A 16-year-old girl presented with fatigue, weight loss, and dysphagia that began several months earlier. She had restless sleep leading to daytime somnolence and poor school performance, and her family reported loud snoring. Her medical history was unremarkable, except for recurrent upper respiratory tract infections.
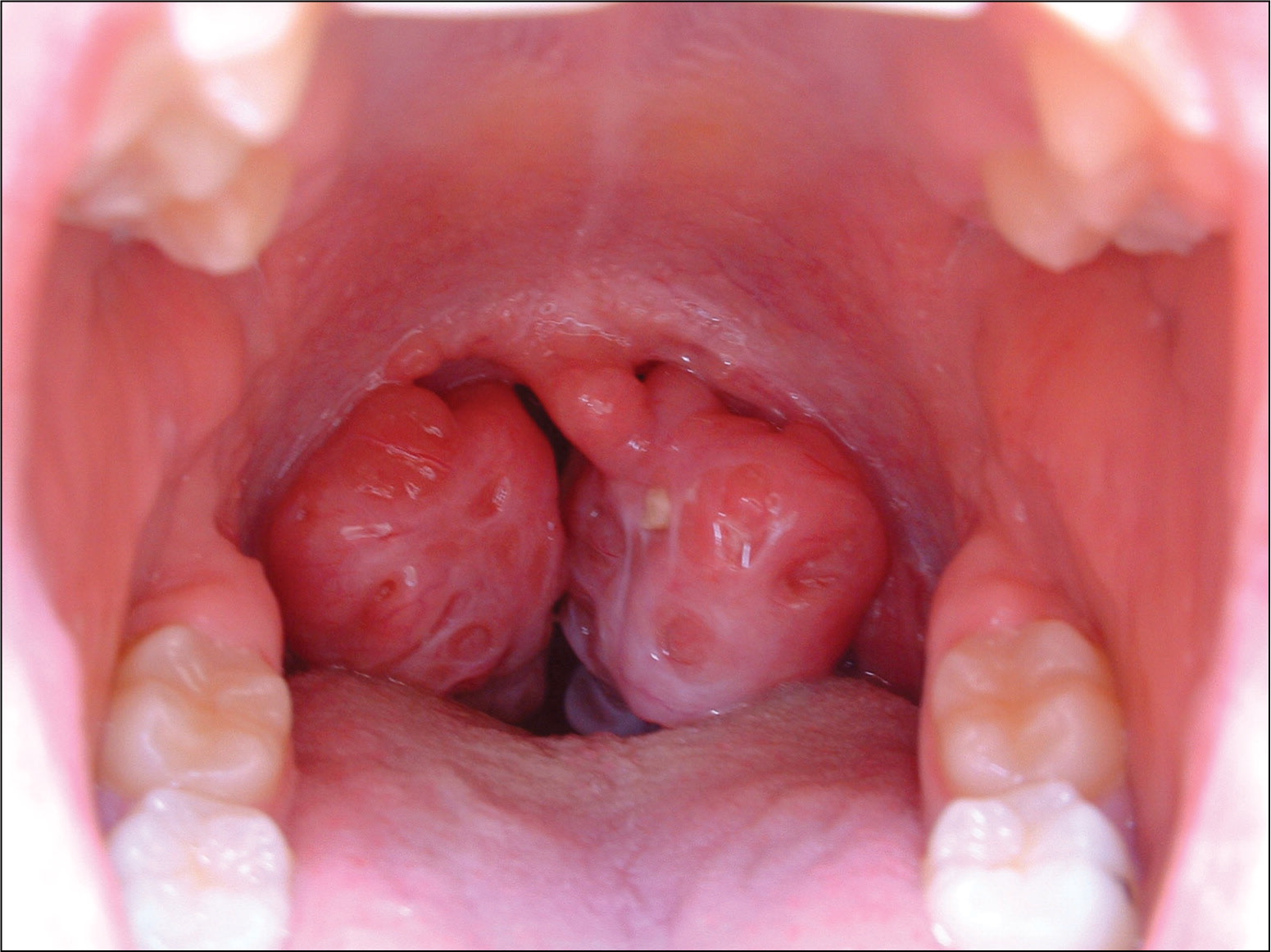
Physical examination revealed noisy respirations with an open mouth, halitosis, and tonsillar swelling (see accompanying figure). She had no fever or lymphadenopathy.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Bilateral tonsillar abscesses.
B. Hypertrophic tonsils.
C. Infectious mononucleosis.
D. Tonsillitis.
Discussion
The answer is B: hypertrophic tonsils. Hypertrophic tonsils can be caused by recurrent pharyngitis and local inflammation, especially in children and young adults. Inspection of the oral cavity may reveal hypertrophy of the palatine tonsils, which is sometimes called “kissing tonsils” when tonsils meet in the midline or overlap. Tonsilloliths may be lodged in the crypts. Although tonsillar enlargement may be asymptomatic, massive tonsils sometimes fall back and occlude the oropharynx, particularly when the patient is recumbent. Most cases of obstructive sleep apnea in children are associated with hypertrophic tonsils.
Symptoms suggestive of tonsillar hypertrophy include difficulty in feeding with small children, mouth breathing, noisy respiration, loud snoring, restless sleep, hypersomnolence, secondary enuresis, night terrors, behavior changes, and poor school performance. Tonsillar hypertrophy may also lead to respiratory and cardiac complications, such as chronic alveolar hypoventilation, pulmonary hypertension, cor pulmonale, and right heart failure.1 Massive tonsillar hypertrophy may require tonsillectomy, especially when associated with obstructive sleep-disordered breathing that causes poor daily cognitive performance, dysphagia, failure to thrive, and cor pulmonale.2,3 This patient's symptoms resolved two weeks after tonsillectomy.
