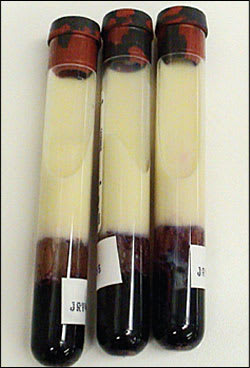
A 44-year-old woman presented to the clinic to establish care. She had a history of hyperlipidemia, type 2 diabetes, childhood polio, and diabetic retinopathy. She had no medical complaints, but admitted that no laboratory testing had been performed recently. At the time of her visit, the patient was fasting. She said that she did not check her blood glucose, exercise, or follow a diabetic diet. A review of her systems was negative, and her vitals were normal. Physical examination revealed obesity, weakness in her right leg secondary to childhood polio, and acanthosis nigricans. Routine laboratory tests were ordered, including complete blood count, comprehensive metabolic panel, lipid level, and urine microalbumin:creatinine ratio. Her blood draw produced white, opaque fluid (see accompanying figure).
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Cryoglobulinemia.
B. Hodgkin lymphoma.
C. Hypertriglyceridemia.
D. Pancreatitis.
E. Sepsis.
Discussion
The answer is C: hypertriglyceridemia. White, opaque serum, along with a history of poorly controlled diabetes and hyperlipidemia, is consistent with severe hypertriglyceridemia. The patient's laboratory results confirmed the diagnosis. Severe hypertriglyceridemia (triglyceride levels greater than 500 mg per dL [5.65 mmol per L])1 may manifest as a grossly lipemic serum sample when levels exceed 1,000 mg per dL (11.30 mmol per L).
The treatment goals for elevated triglyceride levels depend on severity. Usually, the primary goal is to achieve a target low-density lipoprotein (LDL) level that is based on the patient's risk stratification. Dietary modification and weight reduction are recommended for borderline-high triglyceride levels (150 to 199 mg per dL [1.70 to 2.25 mmol per L]). However, when triglyceride levels are high (200 to 499 mg per dL [2.26 to 5.64 mmol per L]), non–high-density lipoprotein cholesterol should be the secondary target of therapy. When triglyceride levels are very high (greater than 500 mg per dL), the primary goal is lowering the triglyceride level to minimize the risk of acute pancreatitis. Recommendations to accomplish this goal include a very low-fat diet (15 percent of total caloric intake), weight reduction, increased physical activity, and pharmacotherapy (e.g., fibrates, nicotinic acid). After triglyceride levels are reduced to less than 500 mg per dL, the focus of treatment returns to LDL reduction to lower the risk of heart disease. Although a combination of statins and fibrates can be used, the risk of myopathy and rhabdomyolysis increases with combination therapy.2 Fenofibrate (Tricor) has a lower risk of myopathy than gemfibrozil (Lopid).2
Cryoglobulinemia is the presence of cryoglobulins in the serum, which leads to a systemic inflammatory syndrome caused by cryoglobulin-containing immune complexes. To confirm the diagnosis, a blood sample must be collected in a warm tube without anticoagulants. The sample should clot before removing the serum via centrifugation. The subtypes of cryoglobulinemia vary in concentration and length of time for precipitation. Cryoglobulinemia does not cause lipemic serum.
Hodgkin lymphoma is a malignancy of lymphatic tissue. Reed-Sternberg cells are present in a background of reactive leukocytes or fibrosis.3 Patients with lymphoma and a triglyceride level greater than 200 mg per dL may develop chylous ascites (milky white ascitic fluid), a rare but well-reported complication.4 However, these patients do not have white, opaque serum.
Pancreatitis is an inflammatory and life-threatening condition that may be caused by gallstones, alcoholism, medications, elevated triglyceride levels, or malignancy. Pancreatitis manifests as multiple systemic and metabolic findings and is generally treated with supportive measures. Acute pancreatitis may cause chylous ascites.5 Pancreatitis with severe hypertriglyceridemia can lead to lipemia.
With sepsis, a systemic infection is followed by a systemic inf lammatory response. Typically, patients are febrile, hypotensive, tachycardic, and tachypneic. Treatment involves hemodynamic support, especially fluid resuscitation; antimicrobials; and other therapies, based on the patient's condition. White, opaque serum is not consistent with sepsis unless hypertriglyceridemia is also present.
Summary Table
| Condition | Characteristics |
|---|---|
| Cryoglobulinemia | Presence of cryoglobulins in serum, leading to an inflammatory response; not associated with white, opaque serum |
| Hodgkin lymphoma | Malignancy of lymphatic tissue; patients with coexisting hypertriglyceridemia may have chylous ascites |
| Severe hypertriglyceridemia | Elevated triglyceride level (generally greater than 500 mg per dL [5.65 mmol per L]) required fordiagnosis of severe hypertriglyceridemia; lipemic serum may be present with levels greater than 1,000 mg per dL (11.30 mmol per L) |
| Pancreatitis | Inflammatory condition caused by gallstones, alcoholism, medications, elevated triglyceride levels, or malignancy; may lead to chylous ascites; patients with coexisting hypertriglyceridemia may have lipemic serum |
| Sepsis | Systemic infection and inflammatory response; does not cause white, opaque serum unless hypertriglyceridemia is also present |

