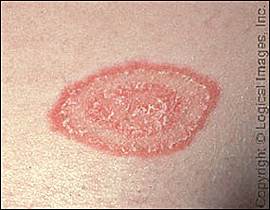
Tinea corporis. Note the well-demarcated margins, active border, and diffuse erythema.
Copyright © Logical Images, Inc.
TREATMENT
Topical treatment is often sufficient to cure tinea corporis, although oral medications can be used for patients with severe infection or for infections that do not respond to topical therapy. A topical antifungal agent is applied to the lesion and a 2-cm area surrounding the lesion once or twice daily; therapy is continued for one week after the lesion appears to resolve. Data show that newer butenafine (Mentax) and terbinafine therapies are more effective than older miconazole (Micatin) and clotrimazole therapies, primarily because of the fungicidal properties of the newer agents compared with the fungistatic action of the older agents.17,18 Combination antifungal/corticosteroid preparations are not recommended because of a greater risk of adverse effects, primarily from the higher-potency steroid component.19 Cure rates are lower and the cost is higher with combination therapy than with antifungal creams alone.
Tinea Corporis Gladiatorum
This special classification of tinea lesions is acquired in wrestlers through skin-to-skin contact. Annular lesions do not always occur; instead, they may appear as erythematous, scaling papules and plaques. They typically occur on the head, neck, and arms, and rarely occur on the legs.20 To prevent transmission, localized lesions should be covered with dressings, and patients with more extensive lesions should not wrestle. Patients can resume participation after one week of topical or systemic therapy.
Tinea Cruris (Jock Itch)
DIAGNOSIS
Tinea cruris is a superficial infection of the groin occurring predominantly in adolescent and young adult men. However, it has become more common in postpubertal females who are overweight or who often wear tight jeans or pantyhose. Because the common causes of tinea pedis (e.g., Trichophyton rubrum, Trichophyton mentagrophytes, Epidermophyton floccosum) are also common causes of tinea cruris, the two infections usually occur together.
Although the clinical presentation of tinea cruris varies, the lesion border is usually active to some degree with pustules or vesicles (unless the lesion is chronic). The background rash is red to reddish-brown and is usually a symmetric macule with fairly well-demarcated borders (Figure 3). The rash usually spares the scrotum and is often pruritic; acute rashes also may have a burning quality.
Figure 3.
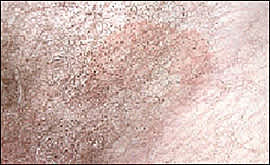
Tinea cruris. Note the well-demarcated margins, diffuse erythema, and light scaling.
TREATMENT
The feet should always be evaluated as a possible initial source of tinea cruris. Although the appearance and symptoms of tinea cruris are distinctive, the condition must be distinguished from other common disorders, including candidal intertrigo and erythrasma. Candidal intertrigo is more uniformly red with no central clearing and may have satellite lesions, whereas erythrasma is a bacterial infection that is more uniformly brown with slight scaling and no active border.
Topical therapy is usually a sufficient treatment for tinea cruris. Therapies include terbinafine cream or spray applied once daily for one week and butenafine 1% cream applied once daily for two weeks.
Tinea Pedis (Athlete's Foot)
DIAGNOSIS
Tinea pedis is caused by the same dermatophyte species as tinea cruris. It is more common in adolescents but rare in prepubertal children. The most important predisposing factor to acquiring tinea pedis appears to be exposure to a moist environment and maceration of the skin. The infection may be less prevalent in societies that do not commonly wear shoes.21
Tinea pedis typically appears as a white macerated area between the toes, although a more diffuse dry scaling process often caused by T. rubrum (“moccasin type”) may also occur. Another pattern of presentation is characterized by an inflammatory vesiculobullous eruption occurring primarily on the soles of the feet (Figure 4). Conditions that may mimic tinea pedis in children include contact and allergic dermatitis and occasionally atopic dermatitis. Unlike tinea pedis, dermatitis generally spares the intertriginous areas.
Figure 4.
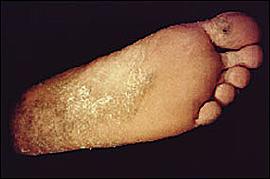
Tinea pedis. Note moderate scaling and deep vesicular changes.
Photo provided by the Centers for Disease Control and Prevention's Public Health Image Library.
TREATMENT
Topical antifungal agents such as terbinafine applied once daily for one week or butenafine 1% applied once daily for two weeks are effective for most forms of tinea pedis. The therapies can be applied directly to the web spaces and other affected areas. As with treatment of tinea cruris, these therapies are more effective than clotrimazole (Lotrimin AF) and miconazole. Occasionally, systemic terbinafine therapy, 250 mg taken orally every day for two weeks, or fluconazole (Diflucan), 150 mg taken once weekly for three weeks, can be used to treat severe or refractory infections.
Tinea Unguium
DIAGNOSIS
Tinea unguium is an infection of the finger- or toenails (Figure 5) and is a subset of onychomycosis, a broader category of infections that also include yeast and nondermatophyte molds. Tinea unguium is fairly uncommon in prepubertal children. Risk factors in adolescents include associated tinea pedis, improperly fitting shoes, and diabetes. Tinea unguium is a common cause of nail dystrophy; however, it should be differentiated from other acquired and congenital conditions. A nail scraping for KOH microscopy with or without a culture is recommended for confirmation. Although studies have shown that histologic analysis of nail clippings using a periodic acid-Schiff stain is the most accurate test, it is costly.22
Figure 5.
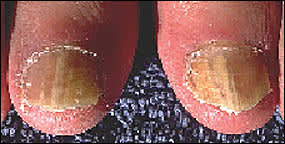
Tinea unguium of the toenails.
Photo provided by the Centers for Disease Control and Prevention's Public Health Image Library and Edwin P. Ewing, Jr., MD.
A recent study found that a KOH preparation (20 percent KOH, briefly heated) of a subungual debris scraping was 80 percent sensitive and 72 percent specific for the diagnosis of tinea unguium. This is compared with a culture, which was only 59 percent sensitive and 82 percent specific at four weeks.23
TREATMENT
The best evidence supports terbinafine for treating adolescents with tinea unguium,24 although griseofulvin is usually used in children. Terbinafine has similar effectiveness and adverse effect profile as itraconazole with a lower cost and a more favorable drug interaction profile. Data show that terbinafine is more effective than itraconazole or fluconazole.24 A recent study found that continuous terbinafine therapy is more effective than pulse (intermittent) terbinafine therapy.25 However, true “success” rates are not high for antifungal therapy, with only 35 to 50 percent of patients who are disease-free at one year.26

