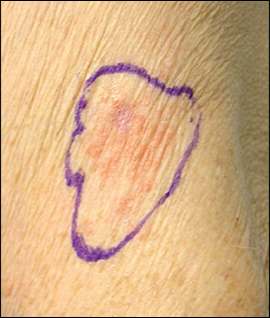
An 89-year-old patient presented with an asymptomatic lesion on her left proximal arm at the site of a childhood vaccination scar. The lesion had persisted for one and a half years. Physical examination revealed a 3.7-cm × 2.9-cm erythematous, ill-defined plaque with thin, overlying scale (see accompanying figure). There was no axillary lymphadenopathy. A full skin examination, including the oral mucosa, was otherwise unremarkable. Results of a potassium hydroxide preparation of a skin scraping were negative.
Question
Based on the patient's history and physical examination, which one of the following is the most appropriate next step?
A. Intralesional steroid.
B. Skin biopsy.
C. Topical antifungal.
D. Topical emollient (e.g., petroleum jelly).
E. Topical steroid.
Discussion
The answer is B: skin biopsy. There are a number of diseases that can lead to red plaques. However, a solitary, changing skin lesion occurring in a vaccination scar is highly suggestive of cutaneous malignancy and warrants a skin biopsy. In this patient, the histologic features are consistent with lentigo maligna melanoma, amelanotic type. Skin lesions not related to vaccines typically lead to more than one lesion in a characteristic distribution.
Although vaccination plays a significant role in disease prevention and maintenance of public health, rare adverse events (e.g., vaccine-associated malignancy) may occur. Basal cell carcinoma is the most commonly reported neoplastic proliferation in vaccination scars and has occurred with smallpox and bacille Calmette-Guérin (BCG) vaccines.1-2 Squamous cell carcinoma,1-2 melanoma,1 dermatofibrosarcoma protuberans,3 and malignant fibrous histiocytoma4 have also been reported in vaccination scars. It is impossible to draw conclusions about predominance in males versus females, age of presentation, and incidence of vaccination because few cases have been reported.5
Although the pathogenesis remains unknown, vaccine-associated malignancies (e.g., Marjolin ulcer, squamous cell carcinoma) may be secondary to chronic inflammation. Although the smallpox and BCG vaccines are live, a component of the vaccines may cause prolonged inflammation. Additionally, the route of administration may contribute to carcinogenesis. Unlike other vaccines, smallpox vaccines are administered by scarification and BCG vaccines by intradermal injection.6 These routes may introduce keratin intradermally, causing a subsequent foreign body granuloma.
Vaccine-associated feline sarcoma may provide insight into the pathogenesis of vaccine-associated malignancies in humans.7 Studies suggest that persistent inflammation from vaccine adjuvants, such as aluminum, is the major factor for carcinogenesis in vaccine-associated feline sarcoma. Epidemiologic evidence supports both a causal and a dose-response relationship between adjuvanted vaccines and development of sarcoma at the vaccination site.
The diagnosis of a skin lesion in a vaccination scar should be confirmed with skin biopsy. Treatment goals depend on the type of cutaneous malignancy diagnosed. The posttreatment course should include periodic skin examinations for tumor recurrence and new primary skin cancers.
A topical emollient (e.g., petroleum jelly) is appropriate for moisturization of xerosis (dry skin). The use of steroids should be restricted to inflammatory skin conditions. Topical antifungal medications are used for dermatophyte infections.
Selected Differential Diagnosis of Red Plaques
| Condition | Characteristics |
|---|---|
| Actinic keratosis | Red, poorly defined papules and plaques with adherent scale; usually involves multiple lesions in sun-exposed areas |
| Lichen planus | Violaceous, polygonal papules and plaques with overlying fine white lines (Wickham striae); usually involves the wrists, lower back, and ankles |
| Nummular eczema | Pruritic, scaly, erythematous patches and plaques affecting numerous body surfaces; often occurs with xerosis (dry skin) |
| Psoriasis | Well-circumscribed, salmon-colored plaques that bleed when the overlying silver-to-white scale is peeled from the plaque (Auspitz sign); usually involves areas of friction (e.g., elbows, knees, umbilicus, gluteal cleft) |
| Tinea | Mildly pruritic, scaly, oval-to-round, red patches; common in body folds; diagnosis is confirmed with microscopy or culture of skin scrapings |

