Frontotemporal dementia (FTD) is one of the most common forms of dementia in persons younger than 65 years. Variants include behavioral variant FTD, semantic dementia, and progressive nonfluent aphasia. Behavioral and language manifestations are core features of FTD, and patients have relatively preserved memory, which differs from Alzheimer disease. Common behavioral features include loss of insight, social inappropriateness, and emotional blunting. Common language features are loss of comprehension and object knowledge (semantic dementia), and nonfluent and hesitant speech (progressive nonfluent aphasia). Neuroimaging (magnetic resonance imaging) usually demonstrates focal atrophy in addition to excluding other etiologies. A careful history and physical examination, and judicious use of magnetic resonance imaging, can help distinguish FTD from other common forms of dementia, including Alzheimer disease, dementia with Lewy bodies, and vascular dementia. Although no cure for FTD exists, symptom management with selective serotonin reuptake inhibitors, antipsychotics, and galantamine has been shown to be beneficial. Primary care physicians have a critical role in identifying patients with FTD and assembling an interdisciplinary team to care for patients with FTD, their families, and caregivers.
Frontotemporal dementia (FTD) is a neurodegenerative disease of unknown etiology, with atrophy and neuronal loss in the frontal and temporal lobes of the brain resulting in a gradual and progressive decline in behavior or language. It was formerly known as Pick disease and was considered rare. Although epidemiologic studies are limited, approximately 20 to 50 percent of persons younger than 65 years with dementia have FTD, a prevalence similar to that of Alzheimer disease in persons 45 to 64 years of age (15 per 100,000).1–3 FTD is underdiagnosed, and primary care physicians have an important role in recognizing this disease. Recent advances in research, neuroimaging, and genetic studies have improved, yet complicated, the field of FTD and related diseases because of a proliferation of terminology, overlapping clinical syndromes, and pathologic classifications. For the purpose of this review, FTD will encompass the distinctly recognizable clinical variants, including behavioral variant FTD, semantic dementia, and progressive nonfluent aphasia. The three FTD syndrome variants are all characterized by the presence of behavioral and personality changes and/or aphasia with overlapping features.4,5 However, each FTD variant is identified by a predominant feature.
Initial symptoms related to FTD are commonly misdiagnosed as primary psychiatric disorders.6–9 A prolonged lag time exists between the onset of presenting symptoms and a correct diagnosis, resulting in extensive testing, cost, and stress for patients and family members. Primary care physicians are well positioned to suspect and diagnose FTD, and to provide the appropriate assistance and resources. In addition, primary care physicians are integral in coordinating an appropriate interdisciplinary team to manage FTD.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Selective serotonin reuptake inhibitors may be beneficial for behavioral symptoms in patients with frontotemporal dementia. | B | 26, 27 |
| Galantamine (Razadyne) may be beneficial in some patients with progressive nonfluent aphasia. | B | 30 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limitedquality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Pathophysiology
Common pathologic findings in FTD are atrophy and neuronal loss affecting the frontal and temporal lobes of the brain.10 There is histologic heterogeneity in patients with FTD, but about 55 percent of patients have FTD with ubiquitin-positive inclusions and 45 percent have FTD with tau-positive inclusions. FTD with Pick bodies is still called Pick disease.10 Recent research has identified the presence of TAR DNA–binding protein (TDP-43), which may be the primary disease protein underlying the ubiquitin-positive cases.11–13 Furthermore, emerging research is allowing for a better understanding of the association between pathologies and clinical syndromes. It appears that both tau and ubiquitin (TDP-43) pathologies are seen in behavioral variant FTD, whereas tau is more often present in progressive nonfluent aphasia, and ubiquitin (TDP-43) is more often present in semantic dementia.10–13 Two genes on chromosome 17, and genes on chromosomes 3 and 9, have been linked to FTD.14 Mutations in the tau gene have been linked to FTD with tau-positive inclusions, and later mutations in the progranulin gene have been linked to FTD with ubiquitin-positive inclusions.
