Am Fam Physician. 2010;82(3):279-280
Author disclosure: Nothing to disclose.
A 55-year-old black woman presented to the emergency department with acute swelling of the tongue and mild respiratory distress. Her tongue began swelling about three hours earlier, and mild respiratory distress developed during the hour before presentation. She had a history of hypertension, diabetes mellitus, seizure disorder, and moderate mental retardation. She was taking aspirin, lisinopril (Zestril), metformin (Glucophage), phenobarbital, and doxazosin (Cardura), and there was no change in medications in the previous three years. She had no known medication or environmental allergies.
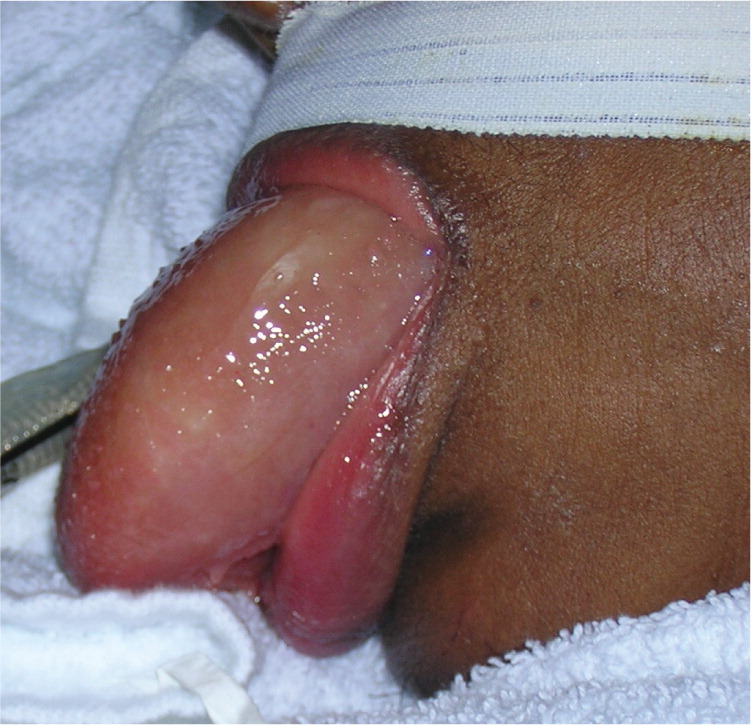
Examination of the oral cavity revealed copious secretions and macroglossia (see accompanying figure). Respiratory examination showed rare crackles, but no wheezing.
Question
Discussion
The answer is D: medication-induced angioedema, likely from the angiotensin-converting enzyme (ACE) inhibitor lisinopril. ACE inhibitor–associated angioedema is a self-limited, localized swelling that commonly affects the lips, tongue, and face. Pruritus and urticaria are usually absent.
The incidence of ACE inhibitor–associated angioedema varies from 0.1 to 6 percent.1 Most cases occur within the first month of starting treatment, with the highest incidence in the first week. However, symptom onset has been reported anywhere from one day to 10 years after starting treatment. Angioedema is more common in black persons, women, smokers, and persons with a history of seasonal allergies. Diabetes seems to decrease the risk.1 The condition is thought to be related to elevations in bradykinin and substance P levels, which cause inflammation and fluid leakage in the postcapillary venules. This leads to a well-demarcated, localized, and nonpitting subdermal edema.1
Although there have been reports of angioedema related to angiotensin receptor blockers (ARBs), the rates are similar to those in the general population. ARBs are generally considered safe in patients with a history of angioedema from ACE inhibitors.2
Angioedema should resolve after the discontinuation of the causative ACE inhibitor, and further treatment with other ACE inhibitors is contraindicated. Depending on the severity of symptoms, supportive care may be required, including treatment with epinephrine and intubation in anticipation of laryngeal obstruction.1,3
