Although easily examined, abnormalities of the tongue can present a diagnostic and therapeutic dilemma for physicians. Recognition and diagnosis require a thorough history, including onset and duration, antecedent symptoms, and tobacco and alcohol use. Examination of tongue morphology and a careful assessment for lymphadenopathy are also important. Geographic tongue, fissured tongue, and hairy tongue are the most common tongue problems and do not require treatment. Median rhomboid glossitis is usually associated with a candidal infection and responds to topical antifungals. Atrophic glossitis is often linked to an underlying nutritional deficiency of iron, folic acid, vitamin B12, riboflavin, or niacin and resolves with correction of the underlying condition. Oral hairy leukoplakia, which can be a marker for underlying immunodeficiency, is caused by the Epstein-Barr virus and is treated with oral antivirals. Tongue growths usually require biopsy to differentiate benign lesions (e.g., granular cell tumors, fibromas, lymphoepithelial cysts) from premalignant leukoplakia or squamous cell carcinoma. Burning mouth syndrome often involves the tongue and has responded to treatment with alpha-lipoic acid, clonazepam, and cognitive behavior therapy in controlled trials. Several trials have also confirmed the effectiveness of surgical division of tongue-tie (ankyloglossia), in the context of optimizing the success of breastfeeding compared with education alone. Tongue lesions of unclear etiology may require biopsy or referral to an oral and maxillofacial surgeon, head and neck surgeon, or a dentist experienced in oral pathology.
Recognition and diagnosis of tongue abnormalities require examination of tongue morphology and a thorough history, including onset and duration, antecedent symptoms, and tobacco and alcohol use. A complete head and neck examination, with careful assessment for lymphadenopathy, is essential.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Ulcerative lichen planus can be treated with topical steroids, such as clobetasol (Temovate) or fluocinonide dental paste. | B | 27 |
| Some oral leukoplakias may become malignant; therefore, biopsy and microscopic analysis should be considered. | C | 31–33 |
| Only alpha-lipoic acid, clonazepam (Klonopin), and cognitive behavior therapy have been shown to reduce symptoms of burning tongue. | B | 44 |
| Frenulectomy is an effective approach in infants with tongue-tie (ankyloglossia) who have breastfeeding difficulties. | B | 46–48 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
According to the National Health and Nutrition Examination Survey, the point prevalence of tongue lesions is 15.5 percent in U.S. adults. Lesion prevalence is increased in those who wear dentures or use tobacco. The most common tongue condition is geographic tongue, followed by fissured tongue and hairy tongue.1 Table 1 summarizes common tongue conditions.
Table 1. Summary of Tongue Conditions
| Condition | Clinical presentation | Treatment | Comments |
|---|---|---|---|
| Median rhomboid glossitis | Smooth, shiny, erythematous, sharply circumscribed, rhomboid shaped plaque; usually asymptomatic, but burning or itching possible; dorsal midline location | Topical antifungals | Often associated with candidal infection |
| Atrophic glossitis | Smooth, glossy appearance with red or pink background | Treat nutritional deficiency or other underlying condition | Caused by underlying disease, medication use, or nutritional deficiencies (e.g., iron, folic acid, vitamin B12, riboflavin, niacin) |
| Fissured tongue | Deep grooves, malodor and discoloration may occur with inflammation or trapping of food | Usually no treatment; gentle brushing of tongue if symptomatic inflammation occurs | Associated with Down syndrome, psoriasis, Sjögren syndrome, Melkersson-Rosenthal syndrome, geographic tongue |
| Geographic tongue | Bare patches on dorsal tongue surrounded by serpiginous, raised, slightly discolored border | No treatment necessary, but topical steroid gels or antihistamine rinses can reduce tongue sensitivity | Associated with fissured tongue, inversely associated with tobacco use |
| Hairy tongue | Hypertrophy of filiform papillae, tongue discoloration (white, tan, black) | No treatment necessary, but gentle brushing or scraping of tongue may be helpful | Associated with tobacco use, poor oral hygiene, antibiotic use |
| Oral hairy leukoplakia | White, hairy appearing lesions on lateral border of tongue | Antiviral medications | Epstein-Barr virus super infection; associated with immunocompromise, human immunodeficiency virus infection |
