Guideline source: Surgical Infection Society, Infectious Diseases Society of America
Literature search described? Yes
Evidence rating system used? Yes
Published source: Clinical Infectious Diseases, January 15, 2010
Available at: http://www.journals.uchicago.edu/doi/full/10.1086/649554
Intra-abdominal infections are the second most common cause of infectious mortality in intensive care units. Complicated intra-abdominal infection, which extends into the peritoneal space, is associated with abscess formation and peritonitis. Uncomplicated infection, which involves intramural inflammation of the gastrointestinal tract, may progress to complicated infection if left untreated.
Treatment of intra-abdominal infections has evolved in recent years because of advances in supportive care, diagnostic imaging, minimally invasive intervention, and antimicrobial therapy. Based on this new evidence, the Surgical Infection Society and the Infectious Diseases Society of America recently updated recommendations for diagnosis and treatment of these infections. The new guideline includes recommendations for treatment of intra-abdominal infections in children, management of appendicitis, and treatment of necrotizing enterocolitis in newborns.
Initial Evaluation
Routine history, physical examination, and laboratory studies will identify most patients who require further evaluation. Intra-abdominal infection should be considered in patients with unreliable physical examination findings (e.g., those with impaired mental status or spinal cord injury) who present with evidence of infection from an undetermined source. Further diagnostic imaging is not necessary in patients with obvious signs of diffuse peritonitis and in whom immediate surgical intervention is required. Computed tomography (CT) should be performed to determine whether an intra-abdominal infection is present in adults who are not undergoing immediate laparotomy.
Fluid Resuscitation
Rapid restoration of intravascular volume should be undertaken, as should any additional measures necessary to promote physiologic stability. In patients with septic shock, resuscitation should begin immediately after hypotension is identified. In patients with no evidence of volume depletion, intravenous fluid therapy should begin as soon as intra-abdominal infection is suspected.
Interventions
A source control procedure to drain infected foci, control ongoing peritoneal contamination, and restore anatomic and physiologic function is recommended in virtually all patients with intra-abdominal infection. Emergency surgery should be performed in patients with diffuse peritonitis, even if measures to restore physiologic stability must be continued during the procedure. An urgent approach also should be taken in hemodynamically stable patients without evidence of acute organ failure. However, intervention may be delayed for up to 24 hours in closely monitored patients who have started antimicrobial therapy. Select patients with minimal physiologic derangement and a well-circumscribed focus of infection can be treated with antimicrobial therapy without a source control procedure if close clinical follow-up is possible.
In patients with severe peritonitis, relaparotomy is not recommended in the absence of intestinal discontinuity, abdominal fascial loss that prevents abdominal wall closure, or intra-abdominal hypertension.
Laboratory Evaluation
Routine blood cultures and Gram stains are not recommended in patients with community-acquired intra-abdominal infection. Anaerobic cultures are not necessary in these patients if empiric antimicrobial therapy is provided. However, routine aerobic and anaerobic cultures may be of value in determining resistance patterns and follow-up oral therapy in lower-risk patients with community-acquired infection.
In higher-risk patients, cultures should be obtained from the infection site, particularly in those with previous antibiotic exposure. The specimen should be representative of the material associated with the infection and should be of sufficient volume (at least 1 mL). For optimal recovery of aerobic bacteria, 1 to 10 mL of fluid should be inoculated directly into an aerobic blood culture bottle. In addition, 0.5 mL of fluid should be sent to the laboratory for Gram stain testing and, if indicated, fungal cultures. If anaerobic cultures are requested, at least 0.5 mL of fluid or 0.5 g of tissue should be placed in an anaerobic transport tube. Alternately, 1 to 10 mL of fluid can be inoculated directly into an anaerobic blood culture bottle.
Routine culture and susceptibility studies should be performed in patients with perforated appendicitis or other community-acquired intra-abdominal infection if a common community isolate (e.g., Escherichia coli) is resistant to antimicrobials in widespread local use. Susceptibility testing should be performed for Pseudomonas, Proteus, Acinetobacter, Staphylococcus aureus, and predominant Enterobacteriaceae (as determined by moderate-to-heavy growth), because resistance is more likely in these organisms.
