Osteoporosis is an important and often overlooked problem in men. Although the lifetime risk of hip fracture is lower in men than in women, men are twice as likely to die after a hip fracture. Bone mineral density measurement with a T-score of −2.5 or less indicates osteoporosis. The American College of Physicians recommends beginning periodic osteoporosis risk assessment in men before 65 years of age and performing dual-energy x-ray absorptiometry for men at increased risk of osteoporosis who are candidates for drug therapy. All men diagnosed with osteoporosis should be evaluated for secondary causes of bone loss. The decision regarding treatment of osteoporosis should be based on clinical evaluation, diagnostic workup, fracture risk assessments, and bone mineral density measurements. Pharmacotherapy is recommended for men with osteoporosis and for high-risk men with low bone mass (osteopenia) with a T-score of −1 to −2.5. Bisphosphonates are the first-line agents for treating osteoporosis in men. Teriparatide (i.e., recombinant human parathyroid hormone) is an option for men with severe osteoporosis. Testosterone therapy is beneficial for men with osteoporosis and hypogonadism. Adequate intake of calcium and vitamin D should be encouraged in all men to maintain bone mass. Men should be educated regarding lifestyle measures, which include weight-bearing exercise, limiting alcohol consumption, and smoking cessation. Fall prevention strategies should be implemented in older men at risk of falls.
Osteoporosis in men is an important public health problem, and its prevalence is increasing as the population ages.1 Although traditionally considered a women's health issue, osteoporosis-related mortality and morbidity rates are higher in men.1 The consequences of osteoporosis are underestimated, and the condition is often unrecognized and untreated in most men.2
