Many barriers exist to finding answers to physicians’ clinical questions. Lack of time, resources, and computer skills, as well as physicians’ environment and attitudes about problem solving, all contribute to unanswered questions. Making use of computer-based information resources can give physicians a framework for answering questions and keeping their practice consistent with the best available evidence.
Admit it. You have questions about patient care that you never take the time to look up. When asked at the end of the day, most physicians can recall one or two questions about patient care that went unanswered.1 But when asked after every patient visit, it turns out that we have 15 to 20 questions per day, most of which went unanswered.1 Whether it is a new language, a new physical skill, or a clinical question, adults learn to solve problems. For physicians, those problems are the questions that arise during the care of our patients.
Why don’t we answer all of our questions? There are many barriers, one of which is lack of time.2 Finding an answer can take time, especially if we have to leave the room or aren’t skilled at using computers. And you do have to use computers, because medical knowledge is changing more and more rapidly. In fact, the average textbook on a family physician’s bookshelf is more than 10 years old.3 Just think how many new drugs, tests, and guidelines have become part of routine practice during that time. Other barriers include lack of skill in searching for information, lack of access to relevant references, and thinking that the answer isn’t available (Table 1).1,2 Some barriers are cultural—if you work in a group where the emphasis is on productivity and not making waves, questions may be discouraged. Figure 1 traces the process of asking and answering questions, including common barriers.1 Think about which barriers exist in your practice and what you might do to address them.
Table 1. Possible Solutions to Barriers to Answering Clinical Questions
| Barrier | Possible solutions |
|---|---|
| Attitude | Value your own questions and write them down as they occur |
| Respond positively when colleagues ask questions | |
| Create a “question-and-answer club” where you and your colleagues share the best available evidence to answer recent clinical questions | |
| Environment | Make computers available where you practice, or carry a tablet computer, PDA, or smartphone |
| Plan adequate time every week or month to review recent literature | |
| Lack of computer skills | Attend computer boot camps at AAFP national meetings |
| Buy a PDA or smartphone and practice using it | |
| Take classes at a local college or read books that teach basic computer skills | |
| Practice searching for answers to become more proficient | |
| Lack of resources | Subscribe to relevant evidence-based information sources |
| Create a Web portal that has links to commonly used information sources (see http://www.google.com/ig or http://www.myhq.com) | |
| Keep a computer, PDA, or smartphone handy while seeing patients or while on rounds | |
| Lack of time | Carry a PDA or smartphone for rapid access to information |
| Make sure computers are available wherever you see patients |
AAFP = American Academy of Family Physicians; PDA = personal digital assistant.
Figure 1.
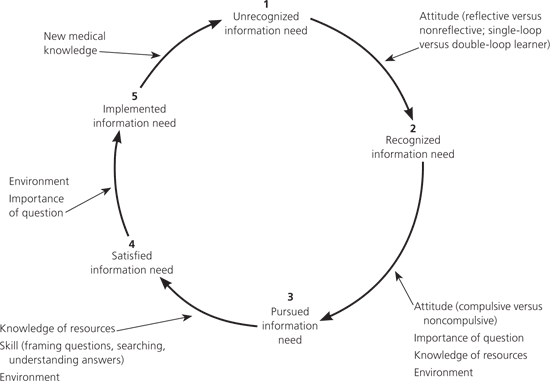
The process of asking and answering clinical questions and relevant barriers.
Reprinted with permission from Ebell M. Information at the point of care: answering clinical questions. J Am Board Fam Pract. 1999;12(3):229.
In addition to a way to answer questions at the point of care, you also need a way to stay current with new studies. Even if you don’t need information from a new study today, you should be alerted to it so you know it is available when you need it. And of course, you need to be able to quickly answer questions between patients. Your information sources should give you access to all types of information.
The most useful information is relevant, valid, and takes little work to access and apply.4 Increasingly, that information is computer-based. Books are out of date the moment they hit the bookshelves, because there is at least a six-month delay between editing and publication. Although some computer-based information sources are also static, many are updated almost continuously—an increasingly important advantage.
Computers also make it easy to take advantage of the increasing number of validated decision-support tools. For example, it would be difficult to remember the Wells rule for diagnosis of pulmonary embolism, which consists of eight findings from the patient’s history and physical examination plus a fairly involved decision algorithm.5 However, it is easy to use this rule when it is converted to an interactive calculator on a handheld computer (Figure 2).5
Figure 2.
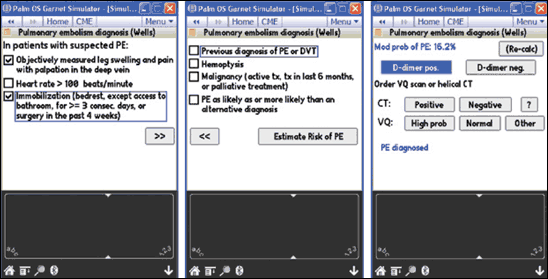
A clinical decision rule for a handheld computer.
