Pneumonia is an important cause of morbidity and mortality in nursing home residents, with 30-day mortality rates ranging from 10 to 30 percent. Streptococcus pneumoniae is the most common cause of nursing home–acquired pneumonia, although Staphylococcus aureus and gram-negative organisms may be more common in severe cases. Antibiotic therapy for nursing home–acquired pneumonia should target a broad range of organisms, and drug-resistant microbes should be considered when making treatment decisions. In the nursing home setting, treatment should consist of an antipneumococcal fluoroquinolone alone or either a high-dose beta-lactam/beta-lactamase inhibitor or a second- or third-generation cephalosporin, in combination with azithromycin. Treatment of hospitalized patients with nursing home–acquired pneumonia requires broad-spectrum antibiotics with coverage of many gram-negative and gram-positive organisms, including methicillin-resistant S. aureus. Appropriate dosing of antibiotics for nursing home–acquired pneumonia is important to optimize effectiveness and avoid adverse effects. Because many nursing home residents take multiple medications, it is important to consider possible drug interactions.
Pneumonia is the second most common cause of infection in nursing home residents, and is associated with notable morbidity and mortality.1 Attributable 30-day mortality rates range from 10 to 30 percent.2–4 Prompt diagnosis and management are therefore essential. This article reviews the clinical management of nursing home–acquired pneumonia, with an emphasis on antimicrobial therapy.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should suspect infection with resistant organisms in nursing home patients who received antibiotics within the previous 90 days; when there is a high incidence of antibiotic resistance in the community or facility; and in patients who receive chronic dialysis, are immunosuppressed, or have difficulty performing activities of daily living. | B | 7, 11 |
| Nursing home–acquired pneumonia should be suspected in patients with new or progressive infiltrate plus a new-onset fever, leukocytosis, purulent sputum, or hypoxia. | C | 7 |
| Nonhospitalized nursing home patients requiring treatment for pneumonia should be treated with an antipneumococcal fluoroquinolone, or either a high-dose beta-lactam/beta-lactamase inhibitor or a second- or third-generation cephalosporin, in combination with azithromycin (Zithromax). | C | 1, 31, 32 |
| Empiric coverage of methicillin-resistant Staphylococcus aureus and double coverage of Pseudomona pneumonia should be prescribed for patients requiring intensive care unit admission. | B | 5–7 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Etiology
Nursing home–acquired pneumonia is usually bacterial in origin, although the specific microbiologic cause is often not identified.5–12 Common bacterial etiologies are listed in Table 1.5–12 Streptococcus pneumoniae is the most common causative agent. However, in severe cases of nursing home–acquired pneumonia requiring hospitalization and mechanical ventilation, the rates of infection with Staphylococcus aureus and enteric gram-negative organisms appear to exceed those of S. pneumoniae.5
Table 1 Common Etiologies of Nursing Home–Acquired Pneumonia
These organisms can be associated with antimicrobial resistance, especially in the nursing home setting. Risk factors for infection with multidrug-resistant pathogens include antibiotic therapy within the preceding 90 days, a high incidence of antibiotic resistance in the community or facility, chronic hemodialysis, and immunosuppression.7 One study found that recent antibiotic use and the inability to perform activities of daily living were independently associated with antibiotic-resistant nursing home–acquired pneumonia requiring intensive care unit (ICU) admission or mechanical ventilation.11
