
A more recent article on common occupational upper extremity musculoskeletal disorders is available.
Am Fam Physician. 2010;82(2):169-174
Author disclosure: Nothing to disclose.
Given the burden of occupational illnesses and injuries in the United States, family physicians should understand the role workplace exposures may play in patients' chief concerns. Incorporating employment screening questions into patients' intake questionnaires is an efficient means of identifying potential occupational causes of symptoms. Recommended questions include what kind of job patients have; whether their symptoms are worse at work; whether they are or have been exposed to dust, fumes, chemicals, radiation, or loud noise; and whether they think their health problems may be related to their work. These questions are especially important when the diagnosis or etiology is in doubt. Depending on patients' responses to the screening questions, a more detailed occupational history may be appropriate. It can be useful to ask about routine tasks performed during a typical work shift, as well as anything out of the ordinary (e.g., a change in routine, an injury or accident). The occupational history should include information about alcohol and tobacco use, second or part-time jobs, military service, hobbies, and home environment. Patients with suspected occupational illnesses or injuries may benefit from referral to an occupational medicine specialist for a more detailed assessment and follow-up.
Occupational illnesses and injuries are conditions that are caused or exacerbated by exposures or stressors in the workplace. In 2008, 3.7 million nonfatal occupational illnesses and injuries were reported to the U.S. Bureau of Labor Statistics,1 and evidence suggests substantial underreporting.2 A considerable proportion of illnesses and injuries managed in the primary care setting are work-related.3–5
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Incorporating occupational screening questions into the patient history can identify potential exposures in the workplace that may be contributing to patients' symptoms. | C | 13 |
| A comprehensive occupational history should include employment history, types of exposures, exposure assessment, time between exposure and symptom onset, and nonoccupational exposures. | C | 13–15 |
| Referral to an occupational medicine specialist may be appropriate for patients who need additional resources or assistance. | C | 20 |
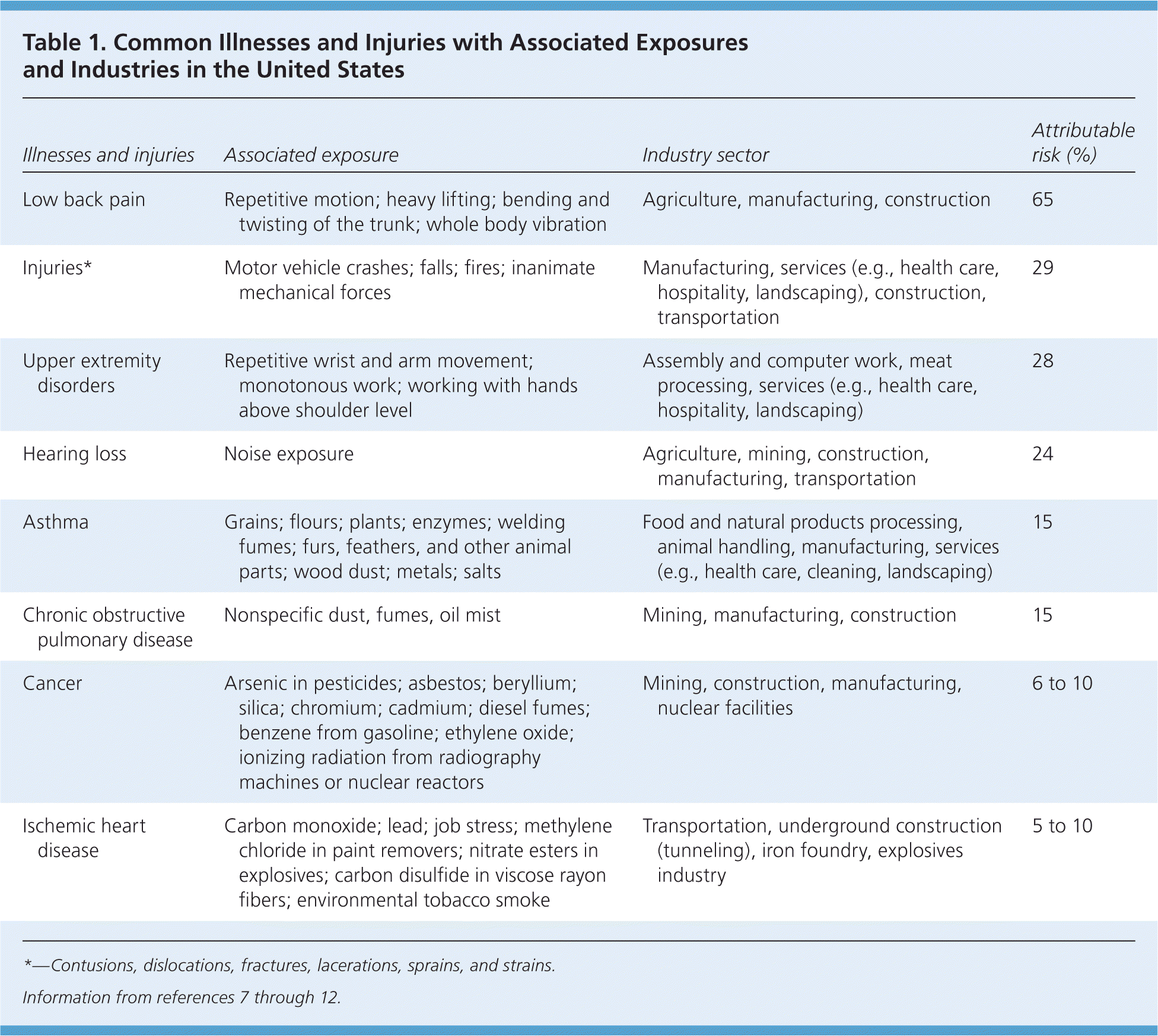
Occupational illnesses and injuries can be difficult to diagnose for several reasons: (1) the similarities in the clinical presentation and pathophysiology between occupational and nonoccupational exposures; (2) the long latency period between exposure and symptom onset; (3) the multifactorial etiology of many chronic diseases; and (4) underreporting of work-related conditions.6 Table 1 lists common illnesses and injuries, potential risk factors in the workplace, the industry sectors where they typically occur, and an estimate of the risk attributable to occupational exposures in the United States.7–12
