Sexual behaviors in children are common, occurring in 42 to 73 percent of children by the time they reach 13 years of age. Developmentally appropriate behavior that is common and frequently observed in children includes trying to view another person's genitals or breasts, standing too close to other persons, and touching their own genitals. Sexual behaviors become less common, less frequent, or more covert after five years of age. Sexual behavior problems are defined as developmentally inappropriate or intrusive sexual acts that typically involve coercion or distress. Such behaviors should be evaluated within the context of other emotional and behavior disorders, socialization difficulties, and family dysfunction, including violence, abuse, and neglect. Although many children with sexual behavior problems have a history of sexual abuse, most children who have been sexually abused do not develop sexual behavior problems. Children who have been sexually abused at a younger age, who have been abused by a family member, or whose abuse involved penetration are at greater risk of developing sexual behavior problems. Although age-appropriate behaviors are managed primarily through reassurance and education of the parent about appropriate behavior redirection, sexual behavior problems often require further assessment and may necessitate a referral to child protective services for suspected abuse or neglect.
When parents present to a physician's office because of concerns about their child's sexual behavior, several issues typically arise: parent anxiety, the extent to which the behavior is disruptive in the home or school setting, the origin of the behavior, and effective management of the behavior. Sexual behaviors in children are common, occurring in 42 to 73 percent of children by the time they reach 13 years of age.1–3 Because child sexual abuse has received considerable media attention, it is not unusual for parents to be concerned that sexual behavior means their child has been sexually abused.4
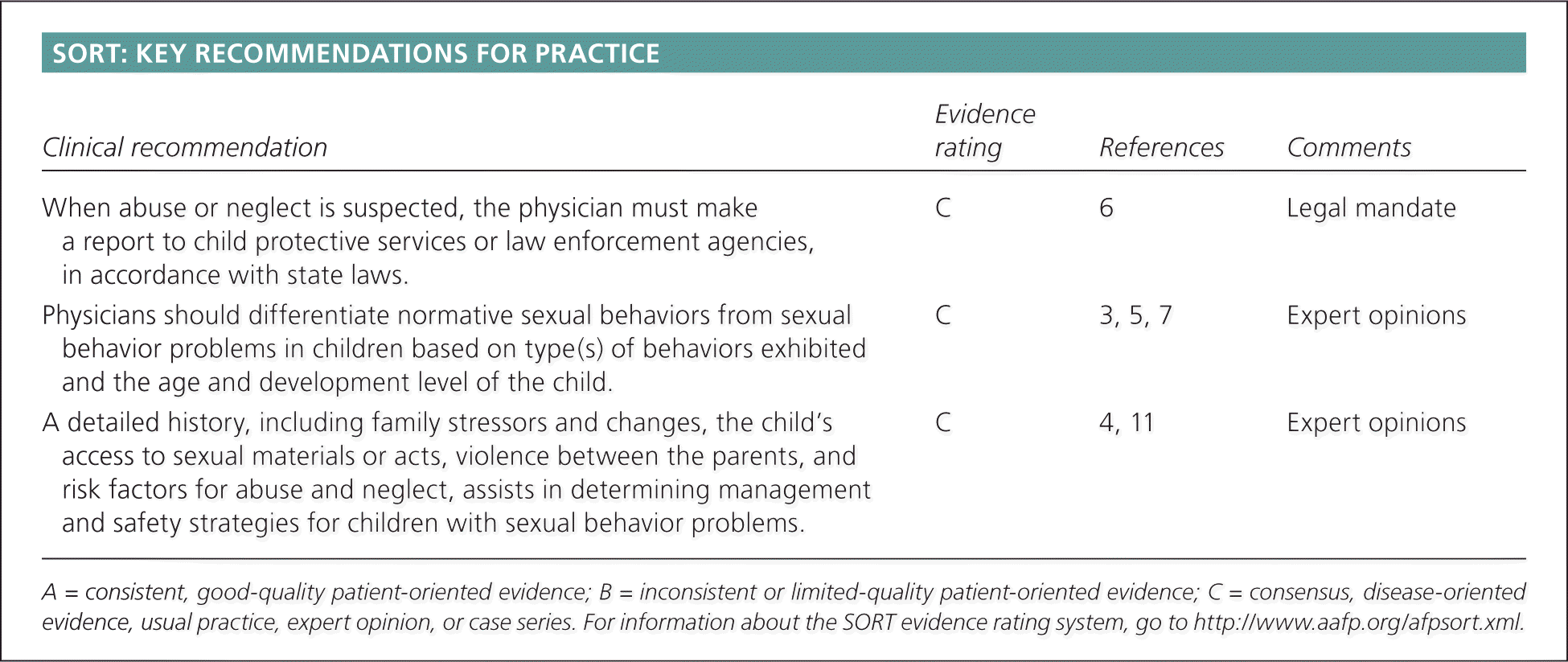
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| When abuse or neglect is suspected, the physician must make a report to child protective services or law enforcement agencies, in accordance with state laws. | C | 6 | Legal mandate |
| Physicians should differentiate normative sexual behaviors from sexual behavior problems in children based on type(s) of behaviors exhibited and the age and development level of the child. | C | 3, 5, 7 | Expert opinions |
| A detailed history, including family stressors and changes, the child's access to sexual materials or acts, violence between the parents, and risk factors for abuse and neglect, assists in determining management and safety strategies for children with sexual behavior problems. | C | 4, 11 | Expert opinions |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Sexual behaviors can be prompted or modified by several factors: normal development, parent reaction to the behavior, changes in family stressors, and access to sexual material. For