Antimicrobial Therapy
Antimicrobial therapy should be started as soon as intra-abdominal infection is diagnosed or suspected. Antibiotics should be administered as soon as possible in patients with septic shock. Those who do not have septic shock should begin antimicrobial therapy in the emergency department. Adequate drug levels should be maintained during the source control procedure, which may necessitate additional administration of antimicrobials.
MILD TO MODERATE COMMUNITY-ACQUIRED INFECTION IN ADULTS
Antibiotics used for empiric treatment of community-acquired intra-abdominal infection should be active against enteric gram-negative aerobic and facultative bacilli and enteric gram-positive streptococci. Coverage for obligate anaerobic bacilli should be provided for distal small bowel, appendiceal, and colon-derived infection and for more proximal gastrointestinal perforations in the presence of obstruction or paralytic ileus.
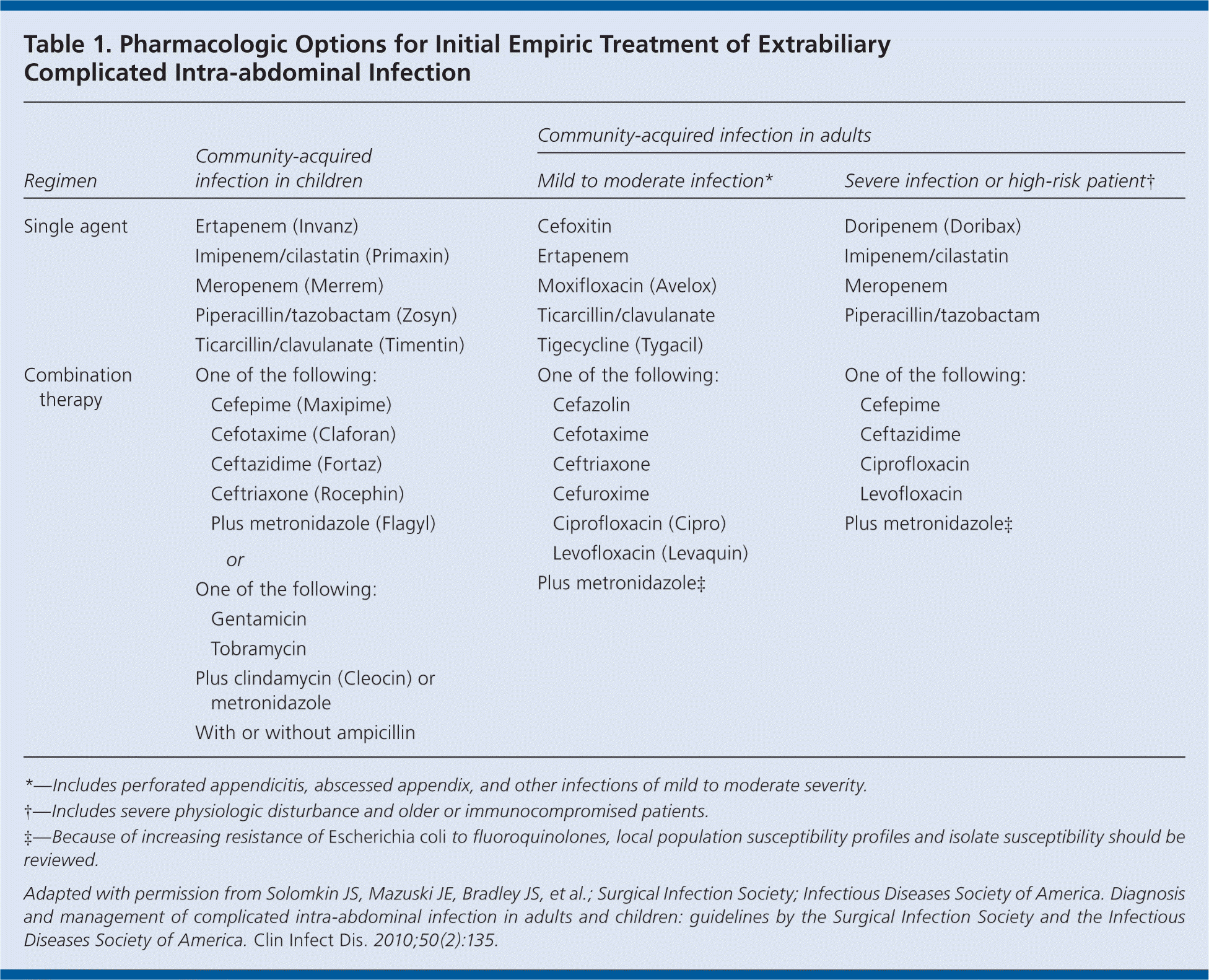
In adults with mild-to-moderate community-acquired infection, the use of ticarcillin/clavulanate (Timentin), cefoxitin, ertapenem (Invanz), moxifloxacin (Avelox), or tigecycline (Tygacil) as a single-agent therapy, or a combination of metronidazole (Flagyl) with cefazolin, cefuroxime, ceftriaxone (Rocephin), cefotaxime (Claforan), levofloxacin (Levaquin), or ciprofloxacin (Cipro) is preferable to regimens with substantial antipseudomonal activity (Table 1).
