A 51-year-old woman presented to the emergency department with painful oral ulcerations and facial swelling that had appeared five days earlier. She could not eat solid food. She had no fever, chills, or recent trauma, and was not taking any medications. The patient had smoked a half pack of cigarettes per day for 18 years. She had abstained from alcohol use for the past five years, but was a heavy drinker before that. She had not seen a physician for five years.
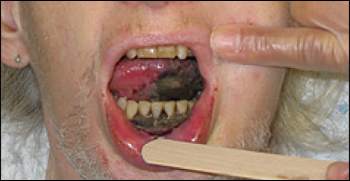
The examination revealed an unkempt woman who appeared older than her age. Oral examination demonstrated extensive gray-black ulcers on the oral mucosa, left side and undersurface of the tongue, and gingiva of the lower incisors (see accompanying figure). The patient also had tender perioral and maxillary swelling, which was more prominent on the left side of the face, and halitosis.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Acute herpetic gingivostomatitis.
B. Aphthous ulcer.
C. Ludwig angina.
D. Necrotizing stomatitis.
E. Syphilis.
Discussion
The answer is D: necrotizing stomatitis. Poor oral hygiene can lead to extensive bacterial overgrowth of normal flora in the oropharynx, producing a continuum of mild to life-threatening diseases.1 In the early stages, acute gingivitis with pain and inflammation of the gingivae can occur.2 If untreated, the bacteria can lead to acute necrotizing gingivitis. This bacterial infection can progress to gingival edema, painful ulcerations, fever, lethargy, and halitosis. The infection can spread to the floor of the mouth or tonsils (Vincent angina), the tongue and buccal mucosa (necrotizing stomatitis), or beyond the oral cavity, leading to destruction of orofacial soft and hard tissues.
The hallmark of necrotizing stomatitis is the necrotic, gray-black, shaggy ulceration of the oropharynx with halitosis, gingival inflammation, and poor dentition. In developed countries, acute necrotizing gingivitis and necrotizing stomatitis often occur in immunocompromised and malnourished persons.2,3 Poor oral hygiene, stress, and tobacco use are contributing factors. In developing countries, the disease is most common in malnourished children,1,2 in whom oral infection can quickly spread from the mucosal surface to the alveolar region. Bony destruction may develop, leading to starvation, aspiration pneumonia, or sepsis.2,3
Initial management of necrotizing stomatitis includes rehydration, nutritional supplementation, local debridement, analgesia, and antibiotic therapy. Antibiotic therapy should focus on common oral organisms, such as alpha-hemolytic streptococci, Actinomyces species, and oral spirochetes. Penicillin and clindamycin (Cleocin) are effective choices.2 Acute herpetic gingivostomatitis is caused by herpes simplex virus infection. The condition produces diffuse, erythematous, shiny lesions involving the gingivae, adjacent oral mucosa, and lips. It is associated with general malaise and cervical lymphadenitis.
Aphthous ulcers are common, painful, shallow ulcers that appear on the mucosal surfaces of the mouth. The ulcers are often triggered by fatigue, stress, or minor trauma (e.g., from brushing the teeth).
Ludwig angina is a rapidly spreading cellulitis of the submandibular and sublingual spaces that originates from a dental abscess. The patient often has elevation of the tongue, fever, drooling, swelling of the neck, trismus, and pain.
Oral manifestations can occur in all stages of syphilis. In primary syphilis, a painless ulcer (chancre) may develop. Secondary syphilis has a diverse appearance that may include nonspecific pharyngitis, glistening plaques, and a mucous patch. An ill-defined, slightly eroded, erythematous plaque on the posterior pharynx, which may be painful, can also occur. Tertiary syphilis may produce destructive granulomas (gummata) in the mouth.
Selected Differential Diagnosis of Painful Oral Ulcerations in an Adult
| Condition | Characteristics |
|---|---|
| Acute herpetic gingivostomatitis | Diffuse, erythematous, shiny lesions involving the gingivae and adjacent oral mucosa; herpes labialis; general malaise and cervical lymphadenitis |
| Aphthous ulcer | Common, painful, shallow ulcers appearing on the mucosal surfaces of the mouth; triggered by fatigue, stress, or minor trauma (e.g., brushing the teeth) |
| Ludwig angina | Cellulitis of the submandibular and sublingual spaces originating from a dental abscess; associated with fever, drooling, neck swelling, trismus, and pain |
| Necrotizing stomatitis | Necrotic, gray-black, shaggy ulcerations of the oropharynx with halitosis |
| Syphilis | Varies depending on stage of disease: painless ulcer or chancre (primary syphilis); mucous patch and ill-defined, painful, erythematous plaque on the posterior pharynx (secondary syphilis); destructive granulomas, or gummata, in the mouth (tertiary syphilis) |