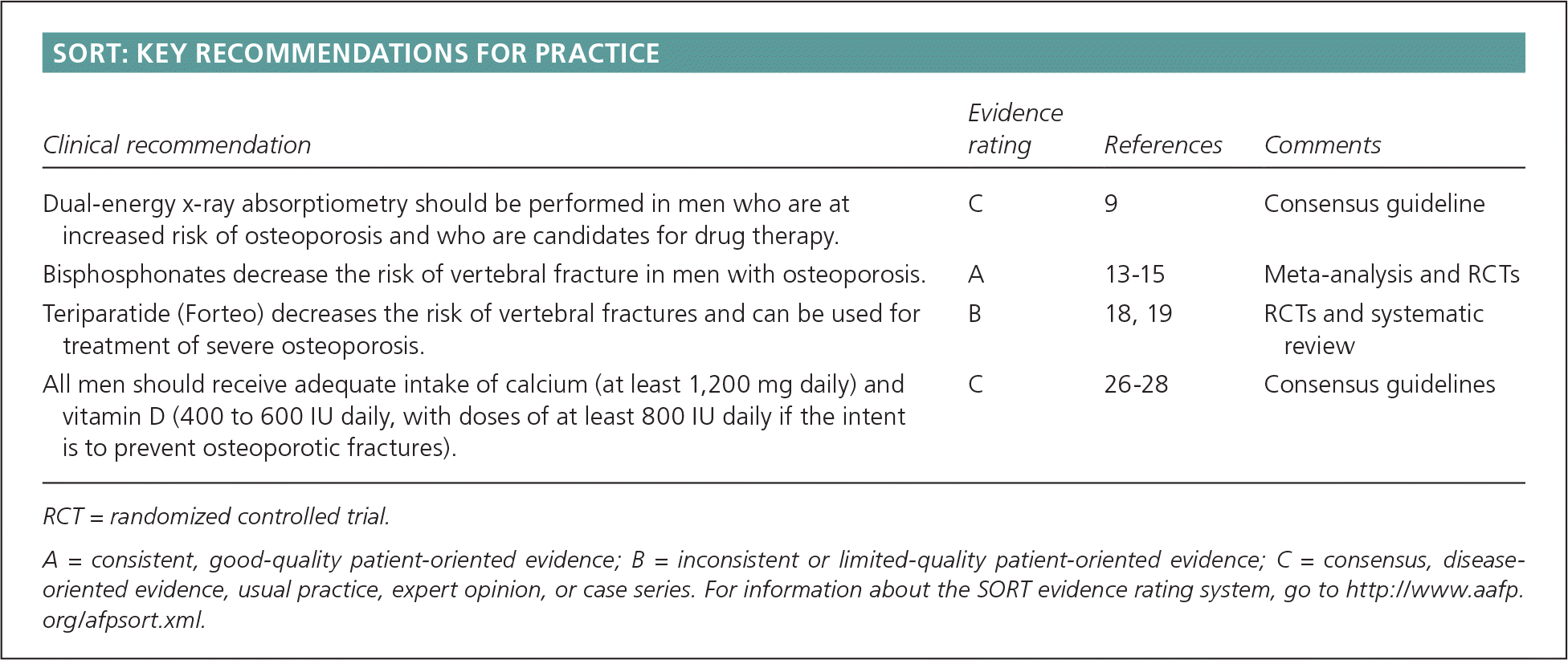
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Dual-energy x-ray absorptiometry should be performed in men who are at increased risk of osteoporosis and who are candidates for drug therapy. | C | 9 | Consensus guideline |
| Bisphosphonates decrease the risk of vertebral fracture in men with osteoporosis. | A | 13–15 | Meta-analysis and RCTs |
| Teriparatide (Forteo) decreases the risk of vertebral fractures and can be used for treatment of severe osteoporosis. | B | 18, 19 | RCTs and systematic review |
| All men should receive adequate intake of calcium (at least 1,200 mg daily) and vitamin D (400 to 600 IU daily, with doses of at least 800 IU daily if the intent is to prevent osteoporotic fractures). | C | 26–28 | Consensus guidelines |
RCT = randomized controlled trial.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Diagnostic Criteria
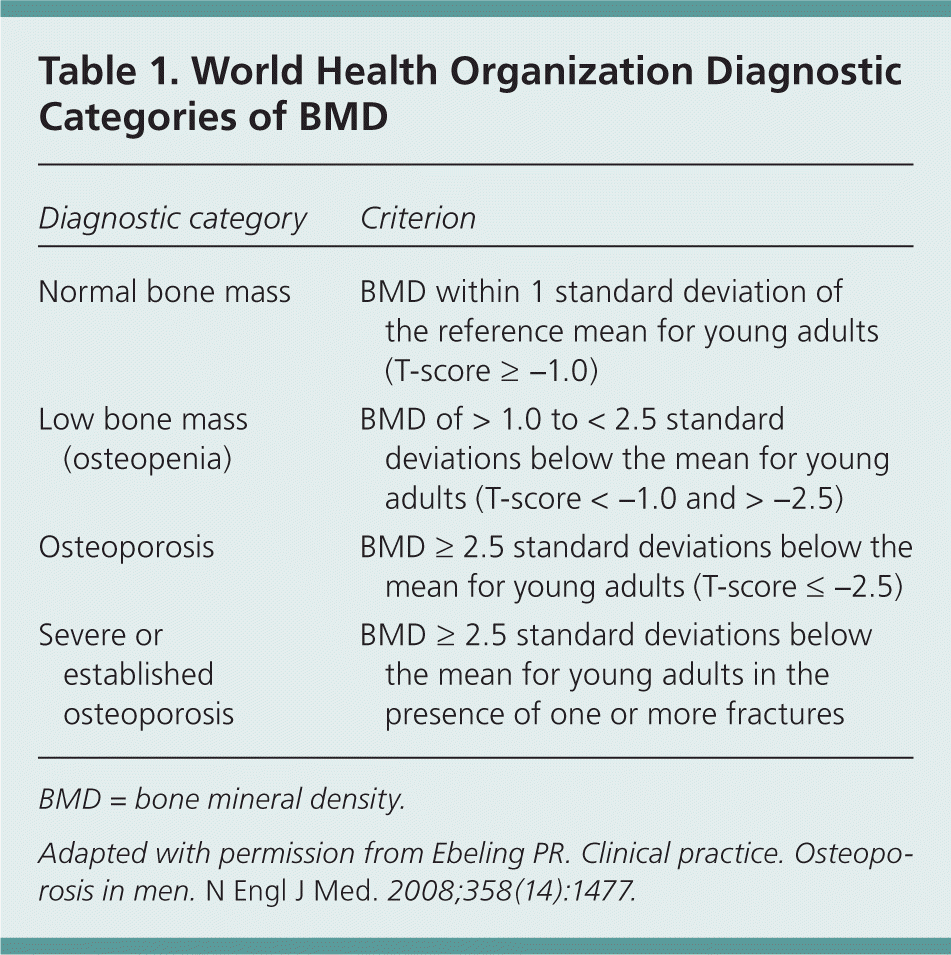
The World Health Organization (WHO) established diagnostic criteria for osteoporosis using bone mineral density (BMD) measurements.3 BMD is reported in T-scores and z scores. A T-score is the number of standard deviations above or below the mean BMD among young adults matched for sex and race (but not age). It classifies patients into three diagnostic categories: normal BMD, low bone mass (i.e., osteopenia), or osteoporosis (Table 1).4 To define osteoporosis, the International Society for Clinical Densitometry recommends using absolute BMD and a T-score of −2.5 or less, based on the male reference database.5 The validity of defining osteoporosis in men using BMD is unclear. However, it is generally agreed that T-scores are useful for identifying men at higher risk of fractures.
