Family physicians play a central role in the suspicion and diagnosis of immunoglobulin E-mediated food allergies, but they are also critical in redirecting the evaluation for symptoms that patients are falsely attributing to allergies. Although any food is a potential allergen, more than 90 percent of acute systemic reactions to food in children are from eggs, milk, soy, wheat, or peanuts, and in adults are from crustaceans, tree nuts, peanuts, or fish. The oral allergy syndrome is more common than anaphylactic reactions to food, but symptoms are transient and limited to the mouth and throat. Skin-prick and radioallergosorbent tests for particular foods have about an 85 percent sensitivity and 30 to 60 percent specificity. Intradermal testing has a higher false-positive rate and greater risk of adverse reactions; therefore, it should not be used for initial evaluations. The double-blind, placebo-controlled food challenge remains the most specific test for confirming diagnosis. Treatment is through recognition and avoidance of the responsible food. Patients with anaphylactic reactions need emergent epinephrine and instruction in self-administration in the event of inadvertent exposure. Antihistamines can be used for more minor reactions.
Food allergies affect 4 to 5 percent of children and 2 to 3 percent of adults, yet false attribution of symptoms to food allergy remains a problem.1,2 Population-based studies of children and adolescents have shown that only 10 percent of those who believe they have food allergy can be proven to have one.1 Disorders associated with food allergy, such as eosinophilic esophagitis, are being increasingly recognized, and some other previously known disorders, such as gastroesophageal reflux disease in infants, are being increasingly attributed to food allergies.3 Food allergy is the leading cause of nondrug-related anaphylaxis.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Immunoglobulin E testing with skin-prick or radioallergosorbent test is appropriate if clinical suspicion for food allergy is high. | C | 17 | Recommendation from guideline based on nonrandomized studies |
| Patients (or caregivers of patients) with known or suspected anaphylactic food allergies should carry injectable epinephrine and be instructed on how to use it. | C | 17 | Recommendation from guideline based on consensus of the Joint Task Force on Practice Parameters |
| Although there is no evidence to support the use of hydrolyzed formula over breastfeeding, there is some evidence that hydrolyzed formulas reduce infant and childhood allergies compared with cow's milk-based formulas. | B | 39,40 | Based on meta-analyses of randomized and nonrandomized studies; however, there was significant inconsistency of results across the trials |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see https://www.aafp.org/afpsort.xml.
Pathophysiology
Despite high acidity in the stomach and enzyme activity, 2 percent of ingested food is absorbed through the intestine in a form that is immunologically intact enough to produce a food allergy.4 However, most patients have oral tolerance (an active nonresponse to antigens delivered orally) and do not ever develop a reaction. Oral tolerance may occur because of the way intestinal epithelial cells present the antigen to mucosal lymphatic cells. Low doses of intestinal food antigens preferentially increase regulatory T cell production within the intestinal lymphoid tissue. These regulatory T cells secrete suppressive cytokines that decrease inflammatory reactions. Infants and young children have a more immature mucosal gut barrier and immune response; therefore, a larger percentage of ingested food is absorbed intact. This is believed to account for the increased prevalence of food allergies in this population.4
Foods Most Likely to Produce Food Allergies
Although any food is a potential allergen, the foods in Table 1 account for more than 90 percent of all systemic food allergies.2,5 Fruits and vegetables can also produce allergies, but they tend to be milder reactions. Seeds (e.g., sesame, sunflower) have been known to cause severe reactions.6,7 Although much less common, allergy to other foods is possible, with manifestations in almost any organ system. Allergy to food additives is also possible, but rare. Food additive allergy should be suspected when the patient reports allergic symptoms after ingestion of a variety of foods with no shared proteins, and when no reaction occurs with a homemade version of the same foods.8 Genetic manipulation of food can also potentially produce proteins that will cross-react with the immunoglobulin E (IgE) of a patient with a food allergy.9
Table 1 Most Common Food Allergies in Children and Adults
Most patients are allergic to between one and three foods. This does not include the cross-reactions to similar proteins that can be common in some food groups. For example, almost all patients who are allergic to cow's milk will also be allergic to sheep's or goat's milk. Most patients who are allergic to shrimp will also react to other crustaceans. Some patients with a latex allergy will react to banana, kiwi, or avocado.