Diagnosis
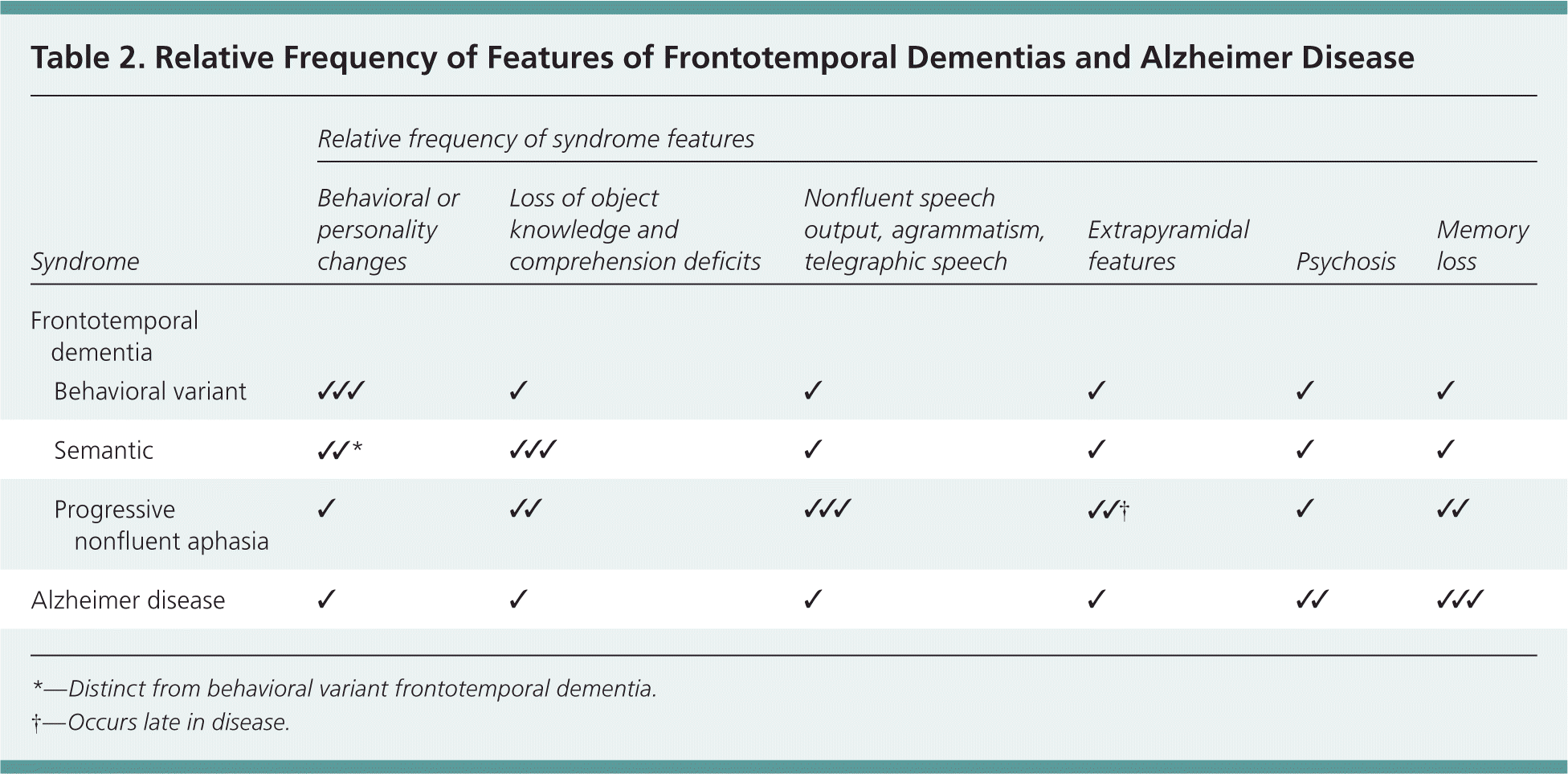
The diagnosis of FTD requires a thorough history, especially family history of dementia, and physical examination, with a focus on the timing and rate of progression of symptoms, and behavioral and personality changes over the previous months or years. Clinical consensus criteria for diagnosing FTD, also referred to as the Neary criteria, were published in 1998. The criteria outline core and supportive features of behavioral variant FTD, semantic dementia, and progressive nonfluent aphasia (Table 1).15 For all FTD variants, onset is insidious and has a gradual progression, and memory is relatively preserved, which differs from Alzheimer disease. Table 2 provides relative frequency of common signs and symptoms of FTD and Alzheimer disease. FTD may be difficult to distinguish from other types of dementia and affective disorders, and primary care physicians may consider, if necessary, a referral for neuropsychological or neurologic evaluation. Neuroimaging (magnetic resonance imaging) is helpful, even essential, in the diagnosis of FTD, and usually demonstrates focal atrophy in addition to excluding other etiologies.
