A 39-year-old man presented with painless red lesions under his fingernails that appeared 15 months earlier. The lesions slowly grew out of the nails, but always returned. The patient had no history of trauma to his nails or of rashes, except for mild rosacea on his face. He was not taking any medication, and his personal and family histories were unremarkable.
On physical examination, linear reddish-brown streaks were noted on both index fingernails and the left middle fingernail (Figures 1 and 2). Multiple nails were enlarged with triangular lunula. There was slight erythema of the nail folds in all of the fingernails. An extensive evaluation revealed no underlying systemic disease.
Figure 1.
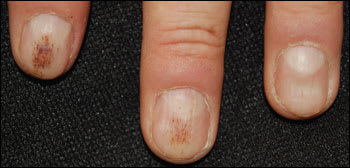
Figure 2.
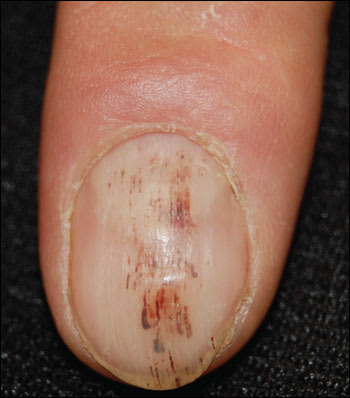
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Beau lines.
B. Longitudinal striations.
C. Muehrcke lines.
D. Splinter hemorrhages.
E. Telangiectasia.
Discussion
The answer is D: splinter hemorrhages. Splinter hemorrhages are nonblanchable, 1- to 3-mm, red to reddish-brown, longitudinal hemorrhages appearing under the nail plate.1 They occur in the dermis after rupture of the capillaries that follow the linear configuration of the epidermal-dermal ridges.2 The blood attaches to the nail plate and moves distally as the nail grows. Occasionally, hemorrhage spots remain stationary if attached to the nail bed and not the nail plate.1 Splinter hemorrhages are more common in men and in persons with dark complexion. They occur mostly in fingernails, but can also appear in toenails.1
Splinter hemorrhages can be caused by environmental factors, skin disorders, systemic diseases, and medication use. However, nail trauma (e.g., from sports, housework, personal habits) is the most common cause, accounting for 20 percent of cases.1–4
Splinter hemorrhages are more commonly associated with nail psoriasis, but can also occur with eczema, vasculitis, or onychomycosis.1 Dermal vascular dilatation and tortuosity from psoriasis can lead to splinter hemorrhages. Splinter hemorrhages of the psoriatic nail are thought to be similar to the cutaneous Auspitz sign.5
Systemic disease may be the cause if the splinter hemorrhages appear in several nails, are located in the proximal portion of the nail plate, or are painful.1,6 Petechiae and splinter hemorrhages are classic lesions of subacute endocarditis, especially when accompanied by fever, Roth spots, Osler nodes, Janeway lesions, or a murmur. Splinter hemorrhages can occur with systemic lupus erythematosus, along with other nail changes such as periungual telangiectasias, hyperkeratotic ragged cuticles, onycholysis, and red lunula.7
Splinter hemorrhages can be an adverse effect of medications that impair blood vessels in the nail bed, although this is uncommon. These reactions are usually dose-related, involve several or all nails, and resolve after the medication is discontinued.8 Medications that may lead to this reaction include antithrombotics and anticoagulants, such as aspirin and warfarin (Coumadin)9; cancer chemotherapeutic agents, such as taxanes10; tetracycline; and ganciclovir (Cytovene).11
Beau lines are transverse lines affecting all nails at the base of the lunula. They are caused by temporary dysfunction of the nail matrix from systemic causes or local trauma.
Longitudinal striations do not involve blood vessels. They are accentuated, parallel, elevated ridges in the nail surface that occur with aging or in association with alopecia areata, vitiligo, atopic dermatitis, or psoriasis.
Muehrcke lines are narrow, white transverse bands that occur in pairs as a sign of hypoalbuminemia. Muehrcke lines can also be associated with trauma, but are usually unilateral.
Telangiectasia can suggest collagen vascular disease, (e.g., lupus erythematosus, scleroderma, dermatomyositis). It appears as altered capillary patterns on the fingernail folds.
Summary Table
| Condition | Characteristics |
|---|---|
| Beau lines | Transverse lines affecting all nails at the base of the lunula; caused by temporary dysfunction of the nail matrix from systemic causes or local trauma |
| Longitudinal striations | Accentuated, parallel, elevated ridges in the nail surface; caused by the normal aging process or associated with alopecia areata, vitiligo, atopic dermatitis, or psoriasis |
| Muehrcke lines | Narrow, white transverse bands; occur in pairs as a sign of hypoalbuminemia; may be associated with trauma; usually unilateral |
| Splinter hemorrhages | Nonblanchable, 1- to 3-mm, red to reddish-brown longitudinal hemorrhages that appear beneath the nail plate; caused by trauma, environmental insults, skin disorders, systemic diseases, or medication use |
| Telangiectasia | Altered capillary patterns on the fingernail folds; can be indicative of collagen vascular disease |