Characteristics of Patients with Food Allergies
Most patients with food allergies have an atopic disorder; however, only 10 percent of patients with atopic disorders have food allergies.10 A family history of food allergy or other atopic disorders increases the risk of developing a food allergy. Genetic predisposition, including specific haplotypes, has been identified for some common food allergies. The oral allergy syndrome is confined to patients who have allergic rhinitis or asthma. Table 2 lists historical factors that increase the risk of food allergies.11
Table 2 Historical Factors that Increase the Risk of Food Allergy
| History of reaction within minutes to hours of ingestion |
| Inadvertent ingestions of the same food have produced similar reactions on repeated exposure |
| Lack of other possible explanations for the reaction besides food allergy |
| Suspected food is known to be a higher risk for food allergies |
| Symptom onset in infant or young child |
| Personal or family history of atopic dermatitis, asthma, allergic rhinitis, or food allergies |
note: Although these features would increase the likelihood of a food allergy, the absence of these features does not preclude the possibility of a food allergy.
Information from reference 11.
Natural History of Patients with Food Allergies
The majority of children will outgrow the most common food allergies; those who do not will have persistent allergies to the same or different foods. Approximately 70 percent of children with egg allergy and 85 percent with milk allergy will outgrow it by five years of age.12,13 However, about 40 to 60 percent of these children will develop asthma and 30 to 55 percent will develop allergic rhinitis.12,13 Risk of persistent allergy to peanut is much greater, with only 20 percent of children ever developing tolerance.14 Adolescents with persistent allergies and adults with new onset are particularly prone to fatal food allergies. Increased risk in adolescents may be explained by their tendency to eat foods that could contain allergens and to not carry epinephrine with them (depending on their social situation).15 Adults with food allergies usually remain allergic.
Differential Diagnosis for Symptoms Suggestive of Food Allergies
Suspicion of food allergy begins with reports of symptoms that appear to be temporally related to food ingestion. Persons with IgE-mediated food allergy develop symptoms within minutes to several hours after exposure; reactions rarely occur later. Even reported reactions within this time are not specific for food allergies. Symptoms from the clinical spectrum reported below, particularly if experienced repeatedly by the patient in response to a food that commonly produces allergies, are more likely to truly represent an allergy. Food-associated symptoms that are not IgE mediated can be further divided into illnesses that are immune mediated, but not completely IgE based (e.g., the principally cell-mediated responses in celiac disease), or the many nonimmune adverse reactions to food.
The nonimmune-mediated reactions include infectious causes, enzymatic food reactions (lactose intolerance), and pharmacologic food reactions (vasoactive amines in scombroid poisoning). Also, symptoms can increase with eating (irrespective of the food ingested) in irritable bowel disease, carcinoid syndrome, and gustatory rhinitis. Distinguishing features of some of these disorders are presented in Table 3.16,17
Table 3 Food and Eating-Related Disorders that May Mimic Food Allergies
| Disorder | Populations affected/presumed etiology/food sources | Symptoms | Diagnosis/treatment |
|---|---|---|---|
| Carcinoid syndrome | Carcinoid tumors occur throughout adulthood and can develop in late childhood |
|
|
| Celiac disease | More common in white persons |
|
|
| Symptoms can start at any age | |||
| Sometimes associated with dermatitis herpetiformis | |||
| Symptoms develop after gluten ingestion (wheat, barley, rye, and, more rarely, oats) | |||
| Giardiasis | Persons who have ingested water or food contaminated with Giardia cysts |
|
|
| Fecal-oral spread also occurs in child daycare settings | |||
| Gustatory rhinitis | Believed to be nonallergic and mediated through vagus nerve |
|
|
| Irritable bowel disease | Chronic symptoms usually start in young adulthood (before 40 years of age) |
|
|
| Lactase deficiency* | Primary deficiency much more likely to develop in adulthood in nonwhite persons, but lesser degrees of lactase deficiency can be found in 25 percent of white persons |
|
|
| Scombroid poisoning | Bacterial production of excess amines, particularly histamine on food |
|
|
| Most cases from tuna, mahi-mahi, and swiss cheese | |||
| Sulfite ingestion† | Sulfites have been banned by the U.S. Food and Drug Administration for preserving raw fruits and vegetables, but they are still found in a variety of cooked and processed foods |
|
|
*— Secondary lactase deficiency can occur with small intestinal mucosa brush border abnormalities, such as gastroenteritis and celiac sprue.
