Red eye is the cardinal sign of ocular inflammation. The condition is usually benign and can be managed by primary care physicians. Conjunctivitis is the most common cause of red eye. Other common causes include blepharitis, corneal abrasion, foreign body, subconjunctival hemorrhage, keratitis, iritis, glaucoma, chemical burn, and scleritis. Signs and symptoms of red eye include eye discharge, redness, pain, photophobia, itching, and visual changes. Generally, viral and bacterial conjunctivitis are self-limiting conditions, and serious complications are rare. Because there is no specific diagnostic test to differentiate viral from bacterial conjunctivitis, most cases are treated using broad-spectrum antibiotics. Allergies or irritants also may cause conjunctivitis. The cause of red eye can be diagnosed through a detailed patient history and careful eye examination, and treatment is based on the underlying etiology. Recognizing the need for emergent referral to an ophthalmologist is key in the primary care management of red eye. Referral is necessary when severe pain is not relieved with topical anesthetics; topical steroids are needed; or the patient has vision loss, copious purulent discharge, corneal involvement, traumatic eye injury, recent ocular surgery, distorted pupil, herpes infection, or recurrent infections.
Red eye is one of the most common ophthalmologic conditions in the primary care setting. Inflammation of almost any part of the eye, including the lacrimal glands and eyelids, or faulty tear film can lead to red eye. Primary care physicians often effectively manage red eye, although knowing when to refer patients to an ophthalmologist is crucial.
SORT: KEY CLINICAL RECOMMENDATIONS
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Good hygiene, such as meticulous hand washing, is important in decreasing the spread of acute viral conjunctivitis. | C | 2, 4 |
| Any ophthalmic antibiotic may be considered for the treatment of acute bacterial conjunctivitis because they have similar cure rates. | A | 23–26 |
| Mild allergic conjunctivitis may be treated with an over-the-counter antihistamine/vasoconstrictor agent, or with a more effective second-generation topical histamine H1 receptor antagonist. | C | 15 |
| Anti-inflammatory agents (e.g., topical cyclosporine [Restasis]), topical corticosteroids, and systemic omega-3 fatty acids are appropriate therapies for moderate dry eye. | C | 32 |
| Patients with chronic blepharitis who do not respond adequately to eyelid hygiene and topical antibiotics may benefit from an oral tetracycline or doxycycline. | C | 4, 33 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Causes of Red Eye
Conjunctivitis is the most common cause of red eye and is one of the leading indications for antibiotics.1 Causes of conjunctivitis may be infectious (e.g., viral, bacterial, chlamydial) or noninfectious (e.g., allergies, irritants).2 Most cases of viral and bacterial conjunctivitis are self-limiting. Other common causes of red eye include blepharitis, corneal abrasion, foreign body, subconjunctival hemorrhage, keratitis, iritis, glaucoma, chemical burn, and scleritis.
A thorough patient history and eye examination may provide clues to the etiology of red eye (Figure 1). The history should include questions about unilateral or bilateral eye involvement, duration of symptoms, type and amount of discharge, visual changes, severity of pain, photophobia, previous treatments, presence of allergies or systemic disease, and the use of contact lenses. The eye examination should include the eyelids, lacrimal sac, pupil size and reaction to light, corneal involvement, and the pattern and location of hyperemia. Preauricular lymph node involvement and visual acuity must also be assessed. Common causes of red eye and their clinical presentations are summarized in Table 1.2–11
Figure 1. Diagnosis of the Underlying Cause of Red Eye
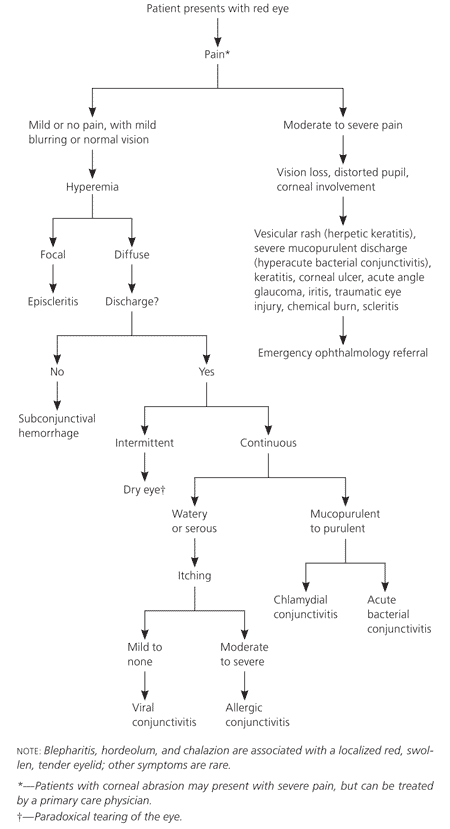
Algorithm for diagnosing the cause of red eye.