example, recent technology, such as the Internet, chat rooms, and texting, has expanded the way children are exposed to sexually explicit information. Contemporary television and music provide more frequent exposure to sexual material; there are an average of eight sexual acts per hour on television, an increase of more than fourfold since 1976.5 However, sexual behavior that is developmentally inappropriate requires an evaluation of additional factors, such as conduct and behavior disorders in the child, and violence, abuse, and neglect in the home. Physicians can be valuable resources for parents by providing anticipatory guidance about common sexual behaviors in children, and by differentiating age-appropriate normative sexual behaviors from sexual behavior problems. Management strategies should focus on appropriate parental response to the behaviors, effective distraction from the behaviors in social settings, reviewing indications for further assessment, referrals for counseling if the behavior persists, and reporting to child protective services or law enforcement agencies (in accordance with state laws) when abuse is suspected.6
Several terms have been used to describe sexual behaviors in children. The terms “sexual play” and “sexualized behaviors” generally refer to developmentally appropriate behaviors that are often observed in children with no known risk factors for abuse; these are also referred to as normative sexual behaviors. In contrast, sexual behavior problems, also referred to as sexual acting out, and sexually abusive behavior generally refer to sexual behavior that is developmentally inappropriate, coercive, or potentially harmful emotionally or physically.7 Children who have been sexually abused who develop sexual behavior problems are sometimes referred to as sexually reactive youth.
Normative Sexual Behaviors
The type and frequency of normative sexual behaviors vary with the age of the child.8 Sexual behaviors in infants are rare, with the exception of hand to genital contact. Beyond infancy, sexual behaviors increase as toddlers become more aware of their body parts, including their genitals, physiologic sensations deriving from their genitals, and gender differences. In general, sexual behaviors in children two to five years of age are of a greater variety and are more common compared with the behaviors in children older than five years.9 Once the child becomes aware of social rules regarding sexual behaviors in public, those behaviors become more covert. Sexual behaviors may not necessarily diminish beyond five years of age, but rather the behaviors are not observed by parents as often because children spend less time at home and more time at school, require less supervision, and learn the social norms for concealing sexual behaviors.10 Also, as children age, these behaviors transition to more socially acceptable alternatives such as increasing interest in sexual topics, including the opposite sex. These other behaviors mirror normal psychosocial development and the emerging importance of peer relationships.
