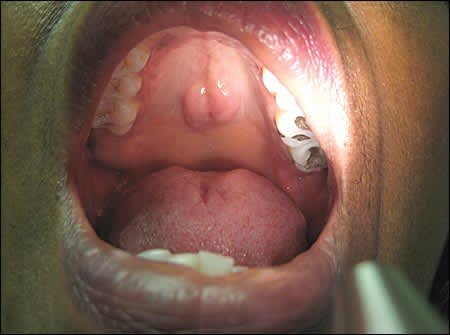
A 68-year-old woman presented with symptoms of upper respiratory tract infection. The physical examination revealed a firm, nontender midline nodule on her hard palate measuring 2 × 2 cm (see accompanying figure). The patient said that the nodule appeared suddenly, two weeks earlier. The lesion did not bleed or cause discomfort, and had not grown in size. She had no history of trauma to her mouth or tobacco use, and she did not use dentures or other oral prosthetics. She had no personal or family history of oral cancer.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Fibroma.
B. Mucocele.
C. Oral neurofibromatosis.
D. Palatine torus.
E. Pyogenic granuloma.
Discussion
The correct answer is D. Palatine torus. Tori are asymptomatic, benign bony prominences that can occur on the hard palate or the lingual aspect of the mandible.1 Palatine and mandibular tori are most common. There may be genetic and environmental factors in the development of tori, with familial occurrence suggesting an autosomal dominant inheritance.1,2 However, some studies suggest that eating tough food may put pressure on the medial palatine region, leading to the thickening of the palatal vault and the development of tori.1 Palatine tori tend to be flat, whereas mandibular tori are usually nodular.1 Most palatine tori are smaller than 2 cm, but the size may vary throughout the patient's life.
Prevalence of palatine tori is reported to be 20 to 25 percent in the United States. The peak incidence is between 20 and 30 years of age, and the condition is more common in women.3 There are conflicting data about the prevalence of palatine torus among ethnic groups. One study found little ethnic variation.1 However, another study found a slightly higher prevalence in Hispanics, followed by blacks and whites.4 Older age appears to be associated with larger tori size.3
Palatine tori are slow-growing, recurrent lesions without potential for malignant transformation,1 and therefore do not usually require treatment. However, tori may become large enough to interfere with function and denture placement.1 Tori may also cause obstructive sleep apnea. Surgical intervention may be needed if tori interfere with function, cause recurrent traumatic surface ulcerations, or occur in a patient requiring oral prosthodontics.1 Interestingly, harvesting bone from tori may be useful for bridge augmentation procedures to replace missing teeth, and as sources of cortical bone in periodontal surgery.1
Fibromas present as asymptomatic, smooth, firm nodules in response to trauma. They most often occur on the occlusal line of the buccal mucosa.5 Fibromas rarely recur after surgical removal.
Mucoceles present as bluish, dome-shaped mucosal swellings caused by local trauma. They may occur anywhere in the mouth, and children and young adults are most often affected.5
Oral neurofibromatosis presents as asymptomatic, slow-growing, nontender submucosal masses. The masses may occur anywhere in the mouth but are most common on the tongue, buccal mucosa, or vestibular areas.6
Pyogenic granulomas present as rapidly growing, erythematous lesions in response to irritation, trauma, or pregnancy hormones. The masses are usually nonpainful and bleed easily. They are most often located on the gingiva.5
Summary Table
| Condition | Characteristics |
|---|---|
| Fibroma | Asymptomatic, smooth, firm, nodule caused by trauma; often located on the occlusal line of the buccal mucosa |
| Mucocele | Bluish, dome-shaped mucosal swelling caused by local trauma; most common in children or young adults |
| Oral neurofibromatosis | Asymptomatic, slow-growing, nontender submucosal mass; most common on the tongue, buccal mucosa, or vestibular areas |
| Palatine torus | Asymptomatic, slow-growing, bony prominence on the hard palate or lingual aspect of the mandible; size is variable |
| Pyogenic granuloma | Rapidly growing, erythematous lesion caused by trauma, irritation, or pregnancy hormones; usually nonpainful and bleeds easily; most common on the gingiva |