Table 1. Selected Differential Diagnosis of Red Eye
| Condition | Signs | Symptoms | Causes |
|---|---|---|---|
| Conjunctivitis | |||
| Viral | Normal vision, normal pupil size and reaction to light, diffuse conjunctival injections (redness), preauricular lymphadenopathy, lymphoid follicle on the undersurface of the eyelid | Mild to no pain, diffuse hyperemia, occasional gritty discomfort with mild itching, watery to serous discharge, photophobia (uncommon), often unilateral at onset with second eye involved within one or two days, severe cases may cause subepithelial corneal opacities and pseudomembranes | Adenovirus (most common), enterovirus, coxsackievirus, VZV, Epstein-Barr virus, HSV, influenza |
| Herpes zoster ophthalmicus | Vesicular rash, keratitis, uveitis | Pain and tingling sensation precedes rash and conjunctivitis, typically unilateral with dermatomal involvement (periocular vesicles) | Herpes zoster |
| Bacterial (acute and chronic) | Eyelid edema, preserved visual acuity, conjunctival injection, normal pupil reaction, no corneal involvement | Mild to moderate pain with stinging sensation, red eye with foreign body sensation, mild to moderate purulent discharge, mucopurulent secretions with bilateral glued eyes upon awakening (best predictor) | Common pathogens in children: Streptococcus pneumoniae, nontypeable Haemophilus influenzae |
| Common pathogen in adults: Staphylococcus aureus | |||
| Other pathogens: Staphylococcus species, Moraxella species, Neisseria gonorrhoeae, gram-negative organisms (e.g., Escherichia coli), Pseudomonas species | |||
| Bacterial (hyperacute) | Chemosis with possible corneal involvement | Severe pain; copious, purulent discharge; diminished vision | N. gonorrhoeae |
| Chlamydial (inclusion conjunctivitis) | Vision usually preserved, pupils reactive to light, conjunctival injections, no corneal involvement, preauricular lymph node swelling is sometimes present | Red, irritated eye; mucopurulent or purulent discharge; glued eyes upon awakening; blurred vision | Chlamydia trachomatis (serotypes D to K) |
| Allergic | Visual acuity preserved, pupils reactive to light, conjunctival injection, no corneal involvement, large cobblestone papillae under upper eyelid, chemosis | Bilateral eye involvement; painless tearing; intense itching; diffuse redness; stringy or ropy, watery discharge | Airborne pollens, dust mites, animal dander, feathers, other environmental antigens |
| Other causes | |||
| Dry eye (kerato-conjunctivitis sicca) | Vision usually preserved, pupils reactive to light; hyperemia, no corneal involvement | Bilateral red, itchy eyes with foreign body sensation; mild pain; intermittent excessive watering | Imbalance in any tear component (production, distribution, evaporation, absorption); medications (anticholinergics, antihistamines, oral contraceptive pills); Sjögren syndrome |
| Blepharitis | Dandruff-like scaling on eyelashes, missing or misdirected eyelashes, swollen eyelids, secondary changes in conjunctiva and cornea leading to conjunctivitis | Red, irritated eye that is worse upon waking; itchy, crusted eyelids | Chronic inflammation of eyelids (base of eyelashes or meibomian glands) by staphylococcal infection |
| Corneal abrasion and foreign body | Reactive miosis, corneal edema or haze, possible foreign body, normal anterior chamber, visual acuity depends on the position of the abrasion in relation to visual axis | Unilateral or bilateral severe eye pain; red, watery eyes; photophobia; foreign body sensation; blepharospasm | Direct injury from an object (e.g., finger, paper, stick, makeup applicator); metallic foreign body; contact lenses |
