Serotonin syndrome is a potentially life-threatening condition caused by excessive serotonergic activity in the nervous system. It is characterized by mental status changes, autonomic instability, and neuromuscular hyperactivity. Most reported cases of serotonin syndrome are in patients using multiple serotonergic drugs or who have had considerable exposure to a single serotonin-augmenting drug. Diagnosis is made using the Hunter Serotonin Toxicity Criteria, which require the presence of one of the following classical features or groups of features: spontaneous clonus; inducible clonus with agitation or diaphoresis; ocular clonus with agitation or diaphoresis; tremor and hyperreflexia; or hypertonia, temperature above 100.4° F (38° C), and ocular or inducible clonus. Most cases of serotonin syndrome are mild and may be treated by withdrawal of the offending agent and supportive care. Benzodiazepines may be used to treat agitation and tremor. Cyproheptadine may be used as an antidote. Patients with moderate or severe cases of serotonin syndrome require hospitalization. Critically ill patients may require neuromuscular paralysis, sedation, and intubation. If serotonin syndrome is recognized and complications are managed appropriately, the prognosis is favorable.
Serotonin syndrome is a potentially life-threatening set of symptoms caused by serotonin toxicity, and usually involves a combination of drugs that increase serotonergic transmission. This syndrome was first described in the literature during the 1960s in studies of single and combination therapy with antidepressant medications.1 Potential mechanisms of serotonin syndrome include increased serotonin synthesis or release; reduced serotonin uptake or metabolism; and direct serotonin receptor activation.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Prevention of serotonin syndrome requires clinical awareness of the toxic potential of serotonergic agents. | C | 1 | Education and use of drug interaction software may be helpful |
| Established criteria should be used to identify and diagnose serotonin syndrome. | C | 1, 14 | Hunter Serotonin Toxicity Criteria are more sensitive and specific than Sternbach's criteria in diagnosing serotonin syndrome |
| First-line management of serotonin syndrome involves withdrawal of the offending drugs and provision of supportive care. | C | 19 | — |
| Cyproheptadine may be used to treat moderate to severe cases of serotonin syndrome. | C | 19, 20 | Based on case reports |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Definition and Etiology
Serotonin syndrome is defined as excessive serotonergic activity in the central and peripheral nervous systems. Classical clinical features include a combination of mental status changes, autonomic instability, and neuromuscular hyperactivity.2–4 The intensity of clinical findings reflects the degree of serotonin toxicity. The term “serotonin syndrome” usually refers to the severe end of the toxicity spectrum.
Serotonin syndrome can occur with any increase in serotonergic neurotransmission. The majority of cases are iatrogenic from synergistic medication use, although cases of intentional self-poisoning with serotonergic agents also occur.5,6 Another mechanism for development of serotonin syndrome is the addition of drugs that inhibit the cytochrome P450 2D6 and/or 3A4 (CYP3A4) isoenzymes to therapeutic regimens of selective serotonin reuptake inhibitors (SSRIs). In one case report, serotonin syndrome was precipitated in a 12-year-old patient taking a stable dosage of sertraline (Zoloft) when erythromycin, a CYP3A4 inhibitor, was also prescribed.7 A remarkable number of drugs from different classes have been implicated as causing serotonin syndrome (Table 1).1,3,8–10 Most reported cases are in patients taking multiple serotonergic agents or who have had considerable exposure to a single serotonin-augmenting drug.11
Table 1. Medications that May Contribute to Serotonin Syndrome
| Amphetamines and derivatives 3,4-methylenedioxymethamphetamine (Ecstasy) Dextroamphetamine Methamphetamine Sibutramine (Meridia) Analgesics Cyclobenzaprine (Flexeril) Fentanyl (Duragesic) Meperidine (Demerol) Tramadol (Ultram) Antidepressants/mood stabilizers Buspirone (Buspar) Lithium Monoamine oxidase inhibitors (e.g., phenelzine [Nardil]) Selective serotonin reuptake inhibitors (e.g., fluoxetine [Prozac]) Serotonin-norepinephrine reuptake inhibitors (e.g., venlafaxine [Effexor]) Serotonin 2A receptor blockers (e.g., trazodone) St. John's wort (Hypericum perforatum) Tricyclic antidepressants (e.g., amitriptyline, nortriptyline [Pamelor]) Antiemetics Metoclopramide (Reglan) Ondansetron (Zofran) Antimigraine drugs Carbamazepine (Tegretol) Ergot alkaloids Triptans Valproic acid (Depakene) Miscellaneous Cocaine Dextromethorphan Linezolid (Zyvox) L-tryptophan 5-hydroxytryptophan |
Incidence
The incidence of serotonin syndrome is rising, reflecting the growing number of serotonergic drugs available and the increased use of these agents in clinical practice. The reported incidence may also reflect an increasing diagnostic awareness of the syndrome (Table 2).12,13 Because many cases go unrecognized, the true incidence of serotonin syndrome is unknown.
