A woman presented with a rash on her neck that had persisted for two days. The rash began as tiny, red, pruritic, painful vesicles under the angle of her left jaw. Within a few hours, the rash had spread to her entire neck. She had a mild fever, but no other notable symptoms. The patient denied any contact with topical medications or allergens. She had a history of atopic dermatitis and bronchial asthma, which were well controlled with medications. Physical examination revealed multiple erythematous, crusted, monomorphous papules (Figures 1 and 2).
Figure 1.
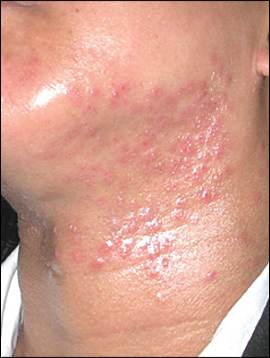
Figure 2.
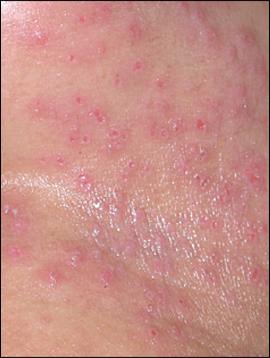
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Acne conglobata.
B. Acute contact dermatitis.
C. Eczema herpeticum.
D. Eosinophilic folliculitis.
E. Molluscum contagiosum.
Discussion
The answer is C: eczema herpeticum. Eczema herpeticum (Kaposi varicelliform eruption) is a herpes simplex virus (HSV) infection. The condition usually occurs in persons with atopic dermatitis, but eczema herpeticum can be used to describe any disseminated skin condition with HSV infection. Eczema herpeticum may cause recurrent skin infections, possibly reflecting a local defect in T cell function. Early onset of atopic dermatitis and elevated immunoglobulin E levels increase the risk of eczema herpeticum.1
Complications of eczema herpeticum vary from a mild outbreak to a fatal reaction. The rash typically begins with small, isolated vesicles that abruptly group over an area of eczematous skin. Newer vesicles continue to appear in monomorphic crops for about one week. The lesions have a central umbilication, but quickly become hemorrhagic, crusted, and eroded.2
Eczema vaccinatum is a severe, widespread eruption that may be similar in appearance to eczema herpeticum. The condition occurs in persons with atopic dermatitis after smallpox vaccination or exposure to others who have been vaccinated.
If standard antibiotic treatment fails in patients with atopic dermatitis and cutaneous infection, culture for bacterial and viral etiology should be performed. Giemsa stain can confirm eczema herpeticum using a smear taken from the floor of a freshly opened, early vesicle. Tzanck testing cannot differentiate HSV type 1, HSV type 2, and varicella-zoster virus; therefore, viral culture is recommended for diagnosis. HSV can be identified with direct immunofluorescence or molecular diagnostic testing. In addition, herpes simplex DNA can be extracted and amplified with polymerase chain reaction using stained and unstained Tzanck smears, crusts, fresh tissue, and paraffin sections of suspected lesions.3
After the diagnosis is confirmed, systemic antiviral therapy should be initiated. If the rash is limited to the skin, oral acyclovir (Zovirax) is the treatment of choice.4 Intravenous treatment may be necessary in patients with severe, disseminated eczema herpeticum.
Acne conglobata is a severe form of acne. It is more common in boys and persons living in tropical climates. Patients typically present with inflammatory nodules and pseudocysts with marked scarring on the face, sternum, or back.
Irritants, such as soaps and detergents, cause 80 percent of acute contact dermatitis cases, although the condition can also be caused by an allergic reaction. Atopic dermatitis leads to the rapid appearance of poorly circumscribed erythema, papulovesicles, or blisters, often with weeping areas.
Eosinophilic folliculitis usually occurs in patients with advanced human immunodeficiency virus infection or AIDS, although it may be idiopathic. Patients present with pruritic papules or pustules on the face, upper back, and arms.
Molluscum contagiosum is caused by the molluscum contagiosum virus (poxvirus). Patients present with one or more pearly white, umbilicated papules. In immuno-compromised patients, the lesions may be larger or more widespread.
Selected Differential Diagnosis of a Monomorphic Rash on the Neck
| Condition | Characteristics |
|---|---|
| Acne conglobata | Inflammatory nodules and pseudocysts with marked scarring, typically on the face, sternum, or back; more common in boys |
| Acute contact dermatitis | Rapid appearance of poorly circumscribed erythema, papulovesicles, or blisters, often with weeping areas |
| Eczema herpeticum | Usually occurs with atopic dermatitis; initial small, isolated vesicles abruptly group over an area of eczematous skin; lesions have central umbilication, but quickly become hemorrhagic, crusted, and eroded |
| Eosinophilic folliculitis | Usually occurs with advanced human immunodeficiency virus infection or AIDS, although it may be idiopathic; pruritic papules or pustules on the face, upper back, and arms |
| Molluscum contagiosum | Pearly white, umbilicated papules; caused by molluscum contagiosum virus (poxvirus) |

