
Am Fam Physician. 2010;82(1):43-49
A more recent article on care of the military veteran is available.
Patient information: See related handout on help for returning veterans, written by the authors of this article.
Author disclosure: Nothing to disclose.
Of the 23.8 million military veterans living in the United States, approximately 3 million have served in Operation Enduring Freedom or Operation Iraqi Freedom. The injuries and illnesses that affect veterans returning from combat are predictable. Blast injuries are common and most often present as mild traumatic brain injury, which is synonymous with concussion. Family physicians caring for returning veterans will also encounter conditions such as posttraumatic stress disorder at rates higher than those in the general population. The symptoms associated with posttraumatic stress disorder and mild traumatic brain injury often overlap and can present concurrently. Treatment of traumatic brain injury should be based on symptoms and guided by clinical practice guidelines from the U.S. Department of Veterans Affairs and Department of Defense. Family physicians should understand the range of post-war health concerns and screen returning service members for posttraumatic stress disorder, substance abuse, suicidality, and clinical depression. Family physicians are well positioned to offer continuity of care for issues affecting returning service members and to coordinate the delivery of specialized care when needed.
The cost of caring for the more than 3 million U.S. service members who have served in Operation Iraqi Freedom and Operation Enduring Freedom in Iraq, Afghanistan, and Africa is conservatively projected to exceed $350 billion.1 Improvements in personal protective combat armor, use of armored vehicles, and improvements in the casualty evacuation system have changed the types of war injuries that are “survivable” on the modern battlefield. Early resuscitation and stabilization of service members can be successfully accomplished at the front lines.2
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Treatment of mild traumatic brain injury should be based on symptoms and guided by clinical practice guidelines from the U.S. Department of Veterans Affairs and Department of Defense. | C | 7 |
| Returning service members who were in life-threatening situations or situations where serious injury could occur should be screened for posttraumatic stress disorder. | C | 14, 16 |
| Suicide prevention is an important element of post-deployment health care. | C | 24 |
Improvements in survivability have contributed to the increase in the number of veterans seeking medical care. There are concerns that the current volume of patients is stretching the capacity of the Veterans Health Administration. There are gaps in care for service members returning from combat operations, particularly in mental health care.3 Traumatic brain injury and posttraumatic stress disorder (PTSD) are the injuries most commonly associated with the current conflicts.4 This article will help family physicians recognize common issues facing returning service members and their families, and provides resources to help improve care.
Concussion/Traumatic Brain Injury
Traumatic brain injury is a blow or penetrating injury to the head that disrupts normal brain function.5 The severity can range from mild (characterized by a brief change in mental status or amnesia; also known as a concussion) to severe (characterized by extended periods of change in mental status, unconsciousness, or amnesia). The severity of the injury usually correlates with level of disability, although sometimes it does not.
Approximately 10 to 20 percent of service members evacuated from Afghanistan and Iraq have had at least one concussion.6 Concussion/mild traumatic brain injury is defined as a brief loss of consciousness (less than 30 minutes); change in mental status for less than 24 hours; posttraumatic amnesia for less than 24 hours; a Glasgow Coma Scale score of 13 to 15, and (if performed) normal structural imaging.7 Blast exposure is one common mechanism of concussion during deployment. Current evidence suggests that concussion after a blast injury is clinically similar to concussion in other settings (such as sports concussions).
As with sports concussions, most patients with mild traumatic brain injury recover completely and rapidly without clinical sequelae. In those who do not, residual symptoms can include headaches, irritability, depression, sleep disturbance, slowed cognition, memory problems, and difficulty concentrating (Table 1).7 These symptoms have been described in the post-combat setting after previous conflicts8 and can result from a variety of underlying conditions, such as concussion, PTSD, depression, prolonged sleep deprivation, physical injuries, and physiologic effects of extreme stress. Because it is often difficult to confirm the specific etiology of post-war symptoms, including those associated with concussion, the goal is to alleviate symptoms; identify those at risk of complications; minimize secondary morbidity; rule out underlying comorbid psychiatric or medical disorders; improve long-term outcomes; and avoid misattribution of symptoms to traumatic brain injury.