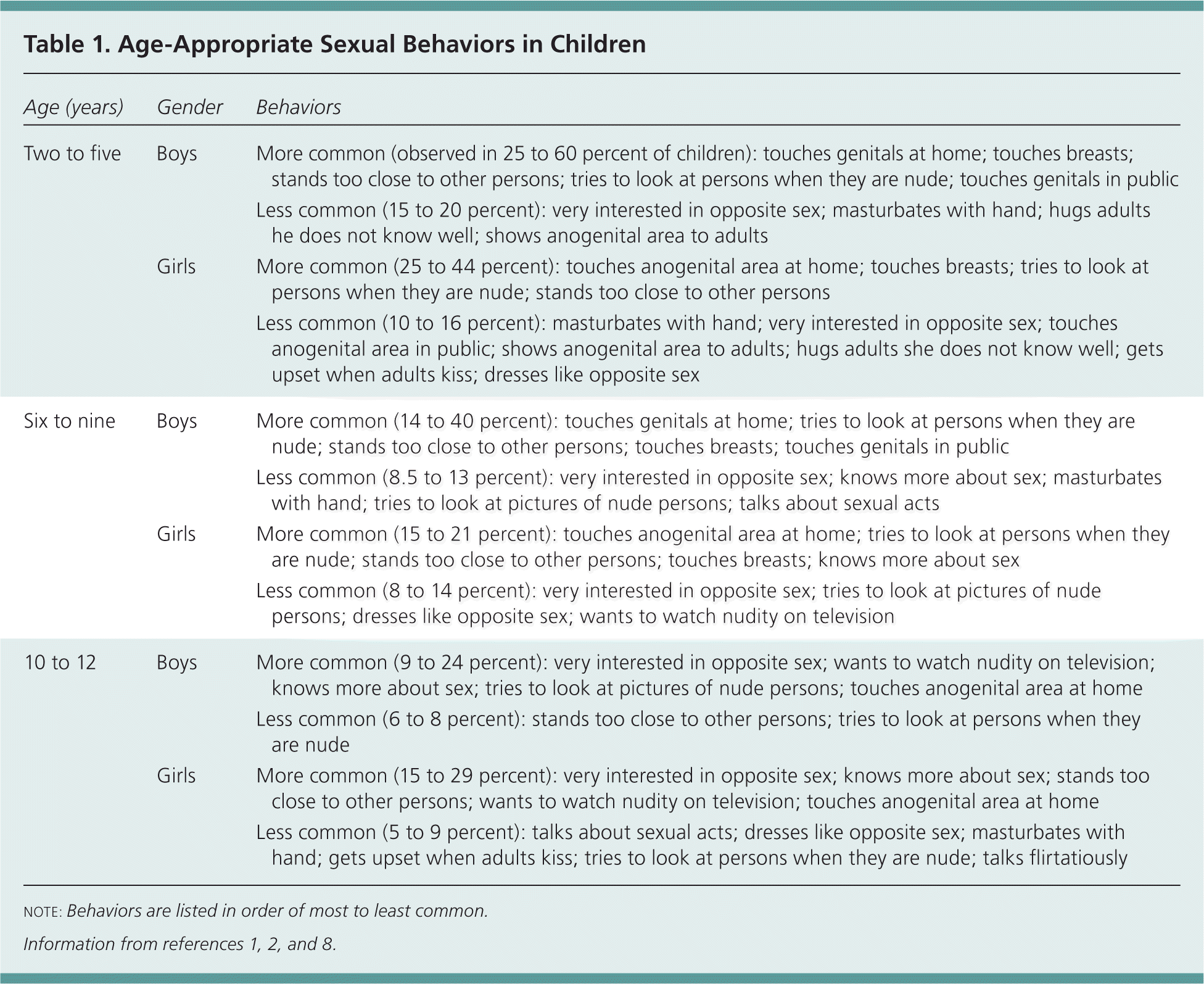
Sexual behavior can be solitary or involve other persons, and may or may not involve sexual contact (Table 1).1,2,8 Children do not necessarily engage in sexual behaviors for sexual gratification; curiosity, imitation of observed sexual behaviors, attention-seeking, and self-soothing are other reasons children may behave sexually.7,11 In general, sexual behaviors that are solitary (e.g., touching one's own genitals) or that do not involve contact (e.g., trying to view another person's genitals or breasts) are common and frequently observed.8 Common, age-appropriate sexual behavior can become a sexual behavior problem if it is disruptive or coercive. For example, a three-year-old boy who touches his genitals several hours a day and cannot focus on other tasks is displaying a normative behavior with abnormal persistence and frequency. In addition, the behaviors that are the least common among the list of normative sexual behaviors may require more extensive assessment to make sure there is no underlying sexual behavior problem.
