Pulmonary rehabilitation is a nonpharmacologic therapy that has emerged as a standard of care for patients with chronic obstructive pulmonary disease. It is a comprehensive, multidisciplinary, patient-centered intervention that includes patient assessment, exercise training, self-management education, and psychosocial support. In the United States, pulmonary rehabilitation is usually given in outpatient, hospital-based programs lasting six to 12 weeks. Positive outcomes from pulmonary rehabilitation include increased exercise tolerance, reduced dyspnea and anxiety, increased self-efficacy, and improvement in health-related quality of life. Hospital admissions after exacerbations of chronic obstructive pulmonary disease are also reduced with this intervention. The positive outcomes associated with pulmonary rehabilitation are realized without demonstrable improvements in lung function. This paradox is explained by the fact that pulmonary rehabilitation identifies and treats the systemic effects of the disease. This intervention should be considered in patients who remain symptomatic or have decreased functional status despite optimal medical management. Medicare now covers up to 36 sessions of pulmonary rehabilitation in patients with moderate, severe, and very severe chronic obstructive pulmonary disease.
Chronic obstructive pulmonary disease (COPD) is characterized by progressive airflow limitation that is not fully reversible, leading to adverse respiratory effects and systemic sequelae. Damage is thought to be mediated by an inflammatory response to toxic substances in the lung, especially cigarette smoke.1 Optimal clinical management of COPD generally requires pharmacologic and nonpharmacologic therapy. This review focuses on pulmonary rehabilitation, an important nonpharmacologic treatment option for patients with chronic respiratory diseases, such as COPD.
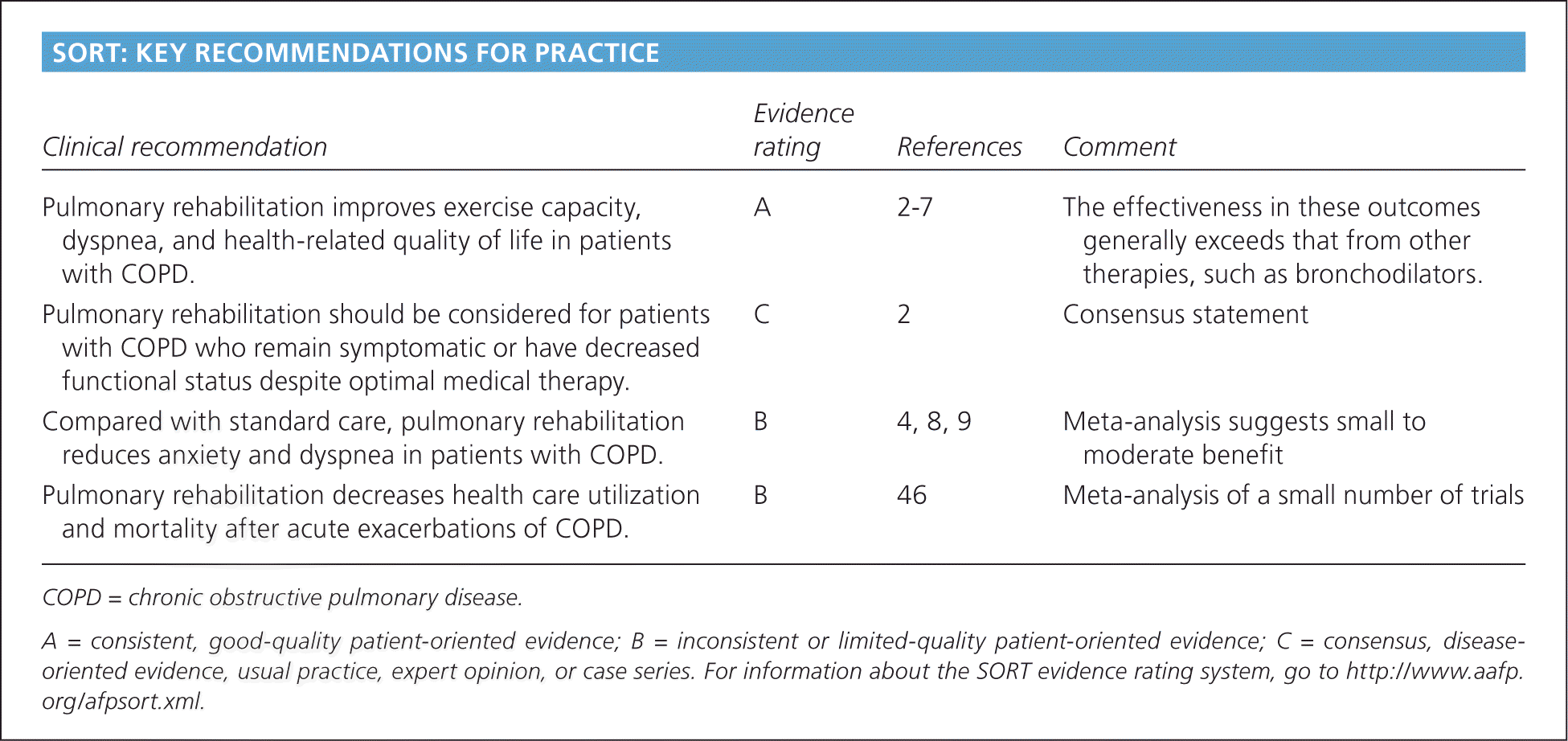
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comment |
|---|---|---|---|
| Pulmonary rehabilitation improves exercise capacity, dyspnea, and health-related quality of life in patients with COPD. | A | 2–7 | The effectiveness in these outcomes generally exceeds that from other therapies, such as bronchodilators. |
| Pulmonary rehabilitation should be considered for patients with COPD who remain symptomatic or have decreased functional status despite optimal medical therapy. | C | 2 | Consensus statement |