Table 1. Pharmacologic Options for Initial Empiric Treatment of Extrabiliary Complicated Intra-abdominal Infection
| Regimen | Community-acquired infection in children | Community-acquired infection in adults | ||||
|---|---|---|---|---|---|---|
| Mild to moderate infection* | Severe infection or high-risk† | |||||
| Single agent | Ertapenem (Invanz) | Cefoxitin | Doripenem (Doribax) | |||
| Imipenem/cilastatin (Primaxin) | Ertapenem | Imipenem/cilastatin | ||||
| Meropenem (Merrem) | Moxifloxacin (Avelox) | Meropenem | ||||
| Piperacillin/tazobactam (Zosyn) | Ticarcillin/clavulanate | Piperacillin/tazobactam | ||||
| Ticarcillin/clavulanate (Timentin) | Tigecycline (Tygacil) | |||||
| Combination therapy | One of the following:
| One of the following:
| One of the following:
| |||
| or | ||||||
One of the following:
| ||||||
*—Includes perforated appendicitis, abscessed appendix, and other infections of mild to moderate severity.
†—Includes severe physiologic disturbance and older or immunocompromised patients.
‡—Because of increasing resistance of Escherichia coli to fluoroquinolones, local population susceptibility profiles and isolate susceptibility should be reviewed.
Adapted with permission from Solomkin JS, Mazuski JE, Bradley JS, et al.; Surgical Infection Society; Infectious Diseases Society of America. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50(2):135.
Ampicillin/sulbactam (Unasyn) is not recommended because of high resistance rates in community-acquired E. coli. Cefotetan and clindamycin (Cleocin) are not recommended because of increasing resistance among the Bacteroides fragilis group. Aminoglycosides are not recommended for routine use in adults with community-acquired intra-abdominal infection because less toxic agents are available that are equally effective.
HIGH-RISK COMMUNITY-ACQUIRED INFECTION IN ADULTS
Patients with severe community-acquired intra-abdominal infection should be treated empirically with antimicrobial regimens that have broad-spectrum activity against gram-negative organisms, such as meropenem (Merrem), imipenem/cilastatin (Primaxin), doripenem (Doribax), or piperacillin/tazobactam (Zosyn) as single agents, or a combination of metronidazole with ciprofloxacin, levofloxacin, ceftazidime (Fortaz), or cefepime (Maxipime; Table 1). A combination of aztreonam (Azactam) and metronidazole is an alternative, but the addition of an agent effective against gram-positive cocci is recommended.
The routine use of aminoglycosides is not recommended unless there is evidence that the patient harbors resistant organisms. The use of agents effective against methicillin-resistant S. aureus (MRSA) or yeast is not recommended unless there is evidence of infection with these organisms. Quinolone-resistant strains of E. coli are common in some communities; therefore, quinolones should not be used unless hospital surveys indicate more than 90 percent susceptibility of E. coli to these agents.