† — Can be ingested or inhaled.
Food diaries can be useful when the patient has symptoms that could potentially be secondary to food allergy, but there is no recognized provoking food. The patient records all foods eaten that day in a diary. The diary is typically continued for weeks.
Family physicians can help determine how likely a patient's symptoms are to be a result of a food allergy and if further testing is indicated. They can redirect the evaluation if symptoms are being falsely attributed to allergies. They can also provide information on food avoidance techniques and can primarily direct the avoidance strategies when the reported reaction is minor (e.g., oral allergy syndrome). Family physicians are often contacted first to assess and treat anaphylactic reactions from food. Allergist referral should be considered when the patient has a history of anaphylactic reactions to food, when there is need for skin-prick or food challenge testing, and when symptoms have not improved with primary care interventions.
Clinical Spectrum of IgE-Mediated Food Allergies
ANAPHYLAXIS
Anaphylaxis symptoms occur in multiple organ systems and can include throat swelling, wheezing, rhinorrhea, urticaria, hypotension, and abdominal cramping (Table 4).18 Risk factors for death from anaphylaxis are adolescent or young adult patient; underlying asthma; allergies to crustaceans, tree nuts, peanuts, or fish; and a delay in or lack of administration of epinephrine.
Table 4 Symptoms of Anaphylaxis
| Abdominal pain, cramping, diarrhea, vomiting |
| Angioedema, flushing, generalized urticaria, pruritus |
| Chest tightness |
| Cough, dyspnea, wheezing |
| Feeling of impending doom |
| Hypotension, shock |
| Metallic taste in mouth |
| Rhinorrhea |
| Throat swelling |
| Uterine contractions |
Information from reference 18.
FOOD-DEPENDENT EXERCISE-INDUCED ANAPHYLAXIS
Food-dependent exercise-induced anaphylaxis is a rare disorder in which patients develop anaphylaxis only if they ingest foods to which they are allergic and then exercise. They are completely asymptomatic if these two elements are not combined. Patients must avoid the provoking foods for as many as six hours before exercise. Wheat is the most common food associated with food-dependent exercise-induced anaphylaxis.19,20
ACUTE URTICARIA
Food allergies account for 30 percent of acute urticaria cases.21 Patients become symptomatic minutes to hours after ingestion of the provoking food. Because acute urticaria can be one manifestation of anaphylaxis, care to identify symptoms in other organ systems that would raise the diagnosis to this more urgent level is warranted. Chronic urticaria is much less commonly caused by food allergies (3 to 4 percent of cases).22
ATOPIC DERMATITIS
About 35 percent of children with atopic dermatitis have a food allergy, based on double-blind, placebo-controlled food challenges.23 Skin manifestations improve when the suspected foods are removed from the diet; eggs, milk, and peanuts are most commonly implicated. In breast-fed infants, elimination of suspected foods in the mother's diet has produced clinical improvement.
ORAL ALLERGY SYNDROME
The oral allergy syndrome is the most common food allergy; it is clinically recognized in up to 10 percent of patients who have allergic rhinitis or asthma from grass, weed, or tree pollen.24 However, it is believed to have a significantly higher prevalence in patients with birch pollen allergy.25
The manifestations of the oral allergy syndrome are brief in duration, are limited to the mouth and throat, and are sometimes so mild that the patient may not seek evaluation. Proteins similar to the aeroantigens to which the patient is sensitive are present in apples, carrots, and cherries (birch pollen); kiwi and tomato (grass pollen); and melons (ragweed pollen). When these foods come into contact with the oropharynx, a local reaction occurs. Table 5 lists common food and aeroantigen cross-reactions.18 Patients may notice lip and tongue swelling and pruritus that can also involve the throat and palate. Progression to systemic manifestations is rare. Denaturing the proteins by cooking, or removing the food from the oropharynx by swallowing or spitting out stops the reaction.
