Exercise is beneficial for women of all ages and is associated with long-term health benefits and enhanced well-being. Nevertheless, active women and girls are at risk for conditions resulting from sports and exercise participation. Because of their unique physiology, children are more susceptible to heat illness than adolescents and younger adults. Childhood sports injuries tend to involve the growth plate. Adolescents share some concerns with child athletes but have injuries more similar to those that occur in adults, especially ligament and tendon injuries. Adolescents and adult women are at risk for anterior cruciate ligament injuries, patellofemoral pain syndrome, and stress fractures. For athletes in these age groups, physicians should screen for pelvic floor dysfunction and the female athlete triad, especially in patients with a history of stress fractures. In adult women, exercise can contribute to disease prevention and management. Continuation of an appropriate exercise routine helps older women maintain independence and prevent falls.
Evidence shows that exercise confers significant health benefits for women of all ages.1–6 Regular physical activity helps prevent disease and promote wellness. The Centers for Disease Control and Prevention recommends moderate-intensity physical activity for at least 30 minutes on most—and preferably all—days of the week.7 Aerobic activities are ideal, but encouraging a woman to choose an exercise she enjoys (aerobic or anaerobic) promotes long-term adherence at all ages. The benefits of exercise, such as improved fitness and weight control, are apparent at a young age; additional benefits, such as the prevention and treatment of chronic disease, extend throughout the life span. Nevertheless, as the female athlete progresses from childhood to maturity, her physiology puts her at risk for a variety of conditions (Figure 1). This article examines some common conditions that physically active girls and women may encounter during different life stages.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Preventive strategies for heat illness include frequent substitutions during competition on hot, humid days; gradual acclimatization to warmer climates with initiation of strenuous activities over 10 to 14 days; adequate hydration before and during activity; frequent mandatory fluid breaks; and wearing light-colored, lightweight, absorbent clothing. | C | 9, 12 |
| Preventive strategies for anterior cruciate ligament injury include proprioceptive training and strength training of the lower extremities and core. | C | 32, 33 |
| High school and college female athletes should be screened for the female athlete triad. | C | 19, 20 |
| Women should exercise regularly during pregnancy. | A | 34, 36 |
| Older women should engage in regular physical activity to improve disease outcomes and help prevent falls. | B | 35, 48 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Figure 1. Common Concerns for Female Athletes by Age
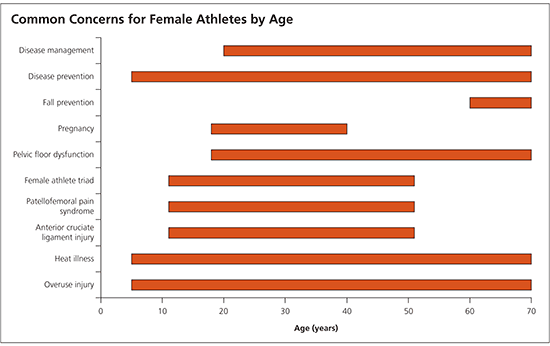
Common conditions and other issues affecting female athletes, grouped by age of most likely occurrence.
Childhood (4 to 10 Years)
Many young girls participate in athletic training. This can predispose them to injury because their immature bodies may not be prepared for the challenges of high levels of activity. Physicians should be alert for heat-related illness and overuse injuries in young athletes.
HEAT-RELATED ILLNESS
Heat-related illness can occur at any age, but children and older adults are at higher risk because of their less efficient thermo-regulatory systems.8 Certain conditions (e.g., obesity, illness, use of prescription or illicit drugs, heavy clothing) increase the risk for dehydration and subsequent heat-related illness, especially in athletes who are unaccustomed to high temperatures.
Symptoms of minor heat-related illness include edema in the lower extremities, cramps with painful muscle spasms, and syncope. These conditions can be effectively treated with sodium replacement, rehydration, supine positioning, and moving to a cooler environment. Heat exhaustion presents with multisystem symptoms, such as headache, dizziness, nausea, vomiting, malaise, vertigo, and weakness. Physical signs include tachycardia and possible elevation of core body temperature to between 100.4°F (38.0°C) and 104.9°F (40.5°C). Treatment is similar to that of minor heat illness. Heat stroke, a medical emergency, presents as acute changes in mental status accompanied by a core body temperature greater than 104.9°F. It is a potentially life-threatening condition with multiorgan system involvement. Prompt diagnosis is essential. Treatment includes rapid cooling, parenteral rehydration with dextrose and normal or half-normal saline, and immediate hospitalization. Rapid cooling in the setting of suspected heat stroke can be life-saving. On-site personnel should actively attempt to cool the athlete while awaiting transport to a medical facility.