| Subconjunctival hemorrhage | Normal vision; pupils equal and reactive to light; well demarcated, bright red patch on white sclera; no corneal involvement | Mild to no pain, no vision disturbances, no discharge | Spontaneous causes: hypertension, severe coughing, straining, atherosclerotic vessels, bleeding disorders |
| Traumatic causes: blunt eye trauma, foreign body, penetrating injury | |||
| Episcleritis | Visual acuity preserved, pupils equal and reactive to light, dilated episcleral blood vessels, edema of episclera, tenderness over the area of injection, confined red patch | Mild to no pain; limited, isolated patches of injection; mild watering | Idiopathic (isolated presentation) |
| Keratitis (corneal inflammation) | Diminished vision, corneal opacities/white spot, fluorescein staining under Wood lamp shows corneal ulcers, eyelid edema, hypopyon | Painful red eye, diminished vision, photophobia, mucopurulent discharge, foreign body sensation | Bacterial (Staphylococcus species, Streptococcus); viral (HSV, VZV, Epstein-Barr virus, cytomegalovirus); abrasion from foreign body; contact lenses |
| Iritis | Diminished vision; poorly reacting, constricted pupils; ciliary/perilimbal injection | Constant eye pain (radiating into brow/temple) developing over hours, watering red eye, blurred vision, photophobia | Exogenous infection from perforating wound or corneal ulcer, autoimmune conditions |
| Glaucoma (acute angle-closure) | Marked reduction in visual acuity, dilated pupils react poorly to light, diffuse redness, eyeball is tender and firm to palpation | Acute onset of severe, throbbing pain; watering red eye; halos appear when patient is around lights | Obstruction to outflow of aqueous humor leading to increased intraocular pressure |
| Chemical burn | Diminished vision, corneal involvement (common) | Severe, painful red eye; photophobia | Common agents include cement, plaster powder, oven cleaner, and drain cleaner |
| Scleritis | Diffuse redness, diminished vision, tenderness, scleral edema, corneal ulceration | Severe, boring pain radiating to periorbital area; pain increases with eye movements; ocular redness; watery discharge; photophobia; intense nighttime pain; pain upon awakening | Systemic diseases, such as rheumatoid arthritis, Wegener granulomatosis, reactive arthritis, sarcoidosis, inflammatory bowel disease, syphilis, tuberculosis |
HSV = herpes simplex virus; VZV = varicella-zoster virus.
Diagnosis and Treatment
VIRAL CONJUNCTIVITIS
Viral conjunctivitis (Figure 2) caused by the adenovirus is highly contagious, whereas conjunctivitis caused by other viruses (e.g., herpes simplex virus [HSV]) are less likely to spread. Viral conjunctivitis usually spreads through direct contact with contaminated fingers, medical instruments, swimming pool water, or personal items. It is often associated with an upper respiratory infection spread through coughing. The clinical presentation of viral conjunctivitis is usually mild with spontaneous remission after one to two weeks.3 Treatment is supportive and may include cold compresses, ocular decongestants, and artificial tears. Topical antibiotics are rarely necessary because secondary bacterial infections are uncommon.12
To prevent the spread of viral conjunctivitis, patients should be counseled to practice strict hand washing and avoid sharing personal items; food handlers and health care workers should not work until eye discharge ceases; and physicians should clean instruments after every use.13 Referral to an ophthalmologist is necessary if symptoms do not resolve after seven to 10 days or if there is corneal involvement.4 Topical corticosteroid therapy for any cause of red eye is used only under direct supervision of an ophthalmologist.5,12 Suspected ocular herpetic infection also warrants immediate ophthalmology referral.