HEALTH CARE–ASSOCIATED INFECTION IN ADULTS
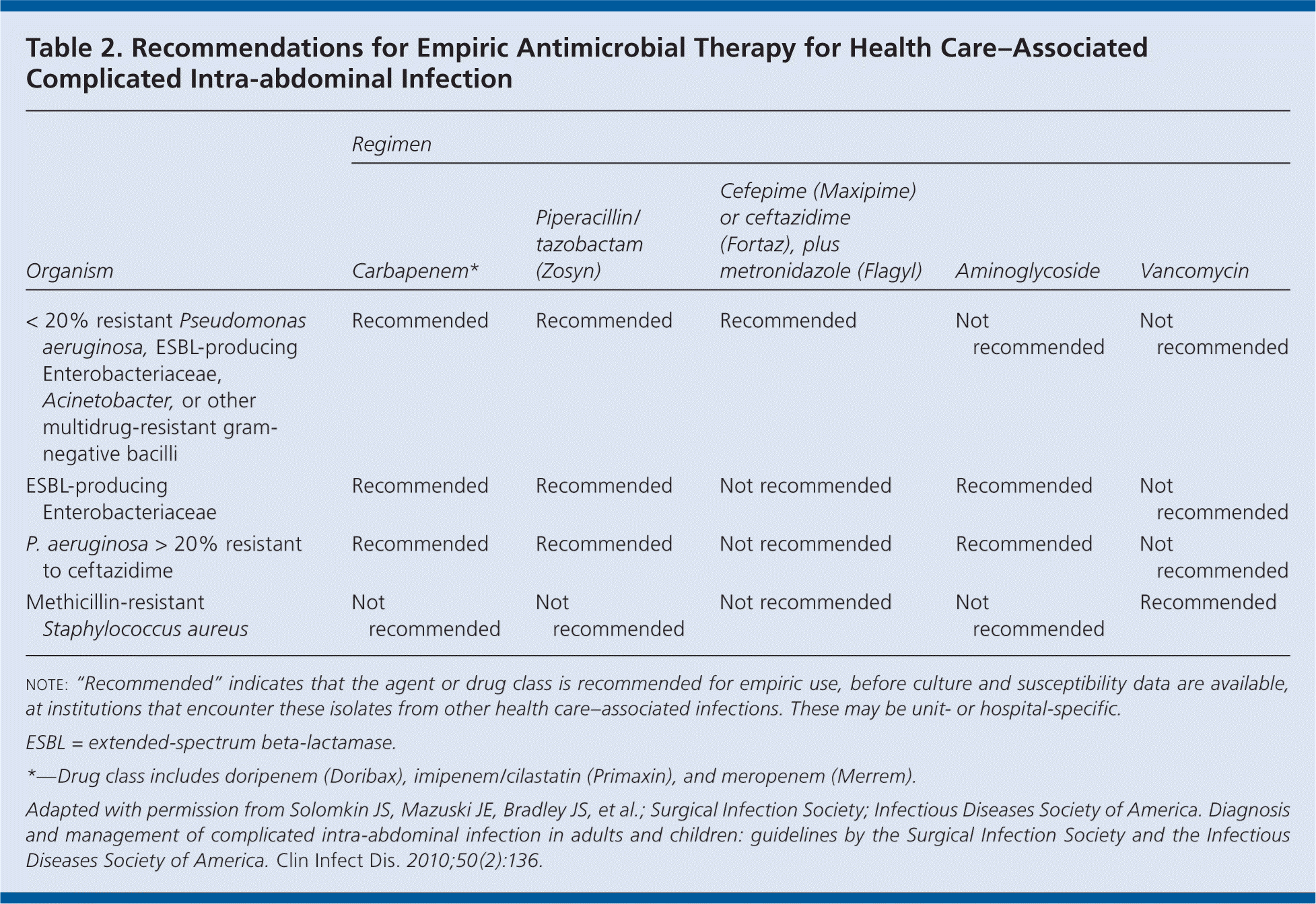
Empiric antibiotic therapy for health care–associated intra-abdominal infection should be driven by local microbiologic results. To achieve empiric coverage of likely pathogens, multidrug regimens that include agents with expanded activity against gram-negative aerobic and facultative bacilli may be necessary (Table 2). Broad-spectrum antimicrobial therapy should be tailored when culture and susceptibility reports become available.