Table 1. Diagnostic Behavioral and Language Features of Frontotemporal Dementia Variants
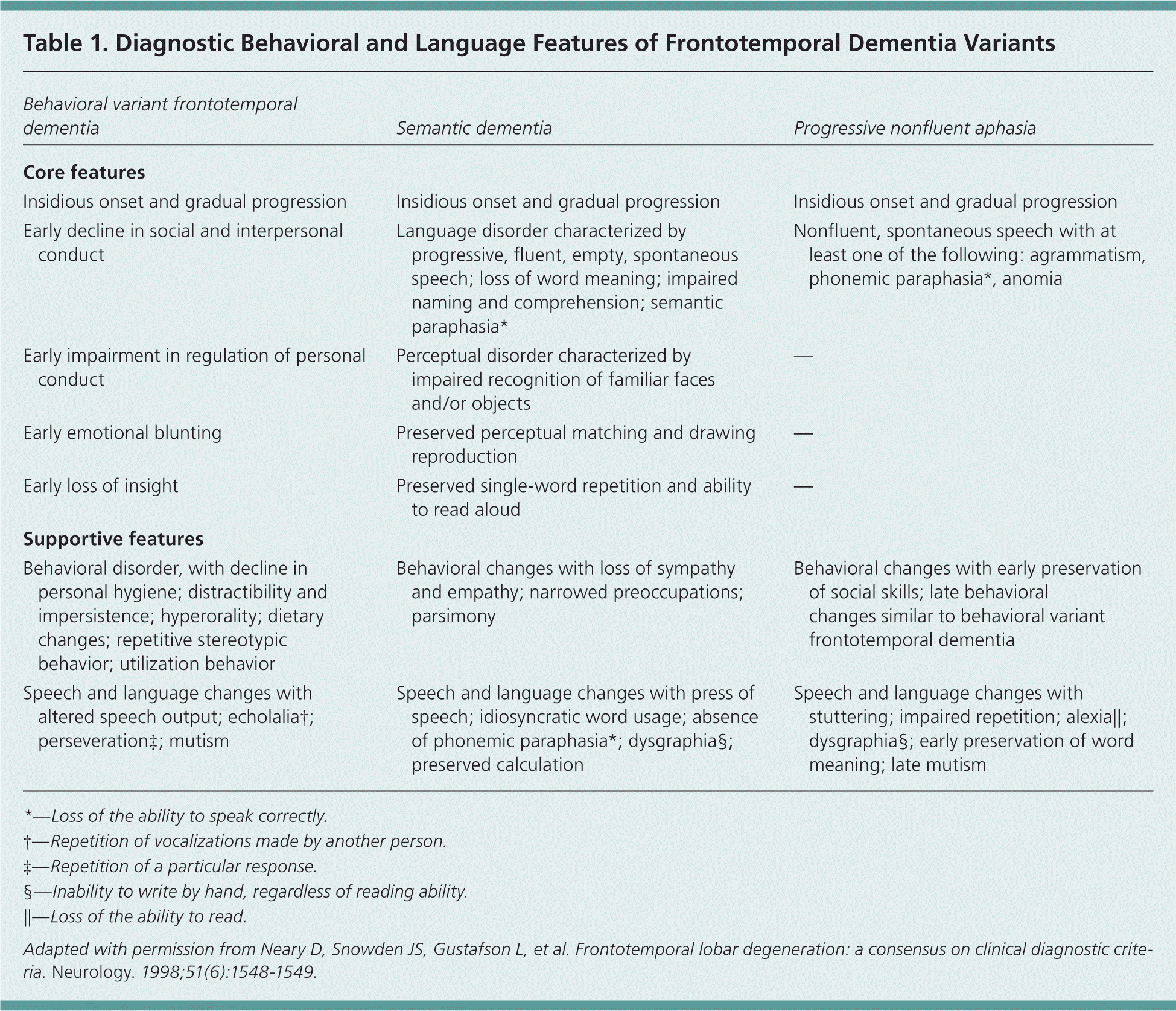
Table 2. Relative Frequency of Features of Frontotemporal Dementias and Alzheimer Disease
| Syndrome | Relative frequency of syndrome features | ||||||
|---|---|---|---|---|---|---|---|
| Behavioral or personality changes | Loss of object knowledge and comprehension deficits | Nonfluent speech output, agrammatism, telegraphic speech | Extrapyramidal features | Psychosis | Memory loss | ||
| Frontotemporal dementia | |||||||
| Behavioral variant | ✓✓✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |
| Semantic | ✓✓* | ✓ ✓ ✓ | ✓ | ✓ | ✓ | ✓ | |
| Progressive nonfluent aphasia | ✓ | ✓ ✓ | ✓ ✓ ✓ | ✓ ✓† | ✓ | ✓ ✓ | |
| Alzheimer disease | ✓ | ✓ | ✓ | ✓ | ✓ ✓ | ✓ ✓ ✓ | |
*—Distinct from behavioral variant frontotemporal dementia.
