A 45-year-old woman presented with a spontaneous bullous eruption on her trunk and extremities that appeared three months earlier. The lesions were occasionally pruritic. She had no fever, chills, or other systemic symptoms. The lesions did not improve after multiple courses of antibiotics, including amoxicillin, cephalexin (Keflex), and cefoxitin. The patient had type 2 diabetes mellitus that was diagnosed three years earlier. Although she was taking metformin (Glucophage), her blood glucose level was not adequately controlled (A1C level of 11 percent). None of her close contacts had a history of similar lesions.
Physical examination revealed pus-containing bullae, 1 to 3 cm in diameter, on an erythematous base (Figures 1 and 2). Some lesions exhibited pooling of fluid in the lower half of the bullae. Other lesions had ruptured, leaving erythematous, tender, and crusted plaques. There was no regional lymphadenopathy.
Figure 1.
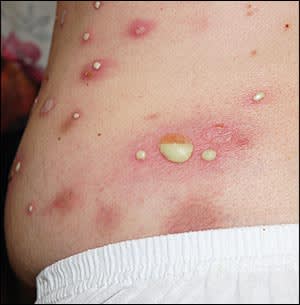
Figure 2.
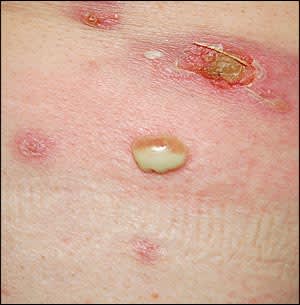
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Bacterial folliculitis.
B. Bullous impetigo.
C. Pemphigus vulgaris.
D. Pustular psoriasis.
E. Subcorneal pustular dermatosis.
Discussion
The correct answer is B: bullous impetigo. Bullous impetigo usually occurs in children younger than two years, but older children and immunocompromised adults may also be affected.1–3 Bullous impetigo is caused by exfoliative toxins produced by Staphylococcus aureus. Skin swabs from this patient showed methicillin-resistant S. aureus (MRSA) sensitive only to clindamycin (Cleocin) and vancomycin.
Bullae usually arise on areas of grossly normal skin, and are characterized initially by clear yellow fluid that subsequently becomes turbid and sometimes pustular. Within a few days, the fragile bullae rupture, forming light brown or golden yellow crusts. Fever, diarrhea, and generalized weakness may be present, but regional lymphadenopathy is often absent. If left untreated, the infection may spread to deeper skin and cause lymphangitis and septicemia. Infants and adults who are immunocompromised or have impaired renal function are especially at risk of progression to staphylococcal scalded skin syndrome.1–3
The infection is transmitted through direct contact with the organism or through contact with contaminated fomites, including clothing and toys. After two weeks of treatment with oral clindamycin and tighter control of her blood glucose level, the patient's lesions resolved completely. Extensive cases may require systemic antibiotics. A follow-up examination is required if lesions do not resolve within seven days of treatment.
MRSA-related bullous impetigo showing borderline-to-moderate resistance to betalactam antibiotics is an emerging problem. Isolation of MRSA from bullous impetigo lesions has been reported in 20 to 50 percent of cases.4–7
Like bullous impetigo, bacterial folliculitis is often caused by S. aureus. However, bacterial folliculitis appears as follicular papulopustules. The condition can occur at any age.
Pemphigus vulgaris is an autoimmune blistering disease that usually involves the skin and mucous membranes. It generally occurs in persons older than 40 years. Histology reveals suprabasal blister formation, and results of direct immunofluorescence are distinctive.3 Bacterial culture results are usually negative unless the lesions are secondarily infected.
Pustular psoriasis is characterized by small sterile pustules on an erythematous base, occasionally in annular configurations. Triggering factors include pregnancy and rapid corticosteroid tapering. A personal or family history of psoriasis is common.
Subcorneal pustular dermatosis is a rare idiopathic, chronic, pustular eruption that commonly affects women older than 40 years.8 The conditions may be clinically indistinguishable from bullous impetigo. The primary lesions are small pustules that appear in crops over the trunk and proximal extremities and that often coalesce in annular, circinate, or serpiginous patterns. After a few days, the pus-containing pustules rupture and form superficial crusts. Unlike bullous impetigo, however, cultures of the pustules do not show bacterial growth.8
Summary Table
| Condition | Characteristics |
|---|---|
| Bacterial folliculitis | Follicular papulopustules, usually secondary to Staphylococcus aureus infection; more severe cases may lead to furuncles, carbuncle, and abscess |
| Bullous impetigo | Usually occurs in children and immunocompromised adults; bullae characterized by yellow fluid that becomes turbid and sometimes pustular; light brown or golden yellow crusting |
| Pemphigus vulgaris | Generally occurs in persons older than 40 years; mucosal and cutaneous erosions and blisters; autoimmune disease with autoantibodies; positive results on direct immunofluorescence |
| Pustular psoriasis | Can occur at any age; extensive small sterile pustules on an erythematous base; occasionally annular configurations; triggered by pregnancy or rapid corticosteroid tapering; personal or family history of psoriasis is common |
| Subcorneal pustular dermatosis | Most common in women older than 40 years; small pustules that appear in crops over the trunk and proximal extremities and that often coalesce in annular, circinate, or serpiginous patterns |