Table 2. Recommendations for Empiric Antimicrobial Therapy for Health Care–Associated Complicated Intra-abdominal Infection
| Organism | Regimen | ||||
|---|---|---|---|---|---|
| Carbapenem* | Piperacillin/tazobactam (Zosyn) | Cefepime (Maxipime) or ceftazidime (Fortaz), plus metronidazole (Flagyl) | Aminoglycoside | Vancomycin | |
| < 20% resistant Pseudomonas aeruginosa, ESBL-producing Enterobacteriaceae, Acinetobacter, or other multidrug-resistant gram-negative bacilli | Recommended | Recommended | Recommended | Not recommended | Not recommended |
| ESBL-producing Enterobacteriaceae | Recommended | Recommended | Not recommended | Recommended | Not recommended |
| P. aeruginosa > 20% resistant to ceftazidime | Recommended | Recommended | Not recommended | Recommended | Not recommended |
| Methicillin-resistant Staphylococcus aureus | Not recommended | Not recommended | Not recommended | Not recommended | Recommended |
note: “Recommended” indicates that the agent or drug class is recommended for empiric use, before culture and susceptibility data are available, at institutions that encounter these isolates from other health care–associated infections. These may be unit- or hospital-specific.
ESBL = extended-spectrum beta-lactamase.
*—Drug class includes doripenem (Doribax), imipenem/cilastatin (Primaxin), and meropenem (Merrem).
Adapted with permission from Solomkin JS, Mazuski JE, Bradley JS, et al.; Surgical Infection Society; Infectious Diseases Society of America. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50(2):136.
CHOLECYSTITIS AND CHOLANGITIS IN ADULTS
Antimicrobial therapy should be initiated in patients with suspected infection and acute cholecystitis or cholangitis (Table 3). However, anaerobic therapy is not indicated unless a biliary-enteric anastomosis is present. If the patient is undergoing cholecystectomy for acute cholecystitis, antimicrobial therapy should be discontinued within 24 hours unless there is evidence of infection outside the wall of the gallbladder.
Table 3. Pharmacologic Options for Initial Empiric Treatment of Biliary Infection in Adults

| Infection | Regimen |
|---|---|
| Community-acquired acute cholecystitis (mild to moderate) | Cefazolin, ceftriaxone (Rocephin), or cefuroxime |
| Community-acquired acute cholecystitis of severe physiologic disturbance, advanced age, or immunocompromised state | One of the following: cefepime (Maxipime), ciprofloxacin (Cipro), doripenem (Doribax), imipenem/cilastatin (Primaxin), levofloxacin (Levaquin), meropenem (Merrem), or piperacillin/tazobactam (Zosyn) |
| Plus metronidazole (Flagyl)* | |
| Acute cholangitis after biliary-enteric anastomosis (any severity) | One of the following: cefepime, ciprofloxacin, doripenem, imipenem/cilastatin, levofloxacin, meropenem, or piperacillin/tazobactam |
| Plus metronidazole* | |
| Health care–associated biliary infection (any severity) | One of the following: cefepime, ciprofloxacin, doripenem, imipenem/cilastatin, levofloxacin, meropenem, or piperacillin/tazobactam |
| Plus metronidazole and vancomycin* |
*—Because of increasing resistance of Escherichia coli to fluoroquinolones, local population susceptibility profiles and isolate susceptibility should be reviewed.
Adapted with permission from Solomkin JS, Mazuski JE, Bradley JS, et al.; Surgical Infection Society; Infectious Diseases Society of America. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50(2):137.
INFECTION IN CHILDREN
Routine use of broad-spectrum antimicrobial agents is not indicated in children with fever and abdominal pain unless complicated appendicitis or other acute intra-abdominal infection is suspected. Selection of antimicrobial regimens should be based on the origin of infection (community versus health care), severity of the illness, and safety profiles of the antimicrobial agents in children.
Acceptable broad-spectrum antimicrobial regimens for children with complicated intra-abdominal infection include aminoglycosides, carbapenems (imipenem/cilastatin, meropenem, or ertapenem), combined betalactam antibiotics or beta-lactamase inhibitors (piperacillin/tazobactam or ticarcillin/clavulanate), and advanced-generation cephalosporins (cefotaxime, ceftriaxone, ceftazidime, or cefepime) with metronidazole (Table 1). For children with severe reactions to beta-lactam antibiotics, a combination of ciprofloxacin and metronidazole or an aminoglycoside-based regimen is recommended.