Nursing home–acquired pneumonia can also be caused by viral infection (Table 15–12). Influenza and respiratory syncytial virus (RSV) are important causes of respiratory illness and mortality in nursing home residents.13,14 Physicians should suspect viral etiologies from late fall through early spring, and whenever outbreaks of respiratory infection occur. Influenza predisposes patients to a secondary bacterial pneumonia.15 In a population-based analysis involving 381 nursing homes over a period of four years, investigators found that each year influenza infection was associated with approximately 28 hospitalizations; 147 courses of antibiotics; and 15 deaths per 1,000 residents with heart or lung disease, diabetes mellitus, or immunosuppression. Similarly, RSV accounted for approximately 15 hospitalizations, 76 courses of antibiotics, and 17 deaths per 1,000 residents with similar conditions.13 A recent report described human metapneumovirus as the cause of an outbreak of respiratory infections, including pneumonia, in a Canadian nursing home.16
Diagnosis
The clinical manifestations of pneumonia in older adults may be subtle. In one study, investigators found that persons 65 years and older are less likely to complain of fever, chills, myalgia, and pleuritic chest pain than younger persons.17 One prospective study revealed that 80 percent of nursing home residents with pneumonia exhibit three or fewer respiratory signs or symptoms, but 92 percent have at least one identifiable respiratory manifestation, such as cough, respiratory rate of 30 breaths per minute or more, presence of crackles, or absence of wheezes on auscultation.18 The 2005 American Thoracic Society/Infectious Diseases Society of America (ATS/IDSA) guideline recommends that the clinical diagnosis of health care–associated pneumonia, including nursing home–acquired pneumonia, be based on a new or progressive infiltrate on chest radiography plus clinical findings consistent with pneumonia (i.e., new-onset fever [temperature greater than 100.4° F (38° C)], leukocytosis, purulent sputum, or hypoxia).7
The 2005 ATS/IDSA guideline also recommends that lower respiratory tract samples be obtained from nursing home residents hospitalized with nursing home–acquired pneumonia, particularly from those who are intubated, to guide treatment.7 Although respiratory cultures from nonintubated patients, and from those managed in the nursing home, could be considered, it is important to note that these are infrequently obtained, tend to produce a low yield of pathogenic microorganisms, and are commonly contaminated with oropharyngeal microflora, making interpretation difficult.19,20
Blood cultures are infrequently positive in patients with pneumonia, but may be considered in those who require intensive care. Rapid antigen tests of respiratory secretions, such as nasal washings, nasopharyngeal swabs, or throat swabs, can assist with the diagnosis of influenza and RSV during the appropriate seasons.21 Urinary antigen testing for S. pneumoniae and Legionella pneumophila serotype 1 may be considered, although most studies examining its use have been performed in patients with community-acquired pneumonia (CAP).22–26 One limitation of urinary antigen testing is the lack of information about antibiotic susceptibility. Therefore, a sputum Gram stain and culture should be considered if patients are able to generate a useful sample and the results can be obtained in time to influence therapeutic decision-making.21
In many nursing home residents with pneumonia, a diagnosis of aspiration pneumonitis or aspiration pneumonia should be considered. Aspiration pneumonitis is an inflammatory syndrome that does not typically require antibiotic therapy,27 whereas aspiration pneumonia is an infection for which antibiotic therapy should be initiated. Risk factors for these conditions include a history of stroke, dementia, gastroesophageal reflux disease, and tube-feeding requirements. Pathogens isolated from nursing home patients with severe aspiration pneumonia have included enteric gram-negative bacteria, S. aureus, and anaerobes.6 The results of a recent prospective cohort study validated a new algorithm for diagnosis of aspiration pneumonitis versus aspiration pneumonia (Figure 1).28
Figure 1. Evaluation of Suspected Aspiration Pneumonia
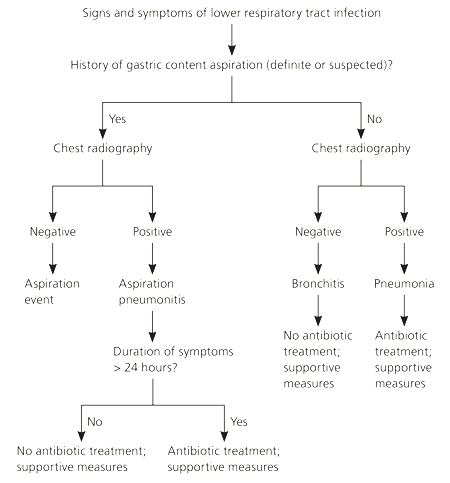
Algorithm for the evaluation of suspected aspiration pneumonia.
Adapted with permission from Mylotte JM, Goodnough S, Gould M. Pneumonia versus aspiration pneumonitis in nursing home residents: prospective application of a clinical algorithm. J Am Geriatr Soc. 2005;53(5):756.