| Lichen planus | Manifests as reticular, white, lacy pattern on dorsal tongue or as shallow, scattered, erythematous ulcerations | No treatment if asymptomatic, topical steroid for symptomatic ulcerative lesions | Consider evaluation and treatment for coexisting candidal infection; biopsy needed for definitive diagnosis of lichen planus |
| Linea alba | Thin white line of thickened epithelium on lateral borders of tongue | No treatment necessary | Caused by chewing trauma to lateral tongue |
| Leukoplakia | White adherent patch or plaque | Close observation, biopsy to rule out malignancy | Strongly associated with tobacco use, but higher malignant potential when occurring in never smokers |
| Squamous cell carcinoma | Thickened white or red patch or plaque, may develop nodularity or ulceration, usually on lateral tongue | Surgical excision, radiation | Associated with tobacco use, alcohol use, older age |
| Papilloma | Single, isolated pedunculated lesion with finger-like projections | Surgical excision or laser ablation | Associated with human papillomavirus type 6 or 11 infection |
| Burning tongue | Daily pain that worsens throughout the day, tongue has normal appearance | Alpha-lipoic acid, clonazepam (Klonopin), cognitive behavior therapy; treatment of any underlying condition | Underlying systemic or local disorders (e.g., nutritional deficiency, endocrine, hyposalivation, infection, allergic reaction) should be excluded |
| Tongue-tie (ankyloglossia) | Shortened frenulum limiting tongue protrusion, breastfeeding difficulties | Surgical division in infants having difficulty breastfeeding | Associated with poor breastfeeding, including nipple pain |
| Macroglossia | Enlarged tongue with scalloping of lateral margin | Treat underlying condition | Associated with various underlying conditions |
Abnormalities of the Tongue Surface
MEDIAN RHOMBOID GLOSSITIS
Median rhomboid glossitis is characterized by a smooth, shiny, erythematous, sharply circumscribed, asymptomatic, plaque-like lesion on the dorsal midline of the tongue (Figure 1). Men are affected three times more often than women.2 Most persons with the condition are asymptomatic, but burning or itching is possible.3 Median rhomboid glossitis is commonly associated with a candidal infection and responds to antifungals (e.g., nystatin, fluconazole [Diflucan], clotrimazole) delivered as a suspension or oral troche.4–6 Candida can be confirmed with a scraping or culture. Other surfaces of the mouth are characteristically spared. However, the presence of palatal inflammation may be indicative of immunosuppression, and human immunodeficiency virus (HIV) infection should be considered.2
Figure 1.
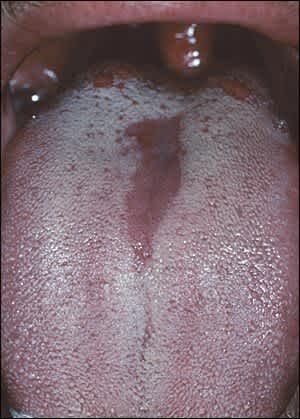
Median rhomboid glossitis. Candidal infection can be confirmed by a scraping from inflamed area.
ATROPHIC GLOSSITIS
Atrophic glossitis is also known as smooth tongue because of the smooth, glossy appearance with a red or pink background. The smooth quality is caused by the atrophy of filiform papillae. Atrophic glossitis is primarily a manifestation of underlying conditions (Table 21,6,7) and warrants thorough diagnostic evaluation. Nutritional deficiencies of iron, folic acid, vitamin B12, riboflavin, and niacin are common causes.2,3,8,9 Other etiologies include systemic infection (e.g., syphilis), localized infection (e.g., Candida), amyloidosis, celiac disease, protein-calorie malnutrition, and xerostomia triggered by some medications and Sjögren syndrome.2,8,10–12 Atrophic glossitis caused by nutritional deficiency often causes a painful sensation in the tongue. Treatment includes replacement of the missing nutrient or treatment of the underlying condition.11–13
Table 2. Conditions Associated with Glossitis
| Amyloidosis |
| Celiac disease |
| Chemical irritants |
| Drug reactions |
| Local infections (especially candidiasis) |
| Nutritional deficiencies (e.g., iron, folic acid, vitamin B12, riboflavin, niacin) |
| Pernicious anemia |
| Protein-calorie malnutrition |
| Sarcoidosis |
| Sjögren syndrome |
| Systemic infections (e.g., syphilis) |
| Vesiculoerosive diseases (e.g., pemphigoid, pemphigus vulgaris, erythema multiforme, Stevens-Johnson syndrome) |
FISSURED TONGUE
With fissured tongue (Figure 2), deep grooves can develop due to physiologic deepening of normal tongue fissures. These typically occur with aging and require no treatment, unless trapping of food and bacteria leads to inflammation of the fissures.2 Gentle brushing of the tongue is useful in persons with symptomatic inflammation. Fissured tongue has been associated with Down syndrome, acromegaly, psoriasis, and Sjögren syndrome.2,14 Melkersson-Rosenthal syndrome is a rare disorder of unclear etiology that is characterized by a triad of severe fissuring, relapsing orofacial edema, and facial nerve palsy.15
Figure 2.
