Appropriate resuscitation must be available for each of the more than 4 million infants born annually in the United States. Ninety percent of infants transition safely, and it is up to the physician to assess risk factors, identify the nearly 10 percent of infants who need resuscitation, and respond appropriately. A team or persons trained in neonatal resuscitation should be promptly available to provide resuscitation. The Neonatal Resuscitation Program, which was initiated in 1987 to identify infants at risk of needing resuscitation and provide high-quality resuscitation, underwent major updates in 2006 and 2010. Among the most important changes are to not intervene with endotracheal suctioning in vigorous infants born through meconium-stained amniotic fluid (although endotracheal suctioning may be appropriate in nonvigorous infants); to provide positive pressure ventilation with one of three devices when necessary; to begin resuscitation of term infants using room air or blended oxygen; and to have a pulse oximeter readily available in the delivery room. The updated guidelines also provide indications for chest compressions and for the use of intravenous epinephrine, which is the preferred route of administration, and recommend not to use sodium bicarbonate or naloxone during resuscitation. Other recommendations include confirming endotracheal tube placement using an exhaled carbon dioxide detector; using less than 100 percent oxygen and adequate thermal support to resuscitate preterm infants; and using therapeutic hypothermia for infants born at 36 weeks' gestation or later with moderate to severe hypoxic-ischemic encephalopathy.
Nearly 10 percent of the more than 4 million infants born in the United States annually need some assistance to begin breathing at birth, with approximately 1 percent needing extensive resuscitation1,2 and about 0.2 to 0.3 percent developing moderate or severe hypoxic-ischemic encephalopathy.3 Mortality in infants with hypoxic-ischemic encephalopathy ranges from 6 to 30 percent, and significant morbidity, such as cerebral palsy and long-term disabilities, occurs in 20 to 30 percent of survivors.4 The Neonatal Resuscitation Program (NRP), which was initiated in 1987 to identify infants at risk of respiratory depression and provide high-quality resuscitation, underwent major updates in 2006 and 2010.1,5–7
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A team or persons trained in neonatal resuscitation should be promptly available at all deliveries to provide complete resuscitation, including endotracheal intubation and administration of medications. | C | 9 |
| If the infant's heart rate is less than 100 beats per minute and/or the infant has apnea or gasping respiration, positive pressure ventilation via face mask should be initiated with 21 percent oxygen (room air) or blended oxygen using a self-inflating bag, flow-inflating bag, or T-piece device while monitoring the inflation pressure. | C | 5, 6 |
| If the infant's heart rate is less than 60 beats per minute after effective positive pressure ventilation, then chest compressions should be initiated with continued positive pressure ventilation (3:1 ratio of compressions to ventilation; 90 compressions and 30 breaths per minute). | C | 5–7 |
| Exhaled carbon dioxide detectors can be used to confirm endotracheal tube placement in an infant. | C | 5, 6 |
| In the resuscitation of an infant, initial oxygen concentration of 21 percent is recommended. | C | 5, 6 |
| If the infant's heart rate is less than 60 beats per minute after adequate positive pressure ventilation and chest compressions, intravenous epinephrine at 0.01 to 0.03 mg per kg (1:10,000 solution) is recommended. | C | 1, 2, 5, 6 |
| Naloxone and sodium bicarbonate are rarely needed and are not recommended during neonatal resuscitation. | C | 1, 2, 5, 6 |
| Therapeutic hypothermia is recommended in infants born at 36 weeks' gestation or later with evolving moderate to severe hypoxic-ischemic encephalopathy. | C | 5–7 |
| Intrapartum suctioning is not recommended in infants born through meconium-stained amniotic fluid. Endotracheal suctioning may be useful in nonvigorous infants with respiratory depression born through meconium-stained amniotic fluid. | C | 1, 2, 5 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Neonatal Resuscitation Team
A 1987 study showed that nearly 78 percent of Canadian hospitals did not have a neonatal resuscitation team, and physicians were called into a significant number of community hospitals (69 percent) for neonatal resuscitation because they were not in-house.8 National guidelines in the United States and Canada recommend that a team or persons trained in neonatal resuscitation be promptly available for every birth.9,10 Actual institutional compliance with this guideline is unknown. In small hospitals, a nonphysician neonatal resuscitation team is one way of providing in-house coverage at all hours. NRP-certified nurses, nurse practitioners, and respiratory therapists have demonstrated the capacity to lead resuscitations.11–13 However, it is recommended that an NRP-certified physician be present in the hospital when a high-risk delivery is anticipated.11–13 One study provides an outline for physicians interested in developing a neonatal resuscitation team.14
Breakdowns in teamwork and communication can lead to perinatal death and injury.15 Team training in simulated resuscitations improves performance and has the potential to improve outcomes.16,17 Ultimately, being able to perform bag and mask ventilation and work in coordination with a team are important for effective neonatal resuscitation.
