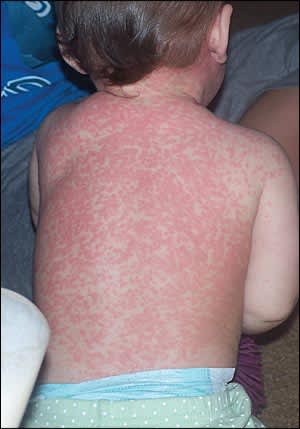
A previously healthy 12-month-old girl presented with an erythematous, macular rash (see accompanying figure) and a fever of 102°F (38.9°C) that began one day earlier. The child attended day care and had two older siblings in the home. One sibling had an upper respiratory tract infection at the time of presentation, and the other had varicella the previous month. The patient received immunizations one week earlier, including hepatitis B; diphtheria and tetanus toxoids, and acellular pertussis (Tripedia); measles, mumps, rubella, and varicella (MMRV); pneumococcal conjugate (Prevnar); and inactivated poliovirus. The child had been irritable, and had decreased oral intake and urination. On physical examination, there were no oral lesions, and the rash was nonpruritic.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Fifth disease.
B. MMRV vaccine adverse reaction.
C. Roseola.
D. Scarlatina.
E. Varicella.
Discussion
The answer is B: MMRV vaccine adverse reaction. The MMRV vaccine is a live virus vaccine, and adverse reactions may represent replication of the measles virus. Adverse events generally occur five to 12 days post-vaccination. Fever is the most common reaction (5 to 15 percent of persons).1 Rash is reported in approximately 5 percent of those receiving measles-containing vaccines.1 The nonpruritic rash typically appears as erythematous macules that begin on the neck and spread caudally to the trunk and extremities, similarly to the exanthem of measles. Discrete lesions may become confluent, copper colored, and nonblanching over time.
Vaccination with MMRV is a safe and effective alternative to the measles, mumps, and rubella vaccine administered separately from the varicella vaccine, although some studies have shown a slightly higher incidence of postvaccination fever and rash with the MMRV vaccine.2,3 Minor adverse effects, such as fever and rash, are not contraindications to the second dose of the MMRV vaccine.4
Fifth disease (human parvovirus B19 infection) is characterized by mild systemic symptoms followed by the development of an erythematous, nonraised, confluent, “slapped cheek” appearance on the child's face. The second phase of fifth disease involves a lacy reticular rash on the trunk and extremities that may persist for several weeks. The rash may be pruritic.
Roseola, an infection with human herpes-virus 6 and 7, initially leads to several days of high fever (greater than 103°F [39.4°C]), followed by a macular, nonpruritic rash. The rash typically persists for hours to days and resolves spontaneously.
Scarlatina is a manifestation of group A streptococcal infection that is typically associated with pharyngitis. A nonpruritic, orange-red colored, punctate eruption with sandpaper-like texture begins on the trunk and spreads to the extremities, often in the skinfolds. Desquamation of skin occurs about one week after eruption of the rash.
Varicella begins on the trunk with teardrop-shaped vesicles on an erythematous base. The pruritic lesions erupt in crops and progress from macule to papule to vesicle, then crust. Lesions in different stages occur simultaneously.
Summary Table
| Condition | Characteristics |
|---|---|
| Fifth disease | Erythematous, nonraised, confluent, “slapped cheek” rash on the face, followed by a lacy reticular rash on the trunk and extremities; may persist for several weeks; pruritus possible |
| MMRV vaccination adverse reaction | Measles-like, nonpruritic, macular rash; begins on the neck and spreads to the trunk and extremities; typically lasts two weeks; discrete lesions may become confluent, copper colored, and nonblanching |
| Roseola | Nonpruritic, macular rash that erupts on trunk after high fever; typically lasts hours to days |
| Scarlatina | Nonpruritic, orange-red colored, punctate rash with sandpaper-like texture; begins on the trunk and spreads to the extremities, often in skinfolds; desquamation typically occurs one week after rash eruption |
| Varicella | Teardrop-shaped vesicles on an erythematous base; pruritic lesions progress from macules to papules to vesicles, then crust; begins on the trunk and spreads to extremities |
MMRV = measles, mumps, rubella, and varicella.

