Peripheral neuropathy has a variety of systemic, metabolic, and toxic causes. The most common treatable causes include diabetes mellitus, hypothyroidism, and nutritional deficiencies. The diagnosis requires careful clinical assessment, judicious laboratory testing, and electrodiagnostic studies or nerve biopsy if the diagnosis remains unclear. A systematic approach begins with localization of the lesion to the peripheral nerves, identification of the underlying etiology, and exclusion of potentially treatable causes. Initial blood tests should include a complete blood count, comprehensive metabolic profile, and measurement of erythrocyte sedimentation rate and fasting blood glucose, vitamin B12, and thyroid-stimulating hormone levels; specialized tests should be ordered if clinically indicated. Lumbar puncture and cerebrospinal fluid analysis may be helpful in the diagnosis of Guillain-Barré syndrome and chronic inflammatory demyelinating neuropathy. Electrodiagnostic studies, including nerve conduction studies and electromyography, can help in the differentiation of axonal versus demyelinating or mixed neuropathy. Treatment should address the underlying disease process, correct any nutritional deficiencies, and provide symptomatic treatment.
The peripheral nerves consist of bundles of long neuronal axons as they exit the central nervous system (CNS). Some peripheral nerves are wrapped in a myelin sheath generated by Schwann cells, whereas others are unmyelinated. Peripheral nerves serve different motor, sensory, and autonomic functions. The term peripheral neuropathy is usually used to describe symmetric and universal damage to adjacent nerves. The damage and clinical manifestations are usually located distally with a proximal progression. Several disorders can damage peripheral nerves and cause peripheral neuropathy; it is important to differentiate actual neuropathy from other disorders that can have a similar clinical presentation.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Initial evaluation of a patient with peripheral neuropathy should include a complete blood count, comprehensive metabolic profile, and measurement of erythrocyte sedimentation rate and fasting blood glucose, vitamin B12, and thyroid-stimulating hormone levels. | C | 5 |
| Electrodiagnostic studies are recommended if symptoms persist and if the diagnosis remains unclear after initial diagnostic testing and a careful history and physical examination. | C | 4, 5 |
| Options for symptomatic treatment of peripheral neuropathy include antiseizure medications, tricyclic antidepressants, and topical medications. | B | 13–18 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Epidemiology
One study estimated that the prevalence of peripheral neuropathy in the family medicine setting is 8 percent in persons 55 years and older.1 The prevalence in the general population may be as high as 2.4 percent.2 A community-based study estimated the prevalence of peripheral neuropathy in patients with type 2 diabetes mellitus to be 26.4 percent.3
Diagnosis
Peripheral neuropathy can be caused by a variety of systemic diseases, toxic exposures, medications, infections, and hereditary disorders (Table 1). The most common treatable causes are diabetes, hypothyroidism, and nutritional deficiencies.