Table 1. Age-Appropriate Sexual Behaviors in Children
| Age (years) | Gender | Behaviors |
|---|---|---|
| Two to five | Boys | More common (observed in 25 to 60 percent of children): touches genitals at home; touches breasts; stands too close to other persons; tries to look at persons when they are nude; touches genitals in public |
| Less common (15 to 20 percent): very interested in opposite sex; masturbates with hand; hugs adults he does not know well; shows anogenital area to adults | ||
| Girls | More common (25 to 44 percent): touches anogenital area at home; touches breasts; tries to look at persons when they are nude; stands too close to other persons | |
| Less common (10 to 16 percent): masturbates with hand; very interested in opposite sex; touches anogenital area in public; shows anogenital area to adults; hugs adults she does not know well; gets upset when adults kiss; dresses like opposite sex | ||
| Six to nine | Boys | More common (14 to 40 percent): touches genitals at home; tries to look at persons when they are nude; stands too close to other persons; touches breasts; touches genitals in public |
| Less common (8.5 to 13 percent): very interested in opposite sex; knows more about sex; masturbates with hand; tries to look at pictures of nude persons; talks about sexual acts | ||
| Girls | More common (15 to 21 percent): touches anogenital area at home; tries to look at persons when they are nude; stands too close to other persons; touches breasts; knows more about sex | |
| Less common (8 to 14 percent): very interested in opposite sex; tries to look at pictures of nude persons; dresses like opposite sex; wants to watch nudity on television | ||
| 10 to 12 | Boys | More common (9 to 24 percent): very interested in opposite sex; wants to watch nudity on television; knows more about sex; tries to look at pictures of nude persons; touches anogenital area at home |
| Less common (6 to 8 percent): stands too close to other persons; tries to look at persons when they are nude | ||
| Girls | More common (15 to 29 percent): very interested in opposite sex; knows more about sex; stands too close to other persons; wants to watch nudity on television; touches anogenital area at home | |
| Less common (5 to 9 percent): talks about sexual acts; dresses like opposite sex; masturbates with hand; gets upset when adults kiss; tries to look at persons when they are nude; talks flirtatiously |
note: Behaviors are listed in order of most to least common.
Sexual behavior should be interpreted with consideration of several factors: the parent's view of sexuality, family stressors, cultural origins, and day care arrangements. Mothers with more years of education are more likely to think sexual behavior in children is normal and to acknowledge these behaviors in their children compared with mothers with fewer years of education, who are less likely to think sexual behavior in children is normal.8 Parents who view all sexual behaviors as unacceptable may indicate that the behavior is disruptive and abnormal when it may be within developmentally normal limits. Parent overreaction to sexual behaviors may also escalate these behaviors if the child is intrigued or reinforced by the parent's distress. In such situations, the parent's discomfort with issues of sexuality may need to be addressed, particularly if the parent's reaction produces more aberrant behavior in the child.
