A 15-year-old girl presented with a history of bilateral swelling of the legs that had worsened over the preceding five years. It first appeared on her left foot, and then it spread to her right foot. Over the years, the swelling spread up her legs. Initially, it was worse in her left leg, but it eventually affected both legs equally (see accompanying figure). Although the swelling persisted throughout the day, it was worse in the evening. The patient had no history of fever, shortness of breath, chest pain, urinary symptoms, or local trauma, and she had never traveled internationally.
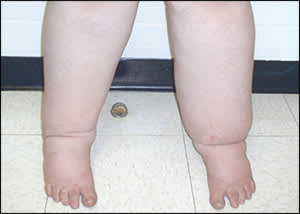
Examination revealed that the patient was obese and had bilateral pitting edema on her lower legs that extended to the upper thighs. The overlying skin was warm, erythematous, thickened, and hyperpigmented. The remainder of her examination was unremarkable. Results from complete blood count, chemistries, lipid panel, urinalysis, and thyroid and liver function tests were normal. Imaging findings, including echocardiography, lower extremity venous Doppler ultrasonography and magnetic resonance imaging, abdominal ultrasonography, and computed tomography were also normal.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Lymphedema praecox.
B. Myxedema.
C. Nephrotic syndrome.
D. Portal vein thrombosis.
E. Systolic heart failure.
Discussion
The answer is A: lymphedema praecox. Lymphedema praecox is a debilitating and disfiguring condition that usually occurs in adolescents. It accounts for 94 percent of all primary (hereditary) lymphedema cases and affects girls 10 times more often than boys. Nearly 75 percent of cases are unilateral, with the left leg more often involved.1 The differential diagnosis of bilateral lower extremity edema includes venous thrombosis, heart failure, liver failure, nephrotic syndrome, hypothyroid myxedema, and venous insufficiency.
The progressive swelling of lymphedema is often soft with pitting at onset and then advances to the classic firm, nonpitting edema. The excessive swelling causes weight gain, fatigue, and impairment in daily activities. Overlying skin undergoes thickening and hyperkeratinization, and is prone to recurrent infection.
Primary lymphedema is a hereditary developmental disorder of the lymphatic system that can be divided into three categories based on the patient's age at onset: congenital lymphedema (Milroy disease) presents at birth; lymphedema praecox (Meige disease) presents between one and 35 years of age, peaking during puberty; and lymphedema tarda presents after 35 years of age.2,3 The exact etiology of lymphedema praecox is unknown; however, hypoplasia of the lymphatic wall tissue and mutations or agenesis of lymphatic valve tissue may be involved.3,4 As the disease progresses, subcutaneous fibrosis leads to nonpitting edema.
Primary lymphedema most often follows an autosomal dominant pattern of inheritance.2 Several studies have suggested specific genetic mutations, including that on chromosome 5. Primary lymphedema may be associated with hypoparathyroidism, microcephaly, distichiasis (i.e., double row of eyelashes on an eyelid), yellow nails, vertebral anomalies, cerebrovascular malformations, and intestinal lymphangiectasia.2
There is no known cure for primary lymphedema. Treatment focuses on controlling edema and limiting progression and complications. Diligent skin and nail hygiene is critical in preventing secondary cellulitis, and exercise should be encouraged for weight control and fluid mobilization. Some patients benefit from decongestive physiotherapy with manual lymphatic drainage massage. Other treatments involve relieving congestion with limb elevation and compressive garments or wraps.4 Intermittent pneumatic compression has been successful in some patients. Diuretics are not indicated in the treatment of lymphedema; however, some studies report benefits with flavonoids (or benzopyrones, not available in the United States).4 Surgical procedures are palliative and focus on debulking or drainage bypass.
Selected Differential Diagnosis of Bilateral Lower Extremity Edema
| Condition | Characteristics |
|---|---|
| Liver failure | Edema caused by portal congestion or hypoalbuminemia, depending on severity of hepatic damage |
| Lymphedema | Edema caused by damage to, or maldevelopment of, the peripheral lymphatic system |
| Myxedema | Soft-tissue edema in patients with severe and advanced hypothyroidism; typically associated with other hypothyroid manifestations, such as bradycardia, constipation, and weight gain |
| Nephrotic syndrome | Edema caused by hypoproteinemia or hypoalbuminemia secondary to kidney disease |
| Systolic heart failure | Decreased cardiac ejection fraction leads to pulmonary, hepatic, and peripheral venous congestion |
| Thrombosis (portal vein, extremity, inferior vena cava) | Edema caused by thrombotic obstruction of venous drainage |
| Venous insufficiency | Edema caused by failure of venous return secondary to deep venous damage and/or incompetence |