Figure 2.
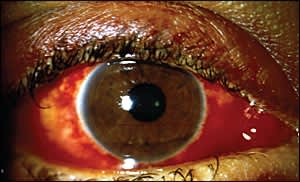
Viral conjunctivitis with intensely hyperemic conjunctiva, perilimbal sparing, and watery discharge.
BACTERIAL CONJUNCTIVITIS
Bacterial conjunctivitis is highly contagious and is most commonly spread through direct contact with contaminated fingers.2 Based on duration and severity of signs and symptoms, bacterial conjunctivitis is categorized as hyperacute, acute, or chronic.4,12
Hyperacute bacterial conjunctivitis (Figure 314 ) is often associated with Neisseria gonorrhoeae in sexually active adults. The infection has a sudden onset and progresses rapidly, leading to corneal perforation. Hyperacute bacterial conjunctivitis is characterized by copious, purulent discharge; pain; and diminished vision loss. Patients need prompt ophthalmology referral for aggressive management.4,12 Acute bacterial conjunctivitis is the most common form of bacterial conjunctivitis in the primary care setting. Signs and symptoms persist for less than three to four weeks. Staphylococcus aureus infection often causes acute bacterial conjunctivitis in adults, whereas Streptococcus pneumoniae and Haemophilus influenzae infections are more common causes in children. Chronic bacterial conjunctivitis is characterized by signs and symptoms that persist for at least four weeks with frequent relapses.2 Patients with chronic bacterial conjunctivitis should be referred to an ophthalmologist.
Figure 3.
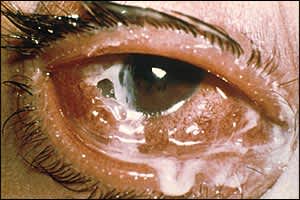
Hyperacute bacterial conjunctivitis with reac-cumulating, copious, purulent discharge; severe pain; chemosis with corneal involvement; and eyelid swelling. Prompt referral to an ophthalmologist is needed.
Reprinted with permission from Fay A. Diseases of the visual system. In: Goldman L, Ausillo D, eds. Cecil Medicine. 23rd ed. Philadelphia, Pa.: Saunders; 2007.
Laboratory tests to identify bacteria and sensitivity to antibiotics are performed only in patients with severe cases, in patients with immune compromise, in contact lens wearers, in neonates, and when initial treatment fails.4,15 Generally, topical antibiotics have been prescribed for the treatment of acute infectious conjunctivitis because of the difficulty in making a clinical distinction between bacterial and viral conjunctivitis. Benefits of antibiotic treatment include quicker recovery, early return to work or school, prevention of further complications, and decreased future physician visits.2,6,16
A meta-analysis based on five randomized controlled trials showed that bacterial conjunctivitis is self-limiting (65 percent of patients improved after two to five days without antibiotic treatment), and that severe complications are rare.2,7,16–19 Studies show that bacterial pathogens are isolated from only 50 percent of clinically diagnosed bacterial conjunctivitis cases.8,16 Moreover, the use of antibiotics is associated with increased antibiotic resistance, additional expense for patients, and the medicalization of minor illness.4,20–22 Therefore, delaying antibiotic therapy is an option for acute bacterial conjunctivitis in many patients (Table 2).2,9 A shared decision-making approach is appropriate, and many patients are willing to delay antibiotic therapy when counseled about the self-limiting nature of the disease. Some schools require proof of antibiotic treatment for at least two days before readmitting students,7 and this should be addressed when making treatment decisions.