| Compared with standard care, pulmonary rehabilitation reduces anxiety and dyspnea in patients with COPD. | B | 4, 8, 9 | Meta-analysis suggests small to moderate benefit |
| Pulmonary rehabilitation decreases health care utilization and mortality after acute exacerbations of COPD. | B | 46 | Meta-analysis of a small number of trials |
COPD = chronic obstructive pulmonary disease.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Pulmonary rehabilitation is an evidence-based, multidisciplinary, and comprehensive intervention for symptomatic patients who may have decreased functional status.2 The goals are to reduce symptoms, optimize functional status, increase participation, and reduce health care costs by stabilizing or reversing systemic manifestations of chronic respiratory disease.2
In the United States, pulmonary rehabilitation is most often a hospital-based, outpatient program that includes patient assessment, exercise training, education, and psychosocial support. Although most pulmonary rehabilitation programs include these aspects, they may vary considerably in their structure. Most programs involve two to three hours of education and exercise, three times weekly for six to 12 weeks. Progress toward specific educational and exercise goals is required. At minimum, pulmonary rehabilitation programs require a medical director and pulmonary rehabilitation coordinator. The latter may be a nurse, physical therapist, or respiratory therapist. Occupational therapists, exercise physiologists, pharmacists, psychologists, dietitians, and social workers may also be included. Medicare recently began covering up to 36 sessions of pulmonary rehabilitation for patients with moderate, severe, or very severe COPD, based on spirometric criteria. Although the availability of pulmonary rehabilitation has been limited in some parts of the United States, this improved Medicare funding may help improve accessibility.
Compared with other available therapies, including bronchodilators, pulmonary rehabilitation generally confers the greatest improvements in dyspnea, exercise capacity, and health-related quality of life.3 As a result, pulmonary rehabilitation is now an integral part of virtually all major guidelines for the treatment of COPD, including the American Thoracic Society/European Respiratory Society standards for diagnosis and management of COPD (Figure 1).1
Figure 1.