†—Occurs late in disease.
The usefulness of standard dementia screening tests, such as the Mini-Mental State Examination or Addenbrooke's Cognitive Examination, is limited to confirming the low language performance versus the relatively preserved memory and visuospatial ability in patients with FTD compared with patients who have Alzheimer disease; patients with Alzheimer disease predominantly have memory loss.16 The Frontal Behavioral Inventory incorporates supporting items from the Neary criteria, and is useful in the differential diagnosis.17
BEHAVIORAL VARIANT FTD
Personality changes and inappropriate social behaviors are central features of behavioral variant FTD.15,18 Specific core features include decline in interpersonal and social conduct, emotional blunting, and loss of insight. Recently, the American Neuropsychiatric Association published a review of neuropsychiatric features of FTD, including supporting evidence.18 The most common initial symptoms associated with behavioral variant FTD are apathy, lack of initiation, diminished interest, and inactivity. Frank apathy is commonly misdiagnosed as depression.4,6 Disinhibition/impulsivity, which is the lack of restraint in motor, emotional, cognitive, and social circumstances, is also a common feature of FTD.
Patients' loss of insight into their disease and the consequences of their behavior is less common in other types of dementia initially and, therefore, is an early clue to FTD.6 Other common behavioral features are socially inappropriate remarks and physical contact, including sexual comments or advances; childish and selfish behavior; roaming; hoarding; and loss of executive functions.6,15,19–21 Other symptoms linked to behavioral variant FTD include dietary changes, repetitive stereotypic behaviors, poor hygiene, hyperorality, and utilization behavior, which is the inability of patients to resist the impulse of using objects that are within their visual field and within reach. Shoplifting may occur.15,22 Psychosis is an uncommon feature of behavioral variant FTD, and occurs at higher rates in patients with Alzheimer disease.23
SEMANTIC DEMENTIA
Patients with semantic dementia have effortless speech that lacks meaning and information.15 These patients have the tendency to use generic or broad terms rather than words with specific meaning. Usually, loss of word meaning needs to be elicited in serial interviews, because speech effort is fluent. Patients often ask what something is when they hear a word in conversation, or ask the names of objects. Patients with semantic dementia tend to replace correct terms with semantically related words, such as “animal” for “cat.”15 This is referred to as semantic paraphasia. Also, these patients tend not to recognize familiar faces, such as well-known celebrities. The loss of object identity and its function (i.e., associative agnosia) also occurs in patients with semantic dementia. Behavioral manifestations similar to behavioral variant FTD often occur.
PROGRESSIVE NONFLUENT APHASIA
Progressive nonfluent aphasia is characterized by nonfluent, agrammatic, and, at times, stuttering and hesitant speech that requires considerable effort from the patient.15 These patients often present with word-finding difficulties and later have problems naming objects (i.e., anomia). The incorrect use or frank omission of a variety of grammatical terms (i.e., agrammatism) is a core feature of progressive nonfluent aphasia. This results in limited speech output and impaired comprehension. Patients with progressive nonfluent aphasia also often demonstrate phonemic paraphasia, such as saying “bog” instead of “dog.”15 Other supporting features may include nonfluent reading abilities and impaired ability to repeat words or short phrases.15 Early-stage progressive nonfluent aphasia usually has preserved social and behavioral skills. However, these features may deteriorate as the disease progresses. Some patients with progressive nonfluent aphasia also develop corticobasal degeneration or behavioral variant FTD.15
Distinguishing Features of Other Common Types of Dementia
More than 90 percent of patients with dementia have Alzheimer disease, dementia with Lewy bodies, vascular dementia, or FTD.24 Parkinson disease with dementia may be part of the spectrum of disease progression associated with dementia with Lewy bodies.25 Primary signs and symptoms associated with Alzheimer disease are memory and visuospatial loss. Patients who have dementia with Lewy bodies also have memory loss, fluctuating cognition, and visual hallucinations, and develop spontaneous parkinsonism motor features. Those with vascular dementia usually have a history of cerebrovascular events and white matter changes on neuroimaging. They may present with focal neurologic deficits, early gait disturbances, changes in personality and mood, and a history of frequent falls or unsteadiness.