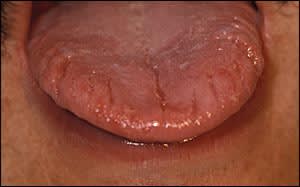
Fissured tongue. Fissures may trap food and bacteria, causing localized inflammation. Changes of geographic tongue are also noted.
GEOGRAPHIC TONGUE
Geographic tongue (Figure 3), also known as benign migratory glossitis or erythema migrans, affects 1 to 14 percent of the U.S. population and is of unknown etiology.1,2,16 Although previous research pointed to associations with diabetes, psoriasis, seborrheic dermatitis, and atopy, recent analysis of population data from U.S. patients does not support these findings.2,14,17–20 The prevalence is higher among white and black persons compared with Mexican Americans, and it has an association with fissured tongue and an inverse association with cigarette smoking.20
Figure 3.
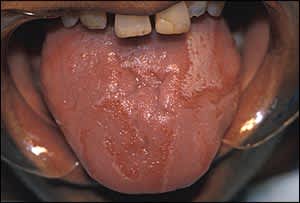
Geographic tongue. Sharply defined demarcation of inflammation is characteristic.
With geographic tongue, the dorsal tongue develops areas of papillary atrophy that appear smooth and are surrounded by raised serpiginous borders. These regions of atrophy spontaneously resolve and migrate, giving the tongue a variegated appearance. The condition is benign and localized, generally requiring no treatment except reassurance. Some patients may have sensitivity to hot or spicy foods.16,21 Topical steroid gels (e.g., triamcinolone dental paste [Oralone]) and antihistamine mouth rinses (e.g., diphenhydramine elixir [Banophen], 12.5 mg per 5 mL diluted in a 1:4 ratio with water) can reduce tongue sensitivity.4,16,22
HAIRY TONGUE
Accumulation of excess keratin on the filiform papillae of the dorsal tongue leads to the formation of elongated strands that resemble hair. The color of the tongue can range from white or tan to black. Darker coloration results from the trapping of debris and bacteria in the elongated strands (Figure 4). This occurs most commonly in smokers and in persons with poor oral hygiene.3,23,24 Hairy tongue has been associated with use of certain antibiotic medications.24,25 Most patients are asymptomatic, but some have halitosis or abnormal taste. No treatment is required, but gentle daily debridement with a tongue scraper or soft toothbrush can remove keratinized tissue.2,24
Figure 4.
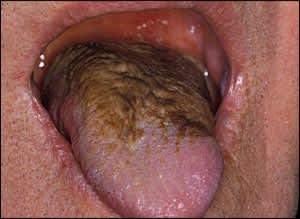
Hairy tongue. The dark coloration is caused by the trapping of debris and bacteria, which is worsened by smoking and poor oral hygiene.
ORAL HAIRY LEUKOPLAKIA
Oral hairy leukoplakia (Figure 5) differs from hairy tongue in its location and association with immunosuppression. The condition is characterized by white, hairy appearing lesions localized to the lateral margins of the tongue, in a unilateral or bilateral fashion. It is caused by Epstein-Barr virus infection.2,26 If oral hairy leukoplakia occurs in the absence of a known immunocompromising condition, HIV testing should be considered. Antiviral medications such as acyclovir (Zovirax; 800 mg five times per day) or ganciclovir (100 mg three times per day) for one to three weeks may be used, although recurrence is common.2,26
Figure 5.