| Illnesses and injuries | Associated exposure | Industry sector | Attributable risk (%) |
|---|---|---|---|
| Low back pain | Repetitive motion; heavy lifting; bending and twisting of the trunk; whole body vibration | Agriculture, manufacturing, construction | 65 |
| Injuries* | Motor vehicle crashes; falls; fires; inanimate mechanical forces | Manufacturing, services (e.g., health care, hospitality, landscaping), construction, transportation | 29 |
| Upper extremity disorders | Repetitive wrist and arm movement; monotonous work; working with hands above shoulder level | Assembly and computer work, meat processing, services (e.g., health care, hospitality, landscaping) | 28 |
| Hearing loss | Noise exposure | Agriculture, mining, construction, manufacturing, transportation | 24 |
| Asthma | Grains; flours; plants; enzymes; welding fumes; furs, feathers, and other animal parts; wood dust; metals; salts | Food and natural products processing, animal handling, manufacturing, services (e.g., health care, cleaning, landscaping) | 15 |
| Chronic obstructive pulmonary disease | Nonspecific dust, fumes, oil mist | Mining, manufacturing, construction | 15 |
| Cancer | Arsenic in pesticides; asbestos; beryllium; silica; chromium; cadmium; diesel fumes; benzene from gasoline; ethylene oxide; ionizing radiation from radiography machines or nuclear reactors | Mining, construction, manufacturing, nuclear facilities | 6 to 10 |
| Ischemic heart disease | Carbon monoxide; lead; job stress; methylene chloride in paint removers; nitrate esters in explosives; carbon disulfide in viscose rayon fibers; environmental tobacco smoke | Transportation, underground construction (tunneling), iron foundry, explosives industry | 5 to 10 |
Optimal management of occupational illnesses and injuries includes modifying or eliminating the precipitating cause in the work environment when possible. Treating patients who have occupationally mediated conditions without recognizing the precipitating workplace exposures may delay recovery and increase associated morbidity, functional limitations, and overall costs of care. In contrast, early identification of an occupational cause or contributor may not only reduce morbidity, but also prevent similar adverse health outcomes in the patient's coworkers. Consequently, gathering basic occupational information during the patient history will facilitate the recognition and diagnosis of work-related conditions. It can also assist family physicians in determining an appropriate course of treatment and deciding when referral to an occupational medicine specialist is warranted.