Table 2. SSRI Ingestions Reported to U.S. Poison Control Centers
| Ingestions | 2002 | 2005 |
|---|---|---|
| Total exposures reported | 46,244 | 48,279 |
| Moderate to major effects* | 7,349 (16 percent) | 8,585 (18 percent) |
| Deaths | 93 (0.2 percent) | 118 (0.2 percent) |
SSRI = selective serotonin reuptake inhibitor.
*—Moderate effects are defined as prolonged, pronounced, or systemic effects requiring treatment but are not considered life threatening. Major effects are defined as signs or symptoms that are life threatening or that lead to significant disability.
Prevention
Prevention of serotonin syndrome begins with awareness by physicians and patients of the potential for toxicity from serotonergic drugs.1 Avoiding the combined use of serotonin-augmenting drugs is essential. Physicians should modify prescribing practices to minimize coprescription of drugs known to have a high probability of inducing serotonin syndrome. A computerized ordering system and medical software can check for possible interactions when multi-drug regimens are required. Currently, there are no established guidelines for the prevention of serotonin syndrome. Eventually, the application of pharmacogenomic principles may help identify and protect patients at risk of serotonin syndrome before the administration of serotonergic agents.
Diagnosis
The diagnosis of serotonin syndrome depends on identifying autonomic instability, neuromuscular signs, and cognitive-behavioral changes in the presence of serotonergic medication use (Table 31,3,8,14 ).1,14 Symptoms occur most commonly after serotonergic medications are added to therapeutic SSRI regimens, when dosages are changed, or after an overdose of serotonergic agents. Symptoms can develop rapidly, often within minutes of drug ingestion, although most patients present within six to 24 hours after a medication change or overdose.15 It is important to note that serotonergic agents include nonprescription drugs, illicit drugs, and diet supplements (Table 1).1,3,8–10 A complete and accurate medication history is critical when making the diagnosis.
Table 3. Signs and Symptoms of Serotonin Syndrome
| Agitation (restlessness)* | |
| Diaphoresis* | |
| Diarrhea* | |
| Disseminated intravascular coagulation† | |
| Fever above 100.4° F (38° C) | |
| Hyperreflexia* | |
| Incoordination (ataxia)* | |
| Mental status changes | |
| Confusion* | |
| Hypomania* | |
| Multi-organ failure† | |
| Myoclonus* | |
| Ocular clonus | |
| Rhabdomyolysis† | |
| Shivering* | |
| Tonic-clonic seizures† | |
| Tremor* | |
*—Sternbach's diagnostic criteria require three of 10 signs and symptoms.
†—Extremely severe cases.
The clinical manifestations of serotonin syndrome are highly variable. The diagnosis should be based on the Hunter Serotonin Toxicity Criteria or Sternbach's criteria, although Hunter's criteria are more sensitive (84 versus 75 percent) and more specific (97 versus 96 percent) than Sternbach's.14 Hunter's criteria use decision rules for predicting serotonin toxicity in patients who are known to have taken a serotonergic agent (Figure 1).14 Diagnosis with Hunter's criteria requires one of the following features or groups of features: spontaneous clonus; inducible clonus with agitation or diaphoresis; ocular clonus with agitation or diaphoresis; tremor and hyperreflexia; or hypertonia, temperature above 100.4°F (38°C), and ocular or inducible clonus. Sternbach's criteria require three of 10 clinical features coincident with an addition or recent increase of known serotonergic drugs to an established medication regimen (Table 31,3,8,14 ). It is necessary to rule out initiation or change of dosage of dopaminergic drugs and other possibilities, such as infection, metabolic disorder, substance intoxication, or withdrawal.1,3,4,8,16
Figure 1. Hunter's Decision Rules for Diagnosis of Serotonin Toxicity
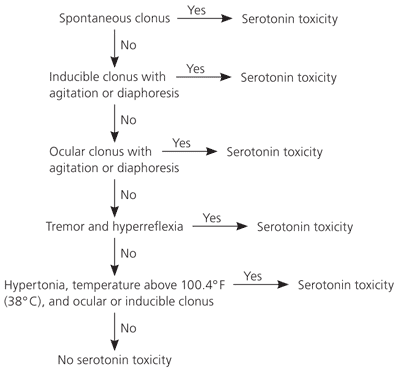
Hunter's decision rules for diagnosis of serotonin toxicity.