Children in environments characterized by nudity or less privacy in dressing, bathing, or sexual activity among adults are more likely to openly engage in sexual behaviors.9 However, when parents knowingly and persistently permit their child to have access to pornographic or harmful sexual material, a referral to child protective services for supervision is needed. In children with sexual behavior problems, failure of a parent to modify the child's access to harmful sexual material in accordance with medical or mental health advice also necessitates a referral to child protective services.
Family stressors, such as separation or divorce, may result in an increase in the number and frequency of sexual behaviors in the children. It can be challenging to discern whether sexual behaviors have escalated because of stress or whether one parent's perception and interpretation of the behavior has changed because he or she suspects the other parent has abused or neglected the child.
Cultural differences in parental observations of sexual behaviors in children are also reported. In three studies of Spanish, Dutch, and Flemish parents who were asked whether they had ever seen their children engaged in sexual play or games, rates varied from 53 to 78 percent in children up to 11 years of age.12–14 In all cultures, younger children were more likely than older children to display sexual behaviors, and sexual behaviors that were rare in American children were also rare in other cultures studied.14–16
The number and frequency of normative sexual behaviors are increased in children in day care with other children compared with children not in day care.8 This trend may be caused by changes in observation patterns, or may represent an increase in opportunities for children to interact with each other in sexual and nonsexual ways.
Sexual Behavior Problems
In contrast to normative sexual behaviors, sexual behavior problems typically involve other persons (but still may include solitary behaviors) and sexual contact. Developmentally inappropriate behavior can be defined as behavior that occurs at a greater frequency or at a much earlier age than would be developmentally or culturally expected, becomes a preoccupation for the child, or recurs after adult intervention or corrective efforts.17 For example, a child touching an adult's genitals or breasts would be age-inappropriate for an 11-year-old, but may be age-appropriate for a four-year-old. Similarly, an 11-year-old child with an intellectual disability who touches an adult's genitals may be exhibiting normal behavior if his or her developmental age is four years.18 When there is a disparity in age or development between children engaged in sexual behaviors, it is common for the older child to “take charge” of the activity, directing the younger child in what to do and threatening him or her to comply and “keep the secret.”10,19 Such behaviors warrant additional evaluation and referral to child protective services if abuse or neglect is suspected. Table 2 lists examples of sexual behavior problems.7,10,20,21
Table 2. Examples of Sexual Behavior Problems in Children

| Behavior type | Examples |
|---|---|
| Solitary | Behaviors that cause emotional distress, anxiety, or physical pain |
| Repeated penetration of vagina or anus with an object or digit | |
| Behaviors that are persistent, and child becomes angry if distracted | |
| Behaviors associated with conduct disorders or aggression | |
| A variety of sexual behaviors displayed frequently or on a daily basis | |
| Involving other persons | Sexual behaviors involving children four or more years apart in age |
| One child coercing another into participating | |
| Explicit imitation of sexual intercourse | |
| Oral-genital contact | |
| Asking an adult to perform a specific sexual act |
Sexual behavior problems have been associated with other emotional and behavior disorders in childhood. In a clinical sample of children six to 12 years of age with sexual behavior problems, the most common comorbid diagnoses were conduct disorder (76 percent), followed by attention-deficit/hyperactivity disorder (40 percent) and oppositional defiant disorder (27 percent).21 These externalizing behavior problems have been strongly associated with sexual behavior problems in childhood,9 suggesting that in some instances, sexual behavior problems are better understood and treated by addressing the etiology of externalizing behaviors.22
Family stress and dysfunction, including violence, abuse, and neglect, can cause or exacerbate externalizing behaviors and sexual behavior problems in children. The number and frequency of sexual behaviors in children increase with the number of family stresses, including violence between parents, incarceration, deaths of family members, and illnesses requiring hospitalization.9,23 In a study of 201 children with sexual behavior problems, 48 percent were sexually abused, 32 percent were physically abused, 35 percent were emotionally abused, and 16 percent were neglected.24 One meta-analysis found that 28 percent of children who were sexually abused developed sexual behavior problems, with the highest prevalence in the youngest age groups.25 Sexual abuse involving a father figure perpetrator and penetrative acts is more likely to result in sexually aggressive behavior in the child.26 Externalizing and sexual behavior problems in children are common reasons why foster care placements for children who are abused or neglected fail or are difficult to maintain.27
Clinical Assessment and Management
Incorporating a discussion about sexual behaviors during health maintenance visits can provide considerable benefits. The physician should provide anticipatory guidance about age-appropriate sexual behaviors, gauging the parent's thoughts and feelings about such topics. When parents learn that sexual behaviors are not necessarily indicative of abuse or a behavior disorder, their reactions to such behaviors are more likely to be appropriate. By discussing sexual behaviors, as well as Internet safety and prevention of access to sexual material, the physician provides an opportunity for parents to talk about such issues, especially those who are embarrassed or nervous about sexual topics. Parents should be encouraged to not punish or admonish the child for normative sexual behaviors, and should use gentle distraction, such as asking the child to hold hands with them, to redirect the behavior when in public settings.