Table 1. World Health Organization Diagnostic Categories of BMD
| Diagnostic category | Criterion |
|---|---|
| Normal bone mass | BMD within 1 standard deviation of the reference mean for young adults (T-score ≥ −1.0) |
| Low bone mass (osteopenia) | BMD of > 1.0 to < 2.5 standard deviations below the mean for young adults (T-score < −1.0 and > −2.5) |
| Osteoporosis | BMD ≥ 2.5 standard deviations below the mean for young adults (T-score ≤ −2.5) |
| Severe or established osteoporosis | BMD ≥ 2.5 standard deviations below the mean for young adults in the presence of one or more fractures |
BMD = bone mineral density.
Adapted with permission from Ebeling PR. Clinical practice. Osteoporosis in men. N Engl J Med. 2008;358(14):1477.
The z score reports the patient's BMD as the number of standard deviations above or below the mean for age, sex, and race. A z score of −2.0 or less is below the expected range for age, and it may increase the likelihood of a secondary form of osteoporosis.5 Z scores are important for the diagnosis of osteoporosis in children and in men younger than 50 years.
Epidemiology
An estimated 1 to 2 million men in the United States have osteoporosis, and an additional 8 to 13 million have low bone mass.1 As in women, the risk of fracture in men increases with age. However, the peak incidence of fractures occurs about 10 years later in men than in women. About 13 percent of white U.S. men older than 50 years will experience at least one osteoporotic fracture in their lifetime.6 Hip fracture is the most serious complication of osteoporosis and results in higher overall mortality in men than in women.7 Compared with women, men are about two times more likely to die in the hospital after a hip fracture.8
Pathogenesis
Osteoporosis in men occurs from a complex interplay of different factors, including age-related sex hormone deficiency, genetics, and lifestyle choices (e.g., physical inactivity, tobacco and excessive alcohol use), as well as specific risk factors (e.g., corticosteroid excess) that cause bone loss and microarchitectural disruption. As men get older, production of estradiol and testosterone decreases. Unlike in women, who experience an abrupt decline in estrogen levels at menopause that leads to accelerated bone loss, men have slower bone loss with a smaller overall decrease in BMD. In men, bone loss occurs in the form of trabecular thinning, whereas in women there is a loss of trabeculae.
