Guideline source: American Heart Association/American Stroke Association
Evidence rating system used? Yes
Literature search described? Yes
Published source:Stroke, January 2011
Available at: http://stroke.ahajournals.org/cgi/content/full/42/1/227
Persons who survive a stroke or transient ischemic attack (TIA) are at increased risk of experiencing another stroke. In the United States, about one-fourth of the nearly 800,000 strokes that occur each year are recurrent events. The risk of stroke within 90 days of a TIA may be as high as 17 percent, with the greatest risk during the first week.
The American Heart Association (AHA) and the American Stroke Association (ASA) have released updated guidelines on preventing recurrent stroke in patients who have had a previous stroke or TIA. The guidelines address risk factors for stroke, including treatable vascular risk factors (Table 1) and modifiable behavioral risk factors (Table 2); interventional approaches for patients with large-artery atherosclerosis; medical treatments for patients with cardiogenic embolism; and antithrombotic therapy for noncardioembolic stroke or TIA. This summary focuses on risk factors and antithrombotic therapy.
Table 1. Recommendations for Treatable Vascular Risk Factors to Prevent Recurrent Stroke
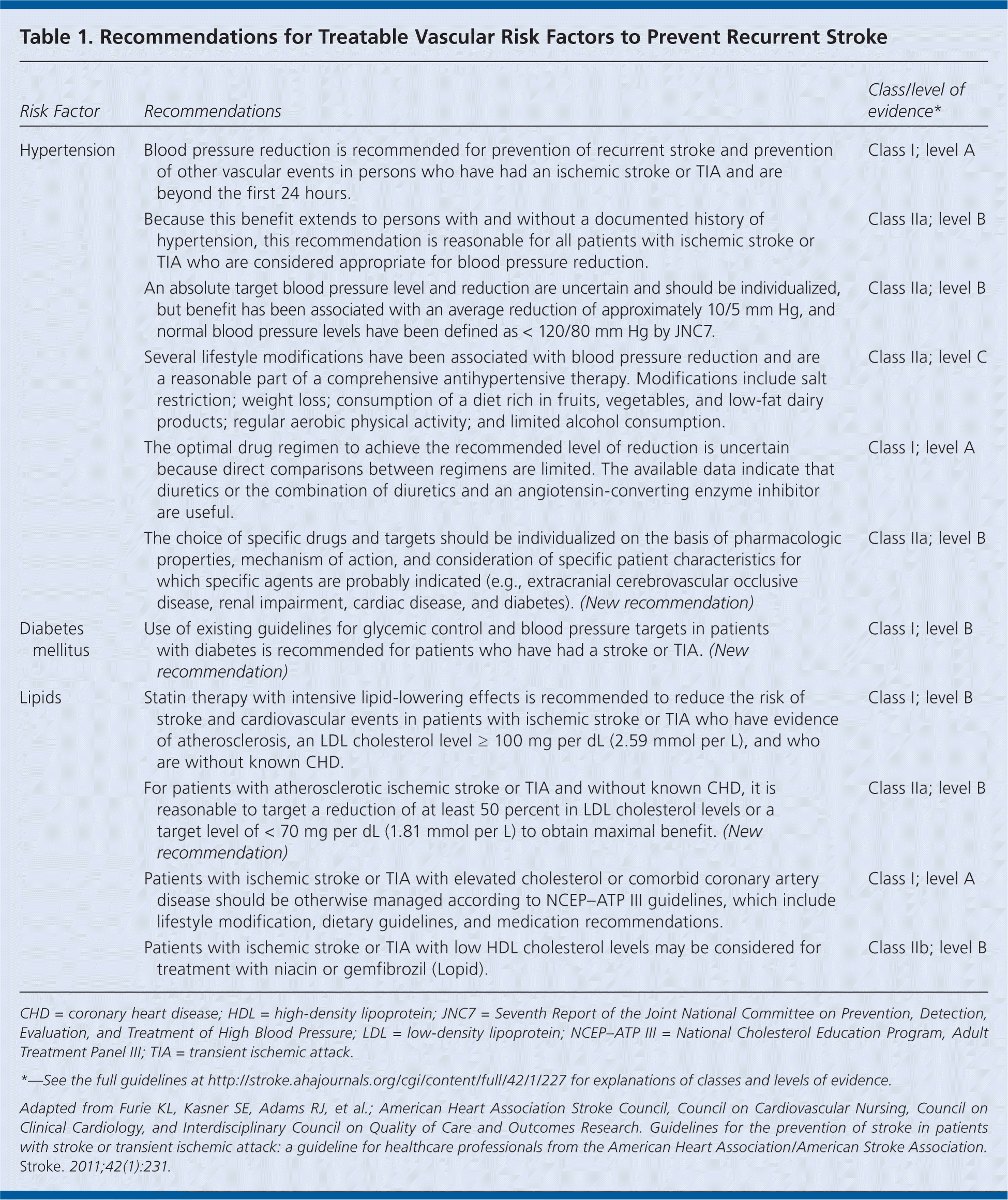
Table 2. Recommendations for Modifiable Behavioral Risk Factors to Prevent Recurrent Stroke

Treatable Vascular Risk Factors
HYPERTENSION
Meta-analyses of randomized controlled trials have shown that lowering blood pressure can reduce the risk of stroke by 30 to 40 percent. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure recommends lifestyle modifications to manage hypertension. Lifestyle changes associated with a reduction in blood pressure include losing weight; restricting salt intake; consuming a diet high in fruits, vegetables, and low-fat dairy products; participating in regular aerobic exercise; and limiting alcohol intake. Although there is a lack of definitive data addressing the management of hypertension immediately following a stroke, a meta-analysis of randomized trials found that treatment with antihypertensive medications significantly reduces the risk of recurrent stroke. The reduction in risk was seen in patients taking diuretics alone and in combination with angiotensin-converting enzyme inhibitors, but not in patients taking beta blockers or angiotensin-converting enzyme inhibitors alone.