Planning and Preparation
Important aspects of neonatal resuscitation are the hospital policy and planning that ensure necessary equipment and personnel are present before delivery.1 Anticipation and preparation are essential elements for successful resuscitation,18 and this requires timely and accurate communication between the obstetric team and the neonatal resuscitation team. Physicians who provide obstetric care should be aware of maternal-fetal risk factors1 and should assess the risk of respiratory depression with each delivery.19 The obstetric team should inform the neonatal resuscitation team of the risk status for each delivery and continue to focus on obstetric care. Once the neonatal resuscitation team is summoned to the delivery room, it is important to obtain a pertinent history; assign roles to each team member; check that all equipment is available and functional,1 including a pulse oximeter and an air/oxygen blender6; optimize room temperature for the infant; and turn on the warmer, light, oxygen, and suction.
Outline of Resuscitation
Resuscitation of an infant with respiratory depression (term and preterm) in the delivery room (Figure 1) focuses on airway, breathing, circulation, and medications. 5 As soon as the infant is delivered, a timer or clock is started. Once the infant is brought to the warmer, the head is kept in the “sniffing” position to open the airway. The airway is cleared (if necessary), and the infant is dried. Breathing is stimulated by gently rubbing the infant's back. The wet cloth beneath the infant is changed.5 Respiratory effort is assessed to see if the infant has apnea or gasping respiration, and the heart rate is counted by feeling the umbilical cord pulsations or by auscultating the heart for six seconds (e.g., heart rate of six in six seconds is 60 beats per minute [bpm]). The heart rate should be verbalized for the team.
Figure 1.
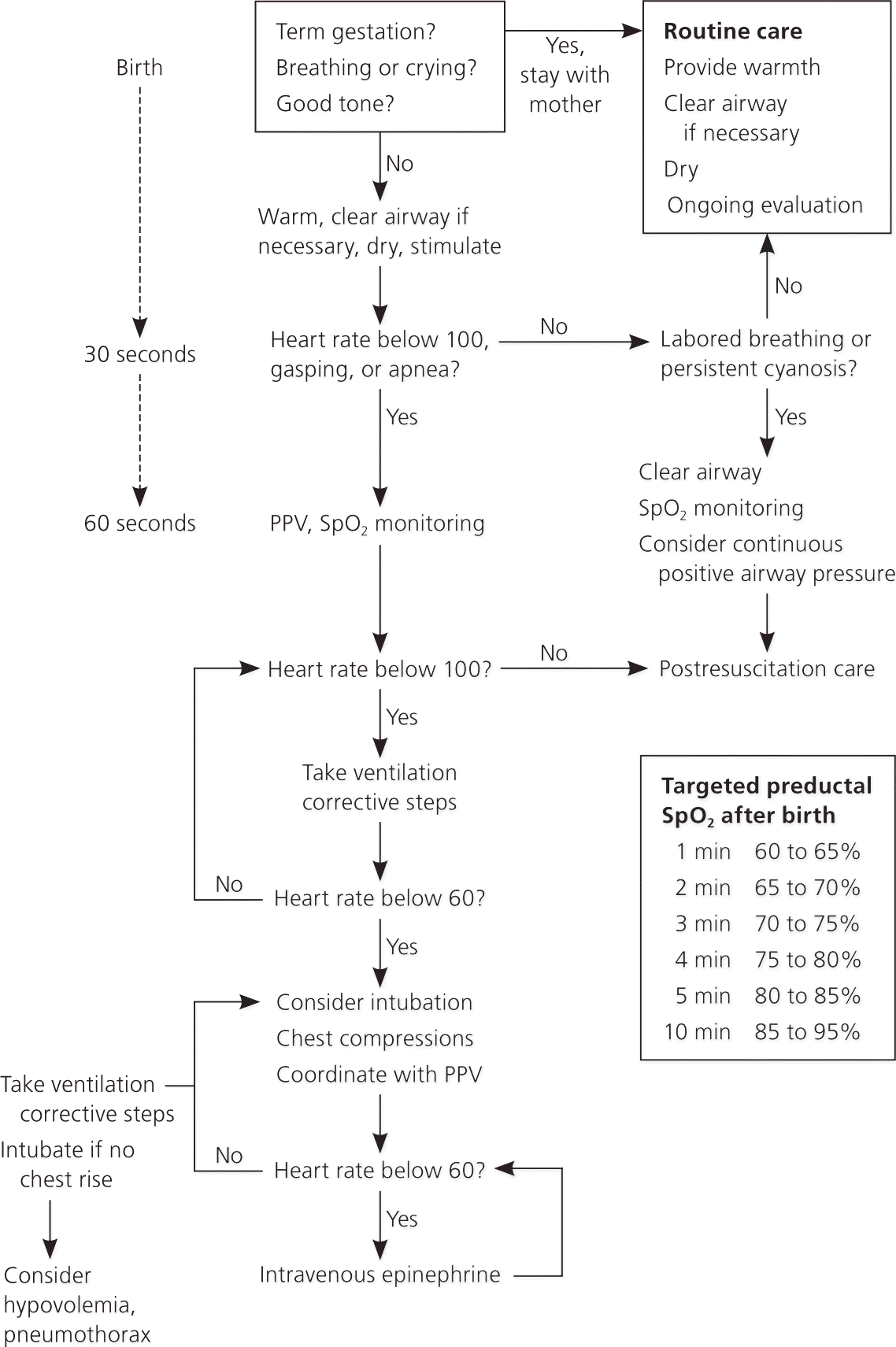
Algorithm outlining neonatal resuscitation. (PPV = positive pressure ventilation; SpO2 = oxygen saturation as measured by pulse oximetry.)
Reprinted with permission from Kattwinkel J, Perlman JM, Aziz K, et al. Part 15: Neonatal resuscitation: 2010 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2010;122(18 suppl 3):S910.
If the heart rate is less than 100 bpm and/or the infant has apnea or gasping respiration, positive pressure ventilation (PPV) via face mask is initiated with 21 percent oxygen (room air) or blended oxygen, and the pulse oximeter probe is applied to the right hand/wrist to monitor heart rate and oxygen saturation.5,6 The heart rate is reassessed after 30 seconds, and if it is less than 100 bpm, PPV is optimized to ensure adequate ventilation, and heart rate is checked again in 30 seconds.5–7 If the heart rate is less than 60 bpm after 30 seconds of effective PPV, chest compressions are started with continued PPV with 100 percent oxygen (3:1 ratio of compressions to ventilation; 90 compressions and 30 breaths per minute) for 45 to 60 seconds.5–7 If the heart rate continues to be less than 60 bpm despite adequate ventilation and chest compressions, epinephrine is administered via umbilical venous catheter (or less optimally via endotracheal tube).5–7