Acromegaly is caused by excess growth hormone and manifests as soft tissue and bony overgrowth. Other features include enlarged face, hands, feet, and tongue; coarsening of facial features; and development of diabetes and macroglossia. Duration of symptoms, from onset to diagnosis, is typically 12 years.4
Amyloidosis is characterized by deposition of the amyloid protein in various parts of the body. Although the kidneys, heart, and liver are the most common sites of deposition, amyloid may infiltrate the muscles and cause pseudohypertrophy of the tongue. Macroglossia may be the first manifestation of amyloidosis.5
Hypothyroidism is usually chronic and causes symptoms such as fatigue, constipation, and cold intolerance. Pale skin, sparse hair, periorbital puffiness, and macroglossia may sometimes progress to a stuporous state and generalized edema. Diagnosis is made by the presence of decreased serum thyroxine and increased thyroid-stimulating hormone levels.6 Superior vena cava syndrome is a manifestation of dilation of the veins in the upper thorax and neck, accompanied by plethora, facial edema, headache, and reduced consciousness. The condition leads to gradual and progressive swelling over days to weeks and is often caused by a malignancy directly compressing the vena cava.7
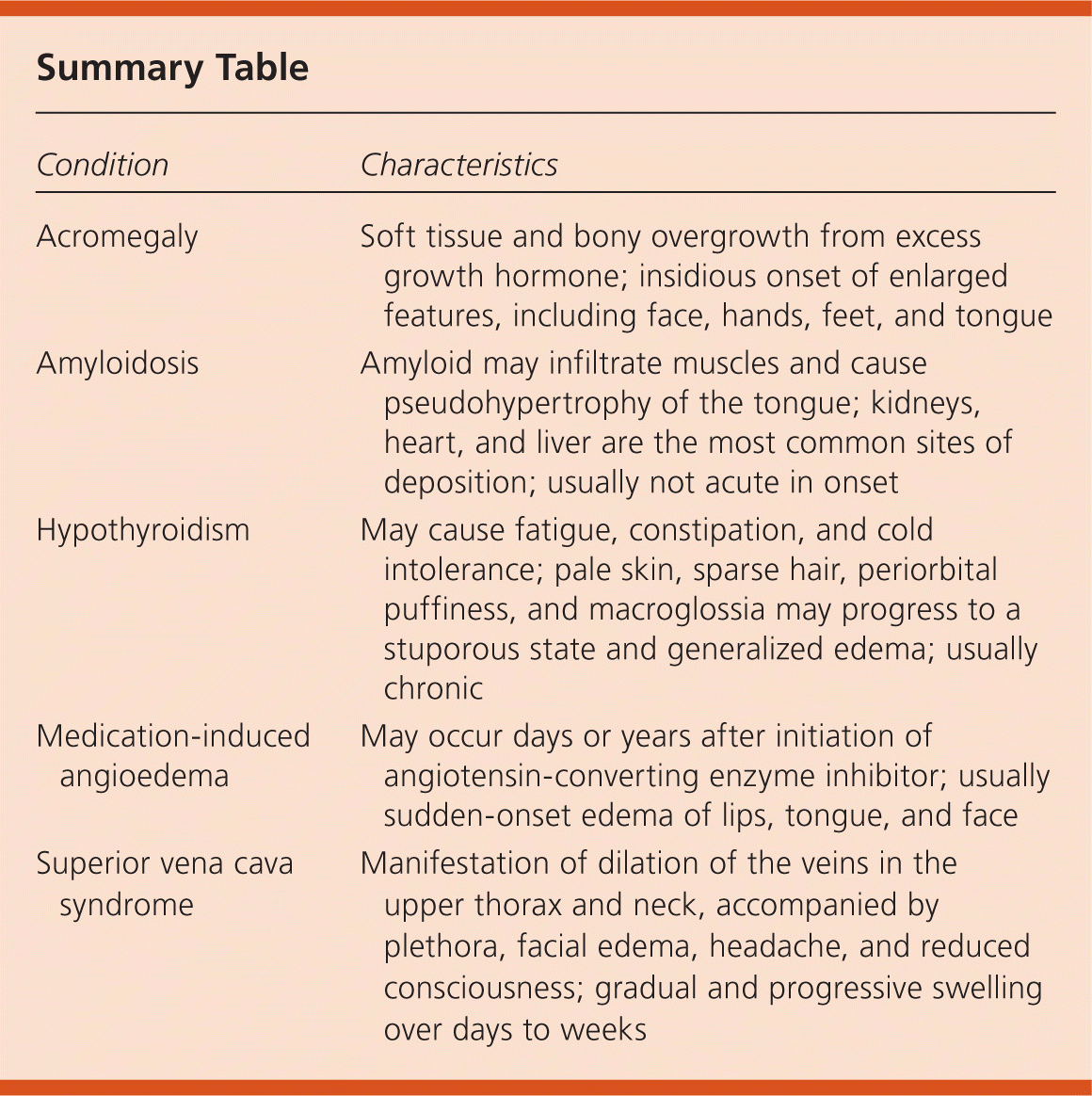
| Condition | Characteristics |
|---|---|
| Acromegaly | Soft tissue and bony overgrowth from excess growth hormone; insidious onset of enlarged features, including face, hands, feet, and tongue |
| Amyloidosis | Amyloid may infiltrate muscles and cause pseudohypertrophy of the tongue; kidneys, heart, and liver are the most common sites of deposition; usually not acute in onset |
| Hypothyroidism | May cause fatigue, constipation, and cold intolerance; pale skin, sparse hair, periorbital puffiness, and macroglossia may progress to a stuporous state and generalized edema; usually chronic |
| Medication-induced angioedema | May occur days or years after initiation of angiotensin-converting enzyme inhibitor; usually sudden-onset edema of lips, tongue, and face |
| Superior vena cava syndrome | Manifestation of dilation of the veins in the upper thorax and neck, accompanied by plethora, facial edema, headache, and reduced consciousness; gradual and progressive swelling over days to weeks |