The physiologic response to heat in children and adolescents differs from homeostatic mechanisms in adults. Compared with adults, children generate more metabolic heat per unit mass during exercise, and they have a slower acclimatization response, a decreased ability to sweat, and a higher surface area-to-body mass ratio, resulting in greater temperature gain from the environment than adults.9 Consequently, children have a reduced ability to adapt to heat stress compared with adults. Thirst is not a reliable indicator of hydration in children because they do not develop an appropriate thirst response to heat.
The level of heat stress and appropriate adjustment of exercise can be determined based on the combination of ambient temperature and humidity (Figure 2).10,11 Relative humidity is an important determinant of heat stress because evaporative cooling from sweat decreases with increasing humidity. The National Athletic Trainer’s Association provides multiple resources, including a practical guide for parents and coaches on the safe participation of children during hot and humid conditions.10
Figure 2. Prevention of Dehydration and Heat Illness in Children
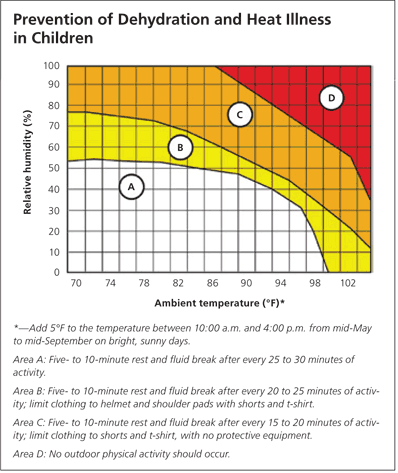
Guide for determining the frequency of rest and fluid breaks to prevent dehydration and heat illness during outdoor activity.
Adapted with permission from Kulka J, Kenny WO. Heat balance limits in football uniforms: how different uniform ensembles alter the equation. Phys Sportsmed. 2002:30(7):29–39, with additional information from reference 10.
Prevention of heat-related illness is the goal. The American Academy of Pediatrics, the American College of Sports Medicine, and other expert groups recommend frequent substitution of players during competition to increase rest periods on hot, humid days; gradual acclimatization to warmer climates (allowing 10 to 14 days for acclimatization); adequate hydration before and during activity (with frequent scheduled mandatory fluid breaks); and wearing light-colored, lightweight, absorbent clothing.8–10,12
OVERUSE INJURIES
Overuse injuries are common at all ages. They occur with repetitive activities and are associated with inadequate rest periods, sudden change in the type or intensity of training, poor technique, and faulty equipment (e.g., worn-out running shoes). Children and adolescents have an increased risk of overuse injury because of muscle imbalance, inflexibility, and the susceptibility of growth cartilage to repetitive stress.13
Overuse injuries in the prepubertal age group are more likely to involve the growth plate. Injured growth cartilage at apophyses can result in tibial tubercle apophysitis (Osgood-Schlatter disease), calcaneal apophysitis (Sever disease), medial epicondyle apophysitis (little leaguer’s elbow), and traction apophysitis of the hip. In addition, physeal (growth plate) injuries can occur from repetitive loading, resulting in partial or complete growth arrest.13 Treatment of growth-plate–related injuries should be targeted to the specific bone affected, but typically involves relative rest (participating in alternative activities), application of ice, analgesic medication use, and rehabilitation.
Overuse injuries should be prevented whenever possible. Training programs for children and adolescents should emphasize global conditioning, flexibility, and refraining from early sport specialization and excessive activity. Sport-specific training programs should be appropriate for the age group and within the physiologic limitations associated with growth. This may require restrictions, such as pitch-count limits in baseball. The intensity of athletic activity should be dictated by the physical well-being of the athlete. Pressure from parents, coaches, or others to increase activity beyond safe limits must be resisted. Gradual progression in training is advised, increasing the total training (duration, intensity, and frequency) by no more than 10 percent per week.13 Scheduled rest intervals are especially important for injury prevention in young athletes.
Strength training complements aerobic activity in all age groups. In children, it can be done safely as long as proper supervision and correct lifting techniques are emphasized. A systematic review evaluated 22 reports of experimental resistance training protocols in pre- and early-pubertal children.14 Strength gains as a result of resistance training were noted. The training programs had no significant influence on the height or weight of participants. Injuries were uncommon, with estimated injury rates of less than 0.2 per 100 participant-hours.14
Adolescence (11 to 17 Years)
Exercise is beneficial for adolescent girls and often leads to lifelong fitness habits. Adolescent girls have some of the same exercise-related concerns as children; however, because of changes in anatomy and physiology during puberty, different types of injuries can occur. Growth plate injuries are less common in adolescents than in children. Conversely, conditions and injuries associated with the adult population, such as overuse injuries, the female athlete triad, sacroiliac dysfunction, and anterior cruciate ligament (ACL) injury, can also occur in adolescents.