Depending on the skill of the resuscitator, the infant can be intubated and PPV delivered via endotracheal tube if chest compressions are needed or if bag and mask ventilation is prolonged or ineffective (with no chest rise).5 Heart rate, respiratory effort, and color are reassessed and verbalized every 30 seconds as PPV and chest compressions are performed. Once the heart rate increases to more than 60 bpm, chest compressions are stopped. When the heart rate increases to more than 100 bpm, PPV may be discontinued if there is effective respiratory effort.5 Oxygen is decreased and discontinued once the infant's oxygen saturation meets the targeted levels (Figure 1).5
If there is no heartbeat after 10 minutes of adequate resuscitative efforts, the team can cease further resuscitation.1,5,6 A member of the team should keep the family informed during the resuscitation process. Table 1 lists evidence and recommendations for interventions during neonatal resuscitation.1,2,5–7,20–43
Table 1. Evidence and Recommendations for Interventions During Neonatal Resuscitation
| Intervention | Evidence | Recommendation | |
|---|---|---|---|
| Treatment of infants born through meconium-stained amniotic fluid | |||
| Intrapartum suctioning | A multicenter randomized trial showed that intrapartum suctioning of meconium does not reduce the risk of meconium aspiration syndrome.20 | ||
| Endotracheal suctioning | A randomized trial showed that endotracheal suctioning of vigorous* infants born through meconium-stained amniotic fluid is not beneficial.21 | ||
| A nonrandomized trial showed that endotracheal suctioning did not decrease the incidence of meconium aspiration syndrome or mortality.22 | |||
| Ventilation strategies for term infants | |||
| Assisted ventilation device | Ventilation using a flow-inflating bag, self-inflating bag, or T-piece device can be effective.23 | ||
| Initial breaths | The primary objective of neonatal resuscitation is effective ventilation; an increase in heart rate indicates effective ventilation.24 |
| |
| Exhaled carbon dioxide detectors to confirm endotracheal tube placement | A prospective study showed that the use of an exhaled carbon dioxide detector is useful to verify endotracheal intubation.25 | ||
| Laryngeal mask airway | A randomized study showed similar success in providing effective ventilation using either laryngeal mask airway or endotracheal tube.26 | ||
| Use of CPAP | Use of CPAP for resuscitating term infants has not been studied.5 | ||
| Use of PEEP | No studies have examined PEEP vs. no PEEP when positive pressure ventilation is used after birth.5 |
| |
| Supplemental oxygen: 100 vs. 21 percent (room air) | There is a reduction of mortality and no evidence of harm in term infants resuscitated with 21 percent compared with 100 percent oxygen.5,6,27 |
| |