DIABETES
The prevalence of diabetes mellitus in patients with ischemic stroke is 15 to 33 percent. Although diabetes is a risk factor for first stroke, there are limited data showing that diabetes is a risk factor for recurrent stroke. It is estimated that diabetes causes approximately 9 percent of recurrent strokes. Diet, exercise, oral hypoglycemic drugs, and insulin are recommended in patients with diabetes to control glycemic levels. Existing guidelines recommend glycemic control and blood pressure management in patients with diabetes who have had a stroke or TIA. Intensive glucose management has not been shown to reduce rates of cardiovascular events or death in persons with a history of cardiovascular disease, stroke, or additional vascular risk factors.
LIPIDS
Large epidemiologic studies have demonstrated a modest association between elevated total cholesterol or low-density lipoprotein levels and an increased risk of ischemic stroke. Other studies have found a link between high serum triglyceride levels and ischemic stroke and large-artery atherosclerotic stroke. Low levels of high-density lipoproteins have also been linked to ischemic stroke. Statin therapy is recommended in patients with ischemic stroke or TIA, even without known coronary heart disease, to reduce the risk of stroke and cardiovascular events. The National Cholesterol Education Program, Adult Treatment Panel III recommends reducing low-density lipoprotein levels as the primary target in managing dyslipidemia. Lifestyle modifications that include decreasing saturated fat and cholesterol intake, achieving ideal body weight, and increasing physical activity are also recommended.
Modifiable Behavioral Risk Factors
CIGARETTE SMOKING
Cigarette smoking is an independent risk factor for ischemic stroke, and growing evidence has shown that exposure to environmental smoke increases the risk of cardiovascular disease, including stroke. Smoking cessation is recommended in persons who have experienced a stroke or TIA.
ALCOHOL CONSUMPTION
Chronic alcoholism and heavy drinking are risk factors for stroke. One cohort study found a significant increase in stroke recurrence in patients with previous heavy alcohol use who had experienced ischemic stroke. Although light or moderate drinking may provide a protective effect against ischemic stroke by increasing high-density lipoprotein levels, heavy drinking can cause hypertension, hypercoagulable state, reduced cerebral blood flow, and atrial fibrillation or cardioembolism from cardiomyopathy. Alcoholism has also been linked to insulin resistance and metabolic syndrome.
OBESITY
Although obesity (defined as a body mass index greater than 30 kg per m2) is an independent risk factor for coronary heart disease and premature mortality, no studies have demonstrated that weight loss reduces the risk of recurrent stroke.
PHYSICAL ACTIVITY
Physical activity has a beneficial effect on several stroke risk factors. However, persons who have had a stroke may experience substantial disability that can make exercising difficult. Studies have shown that aerobic exercise and strength training improve cardiovascular fitness, mobility, balance, and endurance after a stroke, but it has not been determined that therapeutic exercise reduces the risk of recurrent stroke. Results from one survey found that patients who received advice on physical activity after a stroke were more likely to exercise than those who did not receive advice. Also, those who exercised after surviving a stroke were less likely to have days with limited activity or poor physical health than those who did not exercise.
METABOLIC SYNDROME
Metabolic syndrome is used to describe the convergence of several abnormalities that increase the risk of vascular disease, including hypertriglyceridemia, low high-density lipoprotein cholesterol levels, high blood pressure, and hyperglycemia. Patients with metabolic syndrome have an increased risk of diabetes, cardiovascular disease, and all-cause mortality. The prevalence of metabolic disease in patients with ischemic stroke is 40 to 50 percent. Studies have confirmed an association between metabolic syndrome and first ischemic stroke, but only one study has examined the association with recurrent stroke. Results found that participants with metabolic syndrome were more likely to have a stroke, myocardial infarction (MI), or vascular death within 1.8 years of follow-up than those without metabolic syndrome. Diet, exercise, and use of medications that enhance insulin sensitivity have been shown to benefit persons with metabolic syndrome.