Table 1. Causes of Peripheral Neuropathy
| Cause | Type of neuropathy | Comments | Laboratory tests | ||
|---|---|---|---|---|---|
| Diseases | |||||
| Acquired immunodeficiency syndrome | A | Mainly sensory | Human immunodeficiency virus test | ||
| Carcinoma (paraneoplastic syndrome) | A | Usually sensory | Paraneoplastic panel (anti-Hu, anti-Yo, anti-Ri, anti-Tr, anti-Ma, and anti-CV2 antibodies) | ||
| Chronic liver disease | M | Mainly demyelinating, especially in viral hepatitis | Hepatic transaminase, bilirubin, albumin, and alkaline phosphatase levels | ||
| Critical illness neuropathy | A | Usually acute or subacute | No specific laboratory test | ||
| Diabetes mellitus | M | Chronic; axonal may predominate | Fasting blood glucose level, glucose tolerance test, A1C level | ||
| End-stage renal disease | A | — | Serum creatinine and blood urea nitrogen levels | ||
| Hypothyroidism | A | Usually acute or subacute, but can be chronic | Thyroid-stimulating hormone level | ||
| Leprosy | A | Usually sensory | Phenolic glycolipid-1 antibody, skin biopsy | ||
| Lyme disease | A | — | Lyme titers | ||
| Lymphoma | M | Mainly axonal | CBC, imaging | ||
| Monoclonal gammopathy | Usually chronic | Urine and serum protein electrophoresis with immunofixation | |||
| Amyloidosis | A | Usually sensory | |||
| Multiple myeloma | M | Axonal damage predominates after treatment | |||
| Plasmacytoma (osteosclerotic myeloma) | D | May have some axonal damage | |||
| Monoclonal gammopathy of undetermined significance | |||||
| IgM | D | Most common; may have some axonal damage | |||
| IgG or IgA | M | Demyelinating features often predominate | |||
| Porphyria | A | Acute | Porphyrin titers | ||
| Syphilis | A | — | Rapid plasma reagin, VDRL, cerebrospinal fluid analysis | ||
| Vitamin B6 deficiency | A | Sensory more than motor | Vitamin B6 level | ||
| Vitamin B12 deficiency | A | Peripheral neuropathy is intermixed with upper motor neuron signs | CBC; vitamin B12 and homocysteine levels; methylmalonic acid test | ||
| Drugs* | |||||
| Amiodarone (Cordarone) | M | Mainly axonal with sensorimotor | No specific tests | ||
| Chloroquine (Aralen) | D | May have some axonal damage | |||
| Digoxin | A | Mainly sensory | |||
| Heroin | A | Sensorimotor | |||
| Hydralazine | A | Mainly sensory | |||
| Isoniazid | A | Mainly sensory | |||
| Lithium | A | Sensorimotor | |||
| Metronidazole (Flagyl) | A | Mainly sensory | |||
| Misoprostol (Cytotec) | A | Motor | |||
| Nitrofurantoin (Furadantin) | A | Sensorimotor | |||
| Phenytoin (Dilantin) | A | Mainly sensory | |||
| Procainamide (Pronestyl) | D | May have some axonal damage | |||
| Statins | A | Mainly sensory | |||
| Vincristine (Oncovin) | A | Sensorimotor | |||
| Vitamin B6 excess | A | Mainly sensory | |||
| Genetic disorders† | |||||
| Charcot-Marie-Tooth disease | Genetic testing | ||||
| Type 1 | D | Also called HMSN-I | |||
| Type 2 | A | Also called HMSN-II | |||
| Metachromatic leukodystrophy | D | — | |||
| Neuropathy with liability to pressure palsies | D | — | |||
| Refsum disease | D | Also called HMSN-IV | |||
| Toxins* | |||||
| Diphtheria toxin | D | Acute presentation | Histopathology | ||
| Ethanol (alcohol) | A | Sensorimotor | No specific or practical laboratory test | ||
| Heavy metals (e.g., arsenic, lead, mercury, gold) | A | Lead and mercury mainly cause motor neuropathy | 24-hour urine collection for heavy metal titers | ||
| Arsenic causes sensorimotor neuropathy | |||||
| Gold may cause some demyelination | |||||
| Organophosphates | A | Sensorimotor | No specific or practical laboratory test | ||
| Tetanus | A | Motor; acute presentation | No specific or practical laboratory test | ||
| Tic paralysis | A | Motor; acute presentation | No specific or practical laboratory test | ||
| Other causes | |||||
| Idiopathic polyneuropathy | A | Diagnosis of exclusion; usually chronic | No laboratory test | ||
A = axonal; CBC = complete blood count; D = demyelinating; HMSN = hereditary motor-sensory neuropathy; Ig = immunoglobulin; M = mixed; VDRL = Venereal Disease Research Laboratory.
*—Usually acute or subacute, but can be chronic.
†—Usually chronic.