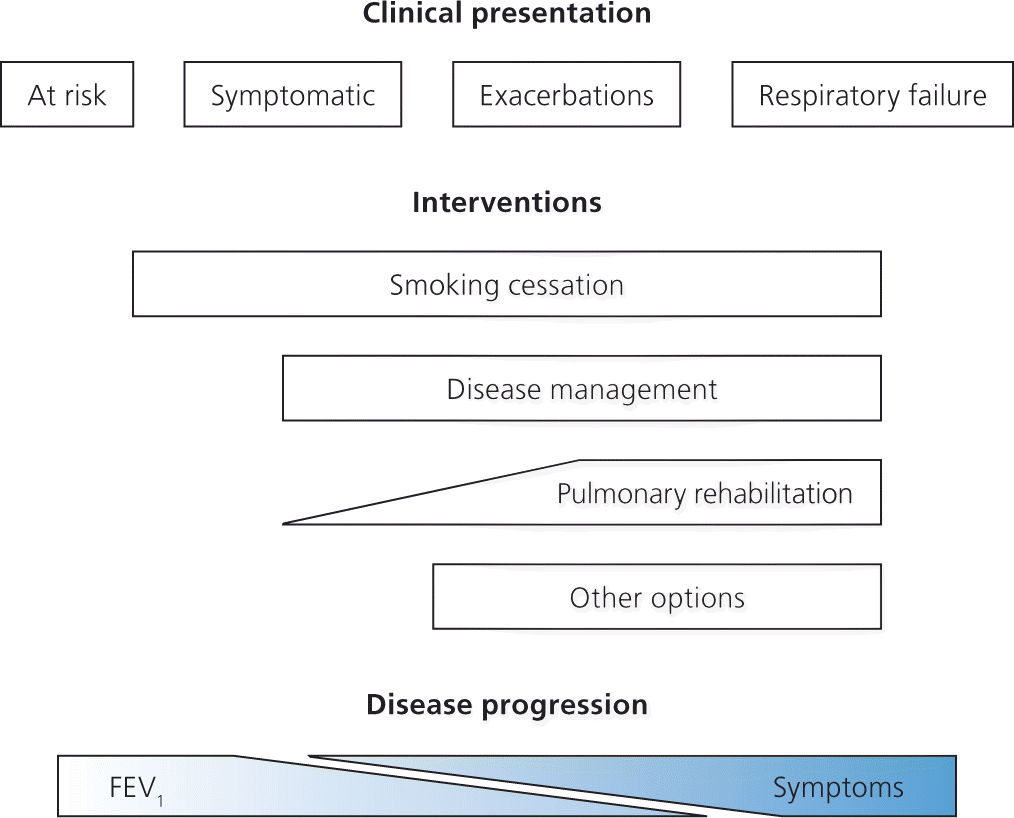
Continuum of care for patients with chronic obstructive pulmonary disease (COPD). As symptoms and functional limitations increase, the need for pulmonary rehabilitation increases. (FEV1 = forced expiratory volume in one second.)
Adapted with permission from Celli BR, MacNee W; ATS/ERS Task Force. Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS/ERS position paper. Eur Respir J. 2004;23(6):943.
Outcomes and Rationale
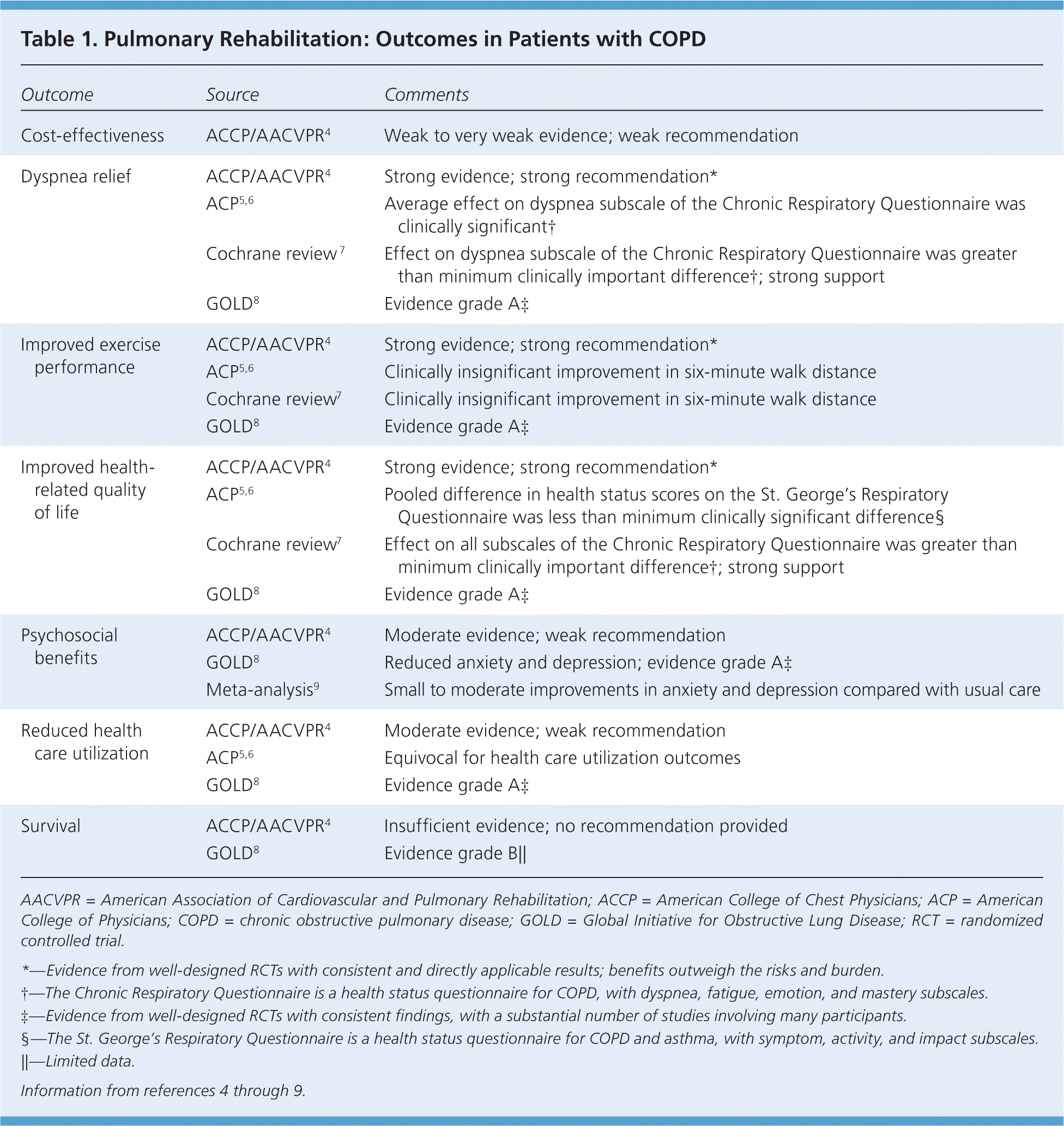
Multiple evidence-based reviews have evaluated the effect of pulmonary rehabilitation on COPD outcomes, including exercise performance, dyspnea relief, quality of life, health care utilization, cost-effectiveness, psychosocial benefits, and survival (Table 1).4–9
Table 1. Pulmonary Rehabilitation: Outcomes in Patients with COPD
| Outcome | Source | Comments |
|---|---|---|
| Cost-effectiveness | ACCP/AACVPR4 | Weak to very weak evidence; weak recommendation |
| Dyspnea relief | ACCP/AACVPR4 | Strong evidence; strong recommendation* |
| ACP5,6 | Average effect on dyspnea subscale of the Chronic Respiratory Questionnaire was clinically significant† | |
| Cochrane review 7 | Effect on dyspnea subscale of the Chronic Respiratory Questionnaire was greater than minimum clinically important difference†; strong support | |
| GOLD8 | Evidence grade A‡ | |
| Improved exercise performance | ACCP/AACVPR4 | Strong evidence; strong recommendation* |