| Ventilation strategies for preterm infants | |||
| Initial breaths | Premature animals exposed to brief high tidal volume ventilation (from high PIP) develop lung injury, impaired gas exchange, and decreased lung compliance.28 | ||
| Use of CPAP | In a randomized trial, the use of mask CPAP compared with endotracheal intubation and mechanical ventilation in spontaneously breathing preterm infants decreased the risk of bronchopulmonary dysplasia or death, and decreased the use of surfactant, but increased the rate of pneumothorax.29 | ||
| Supplemental oxygen | Preterm infants less than 32 weeks' gestation are more likely to develop hyperoxemia with the initial use of 100 percent oxygen, and develop hypoxemia with 21 percent oxygen compared with an initial concentration of 30 or 90 percent oxygen.30,31 | ||
| Chest compressions | |||
| During resuscitation | A combination of chest compressions and ventilation resulted in better outcomes than ventilation or compressions alone in piglet studies.6,32 |
| |
| A 3:1 ratio of compressions to ventilation provided more ventilations than higher ratios in manikin studies.6,33 | |||
| The chest compression technique of using two thumbs, with the fingers encircling the chest and supporting the back, achieved better results in swine models compared with the technique of using two fingers, with a second hand supporting the back.5,6,34 | |||
| Medications | |||
| Route and dose of epinephrine | In a case series, endotracheal epinephrine (0.01 mg per kg) was less effective than intravenous epinephrine.35 |
| |
| Higher doses (0.05 to 0.1 mg per kg) of endotracheal epinephrine are needed to achieve an increase in blood epinephrine concentration.36 | |||
| Volume expansion | In a retrospective study, volume infusion was given more often for slow response of bradycardia to resuscitation than for overt hypovolemia.37 | ||
| Naloxone | There was no difference in Apgar scores or blood gas with naloxone compared with placebo.38 | ||
| Sodium bicarbonate | In a randomized trial, the use of sodium bicarbonate in the delivery room did not improve survival or neurologic outcome.39 |
| |
| Postresuscitation management | |||
| Induced therapeutic hypothermia | Randomized trials have shown that infants born at 36 weeks' gestation or later with moderate to severe hypoxic-ischemic encephalopathy who were cooled to 92.3°F (33.5°C) within six hours after birth had significantly lower mortality and less disability at 18 months compared with those not cooled.40,41 | ||
| Glucose | In a retrospective review, early hypoglycemia was a risk factor for brain injury in infants with acidemia requiring resuscitation.42 | ||
| Resuscitation of preterm infants | |||
| Temperature control | Hypothermia at birth is associated with increased mortality in preterm infants. | ||
| Wrapping, in addition to radiant heat, improves admission temperature of preterm infants.43 |
| ||
bpm = beats per minute; CPAP = continuous positive airway pressure; PEEP = positive end-expiratory pressure; PIP = peak inspiratory pressure.