HISTORY AND PHYSICAL EXAMINATION
When a patient presents with symptoms of distal numbness, tingling and pain, or weakness, the first step is to determine whether the symptoms are the result of peripheral neuropathy or of a lesion in the CNS, and whether a single nerve root, multiple nerve roots, or a peripheral nerve plexus is involved. CNS lesions may be associated with other features, such as speech difficulty, double vision, ataxia, cranial nerve involvement, or, in cases of myelopathy, impairment of bowel and bladder functions. Deep tendon reflexes are usually brisk, and muscle tone is spastic. Lesions of the peripheral nerve roots are typically asymmetric, follow a dermatomal pattern of sensory symptoms, and may have associated neck and low back pain. Lesions of the plexus are asymmetric with sensorimotor involvement of multiple nerves in one extremity.
A 128-Hz tuning fork should be used to test the vibratory sensations in extremities. Loss of sensation (including vibration, proprioception, temperature, and pinprick sensations) in distal extremities suggests peripheral neuropathy, as does a distal-to-proximal gradient of reflex elicitation.
Once the lesion has been localized to peripheral nerves, the next step is to find the etiology and exclude potentially treatable causes, such as acquired toxic, nutritional, inflammatory, or immune-mediated demyelinating disorders. The neuropathies must be further characterized by onset and chronicity of symptoms, the pattern and extent of involvement, and the type of nerve fibers involved (i.e., sensory, motor, or autonomic).
In the early stages of peripheral neuropathy, patients typically present with progressive symptoms, including sensory loss, numbness, and pain or burning sensations in distal limbs in a “stocking and glove” distribution. Over time, the numbness may extend proximally, and mild distal muscle weakness and atrophy may occur. In disorders that cause acute peripheral neuropathy, such as those produced by toxic exposures, patients may present with similar but more fulminant symptoms, and pain predominates; symptoms also typically have a faster progression. In other disorders, such as acute inflammatory demyelinating disorder (i.e., Guillain-Barré syndrome) and chronic inflammatory demyelinating polyneuropathy, weakness rather than sensory loss typically predominates and may be the earliest sign of the disease.
The presence of neuropathic symptoms, decreased ankle reflexes, and decreased distal sensations, regardless of distal muscle weakness and atrophy, makes the diagnosis of peripheral neuropathy likely.4 The isolated presence of neuropathic symptoms or decreased ankle reflexes is less valuable for diagnosis. Some causes of peripheral neuropathy are characterized by mononeuropathy, some involve multiple nerves, and others have autonomic dysfunction or pain prominence (Table 2).
Table 2. Causes of Peripheral Neuropathy Based on Clinical Presentation
| Conditions causing mononeuropathy | |
| Acute (trauma-related) | |
| Chronic (nerve entrapment) | |
| Disorders causing mononeuropathy multiplex | |
| Acute | |
| Diabetes mellitus* | |
| Multifocal motor neuropathy | |
| Vasculitic syndromes | |
| Chronic | |
| Acquired immunodeficiency syndrome | |
| Leprosy* | |
| Sarcoidosis | |
| Conditions causing neuropathy with autonomic features | |
| Alcoholism | |
| Amyloidosis | |
| Chemotherapy-related neuropathy | |
| Diabetes | |
| Heavy metal toxicity | |
| Porphyria | |
| Primary dysautonomia | |
| Vitamin B12 deficiency | |
| Conditions causing painful neuropathy | |
| Alcoholism | |
| Amyloidosis | |
| Chemotherapy (heavy metal toxicity) | |
| Diabetes | |
| Idiopathic polyneuropathy | |
| Porphyria | |
| Paraneoplastic syndrome | |
*—May cause symmetric peripheral neuropathy.