Table 5 Potential Cross-Reactions Between Airborne Allergens and Foods
| Airborne allergen | Food |
|---|---|
| Birch pollen | Carrots |
| Celery | |
| Fresh fruit (e.g., apples, cherries, nectarines, peaches, pears) | |
| Hazelnuts | |
| Parsnips | |
| Potatoes | |
| Grass pollen | Kiwi |
| Tomatoes | |
| Ragweed pollen | Bananas |
| Melons (e.g., cantaloupe, honeydew, watermelon) |
Information from reference 18.
ALLERGIC EOSINOPHILIC GA STROINTESTINAL DISORDERS
Allergic eosinophilic gastrointestinal disorders are particularly prevalent in children and are thought to be caused by an IgE- and cell-mediated response to specific foods. Patients with these disorders have excess eosinophils in the mucosal and serosal layers of the portion of the gastrointestinal tract that produces their symptoms.26 Only about 50 percent of children with eosinophilic gastrointestinal disorders are positive for specific food allergies on IgE testing,18 but almost all children improve when switched from milk or soy to an extensively hydrolyzed formula (processed so that peptides are less than 3,000 Da) or to an elemental diet (no proteins; only amino acids) (Table 626,27 ).
Table 6 Subclassification of Eosinophilic Gastrointestinal Disorders
| Disorder | Population | Signs and symptoms |
|---|---|---|
| Allergic eosinophilic esophagitis | Most commonly diagnosed in neonates and infants, but can affect older children and adults | Emesis, dysphagia, or epigastric pain that continues despite antireflux therapy |
| Normal esophageal pH | ||
| Allergic eosinophilic gastritis | Children and adolescents | Failure to thrive, diarrhea, emesis, epigastric pain, occult blood in stool, gastric outlet obstruction |
| Allergic proctocolitis | Usually in young infants; more than 50 percent are exclusively breastfed | Can occasionally produce blood-streaked stools |
| Sometimes occurs in older children |
Diagnostic Testing
All IgE testing for food allergies must be interpreted in the context of the patient's clinical reactions. Many patients will have positive IgE tests to foods despite never having a clinical reaction. Also, IgE will remain positive if they once had food allergies, but have since developed tolerance. The most commonly used method to assess for food-specific IgE is skin-prick testing. In skin-prick testing, a portion of a commercial extract of the food in question is pushed into the epidermis with a needle or probe, and the area is observed for a wheal and flare reaction after 15 to 20 minutes. Some allergists believe that fresh extracts of fruits and vegetables have superior sensitivity and specificity and use them in skin-prick tests. Although generalized reactions rarely occur (about 0.05 percent overall rate), there have been no reported deaths after skin-prick testing.28
Recent reports have suggested similar sensitivity and specificity for the radioallergosorbent test (RAST) compared with skin-prick testing; however, many allergists believe that RAST sensitivity is lower, particularly in older children and adults. RAST involves the detection of preformed antibodies in the patient's serum and thus carries no potential for allergic reactions. In this article, RAST refers to any in vitro, food-specific IgE antibody test. IgE testing with skin-prick test or RAST is appropriate if clinical suspicion of food allergy is high.17 Figure 1 outlines the evaluation for suspected food allergy.18
Figure 1. Evaluation of Suspected Food Allergy
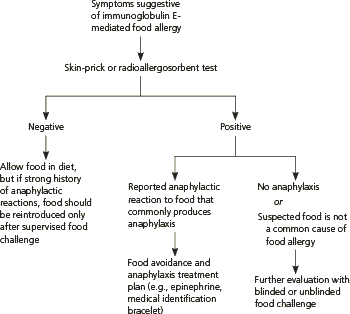
Algorithm for the evaluation of suspected food allergy.
Information from reference 18.