Occupational History
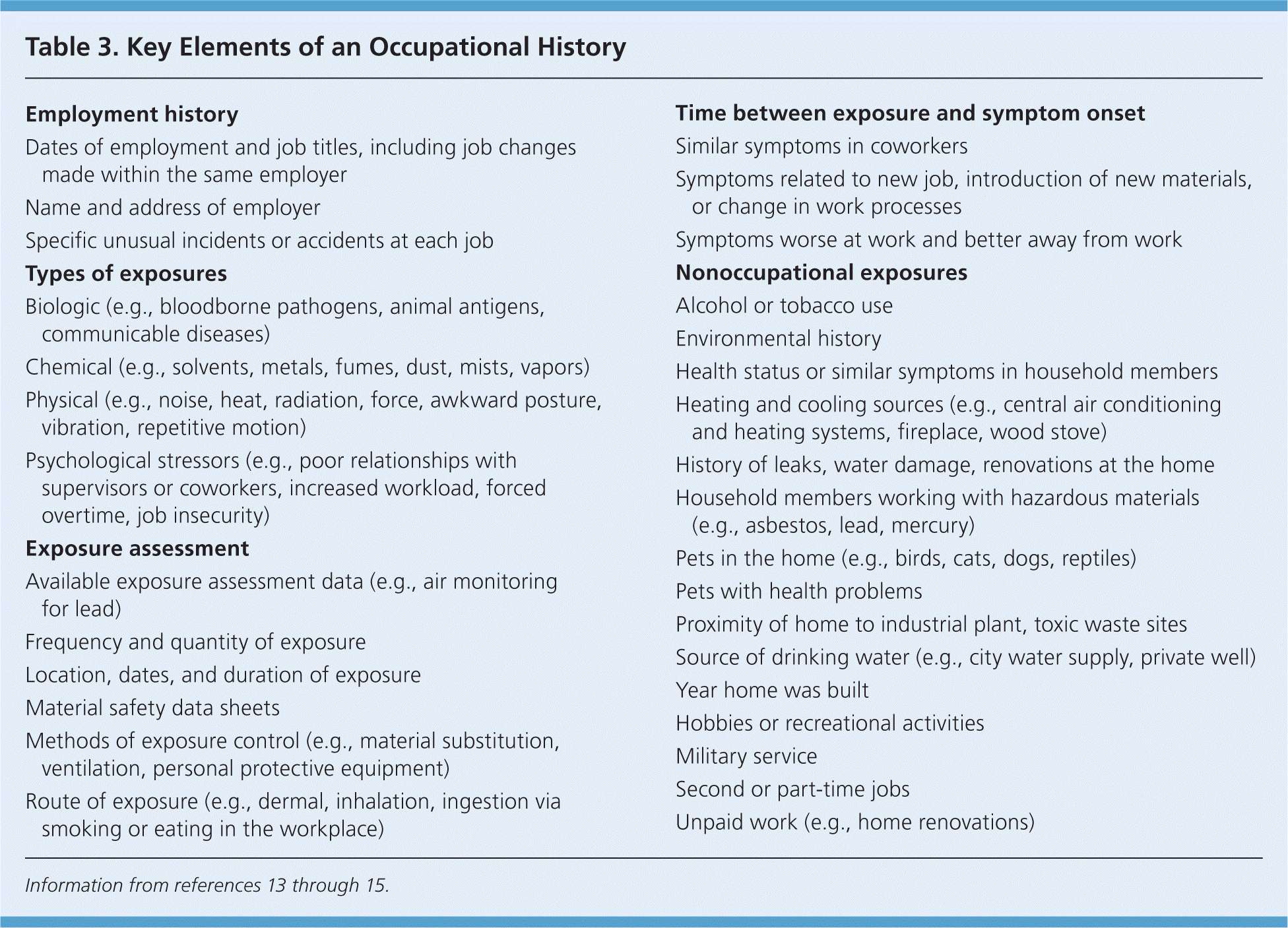
The most efficient way to identify potential work-related contributors to illness or injury is to routinely ask the screening questions outlined in Table 2 during the patient history.13 This is especially important if the diagnosis or etiology is in doubt. Screening questions can be easily incorporated into an intake questionnaire to be completed by the patient or office staff. Depending on patients' responses, follow-up with a more detailed occupational history may be appropriate. Table 3 outlines the key elements of a comprehensive occupational history.13–15 Because a busy family physician may not have time to take a comprehensive occupational history, it is important to focus on components of the occupational history that may be relevant to the patient's condition.