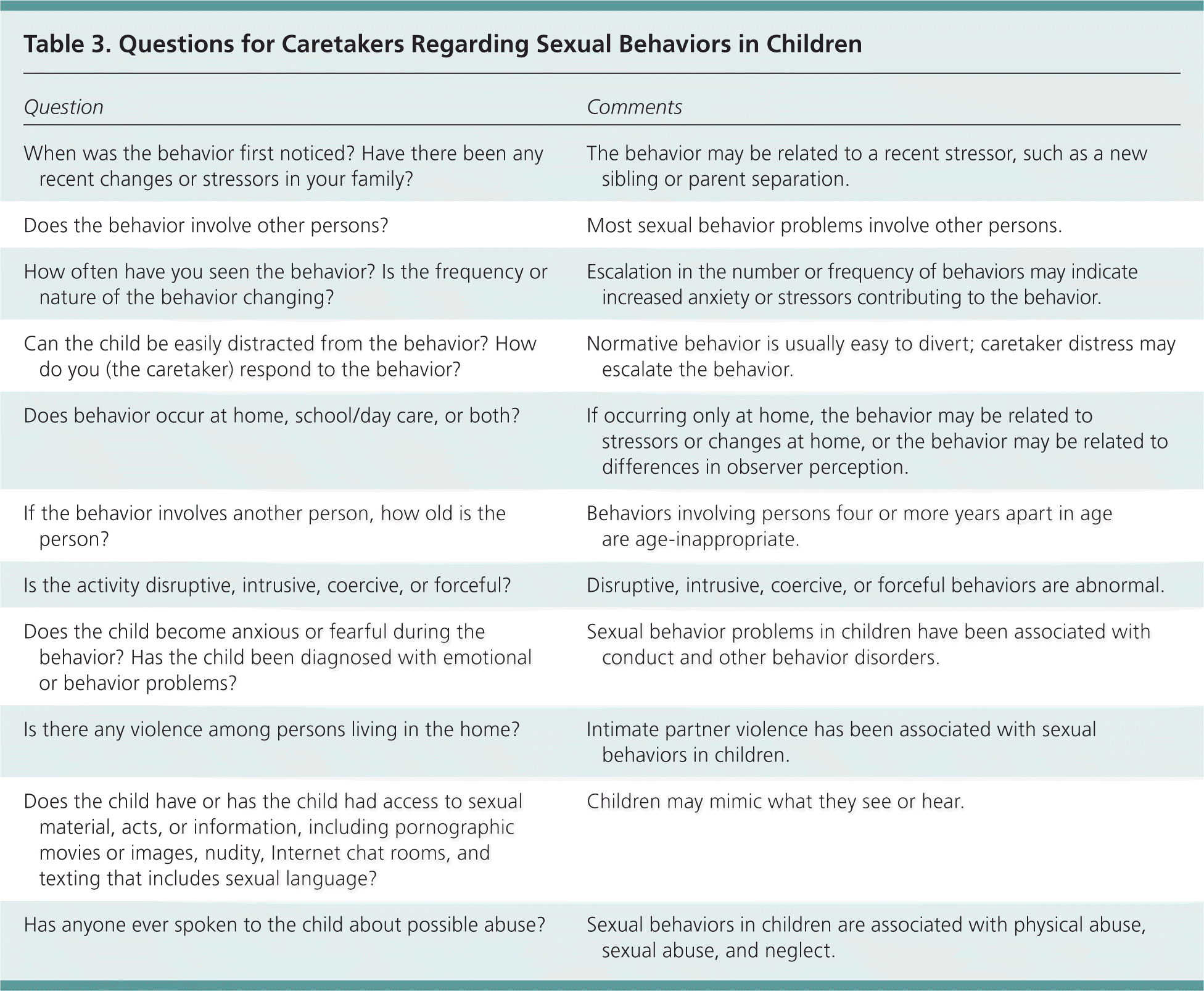
A detailed history can assist in differentiating between normative age-appropriate sexual behavior and sexual behavior problems in children. The parent should be asked to describe the types and frequency of the behaviors; emotional demeanor of the child during the behavior; ages of children involved in the behavior; and whether any coercion or force is used (Table 3). It is also important to evaluate whether this is a new behavior or a change in observer interpretation of the behavior (e.g., new caretakers may notice behaviors that are already present, parents may perceive behavior differently if they are concerned about abuse). If the sexual behaviors described are less commonly seen or are disruptive, then an assessment of situational factors (e.g., changes in day care arrangements, recent serious illnesses in family members, a new infant, family nudity, accessibility of sexual materials) is warranted.
Table 3. Questions for Caretakers Regarding Sexual Behaviors in Children
| Question | Comments |
|---|---|
| When was the behavior first noticed? Have there been any recent changes or stressors in your family? | The behavior may be related to a recent stressor, such as a new sibling or parent separation. |
| Does the behavior involve other persons? | Most sexual behavior problems involve other persons. |
| How often have you seen the behavior? Is the frequency or nature of the behavior changing? | Escalation in the number or frequency of behaviors may indicate increased anxiety or stressors contributing to the behavior. |
| Can the child be easily distracted from the behavior? How do you (the caretaker) respond to the behavior? | Normative behavior is usually easy to divert; caretaker distress may escalate the behavior. |