Risk Factors and Screening
The incidence of hip fracture in men increases substantially after the age of 70 years. In addition to age, risk factors for osteoporosis in men include low body weight (i.e., body mass index of less than 20 to 25 kg per m2), weight loss of more than 10 percent of body weight, physical inactivity, corticosteroid use, androgen deprivation therapy (e.g., for prostate cancer), previous fragility fracture, and spinal cord injury.9
The U.S. Preventive Services Task Force does not make any specific recommendations on osteoporosis screening in men. The American College of Physicians proposes that physicians initiate periodic risk assessment in older men before the age of 65 years; based on a meta-analysis, it recommends dual-energy x-ray absorptiometry (DEXA) in men at increased risk of osteoporosis who are candidates for drug therapy.9
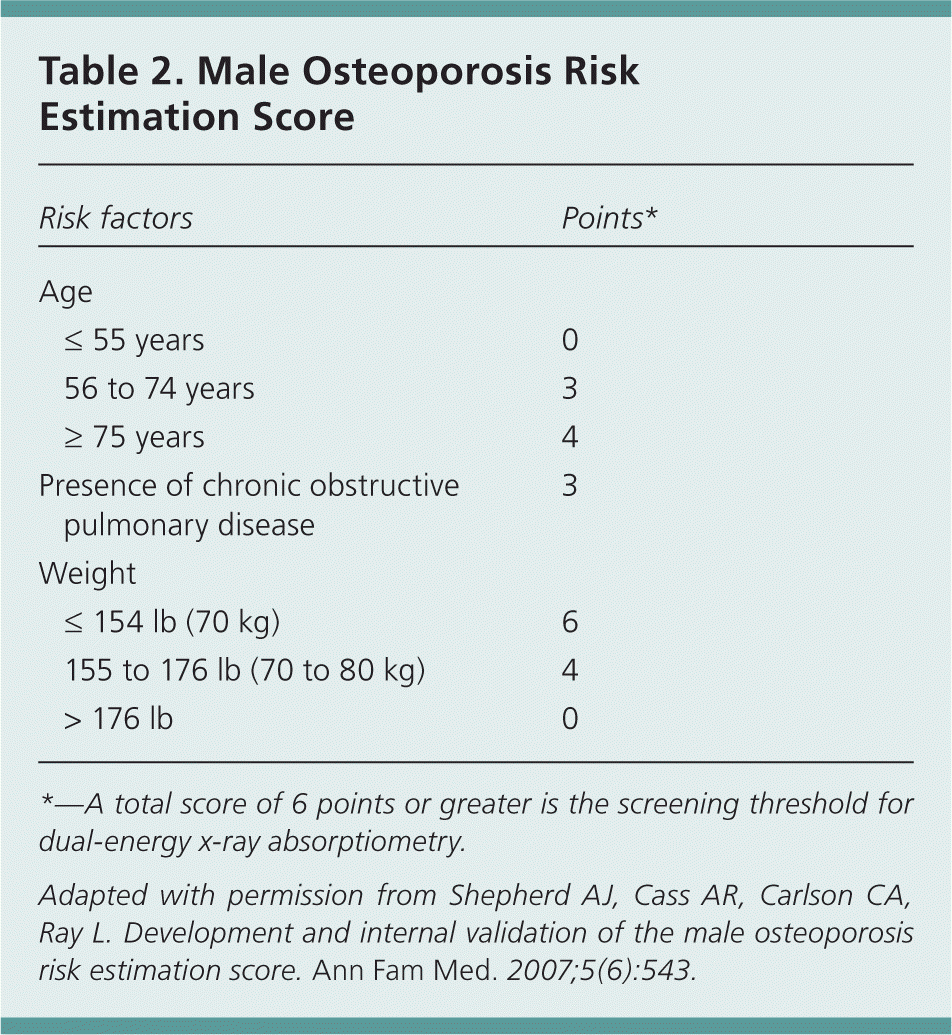
The male osteoporosis risk estimation score (MORES) is a clinically useful approach to identifying men 60 years and older who are at risk of osteoporosis and who should be referred for confirmatory DEXA.10 MORES uses a simple scoring system (Table 210 ) that includes three variables: age, weight, and history of chronic obstructive pulmonary disease. In a study evaluating the clinical utility of MORES, a score of 6 or greater resulted in an overall sensitivity of 93 percent (95% confidence interval [CI], 85 to 97 percent).10 Using MORES, the number needed to screen for 10-year prevention of hip fracture is 279.10
Table 2. Male Osteoporosis Risk Estimation Score
| Risk factors | Points* | |
|---|---|---|
| Age | ||
| ≤55 years | 0 | |
| 56 to 74 years | 3 | |
| ≥75 years | 4 | |
| Presence of chronic obstructive pulmonary disease | 3 | |
| Weight | ||
| ≤ 154 lb (70 kg) | 6 | |
| 155 to 176 lb (70 to 80 kg) | 4 | |
| > 176 lb | 0 | |
*—A total score of 6 points or greater is the screening threshold for dual-energy x-ray absorptiometry.
Adapted with permission from Shepherd AJ, Cass AR, Carlson CA, Ray L. Development and internal validation of the male osteoporosis risk estimation score. Ann Fam Med. 2007;5(6):543.