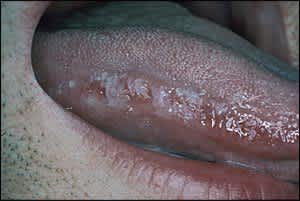
Oral hairy leukoplakia. The lateral tongue location differentiates this condition from hairy tongue. Biopsy is needed if squamous cell carcinoma is suspected.
LICHEN PLANUS
Lichen planus is an immunologic condition that affects skin or mucosal surfaces, such as the mouth and tongue (Figure 6). Two manifestations of lichen planus have been described: a reticular, white, lacy pattern that affects the buccal mucosa of the tongue and an erosive form that appears as shallow ulcerations. Candida can coexist with lichen planus and requires treatment with an antifungal agent. Reticular lichen planus does not require treatment. Ulcerative lichen planus can be treated with topical steroids, such as fluocinonide dental paste or clobetasol gel (Temovate) applied twice per day for two to three weeks.27 Biopsy is indicated if the diagnosis is unclear.
Figure 6.
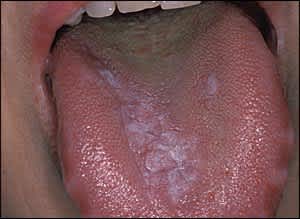
Lichen planus. This condition is of unknown etiology, although a scraping should be performed to exclude candidal infection, and biopsy can aid diagnosis.
LINEA ALBA
Linea alba appears as a thin white line caused by thickening of the epithelium from recurrent low-grade trauma from chewing. Although usually located on the buccal mucosa, it may occur on the bilateral edges of the tongue. Linea alba is benign, and no therapy is indicated.
Tongue Growths
GRANULAR CELL TUMORS
Granular cell tumors are small, solitary, firm, painless tumors that can occur throughout the body. More than one half of cases occur in the oral cavity, and up to one third involve the dorsum of the tongue.28 In contrast to squamous cell cancers, which have a rough or ulcerated surface, granular cell tumors have a smooth surface. These tumors are more common after 30 years of age and in women.28 Biopsy is needed to confirm the diagnosis. Rarely, malignant transformation occurs requiring wide local excision.29
TRAUMATIC FIBROMA
Traumatic fibroma (Figure 7) is a common lesion of the oral cavity. It usually appears along the bite line as a focal, thickened area that is typically dome shaped, pink, and smooth. It is caused by the accumulation of dense, collagenous connective tissue at the site of chronic irritation. Because it can be difficult to differentiate this lesion from other neoplasms, excisional biopsy is indicated. Chronic trauma can also precipitate the development of pyogenic granulomas at the site of traumatic fibromas.30
Figure 7.
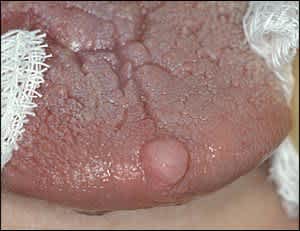
Traumatic fibroma. Biopsy is necessary to differentiate from other neoplasms.
LEUKOPLAKIA AND ERYTHROPLAKIA
Leukoplakia is a white adherent patch or plaque that can occur on the tongue. Erythroplakia is a similar lesion that is red in appearance. A lesion with a combined white and red speckled appearance is referred to as erythroleukoplakia.31 These lesions all have premalignant potential; therefore, biopsy and microscopic analysis are recommended. The risk of premalignancy is higher with erythroplakia and erythroleukoplakia.31–33 The premalignant potential of leukoplakia increases with age, and with size and number of lesions. The risk is also higher in women, and in persons with lesions located on the tongue or floor of the mouth or that have a nonhomogenous or speckled appearance.32,33 The most common factor associated with leukoplakia is tobacco use, and the condition may spontaneously resolve after tobacco cessation.31–33
SQUAMOUS CELL CARCINOMA
Risk factors for squamous cell carcinoma include older age, tobacco use, and alcohol use.34 Intraoral squamous cell carcinoma commonly involves the lateral surface of the tongue (Figure 8). Patients younger than 40 years who develop intraoral squamous cell carcinoma often do not have risk factors.34,35 Initially, lesions appear as a slight thickening over a red or white base. This may lead to nodularity or ulceration, causing pain and discomfort. Biopsy is critical to confirm the diagnosis and allow for prompt treatment before extensive local invasion occurs. Treatment typically requires surgery and radiation therapy.36
Figure 8.