*—Defined as strong respiratory effort, good muscle tone, and a heart rate greater than 100 bpm.
Information from references 1, 2, 5 through 7, and 20 through 43.
Interventions
POSITIVE PRESSURE VENTILATION
If the infant's heart rate is less than 100 bpm, PPV via face mask (not mask continuous positive airway pressure) is initiated at a rate of 40 to 60 breaths per minute to achieve and maintain a heart rate of more than 100 bpm.1,2,5–7 PPV can be administered via flow-inflating bag, self-inflating bag, or T-piece device.1,6 There is no major advantage of using one ventilatory device over another.23 Thus, each institution should standardize its equipment and train the neonatal resuscitation team appropriately.
If the infant needs PPV, the recommended approach is to monitor the inflation pressure and to initiate PPV using a peak inspiratory pressure (PIP) of 20 cm H2O for the first few breaths; however, a PIP of 30 to 40 cm H2O (in some term infants) may be required at a rate of 40 to 60 breaths per minute.5,6 The best measure of adequate ventilation is prompt improvement in heart rate.24 Auscultation of the precordium is the primary means of assessing heart rate, but for infants requiring respiratory support, pulse oximetry is recommended.5,6 However, if the heart rate does not increase with mask PPV and there is no chest rise, ventilation should be optimized by implementing the following six steps: (1) adjust the mask to ensure a good seal; (2) reposition the airway by adjusting the position of the head; (3) suction the secretions in the mouth and nose; (4) open the mouth slightly and move the jaw forward; (5) increase the PIP enough to move the chest; and (6) consider an alternate airway (endotracheal intubation or laryngeal mask airway).5 PIP may be decreased when the heart rate increases to more than 60 bpm, and PPV may be discontinued once the heart rate is more than 100 bpm and there is spontaneous breathing.
The usefulness of positive end-expiratory pressure during PPV for term infant resuscitation has not been studied.6 A recent study showed that use of mask continuous positive airway pressure for resuscitation and treatment of respiratory distress syndrome in spontaneously breathing preterm infants reduced the need for intubation and subsequent mechanical ventilation without increasing the risk of bronchopulmonary dysplasia or death.29 In a preterm infant needing PPV, a PIP of 20 to 25 cm H2O may be adequate to increase heart rate while avoiding a higher PIP to prevent injury to preterm lungs, and positive end-expiratory pressure may be beneficial if suitable equipment is available.6
ENDOTRACHEAL INTUBATION
Endotracheal intubation is indicated in very premature infants; for suctioning of nonvigorous infants born through meconium-stained amniotic fluid; and when bag and mask ventilation is necessary for more than two to three minutes, PPV via face mask does not increase heart rate, or chest compressions are needed. If skilled health care professionals are available, infants weighing less than 1 kg, 1 to 3 kg, and 3 kg or more can be intubated with 2.5-, 3-, and 3.5-mm endotracheal tubes, respectively. 1 Exhaled carbon dioxide detection is the recommended method of confirming endotracheal intubation. The exhaled carbon dioxide detector changes from purple to yellow with endotracheal intubation, and a negative result suggests esophageal intubation.5,6,25 Clinical indicators of endotracheal intubation, such as condensation in the tube, chest wall movement, or presence of bilateral equal breath sounds, have not been well studied.