DIAGNOSTIC TESTING
The evaluation of a patient with peripheral neuropathy starts with simple blood tests, including a complete blood count, comprehensive metabolic profile, and measurement of erythrocyte sedimentation rate and fasting blood glucose, vitamin B12, and thyroid-stimulating hormone levels5 (Figure 1). Additional tests, if clinically indicated, may include a paraneoplastic panel to evaluate for occult malignancy; antimyelin-associated glycoprotein antibodies to evaluate for sensorimotor neuropathies; antiganglioside antibodies; cryoglobulins; cerebrospinal fluid (CSF) analysis to evaluate for chronic inflammatory demyelinating neuropathy; antisulfatide antibodies to evaluate for auto-immune polyneuropathy; and genetic testing if hereditary peripheral neuropathy is suspected (Table 3).
Figure 1. Diagnosis of the Patient with Suspected Peripheral Neuropathy
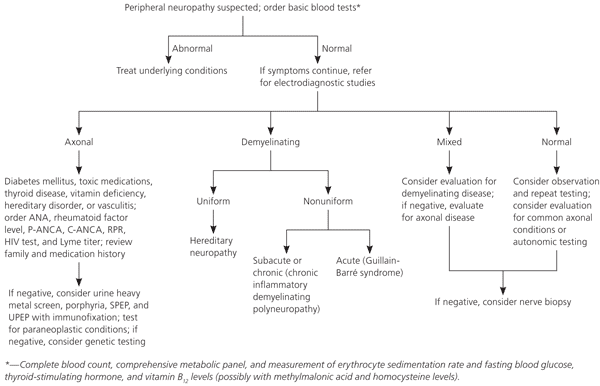
Approach to the patient with peripheral neuropathy. (ANA = antinuclear antibodies; C-ANCA = cytoplasmic anti-neutrophil cytoplasmic antibodies; HIV = human immunodeficiency virus; P-ANCA = perinuclear antineutrophil cytoplasmic antibodies; RPR = rapid plasma reagin; SPEP = serum protein electrophoresis; UPEP = urine protein electrophoresis.)
Table 3. Tests Indicated in Patients with Peripheral Neuropathy
| Tests | Clinical disorders |
|---|---|
| Routine | |
| Complete blood count | — |
| Comprehensive metabolic panel | — |
| Erythrocyte sedimentation rate | — |
| Fasting blood glucose level | — |
| Thyroid-stimulating hormone level | — |
| level | — |
| Vitamin B12 | |
| If indicated by clinical suspicion | |
| Glucose tolerance test, A1C level | Diabetes mellitus |
| HIV antibodies | HIV |
| Hepatic panel | Liver disorders |
| Lyme antibodies | Lyme disease |
| Rapid plasma reagin, VDRL | Syphilis |
| Urinalysis (including 24-hour urine collection) | Heavy metal toxicity, porphyrias, multiple myeloma |
| Urine and serum protein electrophoresis with immunofixation | Demyelinating neuropathy |
| Angiotensin-converting enzyme levels | Sarcoidosis |
| Antinuclear antibodies, P-ANCA, C-ANCA | Vasculitis |
| Tests for uncommon conditions | |
| Paraneoplastic panel | Underlying malignancy |
| Antimyelin-associated glycoprotein and antiganglioside antibodies | Sensorimotor neuropathy |
| Antisulfatide antibodies | Autoimmune polyneuropathy |
| Cryoglobulins | Cryoglobulinemia |
| Salivary flow rate, Schirmer test, rose bengal test, labial gland biopsy | Sjögren syndrome |
| Cerebrospinal fluid analysis | Acute or chronic inflammatory demyelinating neuropathy |
| Genetic testing | Hereditary neuropathy |
note: Tests are listed in the approximate frequency of the potential underlying disorder.
C-ANCA = cytoplasmic antineutrophil cytoplasmic antibodies; HIV = human immunodeficiency virus; P-ANCA = perinuclear antineutrophil cytoplasmic antibodies; VDRL = Venereal Disease Research Laboratory.