Adapted with permission from Dunkley EJ, Isbister GK, Sibbritt D, Dawson AH, Whyte IM. The Hunter Serotonin Toxicity Criteria; simple and accurate diagnositc decision rules for serotonin toxicity. QJM. 2003;96(9):639.
The primary differential diagnosis of serotonin syndrome includes anticholinergic syndrome, malignant hyperthermia, and neuroleptic malignant syndrome (Table 4).8,14,17,18 An accurate history of the drugs or substances ingested is helpful in ruling out these conditions. Other potential diagnoses may include tetanus, overdose of sympathomimetic drugs, meningitis, encephalitis, thyroid storm, heat stroke, delirium tremens, or sepsis.8,14,17,18 Laboratory tests and other diagnostic tests, such as imaging studies, may be ordered based on physical examination and medication history.3,8 There are no specific laboratory tests to diagnose serotonin syndrome; laboratory and other diagnostic testing are used to rule out alternative explanations of symptoms.
Table 4. Differential Diagnosis of Serotonin Syndrome
| Clinical condition | History | Vital signs | Clinical features |
|---|---|---|---|
| Anticholinergic syndrome | Use of tricyclic antidepressants or other anticholinergic drugs | Tachycardia, tachypnea, hyperthermia (usually 102.2°F [39°C] or below) | Dry mouth, blurred vision, mydriasis, flushed skin, agitation/delirium, decreased bowel sounds |
| Malignant hyperthermia | Administration of halogenated inhalational anesthetics or depolarizing muscle relaxants | Hypertension, tachycardia, tachypnea, hyperthermia (up to 114.8°F [46°C]) | Diaphoresis, mottled skin, agitation, decreased bowel sounds, muscular rigidity, hyporeflexia |
| Neuroleptic malignant syndrome | Ingestion of antipsychotic medications | Hypertension, tachycardia, tachypnea, hyperthermia (above 105.8°F [41°C]) | Sialorrhea, diaphoresis, pallor, stupor, mutism, coma, normal or decreased bowel sounds, lead-pipe rigidity, bradyreflexia |
Management
When serotonin syndrome is recognized promptly and its complications are treated appropriately, the prognosis is generally favorable. First-line management involves withdrawal of the offending serotonergic drugs and provision of supportive care. The intensity of treatment depends on the severity of the syndrome.19 Mild cases generally resolve within 24 to 72 hours with conservative therapy and removal of the causative drugs. Most patients with mild cases do not require hospital admission. Patients with moderate to severe cases involving hypertonicity, hyperthermia, autonomic instability, or progressive cognitive changes require hospitalization.3,8 Benzodiazepines may be used for control of agitation and tremor. Patients may also benefit from cyproheptadine, olanzapine (Zyprexa), or chlorpromazine. Chlorpromazine and olanzapine are not routinely used because of the potential for adverse effects and toxicity. Cyproheptadine, a serotonin 2A antagonist, is usually recommended and is the most widely used antidote.19,20 An initial dose of 12 mg should be considered, followed by an additional 2 mg every two hours if symptoms continue. After the patient is stabilized, a maintenance dosage of 8 mg every six hours may be administered. Although cyproheptadine is widely used, definitive evidence is lacking on its effectiveness in serotonin syndrome. The mainstays of therapy in managing hyperthermia and increased muscle rigidity in severely ill patients are neuromuscular paralysis, sedation, and possible intubation.

