Clinical Question
What is the best way to diagnose gastroesophageal reflux disease (GERD)?
Evidence Summary
Diagnosis of GERD may be clinical (presentation with typical symptoms, such as heartburn); physiologic (evidence of abnormal pH levels in the distal esophagus); anatomic (evidence of esophagitis on endoscopy); or functional (clinical response to antacid medications). However, the correlation between these diagnostic approaches is relatively poor. For example, many asymptomatic patients have esophagitis, abnormal pH values, or even Barrett esophagus.1 Furthermore, most studies of GERD diagnosis have taken place in referral populations, so their applicability to the primary care setting is uncertain. Finally, although symptom scores have been developed, they are most helpful in assessing and monitoring the severity of GERD in patients with a known diagnosis,2–4 they have not been validated,5 or they used an inadequate reference standard.6,7
A recent study developed a new diagnostic score, the GerdQ, which is based on data from primary care patients with upper gastrointestinal (GI) symptoms.8 The study used variables from several previous symptom scores, and used focus groups to ensure that the resulting questionnaire was easy for patients to use as a self-reported instrument. The reference standard for GERD was defined as any of the following:
- Esophageal pH of less than 4 for more than 80 minutes per day
- Evidence of esophagitis on endoscopy
- Indeterminate esophageal pH in combination with a positive response to a 14-day course of a proton pump inhibitor
- A highly abnormal symptom score
The final GerdQ tool was evaluated in a group of 308 primary care patients with upper GI symptoms (Table 1).8 Increasing scores correlated with increasing severity of heartburn symptoms. The overall accuracy was similar to that of clinical diagnosis by a gastroenterologist.
Table 1. GerdQ Questionnaire
| Symptom | How many times does this occur per week? | |||
|---|---|---|---|---|
| 0 days | 1 day | 2 or 3 days | 4 to 7 days | |
| Burning feeling behind the breastbone (heartburn) | 0 | 1 | 2 | 3 |
| Stomach contents moving up to the throat or mouth (regurgitation) | 0 | 1 | 2 | 3 |
| Pain in the middle of the upper stomach area | 3 | 2 | 1 | 0 |
| Nausea | 3 | 2 | 1 | 0 |
| Trouble getting a good night's sleep because of heartburn or regurgitation | 0 | 1 | 2 | 3 |
| Need for over-the-counter medicine for heartburn or regurgitation (such as Tums, Rolaids, Maalox, or other antacids), in addition to the medicine your doctor prescribed | 0 | 1 | 2 | 3 |
note: Add the point values for each corresponding answer. Total score of 0 to 2 points = 0 percent likelihood of GERD; 3 to 7 points = 50 percent likelihood; 8 to 10 points = 79 percent likelihood; 11 to 18 points = 89 percent likelihood.
GERD = gastroesophageal reflux disease.
Adapted with permission from Jones R, Junghard O, Dent J, et al. Development of the GerdQ, a tool for the diagnosis and management of gastrooesophageal reflux disease in primary care. Aliment Pharmacol Ther. 2009;30(10):1034.
Another study developed and validated a score to predict the likelihood that patients with upper GI symptoms would respond to the proton pump inhibitor omeprazole (Prilosec).9 Using data from 471 patients with GERD-like or ulcer-like dyspepsia, the study identified increasing body mass index (BMI), recent use of antacids or histamine H2 blockers, nighttime pain, and absence of nausea as independent predictors of response to a two-week course of omeprazole (Figure 1).9 A BMI of greater than 29 kg per m2 adds points to the score, whereas a BMI of less than 29 kg per m2 subtracts points. A simple heuristic is that in patients of average or increased weight, nighttime pain or recent antacid use (in the absence of nausea) predicts a good response to omeprazole.
Figure 1. Likelihood of Response to Omeprazole (Prilosec)
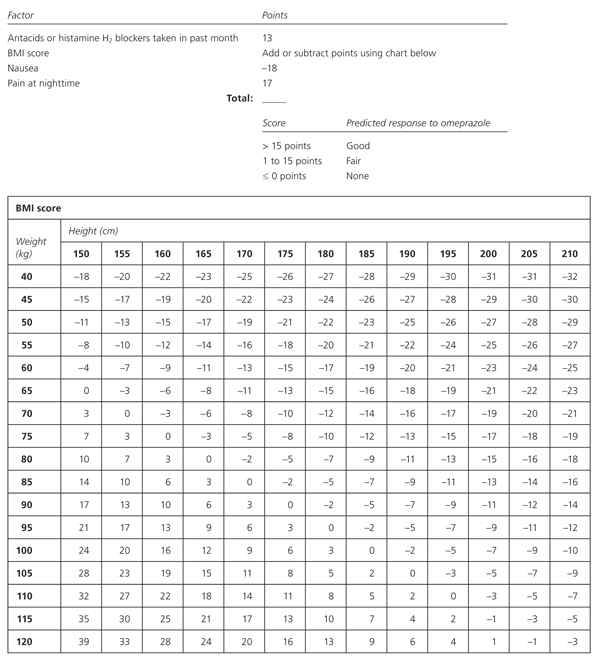
Score to determine the likelihood of response to omeprazole (Prilosec). (BMI = body mass index.)
Adapted from Meineche-Schmidt V, Christensen E. Which dyspepsia patients will benefit from omeprazole treatment? Analysis of a Danish multicenter trial. Am J Gastroenterol. 2000;95(10):2781.