Treatment
IN THE NURSING HOME SETTING
There is little evidence to suggest the clinical superiority of one antibiotic over another for nursing home–acquired pneumonia, particularly in the nursing home setting. Previous guidelines have recommended antibiotic therapy based primarily on microbiologic data.7,29,30
The 2005 ATS/IDSA guideline for the treatment of health care–associated pneumonia does not specifically address treatment of nursing home–acquired pneumonia in the nursing home setting.7 Guidelines based on limited data and expert opinion recommend the use of an antipneumococcal fluoroquinolone (e.g., levofloxacin [Levaquin] or moxifloxacin [Avelox]) alone or either a high-dose beta-lactam/beta-lactamase inhibitor (e.g., amoxicillin/clavulanate [Augmentin]) or a second- or third-generation cephalosporin (e.g., cefuroxime [Ceftin], cefpodoxime [Vantin], ceftriaxone [Rocephin]), in combination with azithromycin (Zithromax). Oral therapy is preferred over parenteral therapy in mild to moderate cases.29,30 Intramuscular cephalosporins also may be used.1,31
A randomized, double-blind trial compared the safety and effectiveness of once-daily intramuscular injections of cefepime (Maxipime) and ceftriaxone for nursing home–acquired pneumonia treated within the nursing home. Sixty-nine residents 60 years and older with radiographically-confirmed pneumonia and creatinine clearances of less than 60 mL per minute were included in the study. Most patients were switched to oral therapy after three days of parenteral therapy. Successful response was documented in 78 percent of patients treated with cefepime and 66 percent of patients treated with ceftriaxone (P = not significant).32 Each year, the Centers for Disease Control and Prevention (CDC) recommendations for influenza treatment should be consulted for updates on recent resistance patterns and treatment or prevention recommendations.
When a viral etiology of nursing home–acquired pneumonia is diagnosed and there is low suspicion of secondary bacterial infection, antibiotics often can be discontinued. However, it should be noted that older patients with influenza are at high risk of bacterial superinfection. Oseltamivir (Tamiflu) and zanamivir (Relenza) are approved for the treatment of influenza A and B in adults, but therapy should begin within two days of symptom onset to confer the most benefit, and increasing resistance to oseltamivir has recently been reported.33 These agents may lessen the severity of influenza manifestations and may reduce the incidence of post-influenza bacterial pneumonia.34
Influenza vaccination is recommended for the prevention of influenza in nursing home residents, but does not provide complete protection.34 Similarly, pneumococcal vaccination is recommended for all nursing home patients in accordance with the latest CDC guidelines for the prevention of pneumococcal pneumonia.35 Oseltamivir should be used prophylactically when an outbreak of influenza A or B occurs within a nursing home.34 There are no data to support specific treatments for RSV and human metapneumovirus in nursing home residents.36
IN HOSPITALIZED PATIENTS
Intravenous antimicrobial therapy should be initiated for nursing home patients hospitalized with pneumonia, with empiric coverage of methicillin-resistant S. aureus (MRSA) and Pseudomonas aeruginosa. Antibiotic coverage of atypical organisms is controversial, and there are no data to support such therapy. If an etiologic agent is identified, antibiotic therapy should be narrowed to minimize antibiotic resistance, toxicity, and cost. Hospitalized patients are more likely to have drug-resistant and highly pathogenic organisms.5–7,11 Antibiotics administered in the past 90 days generally should not be prescribed again, because the risk of infection with resistant pathogens is increased.37
Nursing home residency is a major risk factor for MRSA colonization, which can lead to subsequent infection. Rates of MRSA from six nursing homes and one skilled-nursing facility in the United States ranged from 24 to 77 percent.38–40 Vancomycin (Vancocin; given intravenously) and linezolid (Zyvox; given orally or intravenously) are recommended for the treatment of MRSA pneumonia.7,41
Risk factors for pneumonia caused by P. aeruginosa were identified in a study of 559 cases of CAP, including 45 cases of nursing home–acquired pneumonia. They include hospitalization within the previous 30 days or pulmonary comorbid illness (e.g., chronic obstructive pulmonary disease, asthma, chronic bronchitis, bronchiectasis, interstitial lung disease).42 When choosing antipseudomonal agents, the physician should refer to local pseudomonal susceptibility patterns.
One prospective, randomized trial compared the effectiveness of cefepime, with or without metronidazole (Flagyl), versus ertapenem (Invanz) for hospital- or skilled facility–acquired pneumonia in nonventilated, non-ICU patients.43 The addition of vancomycin was permitted for patients with suspected MRSA infection. Enterobacteriaceae, S. pneumoniae, and S. aureus comprised 19.5, 12.9, and 11.6 percent of the pathogens recovered, respectively. Forty percent of the S. aureus isolates were methicillin-resistant. Outcomes were similar; 87.3 percent of patients who received ertapenem and 86.0 percent of patients who received cefepime improved.