Tonsillar abscess is a severe, suppurative complication of tonsillitis or pharyngitis. It usually presents with intermittent odynophagia, voice changes (“hot potato voice”), and high fever in a young adult.4 Most cases are unilateral with contralateral displacement of the uvula. In patients with bilateral abscesses, examination reveals bilateral swelling of the soft palate with a midline uvula displaced anteriorly. Group A streptococci and anaerobic bacteria of the oral flora are common causes of this condition. Surgical treatment and parenteral antibiotics may be required.
Infectious mononucleosis usually affects patients 15 to 30 years of age. The most common symptoms include fever, sore throat, and malaise. Examination shows pharyngeal injection with exudates. Patients often have posterior cervical lymphadenopathy. 4
Tonsillitis is one of the most common infections encountered by family physicians. Patients have sore throat, acute fever, and pain on swallowing. Physical examination reveals pharyngeal swelling, tonsillar erythema and exudates, and tender anterior cervical lymphadenopathy. Viruses are the most common causes of tonsillitis, although group A beta-hemolytic streptococcus accounts for 5 to 30 percent of cases. Streptococcal infection requires an antibiotic regimen.4
Summary Table
| Condition | Characteristics |
|---|---|
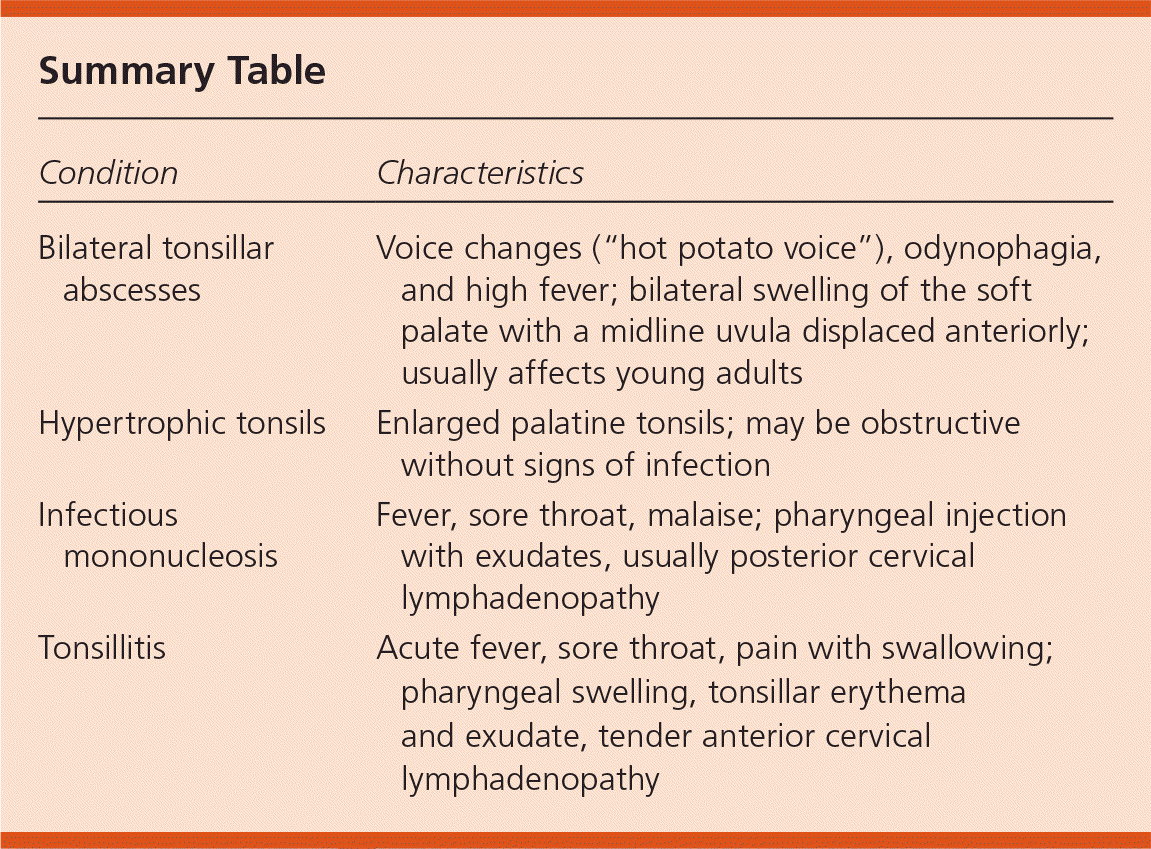
| Bilateral tonsillar abscesses | Voice changes (“hot potato voice”), odynophagia, and high fever; bilateral swelling of the soft palate with a midline uvula displaced anteriorly; usually affects young adults |
| Hypertrophic tonsils | Enlarged palatine tonsils; may be obstructive without signs of infection |
| Infectious mononucleosis | Fever, sore throat, malaise; pharyngeal injection with exudates, usually posterior cervical lymphadenopathy |
| Tonsillitis | Acute fever, sore throat, pain with swallowing; pharyngeal swelling, tonsillar erythema and exudate, tender anterior cervical lymphadenopathy |