| Common behavioral and cognitive symptoms* |
| Anxiety |
| Depression |
| Fatigue |
| Irritability |
| Loss of energy |
| Memory problems |
| Poor frustration tolerance |
| Trouble concentrating |
| Trouble making decisions |
| Differential diagnosis and common comorbidities |
| Anxiety disorders |
| Chronic fatigue syndrome |
| Chronic pain |
| Depression or other mood disorders |
| Insomnia |
| Metabolic disorders |
| Sleep apnea |
| Stress disorders |
| Substance use |
| Laboratory tests |
| Complete blood count |
| Electrolyte levels |
| Thyroid function testing |
There is no diagnostic test for mild traumatic brain injury that has sufficient sensitivity or specificity. Many patients do not present until weeks to months after the injury. Therefore, a systematic evaluation should be performed in patients with a potential traumatic brain injury. This evaluation should include a detailed history of the inciting event, including the mechanism of injury and course of symptoms. The history should explore other traumatic events and symptoms of depression and combat reactions, such as hypervigilance and intrusive or ruminative thoughts related to the event. The U.S. Department of Defense (DoD) uses a four-question post-deployment survey to screen for mild traumatic brain injury (http://www.pdhealth.mil/dcs/pdhra.asp). However, there have been concerns that the screening process itself may promote misattribution of symptoms to concussion/mild traumatic brain injury. The DoD and the U.S. Department of Veterans Affairs (VA) recently published a clinical practice guideline on identification and management of concussion and mild traumatic brain injury.7