Secondary Causes
The role of laboratory testing in terms of diagnostic yield and cost-effectiveness for evaluating osteoporosis in men is unclear. It is important to consider and exclude secondary causes of bone loss in all men diagnosed with osteoporosis (Table 34 ). Hypogonadism, corticosteroid use, smoking, excessive alcohol consumption, low calcium intake, and vitamin D deficiency are common secondary causes of osteoporosis in men. A careful history, physical examination, and routine laboratory testing can identify most secondary causes. Initial laboratory evaluation in all men diagnosed with osteoporosis should include a complete blood count, liver function testing, and measurement of thyroid-stimulating hormone, serum testosterone, creatinine, calcium, and serum 25-hydroxyvitamin D levels. Measuring 24-hour urine calcium and creatinine levels to identify hypercalciuria may be indicated in men with idiopathic osteoporosis that occurs before the age of 60 years, or if initial diagnostic methods fail to determine a cause of low bone mass. Up to 40 percent of cases of osteoporosis in men are primary or idiopathic.4
Table 3. Causes of Osteoporosis in Men

| Causes | Clinical clues and tests |
|---|---|
| Common | |
| Corticosteroids | At least 5 mg prednisone daily for > 3 months |
| Family history | Family history of minimal-trauma fracture |
| Lifestyle | Smoking; high alcohol consumption (i.e., > 2 drinks daily) |
| Primary or secondary hypogonadism | Low testosterone levels; medication use (e.g., corticosteroids, opioids, androgen deprivation therapy) |
| Vitamin D deficiency and low calcium intake | Serum 25-hydroxyvitamin D < 30 ng per mL [74.88 nmol per L]; after correction for renal disease, urinary calcium < 50 mg daily suggests inadequate calcium and/or vitamin D intake |
| Less common | |
| Antiepileptic drugs | Use of phenytoin (Dilantin), phenobarbital, primidone (Mysoline), or carbamazepine (Tegretol) |
| Chronic liver or kidney disease | Elevated creatinine; elevated liver enzymes or other abnormalities of liver function tests |
| Cushing syndrome | 24-hour urine for free cortisol; consider testing in men with clinical signs of Cushing syndrome and unexplained vertebral fractures |
| Eating disorders | Low body mass index (< 20 to 25 kg per m2); preoccupation with weight; hypotension; electrolyte abnormalities |
| HIV infection | Positive HIV antibodies; treatment with protease inhibitors |
| Hypercalciuria | High urinary calcium (> 250 mg daily) may suggest excessive intake of calcium or vitamin D, or impaired renal retention of calcium |
| Malabsorption (e.g., celiac disease) | Low levels of serum 25-hydroxyvitamin D and/or urinary calcium; positive tissue transglutaminase antibodies |
| Mastocytosis | Fractures, unexplained osteoporosis, and bone pain; high serum tryptase levels (> 20 ng per mL [20 mcg per L]) |
| Multiple myeloma or other monoclonal gammopathies | Anemia; renal insufficiency; elevated calcium and erythrocyte sedimentation rate; abnormal immunoglobulin protein (M protein) on serum and urine protein electrophoresis |
| Organ transplantation | Use of immunosuppressive agents (e.g., cyclosporine [Sandimmune], tacrolimus [Prograf]) |
| Osteogenesis imperfecta | Fractures; hearing loss; positive collagen type I genetic test |
| Osteomalacia | Serum 25-hydroxyvitamin D may be very low (< 15 ng per mL [37.44 nmol per L]); high-normal or elevated alkaline phosphatase and low-normal or low serum calcium or phosphorous |
| Primary or secondary hyperparathyroidism | High parathyroid hormone (may be caused by inadequate calcium and/or vitamin D intake); serum calcium and phosphorous may be normal or high |
| Rheumatoid arthritis or ankylosing spondylitis | High rheumatoid factor, cyclic citrullinated peptide, and erythrocyte sedimentation rate |
| Thyrotoxicosis or thyroxine over-replacement | Low thyroid-stimulating hormone, high free T4 |
| Type 1 or 2 diabetes mellitus | High fasting glucose, random glucose, or A1C |
note: Additional testing for secondary causes is based on clinical or routine laboratory evaluation. Initial laboratory testing should include complete blood count; liver function test; and thyrotropin, serum testosterone, 25-hydroxyvitamin D, calcium, and creatinine levels (consider measuring 24-hour urine calcium and creatinine).
HIV = human immunodeficiency virus.
Adapted with permission from Ebeling PR. Clinical practice. Osteoporosis in men. N Engl J Med. 2008;358(14):1475.