OVERUSE INJURIES
Common overuse injuries in postpubescent girls include patellofemoral pain syndrome and stress fractures.
Patellofemoral Pain Syndrome. Patellofemoral pain syndrome is common in adolescent girls. This condition is characterized by anterior knee pain that is related to activity. The pain is exacerbated by going up or down stairs or running on hilly terrain. It is associated with lower extremity malalignment and weakness, as well as inadequate core and hip abductor strength. This condition rarely requires surgical intervention. A rigorous rehabilitation program designed specifically for the athlete and her sport should be prescribed.15
Stress Fractures. Stress fractures occur as a result of repetitive loading that exceeds the bone’s ability to heal. Stress fractures occur more commonly in females than in males, and they can occur in any sport.16,17 Common sites include the tibia, tarsals, metatarsals, and femur. After identifying a stress fracture, it is important to evaluate lower extremity alignment, strength, and gait, and to screen for risk factors, such as disordered eating, menstrual dysfunction, and other chronic medical conditions that may predispose the athlete to bone loss. Most stress fractures are treated nonsurgically, but specific therapy depends on the location of the injury. High-risk stress fractures, such as those in the femoral neck, anterior cortex of the tibia, and proximal fifth metatarsal, should be referred to a sports medicine or orthopedic subspecialist because of the high likelihood of fracture-related complications.
FEMALE ATHLETE TRIAD
Female high school and collegiate athletes should be screened for components of the female athlete triad (i.e., disordered eating, menstrual dysfunction, and loss of bone mineral density) during the preparticipation physical evaluation.18–20 Athletes identified as having one or more components, or who are found to be at risk, should be referred to specialists experienced in the evaluation and management of this condition. A multi-disciplinary team approach to evaluation and treatment of disordered eating is the preferred method of care.21,22 The treatment team should consist of a physician, nutritionist, and mental health provider. Additional team members may include an athletic trainer and strength and conditioning coach. Coaches are discouraged from active participation in the treatment of eating disorders. In addition to conflicts of interest, coaches may be perceived to pressure athletes (for example, in maintaining a place on the team or continued scholarship support).
Continued participation in training and competition depends on the physical and mental health of the athlete. Athletes who weigh less than 80 percent of their ideal body weight may not be able to safely participate. Athletes with evidence of health consequences of disordered eating (e.g., electrolyte disturbances, anemia, hypotension, bradycardia, syncope, hematemesis, depression, suicidal ideation or intent) should be closely monitored by a physician.23 Medical safety should be ensured before allowing the athlete to return to training or competition.
Menstrual dysfunction in athletic women generally presents as secondary amenorrhea or oligomenorrhea. Pregnancy must be excluded as a cause of menstrual dysfunction.24 Assessment of menstrual dysfunction should include medical, menstrual, reproductive, and family history, and specific questions related to disordered eating. The physical examination should include a pelvic examination, evaluation of secondary sexual characteristics, and laboratory evaluation targeting the most likely causes of symptoms25 (Table 1). Athletes with prolonged oligomenorrhea or amenorrhea lasting for at least six months should undergo bone density evaluation with a dual-energy x-ray absorptiometry (DEXA) scan.26 DEXA screening should also be performed on female athletes who have normal menstrual cycles but have experienced two or more stress fractures.25,27,28
Table 1. Differential Diagnosis of Menstrual Dysfunction
| Condition | Initial laboratory testing |
|---|---|
| Polycystic ovary syndrome | Luteinizing hormone level |
| FSH level | |
| Dehydroepiandrosterone sulfate level | |
| Free and total testosterone levels | |
| Pregnancy | Pregnancy test |
| Premature ovarian failure | FSH level |
| Prolactinoma | Prolactin level |
| Thyroid disease | Thyroid-stimulating hormone level |
FSH = follicle-stimulating hormone.