Table 2. Management Options for Suspected Acute Bacterial Conjunctivitis
| Management option | Patient group |
|---|---|
| Consider immediate antibiotic therapy | Health care workers |
| Patients who are in a hospital or other health care facility | |
| Patients with risk factors, such as immune compromise, uncontrolled diabetes mellitus, contact lens use, dry eye, or recent ocular surgery | |
| Children going to schools or day care centers that require antibiotic therapy before returning | |
| Consider delaying antibiotic therapy | Patients without risk factors who are well informed and have access to follow-up care |
| Patients without risk factors who do not want immediate antibiotic therapy |
Studies comparing the effectiveness of different ophthalmic antibiotics did not show one to be superior.23–26 The choice of antibiotic (Table 3) should be based on cost-effectiveness and local bacterial resistance patterns. If the infection does not improve within one week of treatment, the patient should be referred to an ophthalmologist.4,5
Table 3. Ophthalmic Therapies for Acute Bacterial Conjunctivitis
| Therapy | Usual dosage | Cost of generic (brand)* | In retail discount programs† |
|---|---|---|---|
| Azithromycin 1% (Azasite) | Solution: One drop two times daily (administered eight to 12 hours apart) for two days, then one drop daily for five days | NA ($82) for 5 mL | |
| Besifloxacin 0.6% (Besivance) | Solution: One drop three times daily for one week | NA ($85) for 5 mL | |
| Ciprofloxacin 0.3% (Ciloxan)‡ | Ointment: 0.5-inch ribbon applied in conjunctival sac three times daily for one week | Ointment: NA ($99) for 3.5 g Solution: $30 ($65) for 5 mL | |
| Solution: One or two drops four times daily for one week | |||
| Erythromycin 0.5% | Ointment: 0.5-inch ribbon applied four times daily for one week | $13 (NA) for 3.5 g | ✓ |
| Gatifloxacin 0.3% (Zymar) or moxifloxacin 0.5% (Vigamox)§ | Solution: One drop three times daily for one week | NA ($84) for 5 mL | |
| Gentamicin 0.3% (Gentak) | Ointment: 0.5-inch ribbon applied four times daily for one week | Ointment: NA ($22) for 3.5 g | ✓ |
| Solution: One to two drops four times daily for one week | Solution: $15 ($18) for 15 mL | ||
| Levofloxacin 1.5% (Iquix) or 0.5% (Quixin)‡ | Solution: One or two drops four times daily for one week | 1.5%: NA ($89) for 5 mL | |
| 0.5%: NA ($57) for 5 mL | |||
| Ofloxacin 0.3% (Ocuflox)‡ | Solution: One or two drops four times daily for one week | $44 ($80) for 5 mL | |
| Sulfacetamide 10% (Bleph-10) | Ointment: Apply to lower conjunctival sac four times daily and at bedtime for one week | $13 ($22) for 5 mL | ✓ |
| Solution: One or two drops every two to three hours for one week | |||
| Tobramycin 0.3% (Tobrex) | Ointment: 0.5-inch ribbon applied in conjunctival sac three times daily for one week | Ointment: NA ($76) for 3.5 g | ✓ |
| Solution: One to two drops four times daily for one week | Solution: $16 ($60) for 5 mL | ||
| Trimethoprim/polymyxin B (Polytrim) | Solution: One or two drops four times daily for one week | NA ($42) for 10 mL | ✓ |
note: Supportive care for acute bacterial conjunctivitis includes warm compresses and eye irrigation, but eye patching should be avoided. Although chloramphenicol is the first-line treatment in other countries, it is no longer available in the United States. In patients who wear contact lenses, pseudomonal coverage is essential; quinolones are highly effective against Pseudomonas.
NA = not available.
*— Estimated retail price based on information obtained at http://www.drugstore.com and Walgreens (November 2009). Generic price listed first; brand price listed in parentheses.
†— May be available at discounted prices ($10 or less for one month's treatment) at one or more national retail chains.
‡— Topical fluoroquinolones are highly effective and should be reserved for severe infections.
§— Gatifloxacin and moxifloxacin have improved coverage against ciprofloxacin-resistant organisms, but decreased activity against Pseudomonas.