| ACP5,6 | Clinically insignificant improvement in six-minute walk distance | |
| Cochrane review7 | Clinically insignificant improvement in six-minute walk distance | |
| GOLD8 | Evidence grade A‡ | |
| Improved health-related quality of life | ACCP/AACVPR4 | Strong evidence; strong recommendation* |
| ACP5,6 | Pooled difference in health status scores on the St. George's Respiratory Questionnaire was less than minimum clinically significant difference§ | |
| Cochrane review7 | Effect on all subscales of the Chronic Respiratory Questionnaire was greater than minimum clinically important difference†; strong support | |
| GOLD8 | Evidence grade A‡ | |
| Psychosocial benefits | ACCP/AACVPR4 | Moderate evidence; weak recommendation |
| GOLD8 | Reduced anxiety and depression; evidence grade A‡ | |
| Meta-analysis9 | Small to moderate improvements in anxiety and depression compared with usual care | |
| Reduced health care utilization | ACCP/AACVPR4 | Moderate evidence; weak recommendation |
| ACP5,6 | Equivocal for health care utilization outcomes | |
| GOLD8 | Evidence grade A‡ | |
| Survival | ACCP/AACVPR4 | Insufficient evidence; no recommendation provided |
| GOLD8 | Evidence grade B∥ |
AACVPR = American Association of Cardiovascular and Pulmonary Rehabilitation; ACCP = American College of Chest Physicians; ACP = American College of Physicians; COPD = chronic obstructive pulmonary disease; GOLD = Global Initiative for Obstructive Lung Disease; RCT = randomized controlled trial.
