A 24-year-old man sustained penetrating soft tissue injuries just distal to the center of the medial right forearm. Surgery was performed immediately to stabilize his wounds and later to reattach the tendons of his forearm.
The patient had sensory loss to his hand but denied any pain. Motor examination revealed that he had the ability to pronate and supinate the forearm; flex and extend the wrist; and form a normal “OK” sign, with his thumb and index finger pinched together. Figure 1 demonstrates the patient's attempt to actively open his hand and extend the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and distal interphalangeal (DIP) joints of his dominant right hand. Figure 2 shows the patient's hands at rest.
Figure 1.
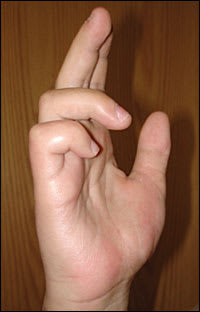
Figure 2.
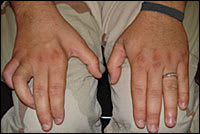
Question
Based on the patient's history and physical examination, which one of the following nerves was most likely injured?
A. Anterior interosseous nerve.
B. Median nerve.
C. Posterior interosseous nerve.
D. Radial nerve.
E. Ulnar nerve.
Discussion
The answer is E: ulnar nerve. The patient has the typical presentation of a clawhand, with injury to the ulnar nerve in the forearm. The ulnar nerve originates from the brachial plexus and contains motor and sensory fibers from the C8 and T1 roots.1, 2 It innervates many intrinsic muscles of the hand, as well as extrinsic muscles for flexion of the ring and little fingers to allow for the power grip.3 When the patient extends his fingers, the MCP, PIP, and DIP joints remain flexed. The MCP joints flex with passive pull of the denervated medial half of the flexor digitorum profundus muscle, whereas the DIP and PIP joints remain in flexion because of paralysis of the medial lumbrical muscles. Sensory loss is noted in palmar and distal dorsal surfaces of the little finger and in the medial half of the ring finger. Muscle wasting and atrophy of the first dorsal interosseous muscle are present (Figure 3).
Figure 3.
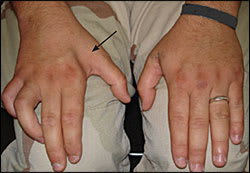
Muscle wasting and atrophy (arrow) in a patient with ulnar nerve injury to the forearm.
Traumatic injury is the most common cause of ulnar nerve damage,4 although leprosy is associated with ulnar nerve lesions. First-degree injury (neurapraxia) is usually reversible within two to three months. Second-degree injury (axonotmesis) involves axon degeneration distal to the injury site. Recovery is possible, with recovery time dependent on the distance from the injury to the end organ. Third-degree injury (neurotmesis) involves complete disruption of the nerve with little potential for recovery.1
The anterior interosseous nerve is a branch of the median nerve. It innervates the flexor pollicis longus, the lateral half of the flexor digitorum profundus, and the pronator quadratus muscles. Persons with injury to the anterior interosseous nerve are unable to form a normal “OK” sign.
The median nerve innervates the thenar compartment, allowing for fine control of the pincer grip.2,3 Damage to the median nerve causes motor and sensory loss to the thumb, index finger, and middle finger. The clinical picture is similar to that of ulnar nerve injury, except in presentation when the patient attempts to close the hand, rather than open it. The unopposed action of the extensors of the index and middle fingers prevents full flexion as the ring and little fingers flex normally. Disruption of the flexor digitorum profundus muscle (innervated by the median nerve laterally) causes benediction hand.
The posterior interosseous nerve, the deep branch of the radial nerve, is a purely motor nerve. It innervates the extensor muscles of the wrist, hand, thumb, and index finger. Damage to the posterior interosseous nerve leads to the inability to extend the wrist, or wristdrop, without sensory loss to the dorsum of the hand.
The radial nerve divides into the superficial and the deep branch (posterior interosseous nerve) at the lateral epicondyle. The superficial branch is a purely sensory nerve. Injury to the superficial branch causes sensory loss in the dorsum of the hand without motor deficits.2 Injury proximal to the branching leads to wristdrop and sensory loss.
Summary Table
| Injured nerve | Characteristics |
|---|---|
| Anterior interosseous | Inability to form the “OK” sign normally, with the thumb and index finger pinched together; weakened pronation |
| Median | Thenar eminence wasting; sensory loss to the thumb, index finger, and middle finger; benediction hand |
| Posterior interosseous | Inability to extend the wrist (wristdrop) without sensory loss to the dorsum of the hand |
| Radial | Wristdrop with sensory loss to the dorsum of the hand |
| Ulnar | Clawhand; motor deficits of the intrinsic muscles of the hand; first dorsal interosseous wasting; hypothenar eminence wasting |

