A three-year-old boy presented with a diffuse, progressive rash on his arms and legs (Figure 1) that had persisted for five days. The eruption first appeared on his right forearm, then spread to his thighs and cheeks (Figure 2). The rash was mildly pruritic and associated with a low-grade fever. The patient had received all age-appropriate immunizations.
Examination revealed an otherwise healthy, active child. Multiple erythematous papules, 2 to 3 mm in diameter, coalescing into plaques with secondary excoriations were noted on his forearms, thighs, and cheeks. Other than two erythematous papules on the upper back, the patient's chest and back were spared.
Figure 1.
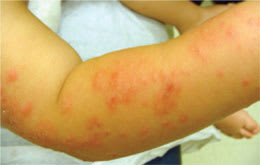
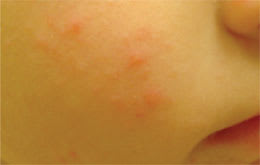
Figure 2.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Erythema multiforme.
B. Gianotti-Crosti syndrome.
C. Lichen planus.
D. Papular urticaria.
E. Scabies.
Discussion
The correct answer is B: Gianotti-Crosti syndrome. Gianotti-Crosti syndrome (papular acrodermatitis of childhood) is a relatively common dermatosis that occurs worldwide. The condition affects children three months to 15 years of age, but typically occurs before four years of age. However, it has been reported in adults.1
Gianotti-Crosti syndrome is characterized by the acute onset of monomorphous, pink to red-brown papules or papulovesicles that may become confluent. The papules are distributed symmetrically on the face, extensor surfaces of the extremities, and buttocks. The rash may be slightly pruritic; is typically nonhyperkeratotic; and spares the trunk, palms of the hands, and soles of the feet.1 It may persist for many weeks. The cutaneous manifestations can be preceded by diarrhea or an upper respiratory tract infection. The rash may be accompanied by a low-grade fever, hepatomegaly, splenomegaly, or inguinal or axillary lymphadenopathy.
Although the exact pathogenesis is unclear, Gianotti-Crosti syndrome is considered a self-limited, cutaneous response to various immunologic triggers. Although the syndrome was first described in association with hepatitis B virus, Epstein-Barr virus is now the most common associated virus in the United States.1 Hepatitis A virus, cytomegalovirus, coxsackievirus, respiratory syncytial virus, parainfluenza virus, rotavirus, mumps, parvovirus, molluscum contagiosum,1 and childhood immunizations have also been associated with the syndrome.2 Recent reports indicate that bacterial infections such as Bartonella henselae, Mycoplasma pneumoniae, and group A streptococci may trigger Gianotti-Crosti syndrome.2 Although the specific reason that children develop Gianotti-Crosti syndrome is unknown, an association with atopy has been suggested.3
Gianotti-Crosti syndrome is diagnosed clinically by the presence of a characteristic rash, although other conditions can be considered in patients with equivocal or atypical cases.1 Because the condition is self-limited, treatment usually is not required. However, topical steroids and oral antihistamines can be prescribed as needed for pruritus. Patients' parents should be reassured that the rash usually resolves without scarring within 10 to 60 days.1
Erythema multiforme causes target-shaped papular and vesiculobullous lesions on the extremities or mucous membranes. The lesions are often distributed symmetrically and may be preceded by fever or upper respiratory tract symptoms. The palms of the hands and soles of the feet are often involved; initial involvement most commonly occurs on the dorsal hands.4 The condition typically affects adolescents and young adults and is usually triggered by recurrent herpes simplex virus infections. More serious forms that include mucosal involvement have been associated with various infections and medications.
Lichen planus is an acute or chronic inf lammatory dermatosis of unknown origin involving skin or mucous membranes. Although the etiology is unknown, there is an association with hepatitis C virus.5 The condition is uncommon in children and is characterized by intensely pruritic, f lat-topped, pink to violaceous, shiny, polygonal papules; fine, linear overlying white scales (Wickham's striae) may develop.5 It usually occurs on the wrists, shins, scalp, lumbar region, glans penis, or mucous membranes.6 Lichen planus rarely involves the cheeks, and there are no systemic manifestations.5
Papular urticaria is characterized by chronic or recurrent eruptions of intensely pruritic papules, vesicles, and wheals caused by a hypersensitivity reaction to insect bites.7 The lesions are usually grouped in linear clusters on exposed skin, but spare the genital, perianal, and axillary regions. Although the condition can occur in all age groups, it predominantly affects children. Intense pruritus and excoriations may be present. The rash of papular urticaria resolves much sooner than that of Gianotti-Crosti syndrome. Papular urticaria is diagnosed in patients of appropriate age with symmetrically distributed lesions, a history of hypersensitivity, and exposure to animals or insects.7
Scabies is caused by the Sarcoptes scabiei mite and is spread through skin-to-skin contact. Intense pruritus, the most prevalent symptom, is usually worse at night and spares the face and head. The mite often infests the skin of the finger webs, wrists, elbows, axillae, buttocks, and genitalia. Cutaneous manifestations include inflammatory papules, burrows, nodules, and excoriations.8
Selected Differential Diagnosis of a Pruritic Acral Rash in a Child
| Condition | Characteristics |
|---|---|
| Erythema multiforme | Target-shaped papular and vesiculobullous lesions distributed symmetrically on extremities and mucous membranes |
| Gianotti-Crosti syndrome | Monomorphous, pink to red-brown papules or papulovesicles distributed symmetrically on the face, extensor surfaces of the extremities, and buttocks; asymptomatic or mildly pruritic |
| Lichen planus | Flat-topped, pink to violaceous, shiny, polygonal papules with overlying white scales (Wickham's striae) on the wrists, shins, scalp, lumbar region, glans penis, or mucous membranes; intensely pruritic |
| Papular urticaria | Linear clusters of papules, vesicles, and wheals on exposed skin that spare the genital, perianal, and axillary regions; intensely pruritic |
| Scabies | Inflammatory papules, burrows, nodules, or excoriations typically on the finger webs, wrists, elbows, axillae, or buttocks; intensely pruritic |
Information from Brandt O, Abeck D, Gianotti R, Burgdorf W. Gianotti-Crosti syndrome. J Am Acad Dermatol. 2006;54(1):136–145.

