A 51-year-old man presented with a lesion on his hand. The patient had recently returned from a trip to the midwestern United States and said that an insect may have bitten him. The rash began as a nonpainful, papular lesion measuring approximately 4 to 5 mm. Over one week, the lesion grew progressively in size, and multiple painful ulcerations developed (see accompanying figure). The patient had no previous rashes, and he denied having fever, chills, or recent illness. He had a history of significant hypertension, which was controlled with lisinopril (Zestril), 40 mg daily. He did not have a history of surgery, and his family and social histories were noncontributory.
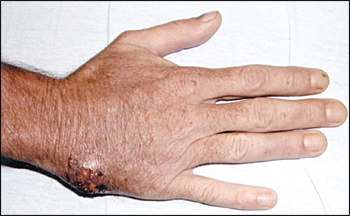
Physical examination demonstrated normal vital signs, and the patient was afebrile. The examination of the hand revealed erythema and swelling over the dorsum of the affected hand with multiple ulcerations. There was no associated lymphadenopathy or other remarkable physical examination findings.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Brown recluse spider bite.
B. Herpes zoster.
C. Latent syphilis.
D. Melanoma.
E. Pyogenic granuloma.
Discussion
The answer is A: brown recluse spider bite. The brown recluse spider (Loxosceles reclusa) is found throughout the midwestern United States. The brown recluse spider bite is capable of causing necrotic wounds.1 In addition to the characteristic physical findings, the diagnosis is based primarily on a careful history.
Early diagnosis is key in avoiding many of the potential complications associated with brown recluse spider bites; necrotizing fasciitis is the most serious complication.2 Tissue damage in the area surrounding the bite causes a painful infarction of the skin that may heal slowly.3 If envenomation occurs, the lesion typically develops into a necrotic ulcer.4
Envenomation with the sphingomyelinase D2 enzyme is thought to be responsible for activating vascular endothelial cells, leading to tissue necrosis.2,4 In addition, sphingomyelinase D2 damages the myelin sheaths, thereby heightening the sensation of pain that is often associated with necrotizing fasciitis.
Treatment of most brown recluse spider bites requires only supportive care,5 such as RICE (rest, ice, compression, elevation) therapy. Nonsteroidal anti-inflammatory drugs, including aspirin, and antihistamines are also used initially to control the inflammatory response. Tetanus prophylaxis should be considered in patients with more progressed lesions because open lesions might increase the risk of tetanus. If there are signs of cellulitis, antibiotics (e.g., erythromycin, a cephalosporin) should be administered.
Treatment with topical dapsone or nitro-glycerin has also been suggested.5,6 Topical dapsone is thought to minimize tissue destruction by suppressing neutrophils, although this is controversial.6 Topical dapsone is effective only if administered within hours of envenomation. Its adverse effects, however, may be severe and include dose-related hemolysis, aplastic anemia, and agranulocytosis, but these effects usually occur with oral doses. In addition, patients with glucose-6-phosphate dehydrogenase deficiency should not receive dapsone.
Topical nitrates seem to enhance circulation and, therefore, assist in tissue repair. The effectiveness of nitrate treatment has not been proven.
Herpes zoster is characterized by a vesicular or bullous eruption limited to a dermatome innervation. Latent syphilis is the stage of the infection in which there are no clinical signs or symptoms. Melanoma usually presents as a pigmented lesion. Pyogenic granuloma presents as a rapidly developing papule with capillary proliferation that bleeds easily.
Summary Table
| Condition | Characteristics |
|---|---|
| Brown recluse spider bite | Rapidly transforming lesions that may ulcerate and necrotize the dermal layers |
| Herpes zoster | Vesicular or bullous eruption limited to a dermatome innervation |
| Latent syphilis | Usually, no signs of infection are apparent at this stage |
| Melanoma | Pigmented lesion that develops much slower than a spider bite |
| Pyogenic granuloma | A rapidly developing papule with capillary proliferation that bleeds easily |