Necrotizing enterocolitis in newborns is managed with fluid resuscitation, intravenous broad-spectrum antibiotics (possibly including antifungal agents), and bowel decompression. Broad-spectrum antibiotic therapies that may be useful in such cases include ampicillin, gentamicin, and metronidazole; ampicillin, cefotaxime, and metronidazole; or meropenem. Vancomycin may be used instead of ampicillin when MRSA or ampicillin-resistant enterococcal infection is suspected.
ANTIFUNGAL THERAPY
Antifungal therapy for patients with severe community-acquired or health care–associated infection is recommended if Candida is isolated from intra-abdominal cultures. If Candida albicans is isolated, fluconazole (Diflucan) is an appropriate treatment option. For fluconazole-resistant Candida species, an echinocandin (e.g., caspofungin [Cancidas], micafungin [Mycamine], or anidulafungin [Eraxis]) is appropriate. In newborns, empiric antifungal therapy should be initiated if Candida is suspected. An echinocandin should be the initial treatment in critically ill patients. Amphotericin B is not recommended as initial therapy because of its toxicity.
ANTI-ENTEROCOCCAL THERAPY
Antimicrobial therapy for enterococci should be given when enterococci are recovered from patients with health care–associated infection. Empiric anti-enterococcal therapy is recommended in patients with health care–associated intra-abdominal infection, particularly those with postoperative infection; in patients who have previously taken cephalosporins or other antimicrobial agents selecting for Enterococcus species; in immunocompromised patients; and in those with valvular heart disease or prosthetic intravascular materials.
Initial empiric anti-enterococcal therapy should be directed against Enterococcus faecalis. Antibiotics that can be used against this organism include ampicillin, piperacillin/tazobactam, and vancomycin. Empiric therapy for vancomycin-resistant Enterococcus faecium is not recommended unless the patient is at high risk of infection.
ANTI-MRSA THERAPY
Empiric antimicrobial coverage against MRSA should be provided to patients with health care–associated intra-abdominal infection who are colonized with the organism or who are at risk of infection because of previous treatment failure and antibiotic exposure. Vancomycin is recommended for treatment of suspected or proven MRSA intra-abdominal infection.
Diagnosis and Management of Patients with Suspected Acute Appendicitis
A constellation of findings, including characteristic abdominal pain, localized abdominal tenderness, and laboratory evidence of acute inflammation, identifies most patients with suspected appendicitis.
Helical CT of the abdomen and pelvis with intravenous—but not oral or rectal—contrast dye is recommended in patients with suspected appendicitis. A pregnancy test should be performed in women of childbearing age before they undergo imaging; if they are in the first trimester of pregnancy, ultrasonography or magnetic resonance imaging should be used instead of CT. Imaging should be performed in all children in whom the diagnosis of appendicitis is uncertain, particularly in those younger than three years. CT is preferred, but ultrasonography is an alternative if exposure to ionizing radiation is a concern. For patients in whom imaging does not detect appendicitis, follow-up at 24 hours is recommended to ensure resolution of signs and symptoms.
Antimicrobial therapy with agents effective against facultative and aerobic gram-negative organisms and anaerobic organisms should be initiated in all patients diagnosed with appendicitis. In patients with suspected appendicitis who have equivocal imaging findings, antimicrobial therapy should be initiated in combination with pain medication and antipyretics, if indicated. Antimicrobial therapy should continue for at least three days in adults, until clinical symptoms and signs of infection resolve or a definitive diagnosis is made.
Laparoscopy or open appendectomy should be performed as soon as possible in patients with acute, nonperforated appendicitis. Nonsurgical treatment can be considered in select patients with acute, nonperforated appendicitis if there is a marked improvement in the patient's condition before surgery.
Patients with perforated appendicitis should undergo urgent intervention for source control. Percutaneous or operative drainage can be performed, if necessary, in patients with a well-circumscribed periappendiceal abscess. Appendectomy is generally deferred in these patients.