When evaluating patients with potential traumatic brain injury (particularly moderate and severe), a thorough cranial nerve examination should be performed, as well as testing of vestibular function and postural stability, visual assessment, and neurocognitive screening. Patients with positive neurocognitive screening merit referral for further evaluation. Neurocognitive screening includes an assessment of mental function (Mini-Mental State Examination) or formal neuropsychiatric testing. Because long-term outcomes are not equivalent in patients with moderate to severe traumatic brain injury, formal neuropsychiatric testing is important in these patients.9 Neuroimaging is not always necessary, but in patients with persistent symptoms and those in whom imaging is needed to rule out other disease (e.g., tumor, ischemia), magnetic resonance imaging is the modality of choice.10 The VA/DoD guideline on the management of concussion and mild traumatic brain injury also provides guidance for pharmacologic treatment in patients with persistent symptoms after potential traumatic brain injury.7 Treatment of patients with mild traumatic brain injury is based on symptoms (Tables 2 and 3).7 Treatment should include nonpharmacologic interventions when possible.7 Behavioral and cognitive symptoms can often be managed with nonpharmacologic techniques, such as regular aerobic activity, sleep hygiene, and activity modification. Medication is most likely to help with pain management and short-term sleep control.7 Selective serotonin reuptake inhibitors (SSRIs) are generally used for pharmacologic management of mood symptoms such as irritability and depression.7
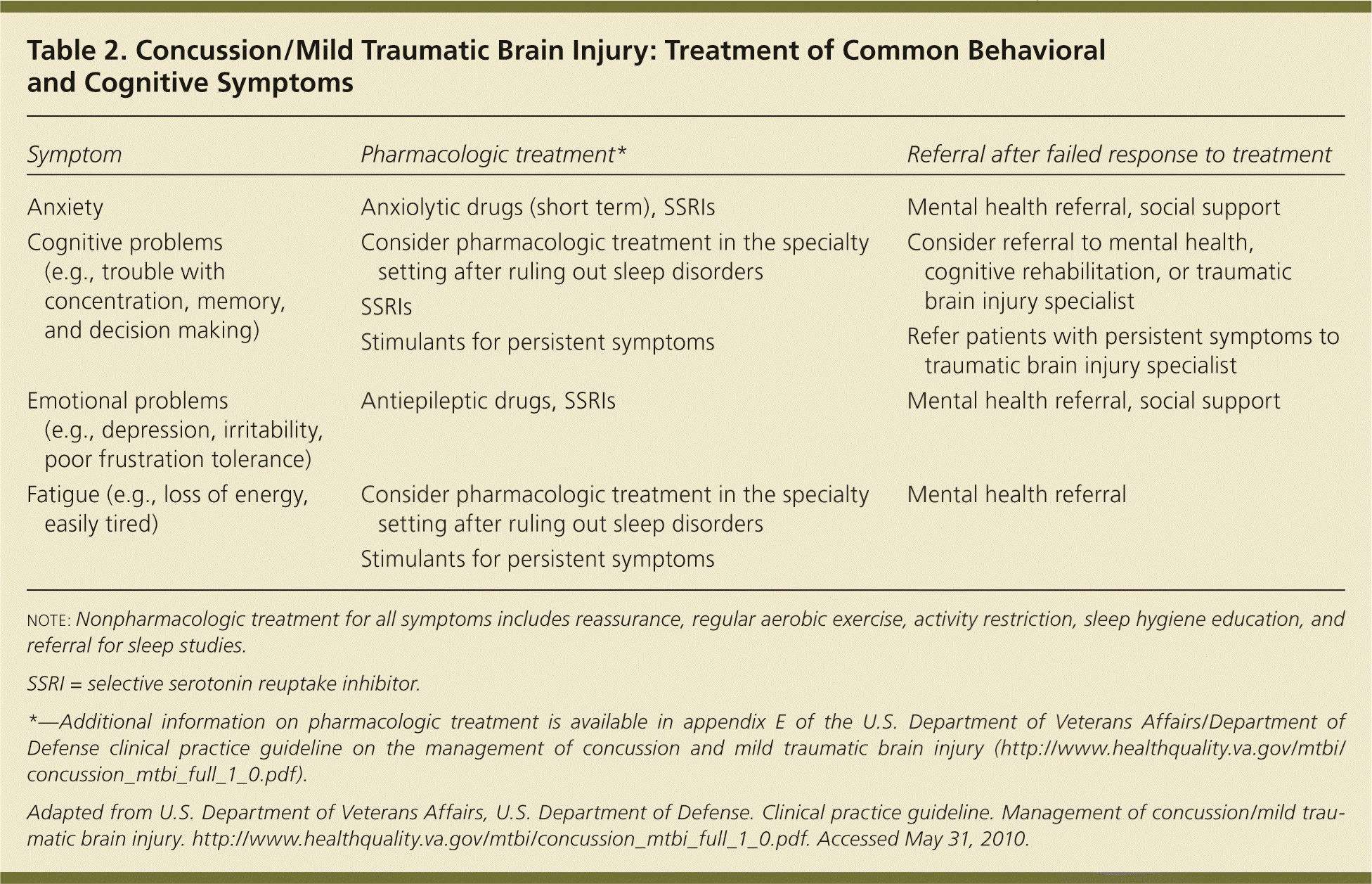
| Symptom | Pharmacologic treatment* | Referral after failed response to treatment |
|---|---|---|
| Anxiety | Anxiolytic drugs (short term), SSRIs | Mental health referral, social support |