Information from reference 5.
Which information sources can you trust? What makes a medical reference, electronic or otherwise, evidence-based? Perhaps the single best indicator is whether the reference clearly states how strong the evidence is to support recommendations about patient care. In American Family Physician, we use the Strength of Recommendation Taxonomy (SORT) system (https://www.aafp.org/online/en/home/publications/journals/afp/afpsort.html). If a medical reference doesn’t tell you the strength of evidence behind key recommendations, it is difficult to know whether there is evidence of benefit for our patients.
Another good sign of evidence-based material is when the reference carefully describes how the literature was searched, so you can be confident they looked at all of the evidence rather than just a selection of it. Finally, you should know if a company or special interest group with a vested interest in the topic sponsored the study. Articles may be biased because the sponsor provided a biased literature search, because the authors are unknowingly biased in favor of the sponsor because of the grant or fee for writing the article, or because in some cases the article is largely written for them by a medical communications company (i.e., “ghost writing”). Table 2 lists some objective, evidence-based sources of information.
Table 2. Selected Evidence-Based Sources of Medical Information
| Source | Comment | Web site |
|---|---|---|
| ACP Physicians’ Information and Education Resource | Subscription-based online textbook from ACP; PDA version available | http://pier.acponline.org |
| Agency for Healthcare Research and Quality | Includes USPSTF and EPC reports; PDA and smartphone application is available for screening and prevention recommendations | USPSTF: http://www.ahrq.gov/clinic/prevenix.htm EPC: http://www.ahrq.gov/clinic/epcix.htm |
| Bandolier | British online periodical that reviews evidence for important clinical questions | http://www.medicine.ox.ac.uk/bandolier |
| Clinical Evidence Handbook | Subscription-based online reference; freely available for physicians who receive the print summary from United Healthcare; PDA and smartphone version available. Excerpted monthly in AFP | http://clinicalevidence.bmj.com |
| Cochrane Collaboration | Extensive database of systematic reviews and clinical trials. Excerpted monthly in AFP | http://www.cochrane.org |
| DynaMed | Subscription-based online textbook | http://dynamicmedical.com |
| Essential Evidence Plus (formerly InfoRetriever) | Subscription-based online reference with extensive calculators, decision support tools, POEMs, and Cochrane systematic reviews; PDA and smartphone version available | http://www.essentialevidenceplus.com |
| Institute for Clinical Systems Improvement | Nonprofit consortium of physicians and insurance companies that writes and disseminates evidence-based practice guidelines | http://www.icsi.org/guidelines_and_more/ |
| National Guideline Clearinghouse | Includes evidence-based and consensus guidelines; limit to former by using “detailed search” option and limiting results to guidelines that weight evidence according to a rating scheme | http://www.guidelines.gov |
| Turning Research Into Practice Database | Searches multiple evidence-based Web sites simultaneously | http://www.tripdatabase.com |
ACP = American College of Physicians; AFP = American Family Physician; EPC = Evidence-based Practice Center; PDA = personal digital assistant; POEM = patient-oriented evidence that matters; USPSTF = U.S. Preventive Services Task Force.
PubMed is the interface to the National Library of Medicine’s repository of medical literature. Although it is an incredible resource, it is not the first place you should look to find answers to your questions. There is so much information it is like trying to drink from a firehose. One way to focus your search is to use the Clinical Queries feature on the PubMed home page. These searches are configured to find the most relevant, valid research on a topic. Once you find a particularly useful article, look at the related articles for additional relevant studies.
Finally, no article on searching the medical literature would be complete without mentioning Google. This search engine is becoming increasingly helpful because it now indexes the National Library of Medicine and provides specific links about diagnosis, treatment, and other clinically relevant subtopics. Although much of the information is aimed toward patients, selecting “for health professionals” in the search results will yield information more tailored to physicians (Figure 3). The Google Scholar search is also helpful (http://www.scholar.google.com).
Figure 3.
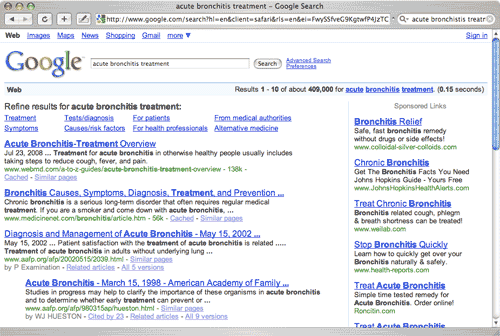
Sample Google search.
Where should you begin? Some practical tips are shown in Table 2. Work with your colleagues to implement strategies that make you a better manager of information, and that give you a framework for answering questions and keeping your practice consistent with the best available evidence.