| What kind of work do you do? |
| Are your symptoms better or worse when you are at home? |
| Are you now or have you previously been exposed to dust, fumes, chemicals, radiation, or loud noise at your workplace? |
| Do you think your health problems are related to your work? |
| Employment history |
| Dates of employment and job titles, including job changes made within the same employer |
| Name and address of employer |
| Specific unusual incidents or accidents at each job |
| Types of exposures |
| Biologic (e.g., bloodborne pathogens, animal antigens, communicable diseases) |
| Chemical (e.g., solvents, metals, fumes, dust, mists, vapors) |
| Physical (e.g., noise, heat, radiation, force, awkward posture, vibration, repetitive motion) |
| Psychological stressors (e.g., poor relationships with supervisors or coworkers, increased workload, forced overtime, job insecurity) |
| Exposure assessment |
| Available exposure assessment data (e.g., air monitoring for lead) |
| Frequency and quantity of exposure |
| Location, dates, and duration of exposure |
| Material safety data sheets |
| Methods of exposure control (e.g., material substitution, ventilation, personal protective equipment) |
| Route of exposure (e.g., dermal, inhalation, ingestion via smoking or eating in the workplace) |
| Time between exposure and symptom onset |
| Similar symptoms in coworkers |
| Symptoms related to new job, introduction of new materials, or change in work processes |
| Symptoms worse at work and better away from work |
| Nonoccupational exposures |
| Alcohol or tobacco use |
| Environmental history |
| Health status or similar symptoms in household members |
| Heating and cooling sources (e.g., central air conditioning and heating systems, fireplace, wood stove) |
| History of leaks, water damage, renovations at the home |
| Household members working with hazardous materials (e.g., asbestos, lead, mercury) |
| Pets in the home (e.g., birds, cats, dogs, reptiles) |
| Pets with health problems |
| Proximity of home to industrial plant, toxic waste sites |
| Source of drinking water (e.g., city water supply, private well) |
| Year home was built |
| Hobbies or recreational activities |
| Military service |
| Second or part-time jobs |
| Unpaid work (e.g., home renovations) |
EMPLOYMENT HISTORY
The employment history includes descriptions of all jobs held by the patient in chronological order, including job title and the duration each job was held. Identifying exposures from previous jobs may be particularly important for diseases with longer latency periods.
TYPES OF EXPOSURES
Work exposures may include physical, chemical, or biologic exposures, as well as psychological stressors. Examples of physical exposures include noise, heat, radiation, force, awkward posture, and vibration. Chemical exposures include solvents, metals, fumes, and dust. Biologic exposures include blood-borne pathogens, animal antigens, and communicable diseases. Psychological stressors may be less obvious and may include poor relationships with supervisors or coworkers, increased workload, forced overtime, and job insecurity. Psychological stressors can manifest as anxiety, depression, chest pain, or poorly controlled hypertension.16
It may be useful to ask patients to describe routine tasks performed during a typical work shift, as well as any unusual activities or accidents. Gathering information about infrequently performed tasks, such as periodic maintenance duties, is important because these occasional activities may suggest different exposures. For example, a machine operator may develop contact dermatitis after cleaning parts of a machine with solvents and solutions, even if the task is performed infrequently. This precipitating exposure could be missed if the history is limited to routine job tasks.
EXPOSURE ASSESSMENT
Physicians should attempt to quantify the specific exposure and understand the potential routes of exposure. Although inhalation and dermal paths are the main routes of exposures in the workplace, ingestion via hand-to-mouth contact through smoking or eating in contaminated areas is possible. For example, exposure to lead occurs primarily through inhalation and dermal exposure; however, ingestion can also occur through contaminated surfaces in the dining area of an industrial facility.
TIME BETWEEN EXPOSURE AND SYMPTOM ONSET
When determining whether an illness or injury is work-related, it is important to note the time between symptom onset and possible exposure. Physicians should ask patients to recall when they started a new job; when they began working with a new process or a new agent; when they noticed a worsening of symptoms while at work or a resolution of symptoms on days off; and whether they noticed the presence of similar symptoms in coworkers.
NONOCCUPATIONAL EXPOSURES
A history of alcohol or tobacco use is pertinent to the patient's occupational history because of the potential for interaction with exposures. For example, the combination of smoking and asbestos exposure may increase the risk of lung cancer.17 Alcohol ingestion can enhance the hepatotoxicity of industrial solvents.18 Physicians should also ask patients about any second or part-time jobs; unpaid work (e.g., home renovation); military service; and hobbies (e.g., hunting, which involves exposure to noise and lead).
The location and history of a patient's home is another potential source of nonoccupational exposures. Factors to consider include the proximity of the home to industrial or toxic waste sites; sources of drinking water; and history of leaks, damages, and renovations. Additionally, it is important to ask about exposure to carbon monoxide and other products of combustion from heating or cooking sources. Other household members may also bring hazardous workplace substances home on work clothes and shoes. Pets in the home may cause symptoms, such as asthma from an allergy to cats. The presence of any of these factors in a patient's home should prompt a detailed environmental exposure assessment or referral to an occupational medicine specialist.
