The use of magnetic resonance imaging (MRI) has become routine in the evaluation of musculoskeletal conditions. Originally, MRI was used mainly as a preoperative planning tool for patients thought to have surgical pathology based on history and physical examination. In recent years, however, MRI often has been used solely to establish a diagnosis, in many cases before any conservative treatment has been instituted. This practice raises the following questions: Is MRI overused in patients with musculoskeletal conditions? What are the indications for MRI?
For most patients with neck, back, knee, or shoulder pain, a diagnosis can be made with a history, physical examination, and plain film radiography; surgery is not indicated. Neck and back pain have many causes, but the majority of patients will improve with conservative management.1,2 Shoulder pain is most often associated with conditions that do not require surgery (e.g., muscle strains, tendinopathy).3 Similarly, knee pain, especially without discrete trauma, is often secondary to nonsurgical conditions such as tendinopathy and patellofemoral syndrome.4 The treatment for these common conditions—which usually involves muscle strengthening and stretching, and possibly physical therapy—would not be dependent on MRI results. Most patients will improve within a few weeks or months.
MRI often identifies pathology that may have no relationship to a patient's symptoms. Approximately 30 to 40 percent of asymptomatic young and middleaged patients have changes in the intervertebral disks, such as a protrusion or desiccation, and these structural abnormalities increase with aging.5 A similar percentage of middle-aged patients and an even higher percentage of older patients have asymptomatic meniscus and rotator cuff tears.6–9
MRI may provide information that is confusing to the patient and physician, and does not necessarily identify the source of pain. The patient may be referred to an orthopedist with the expectation of being “fixed” quickly, even though the problem may have been treated successfully without surgery. In these cases, the patient becomes more of a passive bystander, rather than actively participating in a stretching-strengthening program. A surgeon may be willing to perform surgery to satisfy the patient and referring physician, although the procedure may not be curative. The patient may be exposed to unnecessary risks, and the cost of care is increased.
The indications for and timing of MRI will depend on whether the problem is emergent, acute, or chronic. Musculoskeletal emergencies that require an immediate MRI are limited primarily to spinal conditions such as suspected cauda equina syndrome and infection.10 There are certain acute neck, back, shoulder, and knee conditions for which MRI should be considered after four to six weeks of conservative care if the findings could alter treatment. In patients who have neck and back pain with persistent radiculopathy or those who have loss of balance and gait problems indicative of cervical myelopathy, MRI can detect disk herniations or spinal stenosis that may benefit from more aggressive treatment.1,2