ACL INJURY
ACL injuries are common in adolescent girls and women, especially in those participating in sports such as soccer and basketball. These are mainly noncontact-type injuries associated with jumping, cutting, and pivoting, and are probably multifactorial in nature. Factors that contribute to ACL injury include lower extremity malalignment, decreased core stability, and muscle strength imbalances (particularly between quadriceps and hamstring muscles).29,30 Hormonal influences may also play a role in these injuries.31 Surgical reconstruction of the torn ACL is usually required, especially if the patient wants to continue to play sports that involve jumping, cutting, or pivoting. Preventive strategies include strength training of the core and lower extremities, proprioceptive training, and exercises to improve jumping, landing, and cutting techniques.32,33
Adults (18 to 49 Years)
Women between the ages of 18 and 49 years experience many of the same conditions as adolescent female athletes, including the female athlete triad, patellofemoral knee pain, and ACL injuries.
PREGNANCY
The American College of Obstetricians and Gynecologists (ACOG) has published guidelines for exercise during pregnancy (Table 2).34,35 ACOG recommends that in the absence of individual contraindications, women should exercise regularly during pregnancy.34,36 Regular exercise during pregnancy is associated with several benefits, including reduced rates of excessive maternal weight gain, gestational diabetes, and preeclampsia. Several studies have found no adverse effects associated with moderate-intensity exercise throughout pregnancy. Few studies, however, have addressed competitive athletics during pregnancy.37 The National Collegiate Athletic Association recently updated its recommendations regarding the participation of pregnant athletes in college sports.38 These guidelines specifically address issues related to the health and safety of pregnant athletes, their return to sport, and issues related to scholarship protection during pregnancy and the postpartum period.
Table 2. Guidelines for Exercise During Pregnancy
| Duration and frequency |
| In the absence of medical or obstetric complications, pregnant women should perform moderate-intensity exercise at least 30 minutes per day on most days of the week |
| Intensity |
| Pregnant women should be advised to participate in exercise of at least moderate intensity (i.e., equivalent in difficulty to brisk walking) |
| Ratings of perceived exertion may be used as an alternative to heart rate monitoring. For moderate exercise, ratings of perceived exertion should be between 12 and 14 (i.e., somewhat hard) on a scale of 6 to 20 |
| Exercise should be performed in a thermoneutral environment or in controlled environmental conditions (e.g., air conditioning). Attention to proper hydration and subjective feelings of heat stress are essential |
| Energy costs of exercise should be estimated and balanced by appropriate energy intake |
| Progression |
| Pregnant women who were sedentary before the pregnancy should gradually progress to 30 minutes of exercise per day |
| Recreation |
| Scuba diving should be avoided throughout pregnancy because of the risk of fetal decompression sickness |
| Type of exercise |
| Aerobic exercise can consist of any activities that use large muscle groups in a continuous, rhythmic manner |
| Physicians should caution pregnant women who engage in activities that increase the risk of falls (e.g., skiing) or that may result in excessive joint stress (e.g., jogging, tennis). However, these activities should be evaluated on an individual basis with consideration for the patient’s abilities |
| Pregnant women should limit repetitive isometric or heavy resistance weightlifting and any exercises that result in a large pressor effect |
PELVIC FLOOR DYSFUNCTION
An estimated 47 percent of women who regularly engage in exercise report some degree of urinary incontinence (mean age, 38.5 years).39 High-impact exercise (e.g., running, aerobics) is associated with more episodes than low-impact exercise, and a significant number of women alter their exercise patterns because of incontinence.39 Even young nulliparous athletes may experience urinary incontinence during exercise. In one study of 156 nulliparous athletes (mean age, 19.9 years), 28 percent noted urine loss while participating in their sport.40 Jumping, high-impact landings, and running were associated with the highest prevalence of urinary incontinence. Mechanical interventions may be helpful, as suggested by a prospective, randomized study that found less urine loss with the placement of a super-absorbency tampon or pessary before exercise.41
Older Adults (50 Years and Older)
Older female athletes share many of the same exercise-related concerns as younger women, but they are more likely to suffer from chronic medical conditions.
DISEASE PREVENTION AND MANAGEMENT
Regular physical activity is associated with a decrease in all-cause mortality rates. It increases bone mineral density, provides cardiovascular protection,27 and contributes to prevention of hypertension42 and diabetes. Exercise is valuable in managing chronic diseases such as hypertension, diabetes, coronary artery disease, dyslipidemia, depression, osteopenia, and osteoporosis.43–47
FALL PREVENTION
Reducing falls in older women is critical to avoid hip fracture and its associated morbidity and mortality. Studies suggest that exercise programs should be multifaceted, targeting strength, flexibility, balance, and overall conditioning. Nevertheless, definitive studies have yet to be performed.48,49 Older athletes can decrease or reverse physiologic changes associated with aging through aerobic, strength, and flexibility training. Exercise can improve postural stability and delay functional disability, thereby reducing fall risk in older women. Physical therapy consultation can target the specific needs of individual patients.50,51