Additional Resources
Because patients often have limited knowledge of the specific substances to which they have been exposed, additional information may be required to supplement the occupational history. Material safety data sheets identify the compositions of materials used in the work-place and include any associated adverse health effects, as well as manufacturer contact numbers. Employers are required by law to maintain these data sheets and provide them to employees on request. Physicians may obtain material safety data sheets from the patient's employer for all chemicals in the workplace.
Other information about specific workplace exposures may be obtained by direct communication with the employer's health and safety personnel, with the patient's permission; from exposure assessment reports generated by industrial hygienists; and through communication with manufacturers, poison control centers, or occupational health specialists. If a physician treats many patients from a particular facility or company, arranging a site visit may be helpful to better understand the nature of the work, possible exposures, and potential opportunities for reassigning patients to minimize or eliminate triggering exposures.
Diagnosis
Diagnosing occupational illnesses and injuries involves the same decision-making process used during any clinical encounter (Table 4). Initially, physicians should obtain a patient history; perform a physical examination to identify the condition; consider whether occupational exposures may have contributed to the condition; and, if necessary, order diagnostic studies to confirm the etiology. This should be followed by a review of known or suspected adverse effects of occupational exposures identified during the occupational history. When looking at the time between possible exposure and symptom onset, physicians must consider whether the latency period is appropriate, especially for chronic conditions such as cancer and interstitial lung disease. Nonoccupational risk factors are also important to consider (e.g., a pregnant woman who performs data entry and presents with new-onset carpal tunnel syndrome).

| Recognize a clinical syndrome based on history, physical examination, and initial diagnostic studies |
| Weigh the potential role of various etiologic categories (e.g., autoimmune, infectious, metabolic, neoplastic, traumatic, occupational, environmental) in the differential diagnosis |
| Identify potential risk factors from the occupational history |
| Review adverse health effects of any identified exposures |
| Determine whether the exposure is the primary cause or a contributing factor to the illness or injury |
| Refer to occupational medicine specialist, if warranted |
Physicians should consider an occupational etiology in a patient who does not fit the typical demographic profile of the condition. For example, sarcoidosis, an idiopathic condition typically found in young black women in the United States, has identical radiographic and histopathologic findings to chronic beryllium disease, an interstitial lung disease caused by beryllium exposure. Consequently, chronic beryllium disease is commonly misdiagnosed as sarcoidosis. A detailed work history can identify beryllium exposure, and chronic beryllium disease can be confirmed with a beryllium lymphocyte proliferation test. Distinguishing between sarcoidosis and chronic beryllium disease is important because a patient with chronic beryllium disease must not be further exposed to beryllium.
Patient Referral
Given the complexity of occupational illnesses and injuries, and the time constraints faced by family physicians,19 referral to an occupational medicine specialist is sometimes appropriate once an occupational illness or injury is suspected or confirmed.20 When needed, occupational medicine specialists have the training and resources to conduct a comprehensive occupational and environmental evaluation. They can also interact with union and company officials, regulatory and public health officials, workers' compensation insurance carriers, and others in the judicial system. In addition, many occupational health centers employ multidisciplinary teams that include occupational physicians, occupational health nurses, industrial hygienists, social workers, and ergonomists. This structure typically includes resources to perform worksite evaluations, provide educational programs, and guide patients through various benefits systems. Occupational health centers may be freestanding clinics, hospital-based health centers, or programs affiliated with academic medical centers. Table 5 provides descriptions and contact information for occupational health and safety resources.

| Agency for Toxic Substances and Disease Registry |
| Federal public health agency that provides health information to prevent harmful exposures and diseases related to toxic substances. |
| Telephone: 800-232-4636 |
| Web site: http://www.atsdr.cdc.gov/ |
| American College of Occupational and Environmental Medicine |
| Organization representing physicians and other health care professionals specializing in the field of occupational and environmental medicine. |
| Telephone: 847-818-1800 |
| Web site: http://www.acoem.org/ |
| Association of Occupational and Environmental Clinics |
| A nationwide network of more than 60 multidisciplinary clinics and more than 250 occupational and environmental medicine professionals. |
| Telephone: 888-347-2632 |
| Web site: http://www.aoec.org/ |
| National Institute for Occupational Safety and Health |
| Federal agency responsible for conducting research and making recommendations for the prevention of work-related illness and injury. |
| Telephone: 800-232-4636 |
| Web site: http://www.cdc.gov/niosh/ |
| Occupational Safety and Health Administration (OSHA) |
| Federal agency responsible for enforcing safety and health legislation. OSHA also offers free on-site consultation services to small- and medium-sized businesses in all states. Consultation services are separate from enforcement and do not result in penalties or citations. |
| Telephone: 800-321-6742 |
| Web site: http://www.osha.gov/ |