| Cognitive problems (e.g., trouble with concentration, memory, and decision making) | Consider pharmacologic treatment in the specialty setting after ruling out sleep disorders SSRIs Stimulants for persistent symptoms | Consider referral to mental health, cognitive rehabilitation, or traumatic brain injury specialist Refer patients with persistent symptoms to traumatic brain injury specialist |
| Emotional problems (e.g., depression, irritability, poor frustration tolerance) | Antiepileptic drugs, SSRIs | Mental health referral, social support |
| Fatigue (e.g., loss of energy, easily tired) | Consider pharmacologic treatment in the specialty setting after ruling out sleep disorders Stimulants for persistent symptoms | Mental health referral |
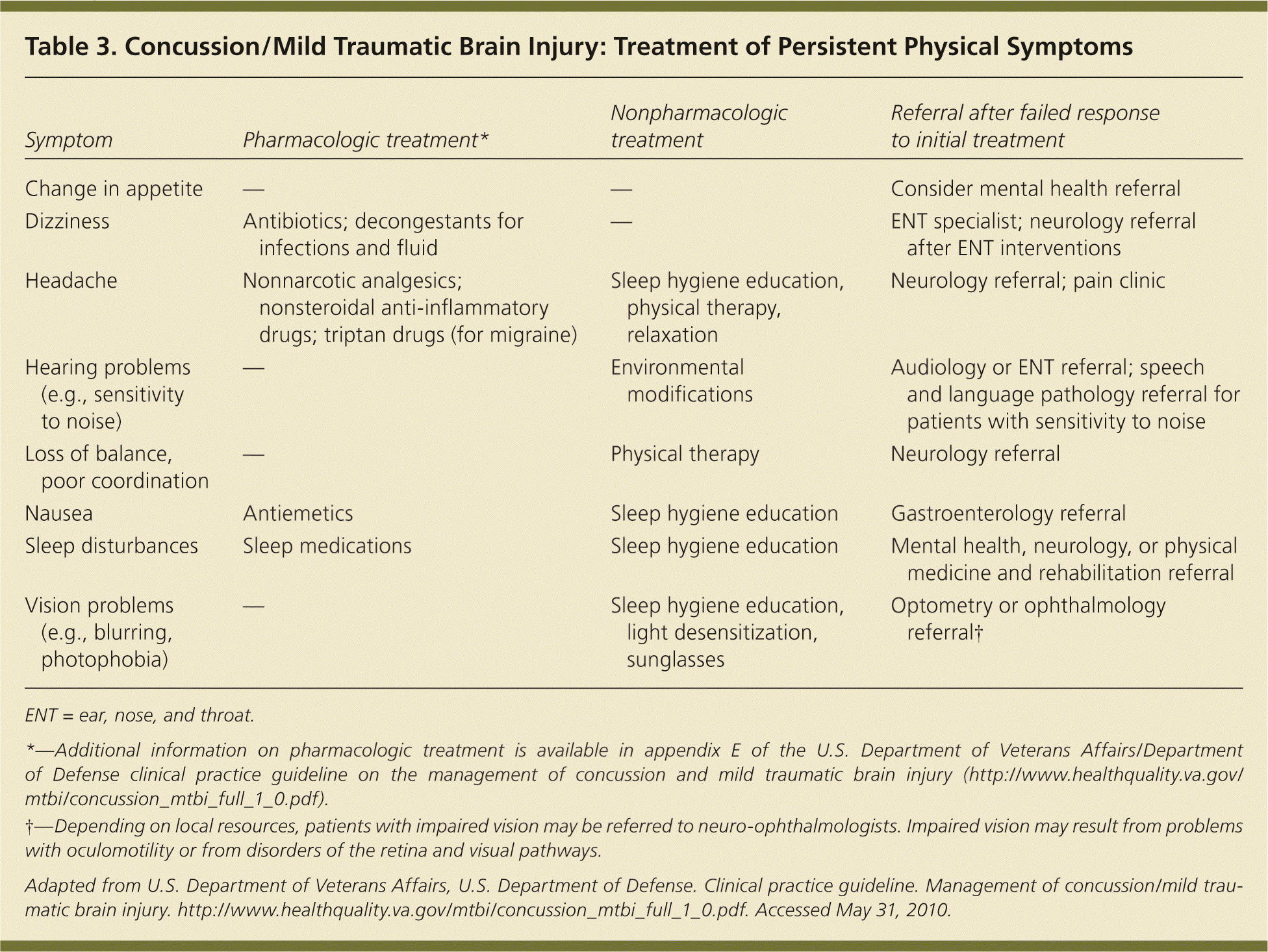
| Symptom | Pharmacologic treatment* | Nonpharmacologic treatment | Referral after failed response to initial treatment |
|---|---|---|---|
| Change in appetite | — | — | Consider mental health referral |
| Dizziness | Antibiotics; decongestants for infections and fluid | — | ENT specialist; neurology referral after ENT interventions |
| Headache | Nonnarcotic analgesics; nonsteroidal anti-inflammatory drugs; triptan drugs (for migraine) | Sleep hygiene education, physical therapy, relaxation | Neurology referral; pain clinic |
| Hearing problems (e.g., sensitivity to noise) | — | Environmental modifications | Audiology or ENT referral; speech and language pathology referral for patients with sensitivity to noise |
| Loss of balance, poor coordination | — | Physical therapy | Neurology referral |
| Nausea | Antiemetics | Sleep hygiene education | Gastroenterology referral |
| Sleep disturbances | Sleep medications | Sleep hygiene education | Mental health, neurology, or physical medicine and rehabilitation referral |
| Vision problems (e.g., blurring, photophobia) | — | Sleep hygiene education, light desensitization, sunglasses | Optometry or ophthalmology referral† |
Posttraumatic Stress Disorder