MRI of the shoulder is indicated after traumatic inury in young and middle-aged patients who have persistent pain and weakness because they may have a complete rotator cuff tear amenable to early repair.11 MRI of the knee is indicated in younger patients who present with posttraumatic swelling and an inability to fully extend because they may have sustained a repairable buckethandle meniscus tear.12,13 Even in these acute situations when a patient presents with significant pain, MRI is not indicated immediately because the clinical picture may be worse than the actual pathology, and the patient may improve with four to six weeks of conservative care. For most patients, especially those who are older with less traumatic, more chronic problems, MRI is indicated only after a few months if conservative treatment has been ineffective. In these more chronic situations, MRI is useful for confirming the suspected pathology when a referral for surgery is contemplated. There will be a small percentage of patients who do not improve and in whom the diagnosis remains unclear. In these cases, MRI can be used to rule out surgical pathology (see accompanying table).1,2,7,8,10,11,13,14
Table. Suggested Indications for MRI for Common Musculoskeletal Conditions
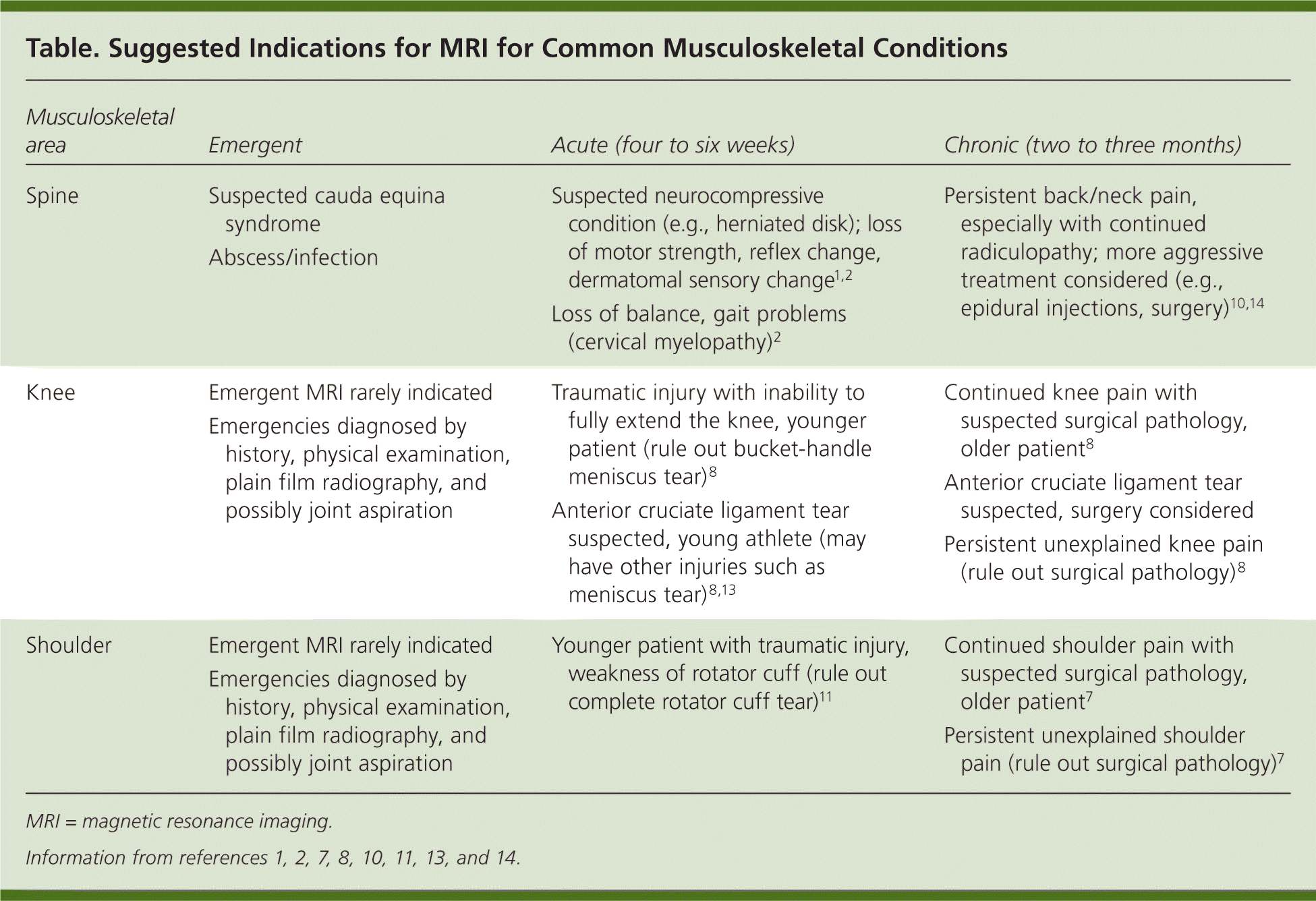
| Musculoskeletal area | Emergent | Acute (four to six weeks) | Chronic (two to three months) |
|---|---|---|---|
| Spine |
| Persistent back/neck pain, especially with continued radiculopathy; more aggressive treatment considered (e.g., epidural injections, surgery)10,14 | |
| Knee |
| Continued knee pain with suspected surgical pathology, older patient8 | |
| Anterior cruciate ligament tear suspected, surgery considered | |||
| Persistent unexplained knee pain (rule out surgical pathology)8 | |||
| Shoulder |
|
| Continued shoulder pain with suspected surgical pathology, older patient7 |
| Persistent unexplained shoulder pain (rule out surgical pathology)7 |
MRI = magnetic resonance imaging.
To optimize patient outcomes, primary care physicians must recognize that most conditions can be diagnosed by history and physical examination, and will respond to conservative treatment. In general, MRI is not indicated for patients in whom the result would not alter the treatment. MRI may identify incidental pathology and result in an unnecessary referral to a subspecialist and possibly even unnecessary surgery. Careful consideration should be given before performing MRI, because the results could lead to more aggressive treatment when conservative management would suffice.

