Am Fam Physician. 2011;83(9):1054
Hospital readmission after discharge is often a costly failing of the U.S. health care system to adequately manage patients who are ill. Increasing the numbers of family physicians (FPs) is associated with significant reductions in hospital readmissions and substantial cost savings.
The Patient Protection and Affordable Care Act (PPACA) seeks to improve health care quality and reduce costs. One provision targets a decrease in hospital readmissions to save $710 million annually.1 Timely management of recovering patients in primary care after discharge may reduce readmission. The Medicare Hospital Compare Database includes readmission rates for pneumonia, heart attack, and heart failure for 4,459 hospitals.2 The Area Resource File contains data for physicians per population at the county level.3 Data show that 30-day readmission rates for these diagnoses decrease as the number of FPs increases. Conversely, increased numbers of physicians in all other major specialties (including general internal medicine) is associated with increased risk of readmission.
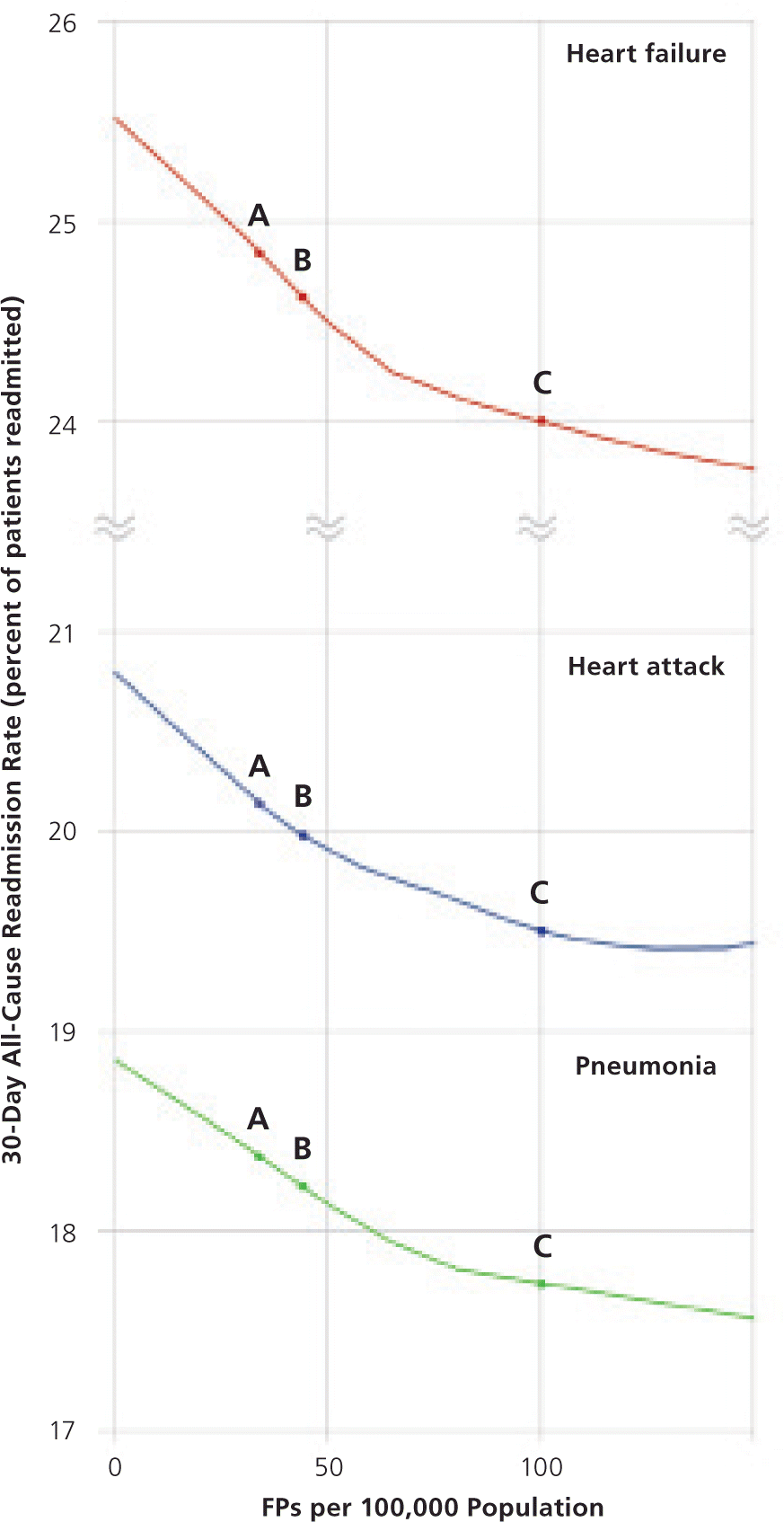
Combined, readmissions for pneumonia, heart attack, and heart failure in 2005 accounted for 15.7 percent of all readmissions and numbered 74,419, 20,866, and 90,273, respectively (see accompanying figure2,3 ); corresponding Medicare expenditures were $533, $136, and $590 million, respectively.4 Adding one FP per 1,000 population, or 100 per 100,000 (adjusted for mortality, sociodemographics, and hospital characteristics), reduces readmission odds for these three conditions by 7, 5, and 8 percent, respectively. An estimated 46 FPs per 100,000 population, recommended by one workforce study, could reduce readmission costs by $81 million per year; furthermore, 100 FPs per 100,000 population could reduce costs by $579 million per year, or 83 percent of the PPACA target.5
Wider experience of the associated effects of FPs on readmission rates could help realize much of the savings sought by the PPACA. Production of FPs fell over the past decade because of payment disparities and other strong incentives for subspecialization, and lack of accountability in U.S. teaching hospitals for producing needed FPs.6