PTSD is a clinical syndrome characterized by the development of symptoms after exposure to a traumatic event. These exposures typically involve actual or threatened death or serious injury.11 The initial response is one of fear, helplessness, or horror. The hallmark of PTSD is re-experiencing the traumatic event through intrusive and disturbing thoughts. Patients avoid situations or stimuli associated with the event, and have persistent symptoms of increased arousal. Distressing dreams during which traumatic events are replayed are common. The sudden feeling that one is back in the threatening environment (referred to as flashbacks) can be associated with distress and heightened sympathetic arousal. Symptoms of anxiety or increased arousal must not have been present before the traumatic exposure. To confirm the diagnosis, symptoms must be present for at least one month and must cause clinically significant distress or impairment in social, occupational, or other areas of daily living (Table 411 and Figure 112 ). Other common symptoms associated with PTSD include difficulty falling or staying asleep, recurrent nightmares, hypervigilance, and an exaggerated startle response.11

| STRESSOR: Exposure to traumatic event with both of the following: | ||
| Experiencing or witnessing an event that involved actual or threatened death (or serious injury); or a threat to physical integrity (or the integrity of others) | ||
| Response to the event involved fear, helplessness, or horror | ||
| INTRUSIVE RECOLLECTION: The event is re-experienced in one of the following ways: | ||
| Recurrent, intrusive recollections of the event | ||
| Recurrent distressing dreams of the event | ||
| A sense of reliving the event (acting or feeling as if the event is re-occurring) | ||
| Marked distress when exposed to cues that symbolize or represent an element of the traumatic event | ||
