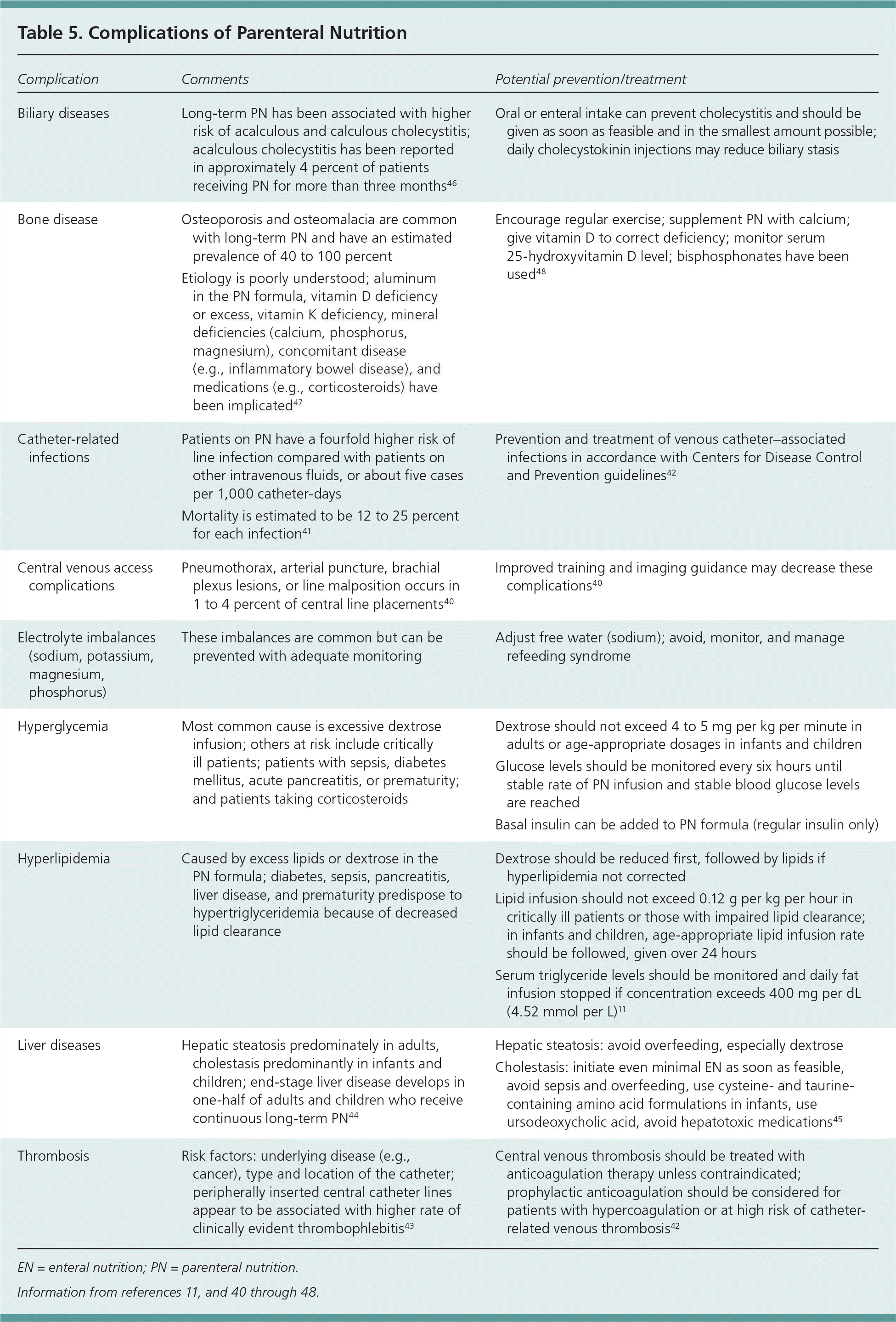
| Biliary diseases | Long-term PN has been associated with higher risk of acalculous and calculous cholecystitis; acalculous cholecystitis has been reported in approximately 4 percent of patients receiving PN for more than three months46 | Oral or enteral intake can prevent cholecystitis and should be given as soon as feasible and in the smallest amount possible; daily cholecystokinin injections may reduce biliary stasis |
| Bone disease | Osteoporosis and osteomalacia are common with long-term PN and have an estimated prevalence of 40 to 100 percent | Encourage regular exercise; supplement PN with calcium; give vitamin D to correct deficiency; monitor serum 25-hydroxyvitamin D level; bisphosphonates have been used48 |
| Etiology is poorly understood; aluminum in the PN formula, vitamin D deficiency or excess, vitamin K deficiency, mineral deficiencies (calcium, phosphorus, magnesium), concomitant disease (e.g., inflammatory bowel disease), and medications (e.g., corticosteroids) have been implicated47 |
| Catheter-related infections | Patients on PN have a fourfold higher risk of line infection compared with patients on other intravenous fluids, or about five cases per 1,000 catheter-days | Prevention and treatment of venous catheter– associated infections in accordance with Centers for Disease Control and Prevention guidelines42 |
| Mortality is estimated to be 12 to 25 percent for each infection41 |
| Central venous access complications | Pneumothorax, arterial puncture, brachial plexus lesions, or line malposition occurs in 1 to 4 percent of central line placements40 | Improved training and imaging guidance may decrease these complications40 |
| Electrolyte imbalances (sodium, potassium, magnesium, phosphorus) | These imbalances are common but can be prevented with adequate monitoring | Adjust free water (sodium); avoid, monitor, and manage refeeding syndrome |
| Hyperglycemia | Most common cause is excessive dextrose infusion; others at risk include critically ill patients; patients with sepsis, diabetes mellitus, acute pancreatitis, or prematurity; and patients taking corticosteroids | Dextrose should not exceed 4 to 5 mg per kg per minute in adults or age-appropriate dosages in infants and children |
| Glucose levels should be monitored every six hours until stable rate of PN infusion and stable blood glucose levels are reached |
| Basal insulin can be added to PN formula (regular insulin only) |
| Hyperlipidemia | Caused by excess lipids or dextrose in the PN formula; diabetes, sepsis, pancreatitis, liver disease, and prematurity predispose to hypertriglyceridemia because of decreased lipid clearance | Dextrose should be reduced first, followed by lipids if hyperlipidemia not corrected |
| Lipid infusion should not exceed 0.12 g per kg per hour in critically ill patients or those with impaired lipid clearance; in infants and children, age-appropriate lipid infusion rate should be followed, given over 24 hours |
| Serum triglyceride levels should be monitored and daily fat infusion stopped if concentration exceeds 400 mg per dL(4.52 mmol per L)11 |
| Liver diseases | Hepatic steatosis predominately in adults, cholestasis predominantly in infants and children; end-stage liver disease develops in one-half of adults and children who receive continuous long-term PN44 | Hepatic steatosis: avoid overfeeding, especially dextrose |
| Cholestasis: initiate even minimal EN as soon as feasible, avoid sepsis and overfeeding, use cysteine- and taurine-containing amino acid formulations in infants, use ursodeoxycholic acid, avoid hepatotoxic medications45 |
| Thrombosis | Risk factors: underlying disease (e.g., cancer), type and location of the catheter; peripherally inserted central catheter lines appear to be associated with higher rate of clinically evident thrombophlebitis43 | Central venous thrombosis should be treated with anticoagulation therapy unless contraindicated; prophylactic anticoagulation should be considered for patients with hypercoagulation or at high risk of catheter-related venous thrombosis42 |