Treatment
There is no specific cure for FTD; treatment is focused on symptom management and support for patients, families, and caregivers. Selective serotonin reuptake inhibitors are commonly used and may be beneficial for behavioral symptoms, including disinhibition, depressive symptoms, and repetitive behaviors.26,27 However, careful observation is needed to ensure that adverse effects do not occur.28
Patients with aggressive behavior or outbursts may respond to small doses of antipsychotics; however, the benefits and risks associated with potential adverse effects must be considered. The role of Alzheimer disease medications, such as acetylcholinesterase inhibitors and N-methyl-d-aspartate receptor antagonists, is unclear and under investigation, because patients with FTD have normal cholinergic function.29 There is evidence that galantamine (Razadyne) may help some patients with progressive nonfluent aphasia.30 Table 3 provides a summary of treatments for FTD based on expert opinion.18 Future treatment targets will likely be the result of the recently identified underlying proteinopathies. Primary care physicians may want to seek guidance from neurologists or other subspecialists, such as psychiatrists, to assist with treatment-refractory FTD or to identify the optimal medication regimen to alleviate symptoms.
Table 3. Treatment Options for Frontotemporal Dementia

| Pharmacologic |
| Acetylcholinesterase inhibitors may be beneficial in patients with progressive nonfluent aphasia. |
| Behavioral symptoms (e.g., disinhibition, depressive symptoms) may respond to selective serotonin reuptake inhibitors. |
| Marked disinhibition/impulsivity or aggressive and disruptive behaviors may respond to small doses of atypical antipsychotics. |
| Nonpharmacologic |
| Address caregiver needs (e.g., support groups), involvement of other family members, and referral for community resources. |
| Address functional issues as they relate to activities of daily living, home environment and safety, transportation and driving, and living situations. |
| Address social stressors, such as financial and legal issues, and the need for conservatorship. |
| Assess the need for psychological counseling for family members and caregivers. |
| Develop behavioral management strategies and interventions for behavioral disturbances (e.g., social misconduct). |
| Ensure coordinated care of services between the primary care physician and subspecialists. |
| Provide education, explain the nature of the disease, and clarify that the neuropsychiatric features are part of the disease, not deliberate behaviors. |
Information from reference 18.
Prognosis
There is limited research on the prognosis of FTD. A retrospective longitudinal study of 177 patients with FTD and 395 patients with Alzheimer disease assessed survival from estimated symptom onset.31 Median survival was 8.7 years (+/– 1.2 years) in patients with FTD compared with 11.8 years (+/– 0.6 years) in patients with Alzheimer disease. Patients similar to those of patients with Alzheimer disease (11.9 years [+/– 0.2 years]).
Future Directions
Current research focuses on molecular biology to better understand the underlying causes of FTD and its variants, treatment strategies, and the role of imaging for diagnostic purposes. Nonetheless, as FTD is better understood and subsequently classified, and as new diagnostic and treatment modalities are discovered, primary care physicians will continue to have an integral role in aiding in the diagnosis of FTD, identifying an appropriate interdisciplinary team based on the needs of each patient, and organizing the necessary resources for patients and families. This can be accomplished during a meeting among the patient, family, physician, and ancillary support staff. In this meeting, the patient's needs are identified, management is planned, and interventions are ordered.
Because of the intense emotional and resource requirements of families and caregivers of patients with FTD, it is important that their needs are also met. Support groups for families and caregivers are important, and their use should not be delayed until the late stages of FTD. The availability of such support services is dependent on the community in which patients and caregivers live. A robust central FTD resource for patients, families, and health care professionals can be found on the Association for Frontotemporal Dementias Web site (http://www.ftd-picks.org). Other useful Web sites include the National Institute on Aging (http://www.nia.nih.gov); National Institute of Neurological Disorders and Stroke (http://www.ninds.nih.gov); Alzheimer's Association (http://www.alz.org); and Family Caregiver Alliance (http://www.caregiver.org).