*—Evidence from well-designed RCTs with consistent and directly applicable results; benefits outweigh the risks and burden.
†—The Chronic Respiratory Questionnaire is a health status questionnaire for COPD, with dyspnea, fatigue, emotion, and mastery subscales.
‡—Evidence from well-designed RCTs with consistent findings, with a substantial number of studies involving many participants.
§—The St. George's Respiratory Questionnaire is a health status questionnaire for COPD and asthma, with symptom, activity, and impact subscales.
∥—Limited data.
The beneficial effects of pulmonary rehabilitation are realized without a demonstrable effect on traditional lung function measurements, such as forced expiratory volume in one second (FEV1). This paradox is explained by the fact that pulmonary rehabilitation identifies and treats the systemic effects of COPD and its common comorbidities.2,3 Prominent systemic effects of COPD include peripheral muscle dysfunction resulting from physical inactivity or systemic inflammation10; muscle wasting11; inadequate selfmanagement skills12; and anxiety and depression.13 Systemic effects and comorbid conditions contribute to the disease burden and may be amenable to therapy. For example, physical conditioning of leg muscles through exercise training reduces lactate production and decreases ventilatory burden.14 A lower ventilatory burden allows the patient to breathe more slowly during exercise, thereby reducing dynamic hyperinflation.15 These effects reduce exertional dyspnea, even without a change in FEV1.
Components of Pulmonary Rehabilitation
Essential components of pulmonary rehabilitation include patient selection and assessment, exercise training, psychosocial support, and self-management education.16
PATIENT SELECTION AND ASSESSMENT
Pulmonary rehabilitation is patient centered; therefore, an initial assessment and goal setting are important. The initial assessment sets the stage for subsequent treatment. Because there are no randomized controlled studies of the assessment process, the strength of evidence is weak, and recommendations are based primarily on expert opinion.2,16
Indications for pulmonary rehabilitation include persistent respiratory symptoms (especially dyspnea) or functional status limitation despite optimal medical therapy.2 Contraindications include conditions that substantially increase risk during rehabilitation (e.g., unstable angina) or conditions that substantially interfere with the rehabilitative process. In many cases, the underlying contraindication can be treated or the pulmonary rehabilitation can be adapted so that the patient can participate.
Pulmonary rehabilitation guidelines state that based on expert opinion, the degree of airflow limitation (as measured by FEV1) is not a major selection criterion for pulmonary rehabilitation, but that symptom burden and functional status limitation are the major indications.2 However, a recent evidence-based practice guideline from the American College of Physicians recommends that physicians consider pulmonary rehabilitation for patients with an FEV1 less than 50 percent of that predicted. 6 It states that the evidence is not clear whether pulmonary rehabilitation is beneficial in patients whose FEV1 is greater than 50 percent of that predicted. The recommendation was graded as weak, based on moderate-quality evidence in the randomized clinical trials that were reviewed. The recommendation contradicts expert opinion that symptomatic patients may benefit from pulmonary rehabilitation, regardless of their FEV1.2,16 The severity of COPD, including its symptom burden, is clearly influenced by more than airflow limitation alone.17
EXERCISE TRAINING
Comprehensive exercise training, including upper- and lower-extremity endurance training and strength training, is an essential component of pulmonary rehabilitation (Table 2).4 COPD can be considered a disease of the peripheral muscles,18 with decreased mass, alterations in fiber-type distribution, and decreased metabolic capacity contributing to exercise intolerance.19–22 These abnormalities may be amenable to exercise training. Higher levels of exercise training are associated with a physiologic training effect, dose-dependent increases in oxidative enzymes in ambulatory muscles, and greater improvement in exercise performance.14,23,24
Table 2. Guidelines for Exercise Training in Patients with COPD

| Recommendation | Strength of evidence |
|---|---|
| Lower-extremity exercise training should be a mandatory component of pulmonary rehabilitation. | Strong evidence; strong recommendation |
| Low- and high-intensity exercise training produces clinical benefits for patients with COPD. | Strong evidence; strong recommendation |
| Lower-extremity exercise training performed at a high level of intensity produces greater physiologic benefits than lower-intensity training. | Moderate evidence; strong recommendation |
| Unsupported upper-extremity endurance training should be included in pulmonary rehabilitation exercise programs. | Strong evidence; strong recommendation |
| Including a strength training component in a pulmonary rehabilitation exercise program increases muscle strength and muscle mass. | Strong evidence; strong recommendation |
| There is no evidence to support the routine use of inspiratory muscle training as an essential component of pulmonary rehabilitation. | Moderate evidence; strong recommendation |
COPD = chronic obstructive pulmonary disease.