Clinical Features
Osteoporosis in the absence of a fracture is an asymptomatic condition. DEXA is obtained less often in men. Consequently, fractures causing significant pain, disability, and functional impairment may be the initial presentation in most men with osteoporosis. In addition, men may present with a loss of height. The most common fracture sites in men are the hip, vertebrae, forearm, and humerus.8
Treatment
The decision regarding osteoporosis treatment should be based on clinical evaluation, diagnostic workup, fracture risk assessments, and BMD measurements. In 2008, the WHO developed the Fracture Risk Assessment Tool (FRAX; available at http://www.shef.ac.uk/FRAX), which estimates the 10-year risk of major osteoporotic fracture and hip fracture.3 This Web-based tool takes into account BMD score and other clinical risk factors, including personal and family history of fracture, age, weight, race, sex, corticosteroid use, smoking, and alcohol consumption.
Recent guidelines recommend treatment for men 50 years and older who present with any of the following: hip or vertebral fracture; T-score of −2.5 or less at the femoral neck or spine after appropriate evaluation to exclude secondary causes; or low bone mass (T-score between −1.0 and −2.5 at the femoral neck or spine) and a 10-year hip fracture risk of at least 3 percent or a 10-year major fracture risk of at least 20 percent (as calculated using the FRAX).11,12
PHARMACOTHERAPY
Oral Bisphosphonates. Bisphosphonates are potent antiresorptive agents and are the mainstay of pharmacotherapy for osteoporosis. Bisphosphonates are also effective in men with bone loss from secondary causes, such as corticosteroid use, androgen deprivation therapy, rheumatologic disorders, and hypogonadism.8 A randomized, placebo-controlled trial of 241 men with osteoporosis who were treated with alendronate (Fosamax) reported an increase in BMD in the spine and femoral neck, and a reduction in the incidence of vertebral fracture.13 Vertebral fractures occurred in 8.1 percent of men in the placebo group versus 3.1 percent of men in the alendronate group (P = .12; absolute risk reduction [ARR] = 5 percent; number needed to treat [NNT] = 20). A meta-analysis comparing the effectiveness of alendronate with placebo, calcium, or vitamin D showed a reduction in vertebral fractures among men treated with alendronate (odds ratio of incident vertebral fractures = 0.44; 95% CI, 0.23 to 0.83).14 (see Editor's Note) [updated]
Intravenous Bisphosphonates. Intravenous bisphosphonates (e.g., zoledronic acid [Reclast], ibandronate [Boniva]) are options for men who cannot tolerate oral bisphosphonates. A recent randomized controlled trial demonstrated that zoledronic acid infusion within 90 days after repair of a hip fracture improved survival and was associated with a reduction in the rate of new clinical fractures (ARR = 5.3 percent; NNT = 19; P = .001).16 There were no cases of osteonecrosis of the jaw in participants taking zoledronic acid.16
Recombinant Human Parathyroid Hormone. Intermittent injection of parathyroid hormone (PTH) directly stimulates bone formation. There is good evidence that recombinant human PTH (teriparatide [Forteo]) increases BMD at the lumbar spine and femoral neck in men with osteoporosis.17 In a placebo-controlled trial, 437 men with a BMD more than two standard deviations below the young adult mean were randomized to receive teriparatide (20 or 40 mcg per day) or placebo.18 The treatment group had a dose-related increase in BMD at the spine (5.4 percent with 20 mcg dose; 9 percent with 40 mcg dose) and femoral neck (1.5 percent with 20 mcg dose; 2.9 percent with 40 mcg dose) compared with placebo. In another randomized study, teriparatide was associated with an increase in BMD of the spine and hip, and a reduction in vertebral fractures.19 Compared with placebo, the men treated with teriparatide showed a 51 percent reduction in the incidence of new vertebral fractures (ARR = 6 percent; NNT = 17; P = .07).19
Teriparatide is indicated in men who have severe osteoporosis or multiple risk factors for fracture, or in whom treatment with bisphosphonates has failed. It is recommended that the use of teriparatide be limited to two years.20 Data do not support combining PTH with a bisphosphonate. In a study of 83 men with low BMD, treatment with PTH alone increased BMD more than alendronate alone or the combination of both.21
Testosterone. Testosterone therapy increases BMD in men who have low levels of testosterone. No trials have evaluated the effect of testosterone on fractures. A meta-analysis of eight trials enrolling 365 men showed that intramuscular testosterone was associated with an 8 percent gain in lumbar BMD compared with placebo (95% CI, 4 to 13 percent).22 So far, the benefits of testosterone have been seen only with intramuscular formulations. The value of testosterone therapy in men with normal testosterone levels is controversial.