| Does behavior occur at home, school/day care, or both? | If occurring only at home, the behavior may be related to stressors or changes at home, or the behavior may be related to differences in observer perception. |
| If the behavior involves another person, how old is the person? | Behaviors involving persons four or more years apart in age are age-inappropriate. |
| Is the activity disruptive, intrusive, coercive, or forceful? | Disruptive, intrusive, coercive, or forceful behaviors are abnormal. |
| Does the child become anxious or fearful during the behavior? Has the child been diagnosed with emotional or behavior problems? | Sexual behavior problems in children have been associated with conduct and other behavior disorders. |
| Is there any violence among persons living in the home? | Intimate partner violence has been associated with sexual behaviors in children. |
| Does the child have or has the child had access to sexual material, acts, or information, including pornographic movies or images, nudity, Internet chat rooms, and texting that includes sexual language? | Children may mimic what they see or hear. |
| Has anyone ever spoken to the child about possible abuse? | Sexual behaviors in children are associated with physical abuse, sexual abuse, and neglect. |
Sexual behavior that is developmentally inappropriate or coercive, or that potentially causes emotional or physical pain, requires further assessment for exposure to family violence, sexual abuse, physical abuse, and neglect. If parents are aware their child is viewing harmful pornographic material in their home and do not take steps to limit such access, then a report to child protective services for supervision should be made. When abuse is not suspected, but the sexual behavior requires further assessment or management, a referral to a mental health professional may be needed.