Intradermal testing has poorer specificity for food allergy and greater risk of adverse reaction than a skin-prick test or RAST and therefore, is not appropriate for initial evaluations.17 Some allergists still argue for its use in subsequent evaluations when clinical suspicion is high and skin-prick test or RAST are negative. Patch testing has shown promise, particularly in children with atopic dermatitis and in the evaluation of delayed reactions, but it requires highly experienced evaluators to properly assess the reactions. Table 729–34 presents methods for IgE testing and Table 817,30 lists types of food challenges and their uses. Patients describing anaphylactic reactions to a food that is commonly associated with anaphylaxis do not require food challenge if their IgE testing is confirmatory. Food challenges are appropriate when a food is clinically suspected of inducing a food allergy, but IgE testing is negative.
Table 7 Immunoglobulin E Determinations for Suspected Food Allergy
| Procedures | Observed response | Comments |
|---|---|---|
| Skin-prick test | ||
| Portion of commercial extract is pushed into area of epidermis with needle or probe; adjacent area has normal saline as control | Observe for wheal and flare reaction developing after 15 to 20 minutes | 85 percent sensitivity and 30 to 60 percent specificity for food allergies based on double-blind, placebo-controlled food challenges29 |
| Patients must avoid antihistamines for 48 hours before testing because they can blunt reaction | ||
| RAST | ||
| Although a serum sample can be assessed for a predetermined food allergy panel, individual food testing based on history is preferred | Levels of immunoglobulin E against predetermined food antigens are measured | Like skin-prick testing, RAST has high sensitivity, but only about 50 percent specificity30,31; however, it has a 95 percent specificity in children with atopic dermatitis who are allergic to eggs, milk, peanuts, or fish32 |
| Preferentially done initially in young children and infants, in adults with significant comorbid conditions, and in patients with such extensive skin involvement that skin-prick testing is prohibited or who cannot discontinue antihistamines for 48 hours before skin-prick testing | ||
| Patch testing | ||
| Commercially prepared food extracts applied to skin and occluded with patch | Remove patch and observe for erythema and induration at site at 48 hours | Studied the most in children with atopic dermatitis where positive patch tests have shown to correlate with food challenge-confirmed milk allergies better than skin-prick testing33 |
| Overall clinical usefulness unclear | Symptomatic reactions can occur earlier, warranting patch removal after physician notification | Positive predictive value of RAST or skin-prick test combined with patch test is so high that food challenges are often unnecessary34 |
RAST = radioallergosorbent test.
Table 8 Food Challenge Testing and Elimination Diet for Suspected Allergies
| Procedures | Uses | Comments |
|---|---|---|
| Double-blind, placebo-controlled food challenge | Older children and adults with atypical reactions or reported reactions to uncommonly involved foods |
|
| Single-blind food challenge | Older children and adults with atypical reactions or reported reactions to uncommonly involved foods, but where there is higher pretest suspicion of true food allergy |
|
| Open food challenge | Can be used to test multiple foods with follow-up blinded food challenges for positive reactions |
|
| Elimination diet | Can be used at any age |
|
| Multiple foods can be eliminated if there is clinical suspicion for more than one food | ||
| Usually followed by food challenge if patients improve on elimination |
note: Procedures are in order of most to least specific.
Management
AVOIDING OFFENDING FOODS
Patients with food allergies, and parents of children with food allergies must habitually read labels of any new food to verify the absence of known allergens. When others are cooking, such as at a restaurant or another person's home, ingredients and cooking methods must be known. Desserts, sauces, and fried foods tend to be higher risk. Cooking with butter or a milk-containing margarine could trigger a reaction in persons with a milk allergy.
ANAPHYLACTIC FOOD ALLERGY
Epinephrine should be urgently administered if anaphylaxis is suspected. Intramuscular diphenhydramine (Benadryl), systemic corticosteroids, and histamine H2 blockers can be added if the patient's symptoms have not completely resolved with epinephrine alone. See Table 918,35 for doses and follow-up. Supplemental oxygen should be administered if the patient has broncho-spasm or laryngeal edema.35
Table 9 Treatment and Follow-Up for Food Allergy Anaphylaxis
| Medication | Adult dose | Children's dose | Follow-up/comments | ||
|---|---|---|---|---|---|
| Epinephrine* | 0.3 to 0.5 mg IM of a 1:1,000 solution of aqueous epinephrine | 0.01 mg per kg IM up to a maximal dose of 0.3 to 0.5 mg | About 20 percent of patients will have recurrence within several hours; therefore, a four-hour monitoring period is recommended | ||
| Diphenhydramine (Benadryl) | 50 mg IM or orally | 1 mg per kg IM or orally up to a maximal dose of 50 mg | Dose can be repeated every four to six hours | ||
| 12.5 mg per 5 mL liquid preparation available for children | |||||
| Ranitidine (Zantac) | 50 mg IM or IV or 150 mg orally twice daily | 2 to 4 mg per kg IV every eight hours up to maximal dose of 50 mg or 2 to 4 mg per kg orally daily (divided into two doses) up to maximal dose of 300 mg per day | Dose can be repeated every 12 hours | ||
| Systemic corticosteroids† | Dexamethasone 6 to 10 mg IV, IM, or orally | Methylprednisolone (Solu-Medrol) 1 to 2 mg per kg IV | Usually not repeated | ||
IM = intramuscularly; IV = intravenously.
