A 32-year-old man presented for an evaluation of his cervical spine to determine whether he had the same congenital anomaly that had been diagnosed in his three-year-old daughter; his daughter required surgery. The man was asymptomatic and had no other medical problems. He denied neck pain, upper and lower extremity numbness or weakness, and bowel or bladder changes. His vital signs were normal. He had full range of motion of his cervical spine with no pain, normal upper and lower extremity strength and sensation, and normal reflexes throughout. Cervical flexion and extension radiography were performed (Figures 1 and 2).
Figure 1
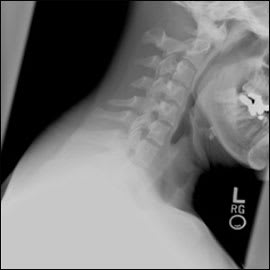
Figure 2
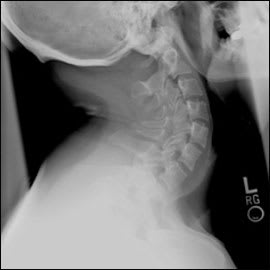
Question
Based on the patient's history, physical examination, and radiographic findings, which one of the following is the most likely diagnosis?
A. Atlantooccipital fusion.
B. Flexion teardrop fracture.
C. Fracture of C1 (Jefferson fracture).
D. Nonfusion of the posterior arch of the atlas.
E. Wedge fracture of the cervical vertebrae.
Discussion
The answer is D: nonfusion of the posterior arch of the atlas. Radiography confirms non-fusion of the posterior arch of C1 (Figure 3). Generally, this rare congenital anomaly is an incidental finding in asymptomatic patients. In a trauma setting, the anomaly may be mistaken for a fracture if there are no prior films for comparison.
Figure 3.
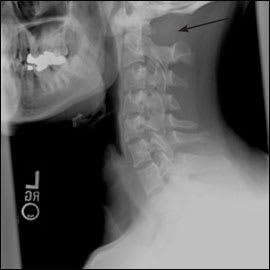
Radiograph showing nonfusion of the posterior arch of C1 (arrow).
Ossification of the posterior arch of the atlas normally begins during the seventh week of gestation. Complete ossification and fusion occur between three and five years of age. When this process is disrupted, nonfusion of the arch results.1 Nonfusion of the posterior arch is in the same spectrum as congenital absence of the posterior arch, which involves a complete failure of cartilage formation during the chondrification stage.2
Patients with posterior arch abnormalities are usually asymptomatic, although some may present with neck pain. Dense, fibrous bands bridge the bony gap, stabilizing the cervical spine. Some patients have atlantoaxial instability and neurologic deficits from cord impingement by a remnant of the posterior arch.3
Computed tomography (CT) can confirm ossification of the posterior arch of the atlas. Magnetic resonance imaging is required in patients with neurologic deficits. Treatment depends on presenting symptoms and radiographic findings. Although no treatment is needed for asymptomatic patients, surgery is warranted in patients with atlantoaxial instability or nerve compression.
Atlantooccipital fusion is partial or complete fusion of the atlas and base of the occiput. It is commonly associated with congenital fusion of C2 and C3. Approximately one half of patients with atlantooccipital fusion develop instability.4 Affected patients may have headache, neck pain, limb numbness and pain, weakness, tinnitus, visual disturbances, and dysphagia or dysarthria from cranial nerve palsies.5
A flexion teardrop fracture is a fracture-dislocation and one of the most unstable types of cervical spine fractures. This injury is caused by combined flexion and compression forces and must be distinguished from a small anterior-inferior avulsion fracture.
A Jefferson fracture of the C1 vertebra is usually caused by axial loading of the cervical spine or hyperextension of the neck. Patients often present with neck pain, normal range of motion, and a normal neurologic examination. An open-mouth odontoid radiograph may show lateral displacement of the lateral masses of C1 on C2. This finding suggests an unstable fracture caused by transverse ligament disruption. Additional imaging with CT and referral are warranted.6
Wedge fractures of the cervical spine may occur with flexion and axial loading forces. In a simple wedge fracture, the anterior body end plate is compressed, but the height of the posterior vertebral cortex is usually preserved. The wedge fracture is a stable fracture usually not associated with neurologic compromise. Initial management involves a cervical collar worn until the neck is no longer tender, about two to four weeks.4
Selected Differential Diagnosis of Cervical Spine Anomaly
| Condition | Characteristics |
|---|---|
| Atlantooccipital fusion | Partial or complete fusion of the atlas and base of the occiput; headache, neck pain, limb numbness and pain, weakness, tinnitus, visual disturbances, and dysphagia or dysarthria may occur |
| Flexion teardrop fracture | One of the most unstable types of cervical spine fractures; caused by combined flexion and compression forces |
| Jefferson fracture | Fracture of C1; usually caused by axial loading or hyperextension of the neck, resulting in a bilateral burst through the posterior arch and lateral masses; patients present with neck pain, normal range of motion, and a normal neurologic examination |
| Nonfusion of the posterior arch of the atlas | Mostly asymptomatic, although neck pain may occur; atlantoaxial instability and neurologic deficits are possible from cord impingement by a remnant of the posterior arch |
| Wedge fracture | Stable cervical fracture from flexion and axial loading of the neck; anterior vertebral body is compressed with no neurologic compromise; cervical orthosis used for management |