For hospitalized patients with nursing home–acquired pneumonia, the 2005 ATS/IDSA guideline7 recommends a combination antibiotic therapy consisting of the following:
- An antipseudomonal cephalosporin, an antipseudomonal carbapenem, or an extended-spectrum beta-lactam/beta-lactamase inhibitor
plus
- An antipseudomonal fluoroquinolone or an amino-glycoside
plus
- An anti-MRSA agent (vancomycin or linezolid).
The broad empiric therapy includes coverage of MRSA and double-coverage of P. aeruginosa. Specific antibiotics and recommended dosages are provided in (Table 2).7 These recommendations are based on microbiologic data from patients with severe pneumonia. Treatment should be tailored to the local microbiology, resistance patterns, and specific patient risk factors.7 Aminoglycoside use increased mortality in a retrospective review.44 If chosen as therapy, aminoglycosides should be used with caution in patients with impaired renal function. Tigecycline (Tygacil) and doripenem (Doribax) are newer antibiotics being investigated in the treatment of health care–associated pneumonia, but they are not approved by the U.S. Food and Drug Administration for this indication. These medications may play a role in the treatment of hospitalized patients with nursing home–acquired pneumonia in the near future.
Table 2 Initial Intravenous, Adult Doses of Antibiotics for Empiric Therapy of Hospital-Acquired Pneumonia, Including Ventilator-Associated Pneumonia, and Healthcare–Associated Pneumonia in Patients with Late-Onset Disease or Risk Factors for Multidrug–Resistant Pathogens
| Antibiotic | Dosage* | |
|---|---|---|
| Antipseudomonal cephalosporin | ||
| Cefepime | 1–2 g every 8–12 h | |
| Ceftazidime | 2 g every 8 h | |
| Carbapenems | ||
| Imipenem | 500 mg every 6 h or 1 g every 8 h | |
| Meropenem | 1 g every 8 h | |
| β-lactam/β-lactamase inhibitor | ||
| Piperacillin–tazobactam | 4.5 g every 6 h | |
| Aminoglycosides | ||
| Gentamicin | 7 mg/kg per d† | |
| Tobramycin | 7 mg/kg per d† | |
| Amikacin | 20 mg/kg per d† | |
| Antipseudomonal quinolones | ||
| Levofloxacin | 750 mg every d | |
| Ciprofloxacin | 400 mg every 8 h | |
| Vancomycin | 15 mg/kg every 12 h‡ | |
| Linezolid | 600 mg every 12 h | |
*— Dosages are based on normal renal and hepatic function.
†— Trough levels for gentamicin and tobramycin should be less than 1 μg/ml, and for amikacin they should be less than 4–5 μg/ml.
‡— Trough levels for vancomycin should be 15–20 μg/ml.
Reprinted with permission from American Thoracic Society; Infectious Diseases Society of America. Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia. Am J Respir Crit Care Med. 2005;171(4):402.
Pharmacotherapeutics
TIMING AND DURATION OF ANTIBIOTIC THERAPY
The timing of initiation of antibiotic therapy in hospitalized patients with nursing home–acquired pneumonia may be an important predictor of outcome.45 Therapy given within four hours of admission was associated with decreased length of stay and decreased mortality in one retrospective study, and is an important outcome measure for the Centers for Medicare and Medicaid Services.45,46 However, other studies have not demonstrated a survival benefit or a more rapid clinical response.47,48 The 2007 IDSA/ATS guideline recommends initiation of antibiotic therapy for CAP within the emergency department or as soon as possible after the diagnosis is made, rather than within a specified time period.21 Although no studies have specifically measured outcomes for nursing home patients, similar recommendations apply to this population.