| Heightened physiologic reactivity when exposed to cues that symbolize or represent an element of the traumatic event | ||
| AVOIDANCE/NUMBING: Persistent avoidance of stimuli associated with the event (not present before exposure to the trauma) as manifested by: | ||
| Attempts to avoid thoughts or feelings associated with the event | ||
| Attempts to avoid activities, places, or individuals that cause recollections of the event | ||
| Inability to remember important elements of the event | ||
| Diminished interest or participation in activities that would otherwise be considered important or significant | ||
| A sense of detachment or estrangement from others | ||
| A restriction in the individual's spectrum of emotions (e.g., inability to cultivate loving feelings) | ||
| Sense of a restricted future (e.g., “I don't think I'll live to see age 60.”) | ||
| HYPERAROUSAL: Persistent symptoms of increased arousal | ||
| Difficulty falling or staying asleep | ||
| Outbursts of anger | ||
| Difficulty with concentration | ||
| Hypervigilance | ||
| Exaggerated startle response | ||
| DURATION: Symptoms present for at least one month | ||
| FUNCTIONAL SIGNIFICANCE: Symptoms cause significant distress or impair social or occupational function | ||
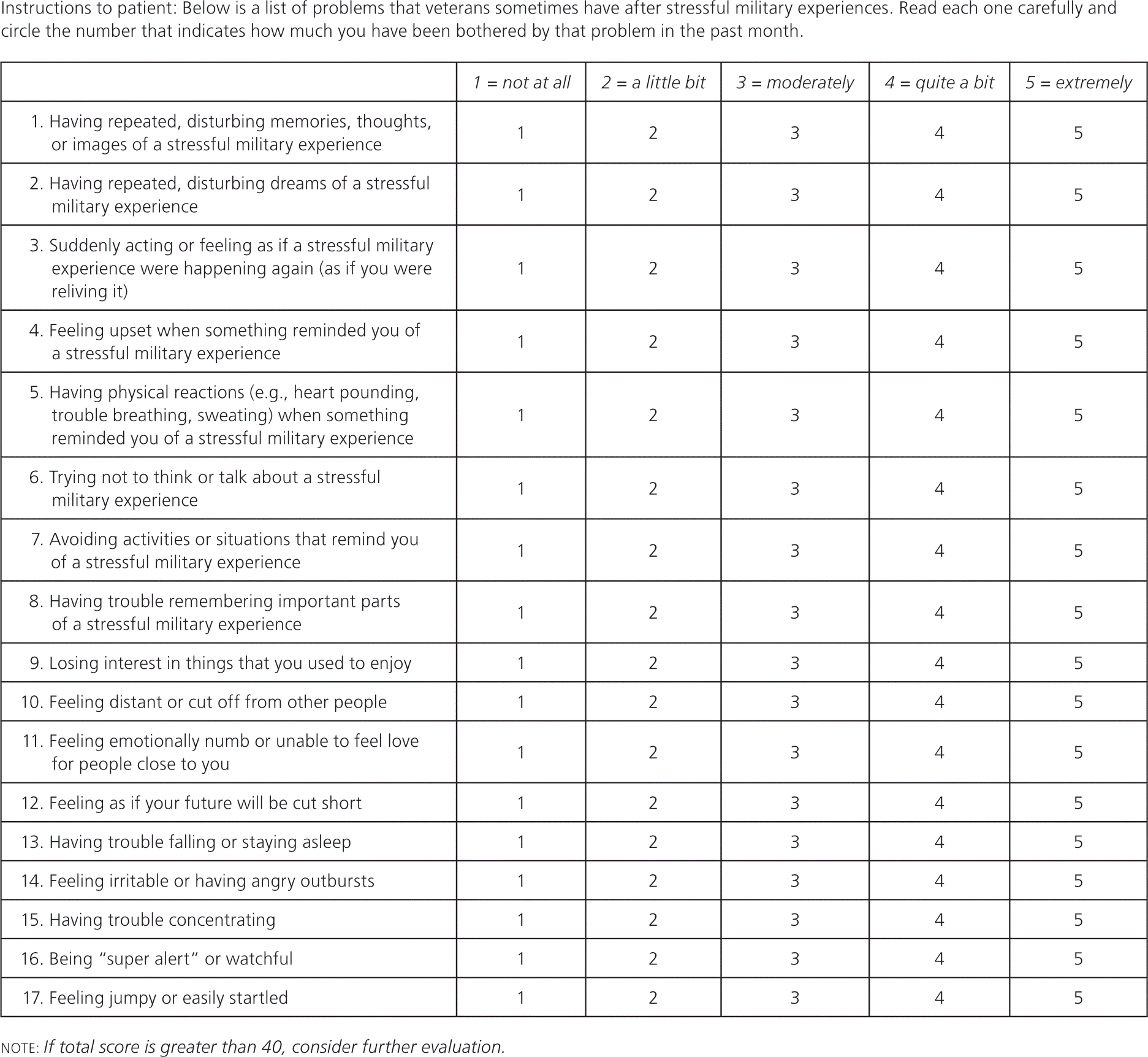
Approximately 19 percent of U.S. service members (about 300,000) who have served in combat in Iraq and Afghanistan report problems with depression, anxiety, or PTSD.13 These rates are similar to those in Vietnam veterans14,15 and civilian accident victims admitted to major trauma centers, but lower than those in victims of physical assault.16 In one study, only 23 to 40 percent of returning service members with positive screens for a mental disorder reported seeking mental health care.3 Commonly cited reasons for not seeking care were concerns about possible stigmatization and other perceived barriers.
