A 23-year-old woman in the third trimester of pregnancy presented with malaise, a low-grade fever, and a pruritic rash. Her three-year-old son had a similar rash two weeks earlier. On examination, vesicles, umbilicated pustules, and crusted lesions were noted on the face, trunk, and limbs (Figures 1 and 2). The rash did not concentrate in the woman’s stretch marks, and all lesions were less than 1 cm in diameter. Other physical examination findings were unremarkable.
Figure 1.
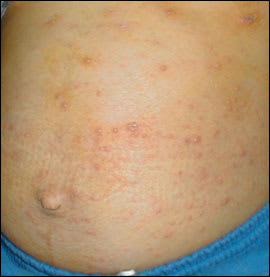
Figure 2.
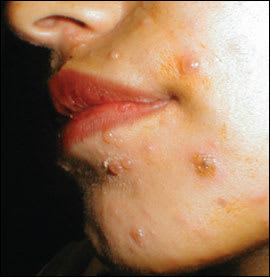
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
A. Coxsackievirus.
B. Impetigo.
C. Measles.
D. Pruritic urticarial papules and plaques of pregnancy (PUPPP).
E. Varicella virus.
Discussion
The answer is E: varicella virus. Varicella (chickenpox) is characterized by the simultaneous development of lesions at various stages. The incubation period of chickenpox is 10 to 21 days. The rash, which may persist for 20 days, begins 48 hours after the onset of headache, malaise, and fever. The lesions appear as vesicles on an erythematous base, and new lesions emerge throughout the first week. The lesions cloud, umbilicate, then crust over. The patient is contagious until all of the lesions have crusted.
Approximately five in 10,000 pregnant women develop chickenpox.1 Infection in pregnancy requires consideration of the mother and the fetus. Adults with varicella infection are at increased risk of pneumonia, hepatitis, and encephalitis. Infection in the first 20 weeks of pregnancy can lead to congenital varicella syndrome in up to 2 percent of fetuses.2 This syndrome is characterized by neurologic abnormalities (e.g., mental retardation, cortical atrophy), eye defects, hypoplastic limbs, and dermatomal skin scarring. In the five days before and the two days after delivery, the mother has not yet transferred protective antibodies to the newborn, increasing the child’s risk of severe disseminated varicella infection. Infants exposed to varicella in utero can develop shingles during infancy or early childhood.
Ideally, persons exposed to varicella should receive prophylaxis with intramuscular varicella-zoster immune globulin (VZIG) within 96 hours of exposure. The varicella vaccine is a live-virus vaccine and should not be administered during pregnancy.2 There is little evidence to support prophylaxis with acyclovir (Zovirax; U.S. Food and Drug Administration [FDA] pregnancy category B).1 Newborns of mothers with late varicella infection should be treated with 125 units of VZIG.2
Once infected, treatment includes isolation from other pregnant women and administration of fluids, analgesia, and antipruritic agents. Oral acyclovir or famciclovir (Famvir; FDA pregnancy category B) may reduce the severity of illness if initiated within 72 hours of rash onset.2 Patients with disseminated disease or pneumonia should be hospitalized and receive intravenous acyclovir, although acyclovir does not reduce the incidence of congenital varicella syndrome.1
Coxsackievirus infection (hand-foot-and-mouth disease) is characterized by nonpruritic vesiculopustules on the soft palate, soles, and palms.
With bullous impetigo, an epidermolytic toxin causes the appearance of thin-walled vesicles that collapse in the center, with yellow crusting over an erythematous base. Fever occurs only with secondary complications, such as osteomyelitis or sepsis. In contrast to those of varicella, the lesions of bullous impetigo can be 2 to 8 cm in diameter and persist for months if not treated.
Measles is characterized by a prodrome of severe cough, coryza, conjunctivitis, and fever, followed by a maculopapular rash on the face that spreads to the trunk. The lesions become confluent, peaking simultaneously, and fade to yellowish-brown patches with a fine scale. Pathognomonic Koplik spots may appear prior to the rash.
PUPPP, also known as polymorphic eruption of pregnancy, is common. The rash begins as intensely pruritic papules in the stretch marks that spread to the extremities and coalesce into urticarial plaques. Vesicles rarely form. The face, palms, and soles are spared. PUPPP also does not cause fever.
Summary Table
| Condition | Characteristics |
|---|---|
| Coxsackievirus | Nonpruritic vesiculopustules on soft palate, soles, and palms |
| Impetigo | Thin-walled vesicles that collapse in the center; appears anywhere on the body; yellow crusting over an erythematous base; often tender or mildly pruritic; no systemic symptoms |
| Measles | Maculopapular, nonvesicular rash; spreads from face to trunk; pathognomonic Koplik spots; prodrome of severe cough, coryza, conjunctivitis, and fever |
| Pruritic urticarial papules and plaques of pregnancy | Intensely pruritic papules that coalesce into urticarial plaques; vesicles are rare; spares the face, palms, and soles; no systemic symptoms |
| Varicella virus | Disseminated rash; simultaneous vesicles, umbilicated pustules, and crusted lesions; fever and malaise |