*— There is increased risk of myocardial infarction and stroke in patients with risk factors. Effectiveness is diminished in patients on beta blockers.
† — Although not effective for acute treatment, they can reduce recurrence of some symptoms.
Patients who have had even a single anaphylactic reaction to food should have two age-appropriate epinephrine pens with initial instruction in technique and follow-up visits for technique assessment.17 The second pen is recommended because the first dose can wear off after 20 minutes, possibly before the patient has reached a medical facility. These patients should also wear a medical identification bracelet that provides information about their allergy. Informing other caretakers and companions of young adults and children about the condition and appropriate use of epinephrine is recommended. Most patients who develop a second phase of anaphylaxis should be admitted to the hospital for observation.35
Oral or parenteral antihistamines can be administered for more minor reactions, such as isolated pruritus or urticaria. Children can take liquid diphenhydramine.35
PREVENTION OF FOOD ALLERGIES
The American College of Allergy, Asthma and Immunology recommends exclusive breastfeeding for the first six months in infants with a family history of two primary relatives with an atopic disease, and continued breast-feeding through at least the first year, with solid food not being introduced until after six months of age.36 Because approximately one half of all women are secretors (what they ingest will appear in their breast milk), the breast-feeding mother should avoid eggs, milk, tree nuts, peanuts, and seafood. In the child's diet, nuts, shellfish, and fish are delayed until three to four years of age. Although there is some evidence of a decrease in food allergies and atopic dermatitis for the first two years of life with this approach, some recent studies have shown no persistent decrease in atopic parameters past the first few years.37,38 Using a soy formula instead of a cow's milk-based formula does not appear to reduce allergies.39 However, there is some evidence that infants on hydrolyzed formulas have fewer allergies, including food allergies, compared with regular cow's milk formulas.40 There is no evidence to support that extensively hydrolyzed formulas reduce allergy development in infants relative to breastfeeding,40 but hydrolyzed formula feeding is an option for high-risk infants whose mothers cannot comply with avoiding likely allergen-containing foods during breastfeeding.
Immunotherapy has not been proven to be effective in the prevention of food allergies.41
PREVENTION OF INADVERTENT EXPOSURES FOR SENSITIZED PATIENTS
Food labels must state if the food contains any of the most common ingredients known to produce systemic reactions. The Food Allergy and Anaphylaxis network (http://www.foodallergy.org) has information for patients and families on home food preparation, restaurant dining, responses to allergic reactions, and adjustments for specific social situations.42
NOVEL TREATMENTS AND POTENTIAL NEW DIRECTIONS
The commercial food abstracts used in IgE testing contain other nonallergic components, resulting in a test that is difficult to standardize. Use of recombinant antigens that are selected based on their association with food allergy instead of commercial food extracts may allow for improved specificity.43,44
Specific oral tolerance induction, which is when patients ingest daily small quantities of the offending food and then increase the amount until reaching what would be in the diet, has shown some promise, but only in small nonplacebo-controlled trials.45
Injection of monoclonal IgG that binds to IgE and masks regions responsible for receptor binding to mast cells and basophiles partially protects patients with peanut allergies and shows promise for use in other food allergies.46
A specific Chinese herbal tea formula has been shown to be highly effective in preventing peanut allergies in animals. Trials in humans will be conducted soon.47