Other Agents. Calcitonin and the selective estrogen receptor modulator raloxifene (Evista) have shown clear benefit in treating women with osteoporosis.23,24 However, there are no good-quality studies evaluating their fracture risk reduction in men.
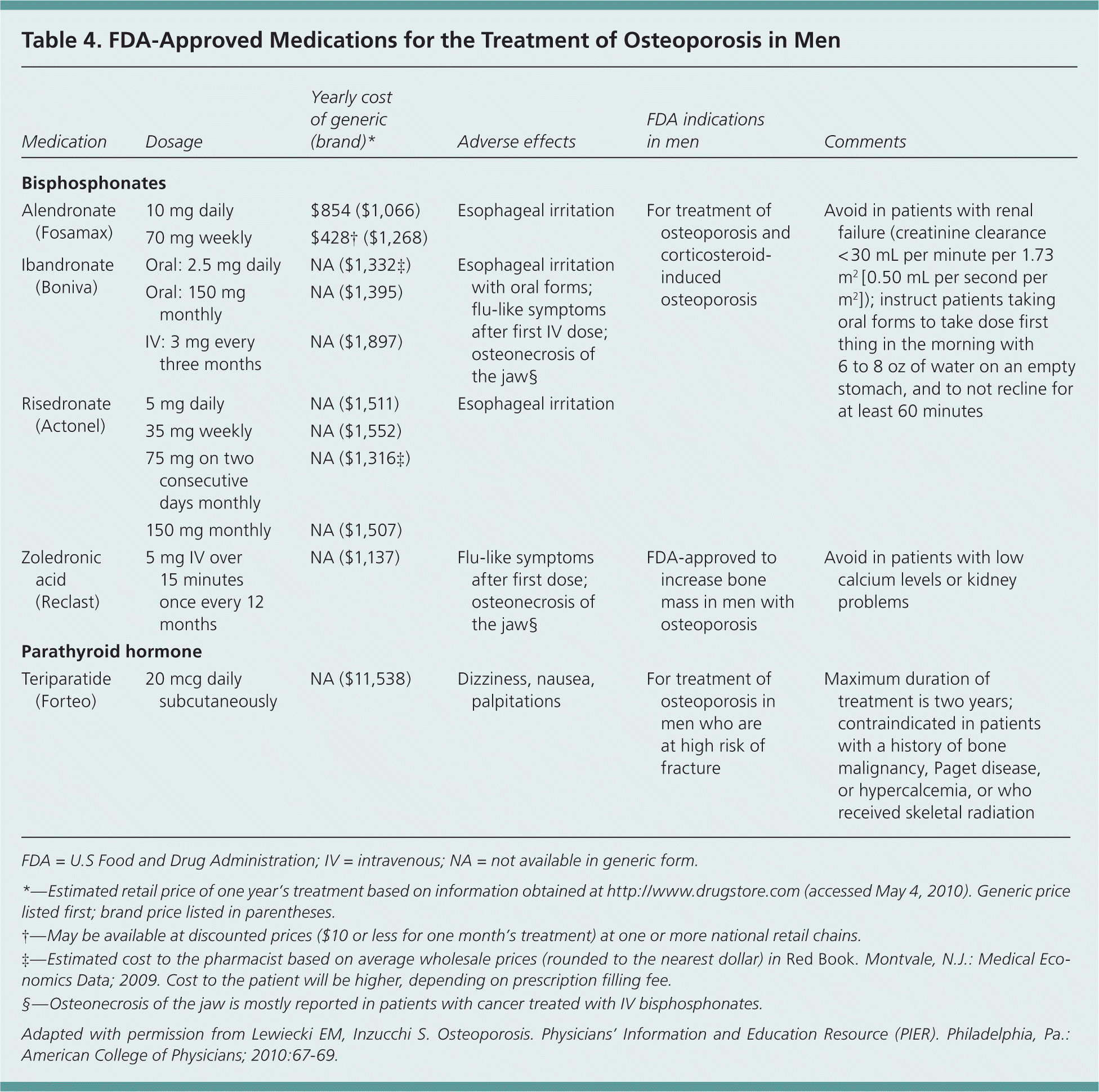
Table 4. FDA-Approved Medications for the Treatment of Osteoporosis in Men
| Medication | Dosage | Yearly cost of generic (brand)* | Adverse effects | FDA indications in men | Comments |
|---|---|---|---|---|---|
| Bisphosphonates | |||||
| Alendronate(Fosamax) | 10 mg daily | $854 ($1,066) | Esophageal irritation | For treatment of osteoporosis and corticosteroid- induced osteoporosis | Avoid in patients with renal failure (creatinine clearance < 30 mL per minute per 1.73 m2 [0.50 mL per second per m2]); instruct patients taking oral forms to take dose first thing in the morning with6 to 8 oz of water on an empty stomach, and to not recline for at least 60 minutes |
| 70 mg weekly | $428†($1,268) | ||||
| Ibandronate (Boniva) | Oral: 2.5 mg daily | NA ($1,332‡) | Esophageal irritation with oral forms; flu-like symptoms after first IV dose; osteonecrosis of the jaw§ | ||
| Oral: 150 mg monthly | NA ($1,395) | ||||
| IV: 3 mg every three months | NA ($1,897) | ||||
| Risedronate (Actonel) | 5 mg daily | NA ($1,511) | Esophageal irritation | ||
| 35 mg weekly | NA ($1,552) | ||||
| 75 mg on two consecutive days monthly | NA ($1,316‡) | ||||
| 150 mg monthly | NA ($1,507) | ||||
| Zoledronic acid (Reclast) | 5 mg IV over 15 minutes once every 12months | NA ($1,137) | Flu-like symptoms after first dose; osteonecrosis of the jaw§ | FDA-approved to increase bone mass in men with osteoporosis | Avoid in patients with low calcium levels or kidney problems |
| Parathyroid hormone | |||||
| Teriparatide (Forteo) | 20 mcg daily subcutaneously | NA ($11,538) | Dizziness, nausea, palpitations | For treatment of osteoporosis in men who are at high risk of fracture | Maximum duration of treatment is two years; contraindicated in patients with a history of bone malignancy, Paget disease, or hypercalcemia, or who received skeletal radiation |
FDA = U.S Food and Drug Administration; IV = intravenous; NA = not available in generic form.