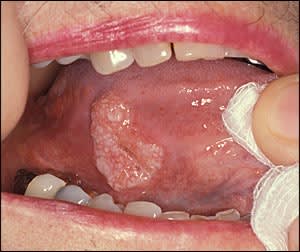
Squamous cell carcinoma. The lack of an erythematous halo and its rough surface help differentiate this condition from an aphthous ulcer.
LINGUAL THYROID NODULE
Almost 90 percent of ectopic thyroid tissue is associated with the dorsum of the tongue. It typically appears as a smooth nodular mass of tissue located in the midline of the posterior dorsal surface of the tongue.37 The presence of a lingual thyroid reflects the lack of descent of thyroid tissue during development. Up to 70 percent of patients with a lingual thyroid have hypothyroidism.38 Some patients have a sensation of a lump or difficulty swallowing. Symptoms are more common during increased metabolic demand, such as in adolescence or pregnancy.39 If hypothyroidism is present, thyroid replacement can decrease the size of the lingual thyroid and improve obstructive symptoms. Surgical excision is often advised for patients with a lingual thyroid and normal thyroid function; however, this may lead to a need for postoperative thyroid replacement because the lingual thyroid is usually the only functioning thyroid tissue in these patients.38
LYMPHOEPITHELIAL CYSTS
Lymphoepithelial cysts are yellowish nodules located on the ventral surface of the tongue, tonsillar region, or floor of the mouth. They are benign and thought to arise from the entrapment of salivary epithelium in lymphoid aggregates during embryogenesis.40 Biopsy is required to confirm the diagnosis.
PAPILLOMA
Squamous papilloma is one of the more common oral lesions, occurring in up to 1 percent of adults. It is generally associated with human papillomavirus type 6 or 11 infection.41 Papillomas typically appear as a single, isolated, pedunculated lesion with finger-like projections. Treatment involves surgical excision or laser ablation.
Burning Tongue
A burning sensation of the tongue can represent a primary syndrome, or it can be secondary to a condition that leads to the denudation of the normal tongue surface (e.g., candidal infection, vitamin deficiency). Burning tongue has an unknown etiology and seems to affect women seven times more often than men.42,43 Prevalence rates vary from 0.7 to 15 percent.44 Patients typically describe sudden onset of a sensation similar to that of a scalded tongue that becomes more frequent over the course of the day. The tongue often appears normal.42 The condition is benign and typically resolves spontaneously after many years.42,45 Only alpha-lipoic acid, clonazepam (Klonopin), and cognitive behavior therapy have been shown to reduce symptoms in controlled trials.44 In refractory cases, an approach similar to that for any chronic neuralgic pain can be helpful.42
Anatomic Tongue Abnormalities
TONGUE-TIE (ANKYLOGLOSSIA)
Tongue-tie, also called ankyloglossia, is a congenital condition caused by an abnormally short lingual frenulum that limits tongue protrusion. In the past, it was thought that tongue-tie rarely caused feeding problems. However, the increasing popularity of breastfeeding, which requires more oral work by the infant than bottle feeding, brought this idea into question.46 Several randomized trials have shown that in infants with tongue-tie and breastfeeding problems, frenulectomy is superior to education and lactation support alone.7,47,48
MACROGLOSSIA
Macroglossia is an abnormal enlargement of the tongue compared with the mouth and jaws. Examination often reveals a scalloping appearance on the lateral margins of the tongue caused by crowding against the teeth.2 Macroglossia is associated with Down syndrome, hypothyroidism, tuberculosis, sarcoidosis, amyloidosis, multiple myeloma, neurofibromatosis, infection (e.g., syphilis), and angioedema or allergic reaction.2,49 It is important to consider macroglossia as a sign of an underlying disorder and proceed with focused diagnostic testing, including possible biopsy. Treatment should be directed at the underlying disorder.
Referral
Patients with a tongue lesion of unclear etiology can be referred to an oral and maxillofacial surgeon, head and neck surgeon, or a dentist experienced in oral pathology.