LARYNGEAL MASK AIRWAY
When attempts at endotracheal intubation are unsuccessful, laryngeal mask airway (size 1) is an alternative for providing PPV in infants weighing more than 2 kg or in infants greater than 34 weeks' gestation.5,6,26
CONCENTRATION OF OXYGEN
Neonatal resuscitation aims to restore tissue oxygen delivery before irreversible damage occurs. Traditionally, 100 percent oxygen has been used to achieve a rapid increase in tissue oxygen in infants with respiratory depression. However, free radicals are generated when successful resuscitation results in reperfusion and restoration of oxygen delivery to organs.44 Use of 100 percent oxygen may increase the load of oxygen free radicals, which can potentially lead to end-organ damage. Recent clinical trials have shown that infants resuscitated with 21 percent oxygen compared with 100 percent oxygen had significantly lower mortality (at one week and one month) and were able to establish regular respiration in a shorter time; the rates of encephalopathy and cerebral palsy were similar in the two groups.45–49 The 2010 NRP guidelines recommend starting resuscitation of term infants with 21 percent oxygen or blended oxygen and increasing the concentration of oxygen (using an air/oxygen blender) if oxygen saturation (measured using a pulse oximeter) is lower than recommended targets (Figure 1).5 Oxygen concentration should be increased to 100 percent if the heart rate is less than 60 bpm despite effective ventilation, and when chest compressions are necessary.5–7
CHEST COMPRESSIONS
If the infant's heart rate is less than 60 bpm, the delivery of PPV is optimized and applied for 30 seconds. The heart rate is reassessed,6 and if it continues to be less than 60 bpm, synchronized chest compressions and PPV are initiated in a 3:1 ratio (three compressions and one PPV).5,6 Chest compressions can be done using two thumbs, with fingers encircling the chest and supporting the back (preferred), or using two fingers, with a second hand supporting the back.5,6 Compressions should be delivered to the lower one-third of the sternum to a depth of approximately one-third of the anteroposterior diameter.5,6 The heart rate is reassessed at 45- to 60-second intervals, and chest compressions are stopped once the heart rate exceeds 60 bpm.5,6
Medications
Epinephrine is indicated if the infant's heart rate continues to be less than 60 bpm after 30 seconds of adequate PPV with 100 percent oxygen and chest compressions. It is important to continue PPV and chest compressions while preparing to deliver medications. The neonatal epinephrine dose is 0.01 to 0.03 mg per kg (1:10,000 solution) given intravenously (via umbilical venous catheter).1,2,5,6 If there is any delay in securing venous access, epinephrine can be given via endotracheal tube at a higher dose of 0.05 to 0.10 mg per kg (1:10,000 solution), followed by intravenous dosing, if necessary, as soon as access is established.5
Naloxone is not recommended during neonatal resuscitation in the delivery room; infants with respiratory depression should be resuscitated with PPV.1,2,5,6 Volume expansion (using crystalloid or red blood cells) is recommended when blood loss is suspected (e.g., pale skin, poor perfusion, weak pulse) and when the infant's heart rate continues to be low despite effective resuscitation.5,6 Sodium bicarbonate is not recommended during neonatal resuscitation in the delivery room, because it does not improve survival or neurologic outcome.6,39
Meconium-Stained Amniotic Fluid
Approximately 7 to 20 percent of deliveries are complicated by meconium-stained amniotic fluid; these infants have a 2 to 9 percent risk of developing meconium aspiration syndrome.50 Oral and nasopharyngeal suction on the perineum is not recommended, because it has not been shown to reduce the risk of meconium aspiration syndrome.20 In the absence of randomized controlled trials, there is insufficient evidence to recommend changing the current practice of intubation and endotracheal suction in nonvigorous infants (as defined by decreased heart rate, respiratory effort, or muscle tone) born through meconium-stained amniotic fluid.1,2,5 However, if attempted intubation is prolonged or unsuccessful, and bradycardia is present, bag and mask ventilation is advised.5,6 Endotracheal suctioning of vigorous infants is not recommended.1,2,5,6
Withholding and Discontinuing Resuscitation
Withholding resuscitation and offering comfort care is appropriate (with parental consent) in certain infants, such as very premature infants (born at less than 23 weeks' gestation or weighing less than 400 g) and infants with anencephaly or trisomy 13 syndrome.5 If there is no detectable heart rate after 10 minutes of resuscitation, it is appropriate to consider discontinuing resuscitation.5,6
Postresuscitation Management
Intravenous glucose infusion should be started soon after resuscitation to avoid hypoglycemia.5,6 In addition, infants born at 36 weeks' gestation or later with evolving moderate to severe hypoxic-ischemic encephalopathy should be offered therapeutic hypothermia, using studied protocols, within six hours at a facility with capabilities of multidisciplinary care and long-term follow-up.5–7