Information from reference 4.
Exercise training is based on general principles of intensity (higher intensity produces greater results), specificity (only those muscles trained show an effect), and reversibility (cessation of regular exercise training results in a decrease in training effect).25 Although patients with COPD often have ventilatory limitations to maximal exercise, a physiologic training effect can be achieved if high training targets are used.26 Exercise intensity of 60 to 80 percent of the patient's peak work rate is often feasible.26
Strength training is also an important component of exercise training and may yield additional benefits.27 Patients who cannot tolerate high levels of exercise training can also benefit from strength training.28 Maximizing bronchodilation, interval training (i.e., alternating high and low intensities), and oxygen supplementation may allow for higher intensity exercise training in some patients.29–34 The optimal duration of training has not been established but depends on the progress of the individual patient. Guidelines from the Global Initiative for Chronic Obstructive Lung Disease state that six weeks (with three sessions per week) is the minimum duration of an effective program,8 but longer duration confers greater benefits.
SELF-MANAGEMENT EDUCATION
Self-management education is an integral component of pulmonary rehabilitation.2,4 It promotes self-efficacy 35–37 and encourages active participation in health care.38,39 Self-management education has been shown to be highly effective in improving health status and reducing health care utilization.40 It is usually provided in small group settings and in a one-on-one format. An initial evaluation helps determine educational needs, which are then reassessed during the course of the program. Discussions about advance directives are an important part of self-management education,41,42 as is counseling about early recognition and treatment of COPD exacerbations.4
PSYCHOSOCIAL SUPPORT
Anxiety, depression, coping problems, and decreased self-efficacy contribute to the burden of advanced respiratory disease.43–45 Although there is minimal evidence to support psychosocial interventions as a single therapeutic modality in patients with COPD, benefits are derived from comprehensive pulmonary rehabilitation programs that include these types of interventions.4,8
A systematic review and meta-analysis that included three randomized trials comparing comprehensive pulmonary rehabilitation with standard care showed that pulmonary rehabilitation led to small to moderate improvements in anxiety and dyspnea.9 Psychosocial and behavioral interventions vary among pulmonary rehabilitation programs, but often involve educational sessions or support groups that focus on coping strategies and stress management. Patients' family members and friends are also encouraged to participate in these support groups. Patients with substantial psychiatric disease should be referred for appropriate care.
Pulmonary Rehabilitation After Acute COPD Exacerbations
COPD exacerbations are responsible for substantial health care utilization and carry a high mortality risk. Recent studies indicate that pulmonary rehabilitation is beneficial shortly after an acute exacerbation of COPD. In an analysis of six trials involving 219 patients with COPD exacerbations, pulmonary rehabilitation significantly reduced hospital admissions and mortality, and improved exercise capacity and health-related quality of life.46
Maintaining Benefits and Integrating Care
The positive outcomes from pulmonary rehabilitation tend to diminish over months to years after discontinuation of the program.47 The reasons for this decline are multifactorial and include decreasing adherence to the exercise program; exacerbations of COPD; development of comorbidities; and longitudinal deterioration from the disease itself. Many programs provide postrehabilitation maintenance; however, the effects on long-term outcomes have not been established. Selfmanagement education may promote long-term adherence to the exercise program, but this has not been proven.
For years, pulmonary rehabilitation has used an integrated, interdisciplinary model in the management of chronic respiratory disease. Integration of services is necessary to provide a seamless transition of care across settings (hospital, rehabilitation, and community) and disciplines (primary care, subspecialty, home services). Although patient selection and assessment, exercise training, self-management education, and psychosocial support make up an interdisciplinary pulmonary rehabilitation program, these components should be integrated into lifelong COPD management for all patients, even if pulmonary rehabilitation is not available. The primary care physician is in a unique position to provide and coordinate this care across settings.48,49