The IDSA/ATS guideline recommends a seven-to eight-day duration of therapy for health care–associated pneumonia that has been treated with appropriate empiric antibiotics, has clinically improved, and that is not caused by nonfermenting gram-negative bacteria such as P. aeruginosa.7
DOSING OF ANTIBIOTICS IN THE NURSING HOME PATIENT
Critically ill patients often have altered pharmacokinetics and pharmacodynamics, and antibiotics must be dosed more aggressively than in other patients.49 Empiric antibiotics in critically ill patients with nursing home–acquired pneumonia should be dosed as outlined in Table 2.7 As renal function declines with age, proper dosing of antibiotic agents must be ensured to avoid adverse effects.50 The Cockcroft-Gault equation is commonly used to estimate creatinine clearance; manufacturers generally use this equation to estimate creatinine clearance when making recommendations about drug dosing in patients with renal insufficiency. Aminoglycosides, which can cause nephro- and ototoxicity, and imipenem/cilastatin (Primaxin), which can cause seizures, should be avoided in older patients with renal impairment.
Vancomycin dosing should be optimized to maintain trough concentrations in the range of 15 to 20 mcg per mL.7 However, a retrospective review of patients with MRSA pneumonia did not demonstrate any correlation between serum vancomycin trough concentrations and mortality.51
ADVERSE EFFECTS OF ANTIMICROBIAL AGENTS IN OLDER ADULTS
Adverse drug events are more likely to occur in older adults than in other patients.50 The safest and most effective medication should be prescribed in an appropriate dose for the shortest duration possible to adequately treat the infection. In a study of nursing home patients, use of antibiotics was associated with preventable adverse drug reactions (Table 350).52
Table 3 Adverse Effects of Antibiotics in Older Patients
| Antimicrobial class/agent | Adverse event |
|---|---|
| Aminoglycosides | Nephrotoxicity, ototoxicity |
| Beta-lactams | Diarrhea, Clostridium difficile–associated disease, drug-related fever, interstitial nephritis, rash, thrombocytopenia, anemia, neutropenia |
| Clindamycin (Cleocin) | Diarrhea, C. difficile–associated disease |
| Fluoroquinolones | Nausea, vomiting, central nervous system effects, decreased seizure threshold, QT prolongation |
| Imipenem/cilastatin (Primaxin) | Seizure |
| Linezolid (Zyvox) | Thrombocytopenia, anemia |
| Macrolides | Gastrointestinal intolerance |
Adapted with permission from Faulkner CM, Cox HL, Williamson JC. Unique aspects of antimicrobial use in older adults. Clin Infect Dis. 2005;40(7):1002.
DRUG INTERACTIONS WITH ANTIMICROBIAL AGENTS IN OLDER ADULTS
Increasing age is associated with an increasing number of medications used on a daily or weekly basis.53 Up to 67 percent of nursing home patients will experience an adverse drug reaction during a six- to 12-month stay, and use of more than eight medications is associated with increased rates of adverse drug reactions.54 Because of the large number of medications prescribed in nursing home patients, the potential for drug interactions is very high. Table 4 lists some common drug interactions with which prescribers should be familiar.50 Most antibiotics alter the anticoagulant effects of warfarin (Coumadin), primarily by increasing these effects. All patients concurrently taking antibiotics and warfarin should have their International Normalized Ratio monitored closely during antibiotic therapy.
Table 4 Selected Drug Interactions of Common Antibiotics
| Antimicrobial class/agent(s) | Interacting agents | Potential clinical effect |
|---|---|---|
| Aminoglycosides | Loop diuretics, nonsteroidal anti-inflammatory drugs, vancomycin (Vancocin) | Additive nephrotoxicity |
| Azithromycin (Zithromax) | Warfarin (Coumadin) | Increased anticoagulant effect (minor) |
| Fluoroquinolones | Aluminum, magnesium, iron, zinc, calcium, sucralfate (Carafate) | Decreased absorption |
| Class IA and III antiarrhythmics | QT prolongation, arrhythmia | |
| Warfarin | Increased anticoagulant effect | |
| Linezolid (Zyvox) | Serotonergic agents (selective serotonin reuptake inhibitors, tricyclic antidepressants, monoamine oxidase inhibitors, tramadol [Ultram]) | Serotonin syndrome |
| Metronidazole (Flagyl) | Warfarin | Increased anticoagulant effect (major) |
| Trimethoprim/sulfamethoxazole | Phenytoin (Dilantin) | Increased concentration of phenytoin |
| Warfarin | Increased anticoagulant effect (major) |
Adapted with permission from Faulkner CM, Cox HL, Williamson JC. Unique aspects of antimicrobial use in older adults. Clin Infect Dis. 2005;40(7):1001.