CHLAMYDIAL CONJUNCTIVITIS
Chlamydial conjunctivitis should be suspected in sexually active patients who have typical signs and symptoms and do not respond to standard antibacterial treatment.2 Patients with chlamydial infection also may present with chronic follicular conjunctivitis. Polymerase chain reaction testing of conjunctival scrapings is diagnostic, but is not usually needed. Treatment includes topical therapy with erythromycin ophthalmic ointment, and oral therapy with azithromycin (Zithromax; single 1-g dose) or doxycycline (100 mg twice a day for 14 days) to clear the genital infection.4 The patient's sexual partners also must be treated.
ALLERGIC CONJUNCTIVITIS
Allergic conjunctivitis is often associated with atopic diseases, such as allergic rhinitis (most common), eczema, and asthma.27 Ocular allergies affect an estimated 25 percent of the population in the United States.28 Itching of the eyes is the most apparent feature of allergic conjunctivitis. Seasonal allergic conjunctivitis is the most common form of the condition, and symptoms are related to season-specific aeroallergens. Perennial allergic conjunctivitis persists throughout the year. Allergic conjunctivitis is primarily a clinical diagnosis.
Avoiding exposure to allergens and using artificial tears are effective methods to alleviate symptoms. Over-the-counter antihistamine/vasoconstrictor agents are effective in treating mild allergic conjunctivitis. Another, more effective, option is a second-generation topical histamine H1 receptor antagonist.15 Table 4 presents ophthalmic therapies for allergic conjunctivitis.
Table 4. Ophthalmic Therapies for Allergic Conjunctivitis
| Therapy | Usual dosage | Cost of generic (brand)* |
|---|---|---|
| Histamine H1 receptor antagonists† | ||
| Azelastine 0.05% (Optivar) | One drop twice daily | $140 ($108) for 6 mL |
| Emedastine 0.05% (Emadine) | One drop four times daily | NA ($72) for 5 mL |
| Mast cell stabilizers‡ | ||
| Cromolyn sodium 4% (Crolom) | One or two drops every four to six hours | $32 ($45) for 10 mL |
| Lodoxamide 0.1% (Alomide) | One or two drops four times daily | NA ($98) for 10 mL |
| Nedocromil 2% (Alocril) | One or two drops twice daily | NA ($90) for 5 mL |
| Mast cell stabilizers and H1 receptor antagonists | ||
| Ketotifen 0.025% (Zaditor; available over the counter as Alaway) | One drop every eight to 12 hours | NA ($70) for 5 mL |
| Olopatadine 0.1% (Patanol) | One drop twice daily | NA ($96) for 5 mL |
| Nonsteroidal anti-inflammatory drugs | ||
| Ketorolac 0.5% (Acular) | One drop four times daily | $110 ($161) for 5 mL |
| Vasoconstrictor/antihistamine§ | ||
| Naphazoline/pheniramine (available over the counter as Opcon-A, Visine-A) | One or two drops up to four times daily | NA ($6 to $11) for 15 mL |
note: Severe cases may require topical corticosteroids and ophthalmology referral.
NA = not available.
*— Estimated retail price based on information obtained at http://www.drugstore.com and Walgreens (November 2009). Generic price listed first; brand price listed in parentheses. None of these therapies are offered in retail discount programs.
†— Relieves itching immediately. Treats mild allergic conjunctivitis.
‡— Takes time for effect to be apparent. Treats mild to moderately severe allergic conjunctivitis.
§— Used for short-term relief of mild allergic conjunctivitis. This therapy is less expensive than others.
DRY EYE
Dry eye (keratoconjunctivitis sicca) is a common condition caused by decreased tear production or poor tear quality. It is associated with increased age, female sex, medications (e.g., anticholinergics), and some medical conditions.29 Diagnosis is based on clinical presentation and diagnostic tests. Tear osmolarity is the best single diagnostic test for dry eye.30,31 The overall accuracy of the diagnosis increases when tear osmolarity is combined with assessment of tear turnover rate and evaporation. Some patients with dry eye may have ocular discomfort without tear film abnormality on examination. In these patients, treatment for dry eye can be initiated based on signs and symptoms. If Sjögren syndrome is suspected, testing for autoantibodies should be performed.