Lumbar puncture and CSF analysis may be helpful in diagnosing Guillain-Barré syndrome and chronic inflammatory demyelinating neuropathy; CSF protein levels may be elevated in patients with these conditions.6,7
ELECTRODIAGNOSTIC STUDIES
Electrodiagnostic studies are recommended if the diagnosis remains unclear after initial diagnostic testing and a careful history and physical examination.4,5 There are two primary types of electrodiagnostic studies: nerve conduction studies and electromyography (EMG). Nerve conduction studies assess the shape, amplitude, latency, and conduction velocity of an electrical signal conducted over the tested nerve. Axonal loss leads to lower amplitudes, and demyelination causes prolonged latency and slow conduction velocity. EMG can detect active axonal damage, as evidenced by the presence of spontaneous muscle fiber activity at rest resulting from the absence of neuro-regulation (denervation). The motor unit action potential on voluntary muscle contraction also is assessed. In neuropathic conditions, reinnervation changes are recorded, the details of which are beyond the scope of this article.
Electrodiagnostic studies can help determine whether the neuropathy is the result of damage to the axons (axonal neuropathy) or the myelin (demyelinating neuropathy), or both (mixed). Normal nerve conduction studies and needle EMG significantly decrease the likelihood of peripheral neuropathy, whereas abnormal nerve conduction findings confirm the diagnosis.
A potential limitation of electrodiagnostic studies is that they are able to test only the large, myelinated nerve fibers. This limits their sensitivity in detecting neuropathies of the small nerve fibers (i.e., those with pain, temperature, and autonomic functions). In these cases, a specialized test directed at autonomic functions, and other non-electrodiagnostic tests (e.g., epidermal skin biopsy) may yield the diagnosis.
NERVE BIOPSY
Nerve biopsy should be considered when the diagnosis remains uncertain after laboratory and electrodiagnostic testing, or when confirmation of the diagnosis is needed before initiating aggressive treatment (e.g., in cases of vasculitis when steroids or chemotherapy is used). Sural and superficial peroneal nerves are preferred for biopsy. When all investigations fail to identify a cause and electrodiagnostic studies show axonal-type symmetric peripheral neuropathy, idiopathic peripheral neuropathy is the presumptive diagnosis. Epidermal skin biopsy can be performed in patients with burning, numbness, and pain, and in whom small, unmyelinated nerve fibers are suspected to be the cause. Small nerve fiber damage may constitute the earliest stages of some peripheral neuropathies and cannot be detected by electrodiagnostic studies.2,5
Principles of Treatment
Treatment of peripheral neuropathy has two goals: controlling the underlying disease process and treating troublesome symptoms. The former is usually achieved by eliminating offending agents, such as toxins or medications; correcting a nutritional deficiency; or treating the underlying disease (e.g., corticosteroid therapy for immune-mediated neuropathy).8 These steps are important to halt the progression of neuropathy, and they may improve symptoms.
Acute inflammatory neuropathies require more urgent and aggressive management with intravenous immunoglobulin9 or plasmaphereis.10 In addition, respiratory function testing and hemodynamic monitoring are warranted. Mechanical ventilation should be considered in patients whose forced vital capacity is less than 20 mL per kg or is reduced by more than 30 percent of baseline, or if maximal inspiratory pressure is less than 30 cm of water.11
It is important to help patients control troublesome symptoms of peripheral neuropathy, such as severe numbness and pain, as well as to alleviate disability resulting from weakness.12 Several pharmacologic options exist to treat neuropathic pain, including some antiseizure medications (e.g., gabapentin [Neurontin], topiramate [Topamax], carbamazepine [Tegretol], pregabalin [Lyrica])13,14 and antidepressants (e.g., amitriptyline).15–17 Topical patches and sprays containing lidocaine (Lidoderm) or capsaicin (Zostrix) also may relieve pain in some patients.18 Other supportive measures, such as foot care, weight reduction, and shoe selection, may also be helpful.2 Narcotics may have a role in the treatment of chronic neuropathic pain in selected patients19; candidates initially should be evaluated for their risk of substance abuse and addiction, and several nonnarcotic regimens should be tried first. A second opinion regarding the patient's diagnosis and management also should be considered before initiating long-term opioid therapy.

