Purpose
Each month, our three presenters review an interesting journal article in a conversational manner. These articles involve “hot topics” that affect family physicians or “bust” commonly held medical myths. The presenters give their opinions about the clinical value of the studies discussed. The opinions reflect the views of the presenters, not those of AFP or the AAFP.
This Month's Article
Bobrow BJ, Clark LL, Ewy GA, et al. Minimally interrupted cardiac resuscitation by emergency medical services for out-of-hospital cardiac arrest. JAMA. 2008;299(10):1158–1165.
Does the ACLS recommendation to limit interruptions during cardiac resuscitation result in improved outcomes for patients with cardiac arrest?
Bob: The American Heart Association created its first set of Advanced Cardiac Life Support (ACLS) guidelines in 1974, with subsequent updates every four to six years. The latest version of the guidelines was introduced in December 2005.1 Among the changes in the new guidelines was an emphasis on avoiding interruptions in chest compressions in patients with cardiac arrest. This recommendation was made on the belief that if interruptions in chest compressions could be avoided, the poor survival rates for patients who have out-of-hospital cardiac arrest could be improved. This study attempts to test this theory.
What does this article say?
Bob: This prospective study was performed by emergency medical services (EMS) in two metropolitan cities in Arizona from January 1, 2005, to June 30, 2007. During the first six months (the “baseline” period), traditional cardiac resuscitation was performed. From July 2005 to January 2006, EMS personnel were instructed on the use of minimally interrupted cardiac resuscitation (MICR). In this technique, a patient with cardiac arrest is given an initial 200 uninterrupted chest compressions at 100 compressions per minute and rhythm analysis with a single shock (if indicated), immediately followed by another 200 chest compressions before any pulse check or rhythm reanalysis (Figure 1). Survival to hospital discharge “before MICR” and “after MICR” initiation was measured.
Figure 1. Minimally Interrupted Cardiac Resuscitation
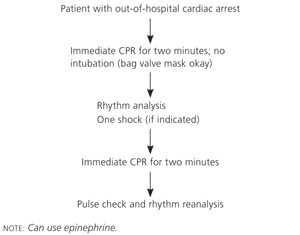
Minimally interrupted cardiac resuscitation technique. (CPR = cardiopulmonary resuscitation.)
In the period before MICR, four of 218 patients survived to hospital discharge (1.8 percent). In the period after MICR, 36 of 668 patients survived to hospital discharge (5.4 percent). The rate of survival was even better in the subgroup of patients with witnessed cardiac arrest and ventricular fibrillation.
Should we believe this study?
Bob: Before we analyze this study, we need to ask a couple questions. One, is there a need to improve cardiac resuscitation? I would suggest there is. Rates of survival for patients with out-of-hospital cardiac arrest are generally dismal. For example, in Chicago, Ottawa, and Los Angeles, the chance of being discharged from a hospital alive after experiencing an out-of-hospital cardiac arrest is 1.7, 5.2, and 1.4 percent, respectively.2–4
Two, are interruptions in cardiac compressions a real problem that needs to be addressed? One famous study revealed that no chest compressions were performed 48 percent of the time by EMS personnel during resuscitation of patients with out-of-hospital cardiac arrest.5 Another study demonstrated that, in hospitalized patients, less than 90 compressions per minute were performed 28 percent of the time during resuscitation efforts.6
Andrea: Clearly, interruptions in chest compressions are common. The reasons for these interruptions include multiple and prolonged attempts at intubation, pulse and rhythm checks, application of defibrillators, and patient transfers. When compressions are halted, no blood is circulated through the coronary and cerebral vasculature.
Bob: So, does this protocol of limiting interruptions really produce a threefold increase in survival? There are some factors that limit the robustness of this conclusion. First, this study used an interrupted time series design (i.e., a “before and after” study). Such studies have many possible confounders that could influence the outcome of the study. Some examples would be: were better-trained EMS personnel present in the later study period? Were EMS response times improved? Were more or better-equipped EMS vehicles available? Were other protocols or interventions (e.g., rapid sequence intubation, new medications) introduced?
Mark: The second reason the threefold increase in survival noted with the MICR technique may be too good to believe is the possible role of the Hawthorne effect. This phenomenon was first noted in a series of studies at the Hawthorne Plant of the Western Electric Company in Cicero, Ill., in which workers' behavior (i.e., productivity) was altered because they knew they were being studied. The same phenomenon can occur in medical studies. In this case, did the MICR training given to the EMS personnel motivate them to provide better care independent of the new MICR protocol? Also, they knew they were in a study. The Hawthorne effect suggests that once the study ends and the participants know they are no longer being observed, results often return to the baseline. Will these gains in survival persist now that the study has ended?
What should the family physician do?
Bob: I think the recommendation to avoid interrupting chest compressions during cardiac resuscitation is reasonable. However, I am a little skeptical that this new technique will universally deliver a sustained threefold improvement in survival for the reasons cited above.
Mark: Perhaps, instead of trying to develop new protocols, we could take a few lessons from the communities in which the survival rates are above the norm. For example, in Seattle, 31 percent of patients are successfully resuscitated from out-of-hospital cardiac arrests, and 43 percent survive to hospital discharge.7 What are they doing right?
Andrea: Although I see value in attempting to improve resuscitation rates, I also see extraordinary resources (financial and manpower) being used to try to increase survival rates by mere percentage points. Does anyone sense that perhaps our resources would be better spent trying to prevent the need for cardiac resuscitation?
Main Points
- Interruptions in chest compressions during cardiac resuscitation are common.
- The 2005 ACLS resuscitation protocol recommends that patients with out-of-hospital cardiac arrest immediately be given 200 uninterrupted chest compressions at 100 compressions per minute and rhythm analysis with a single shock (if indicated), followed by another 200 chest compressions before any pulse check or rhythm reanalysis.
EBM Points
- Studies with an interrupted time series design, also known as “before and after” studies, are subject to numerous potential confounders because of uncontrolled changes that occur in the study environment over time.
- The Hawthorne effect is a temporary change in behavior (and consequently, study outcomes) that can occur when study participants know they are being observed. Gains achieved during the study period often regress when the study ends.