*—Estimated retail price of one year's treatment based on information obtained at http://www.drugstore.com (accessed May 4, 2010). Generic price listed first; brand price listed in parentheses.
†—May be available at discounted prices ($10 or less for one month's treatment) at one or more national retail chains.
‡—Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, N.J.: Medical Economics Data; 2009. Cost to the patient will be higher, depending on prescription filling fee.
§—Osteonecrosis of the jaw is mostly reported in patients with cancer treated with IV bisphosphonates.
Adapted with permission from Lewiecki EM, Inzucchi S. Osteoporosis. Physicians' Information and Education Resource (PIER). Philadelphia, Pa.: American College of Physicians; 2010:67–69.
CALCIUM AND VITAMIN D
Calcium alone or in combination with vitamin D reduces fracture risk by 12 percent in men and women 50 years and older (NNT = 63).26 The Food and Nutrition Board at the Institute of Medicine has established a daily intake for calcium and vitamin D sufficient to maintain bone health and normal calcium metabolism in healthy persons.27 The calcium intake in men older than 50 years is 1,200 mg. The vitamin D intake in men 51 to 70 years of age is 400 IU, and in men older than 70 years is 600 IU. However, the recommended intake for preventing osteoporotic fractures is at least 800 IU per day.26 Most experts agree that the goal is to maintain serum 25-hydroxyvitamin D levels above 30 ng per mL (74.88 nmol per L).28
LIFESTYLE
All men should be counseled on lifestyle measures, such as smoking cessation and limiting alcohol consumption to less than two drinks per day. Weight-bearing exercise can increase BMD in older men.29 It also is important to implement fall prevention strategies (e.g., gait training), minimize the use of psychotropic medications, and eliminate environmental hazards.
Editor's Note: On September 1, 2016, JAMA Internal Medicine published a Notice of Retraction regarding Reference #15 “due to acknowledgment of scientific misconduct resulting in concerns about data integrity and inappropriate assignment of authorship.” The relevant text of this article has been omitted. Risedronate remains FDA-approved for treatment of osteoporosis in men.