Treatment includes frequent applications of artificial tears throughout the day and nightly application of lubricant ointments, which reduce the rate of tear evaporation. The use of humidifiers and well-fitting eyeglasses with side shields can also decrease tear loss. If artificial tears cause itching or irritation, it may be necessary to switch to a preservative-free form or an alternative preparation. When inflammation is the main factor in dry eye, cyclosporine ophthalmic drops (Restasis) may increase tear production.5 Topical cyclosporine may take several months to provide subjective improvement. Systemic omega-3 fatty acids have also been shown to be helpful.32 Topical corticosteroids are shown to be effective in treating inflammation associated with dry eye.32 The goal of treatment is to prevent corneal scarring and perforation. Ophthalmology referral is indicated if the patient needs topical steroid therapy or surgical procedures.
BLEPHARITIS
Blepharitis is a chronic inflammatory condition of the eyelid margins and is diagnosed clinically. Patients should be examined for scalp or facial skin flaking (seborrheic dermatitis), facial flushing, and redness and swelling on the nose or cheeks (rosacea). Treatment involves eyelid hygiene (cleansing with a mild soap, such as diluted baby shampoo, or eye scrub solution), gentle lid massage, and warm compresses. This regimen should continue indefinitely. Topical erythromycin or bacitracin ophthalmic ointment applied to eyelids may be used in patients who do not respond to eyelid hygiene. Azithromycin eye drops may also be used in the treatment of blepharitis. In severe cases, prolonged use of oral antibiotics (doxycycline or tetracycline) may be beneficial.33 Topical steroids may also be useful for severe cases.30
CORNEAL ABRASION
Corneal abrasion is diagnosed based on the clinical presentation and eye examination. If needed, short-term topical anesthetics may be used to facilitate the eye examination. Fluorescein staining under a cobalt blue filter or Wood lamp is confirmatory. A branching pattern of staining suggests HSV infection or a healing abrasion. HSV infection with corneal involvement warrants ophthalmology referral within one to two days. In patients with corneal abrasion, it is good practice to check for a retained foreign body under the upper eyelid.
Treatment includes supportive care, cycloplegics (atropine, cyclopentolate [Cyclogyl], homatropine, scopolamine, and tropicamide), and pain control (topical nonsteroidal anti-inflammatory drugs [NSAIDs] or oral analgesics). The need for topical antibiotics for uncomplicated abrasions has not been proven. Topical aminoglycosides should be avoided because they are toxic to corneal epi-thelium.34 Studies show that eye patches do not improve patient comfort or healing of corneal abrasion.35 All steroid preparations are contraindicated in patients with corneal abrasion. Referral to an ophthalmologist is indicated if symptoms worsen or do not resolve within 48 hours.
SUBCONJUNCTIVAL HEMORRHAGE
Subconjunctival hemorrhage is diagnosed clinically. It is harmless, with blood reabsorption over a few weeks, and no treatment is needed. Warm compresses and ophthalmic lubricants (e.g., hydroxypropyl cellulose [Lacrisert], methylcellulose [Murocel], artificial tears) may relieve symptoms. If pain is present, a cause must be identified. It is good practice to check for corneal involvement or penetrating injury, and to consider urgent referral to ophthalmology. Recurrent hemorrhages may require a workup for bleeding disorders. If the patient is taking warfarin (Coumadin), the International Normalized Ratio should be checked.
EPISCLERITIS
Episcleritis is a localized area of inflammation involving superficial layers of episclera. It is usually self-limiting (lasting up to three weeks) and is diagnosed clinically. Investigation of underlying causes is needed only for recurrent episodes and for symptoms suggestive of associated systemic diseases, such as rheumatoid arthritis. Treatment involves supportive care and use of artificial tears. Topical NSAIDs have not been shown to have significant benefit over placebo in the treatment of episcleritis.36 Topical steroids may be useful for severe cases. Ophthalmology referral is required for recurrent episodes, an unclear diagnosis (early scleritis), and worsening symptoms.