Antithrombotic Therapy
ANTIPLATELET AGENTS
Four antiplatelet medications have been approved by the U.S. Food and Drug Administration for preventing vascular events in patients with a stroke or TIA: aspirin, ticlopidine, clopidogrel (Plavix), and combination aspirin/dipyridamole (Aggrenox). On average, these agents have been shown to reduce the relative risk of stroke, MI, or death by more than 20 percent. Table 3 lists recommendations for antithrombotic therapy for noncardioembolic stroke or TIA.
Table 3. Recommendations for Antithrombotic Therapy for Noncardioembolic Stroke or TIA

Aspirin. Aspirin therapy prevents stroke in patients who have had a recent stroke or TIA. Although the level of benefit is comparable for dosages between 50 and 1,500 mg per day, higher dosages are associated with an increased risk of gastrointestinal hemorrhage. The increased risk of hemorrhagic stroke in patients taking aspirin is smaller than the risk of ischemic stroke, which results in a net benefit of aspirin therapy.
Ticlopidine. Three randomized trials have investigated the use of ticlopidine in patients with cerebrovascular disease with mixed results. One trial evaluated ticlopidine therapy and placebo for prevention of stroke, MI, or vascular death in patients with ischemic stroke. Persons assigned to ticlopidine therapy had fewer outcomes per year after a mean follow-up of two years. A second trial compared ticlopidine with aspirin use in patients with recent minor stroke or TIA, and found that those taking ticlopidine had a lower rate of stroke or death. A third trial assigned black patients with recent noncardioembolic ischemic stroke to receive aspirin or ticlopidine. No difference was found between the groups in the risk of the combination of stroke, MI, or vascular death at two years.
Adverse effects associated with ticlopidine use include diarrhea and rash. Ticlopidine is also associated with thrombotic thrombocytopenic purpura. Rates of gastrointestinal bleeding are similar or lower in patients taking ticlopidine than in patients taking aspirin.
Clopidogrel. Two trials have evaluated the use of clopidogrel for secondary stroke prevention. One trial compared clopidogrel with aspirin alone, and the other with combination aspirin/dipyridamole. Results from both trials found that rates of primary outcomes were similar between treatment groups. Adverse effects of clopidogrel include diarrhea and rash, although gastrointestinal symptoms and hemorrhage are less common than in persons taking aspirin. Proton pump inhibitors have been shown to reduce the effectiveness of clopidogrel, and may also increase the risk of major cardiovascular events when taken with clopidogrel.
Aspirin/dipyridamole. Four large randomized trials have examined the effects of combination aspirin/dipyridamole in patients with TIA or stroke. Results showed that combination therapy is at least as effective as aspirin alone for prevention of stroke; however, it is not tolerated as well by patients.
Clopidogrel and aspirin. Compared with clopidogrel alone, the combination of clopidogrel and aspirin for prevention of vascular effects in persons with a recent TIA or ischemic stroke was not found to have a significant benefit. There was a significantly increased risk of major hemorrhage in persons taking combination therapy compared with those taking clopidogrel alone. When compared with aspirin alone, combination clopidogrel and aspirin did not have a statistically significant benefit but did increase the risk of bleeding in patients who had previously had a stroke.
Selecting oral antiplatelet therapy. Selecting between aspirin, ticlopidine, clopidogrel, and combination aspirin/dipyridamole should be based on relative effectiveness, safety, cost, patient characteristics, and patient preference. Evidence shows that each therapy is effective for the prevention of secondary stroke. In persons who experience a stroke while on antiplatelet therapy, no studies have shown that switching to a different antiplatelet agent reduces the risk of a subsequent event.
Three additional antiplatelet agents are being investigated for effectiveness in secondary stroke prevention: triflusal, cilostazol (Pletal), and sarpogrelate. At this time, none has been approved by the U.S. Food and Drug Administration for prevention of recurrent stroke.
ORAL ANTICOAGULANTS
Oral anticoagulants have been evaluated for the prevention of recurrent stroke in patients with noncardioembolic stroke. One trial was stopped and reformatted because of increased bleeding in patients taking highintensity oral anticoagulants. After reformulating the study to compare warfarin (Coumadin) with aspirin alone or with aspirin plus extended-release dipyridamole, the trial was halted again because of the superiority in patients taking combination aspirin/dipyridamole. Compared with patients taking aspirin alone, patients taking warfarin experienced a significantly higher rate of major bleeding, but a nonstatistically significant decrease in the rate ischemic events.