There are strong associations between PTSD and other indicators of general well-being. Compared with veterans who do not have PTSD, those with the condition are more likely to describe their health as poor, more likely to miss work, and more likely to report a variety of somatic concerns.17,18 Persons with PTSD are also more likely to have depression and problems with substance abuse and interpersonal relationships.19
The most effective treatment for PTSD is cognitive behavioral therapy.20 Cognitive behavioral therapy includes a combination of exposure therapy, cognitive restructuring, and stress-reduction techniques, such as diaphragmatic breathing. Eye movement desensitization and reprocessing, a form of exposure therapy, has also been proven effective in treating PTSD.21 Medications such as SSRIs have been used in conjunction with cognitive behavioral therapy to treat patients with PTSD.22 In general, treatment should be coordinated with therapists who have experience in cognitive techniques and PTSD.
A national PTSD information hotline is available (802-296-6300; e-mail: ncptsd@va.gov), and an interactive guide to VA treatment facilities is available online (http://www2.va.gov/directory/guide/home.asp? is Flash = 1). The International Society for Traumatic Stress Studies also has several resources for physicians interested in learning more about cognitive behavioral therapy for the management of PTSD (http://www.istss.org/ResourcesforProfessionals/1956.htm).
Suicide
Before Operation Iraqi Freedom and Operation Enduring Freedom, suicide rates in service members were consistently 20 to 30 percent lower than demographically matched civilian rates.23 In the past several years, suicide rates have risen in the Army and Marine Corps. These increases are presumably because of the stresses of ongoing wartime service. There have been conflicting data on suicide rates in veterans, which may be related to problems with death classifications24; however, service members with a history of combat-related injury or other mental health condition (e.g., PTSD) seem to be at particular risk.14,25,26
Concern that suicide rates are increasing among veterans recently prompted a report to the VA secretary.24 Current efforts focus on identifying veterans and active duty service members who are at increased risk of suicide. The DoD has instituted a health assessment to be completed immediately before return from deployment, with reassessment after six months. These assessments specifically evaluate for post-deployment concerns, including PTSD, depression, and suicide risk. The VA has enacted mandatory screening for depression and PTSD, and has established suicide prevention coordinators at each VA medical center (http://www.mentalhealth.va.gov/suicide_prevention/).
Family physicians caring for veterans and active duty service members returning from combat should screen patients for depression, PTSD, and suicidality. Patients with multiple somatic symptoms warrant further screening. The VA Suicide Prevention Lifeline (800-273-TALK) provides 24-hour live access to a counselor to assist veterans in crisis. The patient information handout lists Web-based resources for service members and their families.
Reintegration into the Family
Returning home is often the most anticipated event of a service member's deployment. However, reintegration into the family and society often proves to be more difficult than anticipated. What many anticipate will be a happy and exciting event often becomes a stressful, prolonged struggle.
There are five typical phases to the return and reunion process.27 The first phase is pre-entry, which takes place in the days before returning home. During this time, the service member typically works long hours, and families make final preparations for the homecoming. The second phase, reunion, is commonly referred to as the “honeymoon” phase. There is a sense of courtship and return of intimacy that lasts for the first days after the return. The disruption phase occurs when problems are introduced into the relationship. Its hallmark is the realization that the family members are not the same as before the service member deployed. Careful attention to the problems and concerns identified in this phase leads to the fourth phase, communication. During the communication phase, veterans and family members reconnect, renegotiate, and redefine their roles within the relationship. Successful passage through the communication phase will lead to the normal phase, which signals the return to a routine.
Final Comment
Working with physicians from the VA and the Military Health System, community-based family physicians have a critical role in the initial and longitudinal treatment of America's service members. The American Academy of Family Physicians recognizes this and supports the Rural Veterans Access to Care Act (H.R. 1527).28
