
Am Fam Physician. 2011;83(10):1219-1227
| Guideline source: American Psychiatric Association |
| Evidence rating system used? Yes |
| Literature search described? Yes |
| Available at: http://www.psychiatryonline.com/pracGuide/pracGuideTopic_7.aspx |
The American Psychiatric Association (APA) recently updated its guideline on the treatment of major depressive disorder. The new evidence-based guideline summarizes recommendations on the use of antidepressants and other drug therapies; psychotherapy, including cognitive behavior therapy; and electroconvulsive therapy (ECT). Because many patients with major depressive disorder have co-occurring psychiatric disorders, including substance use disorders, physicians should also consider appropriate treatments for these diagnoses. Patients who have depressive symptoms in the context of another disorder but who do not meet the diagnostic criteria for major depressive disorder should be treated according to guidelines pertaining to the primary diagnosis.
Acute Phase
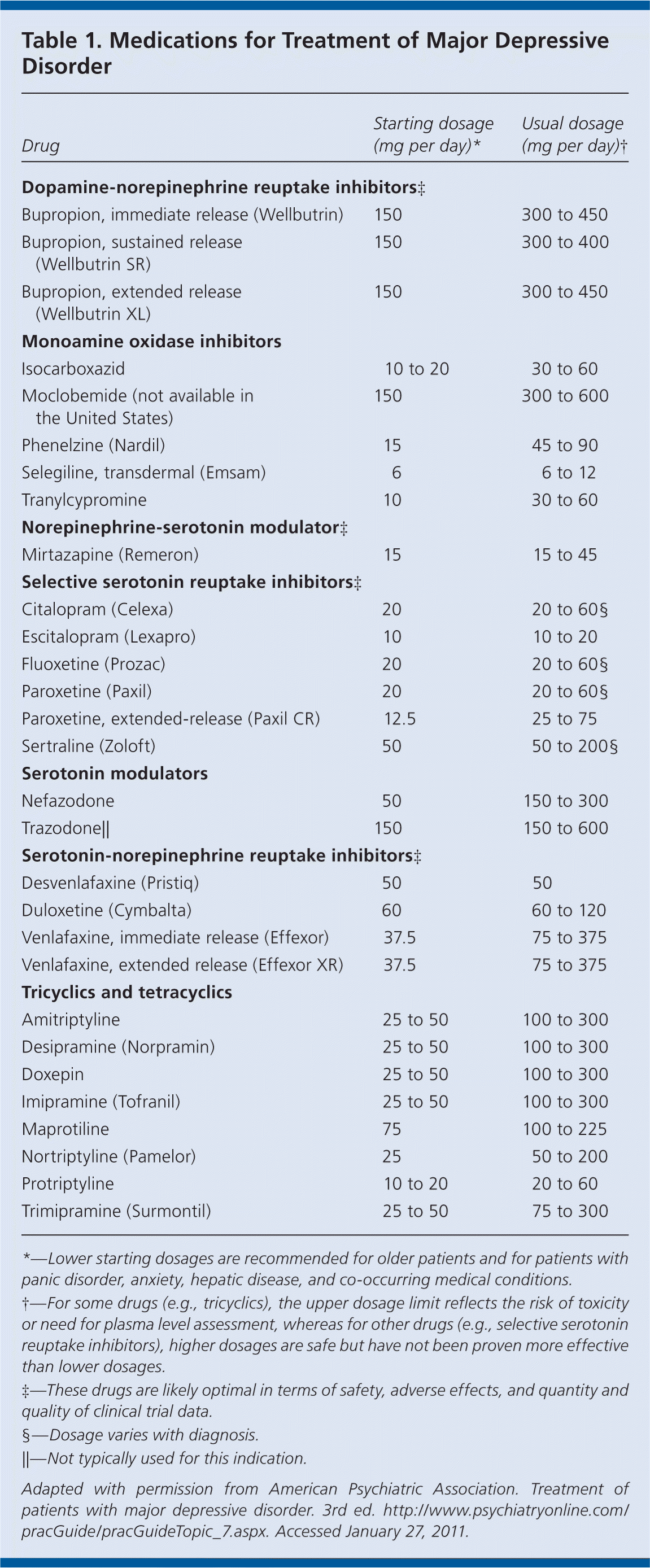
Treatment in the acute phase should be aimed at inducing remission of the depressive episode and achieving a full return to the baseline level of functioning. Patients with mild to moderate depression should be treated with antidepressants (Table 1) or psychotherapy. Combined pharmacotherapy and psychotherapy may be useful in patients with psychosocial or interpersonal problems, intrapsychic conflict, or a co-occurring axis II disorder. ECT can be used in select patients.
In patients with severe depression without psychotic features, pharmacotherapy, combined pharmacotherapy and psychotherapy, or ECT can be used; however, psychotherapy should not be used alone. In patients with severe depression with psychotic features, antidepressant and antipsychotic agents should be used, with or without psychotherapy. ECT is also an option.
Selection of an initial treatment modality should be influenced by clinical features, such as severity of symptoms and presence of co-occurring disorders, as well as other factors, such as patient preferences and prior treatment experiences. Because the effectiveness of antidepressants is generally comparable between and within drug classes, the initial selection will be based largely on anticipated adverse effects, safety and tolerability, pharmacologic properties (e.g., half-life, drug interactions), and cost. For most patients, optimal treatments include a selective serotonin reuptake inhibitor, a serotonin-norepinephrine reuptake inhibitor, mirtazapine (Remeron), or bupropion (Wellbutrin). The use of nonselective monoamine oxidase inhibitors should be restricted to patients who do not respond to other treatments. In patients who prefer complementary and alternative therapies, S-adenosylmethionine (SAM-e) or St. John's wort can be considered. However, patients who take St. John's wort should be monitored carefully for drug interactions.
Once an antidepressant has been selected, it should be titrated based on the patient's age, the treatment setting, and the presence of co-occurring disorders, concomitant pharmacotherapy, or adverse effects of medication. If adverse effects occur, the dosage can be lowered or the patient should be switched to a different medication.
An incomplete response to treatment is associated with poor functional outcomes; therefore, the acute phase of treatment should not be concluded prematurely in patients who do not fully respond. If a moderate improvement in symptoms does not occur within four to eight weeks after treatment initiation, the diagnosis should be reconsidered, adverse effects and adherence to therapy assessed, comorbidities and psychosocial factors reviewed, and the treatment plan adjusted. For patients who are being treated with psychotherapy, the frequency of sessions and the specific approach to psychotherapy should be reassessed. If minimal or no improvement is noted after an additional four to eight weeks, the treatment plan should be readjusted, and consultation should be considered.
Continuation Phase
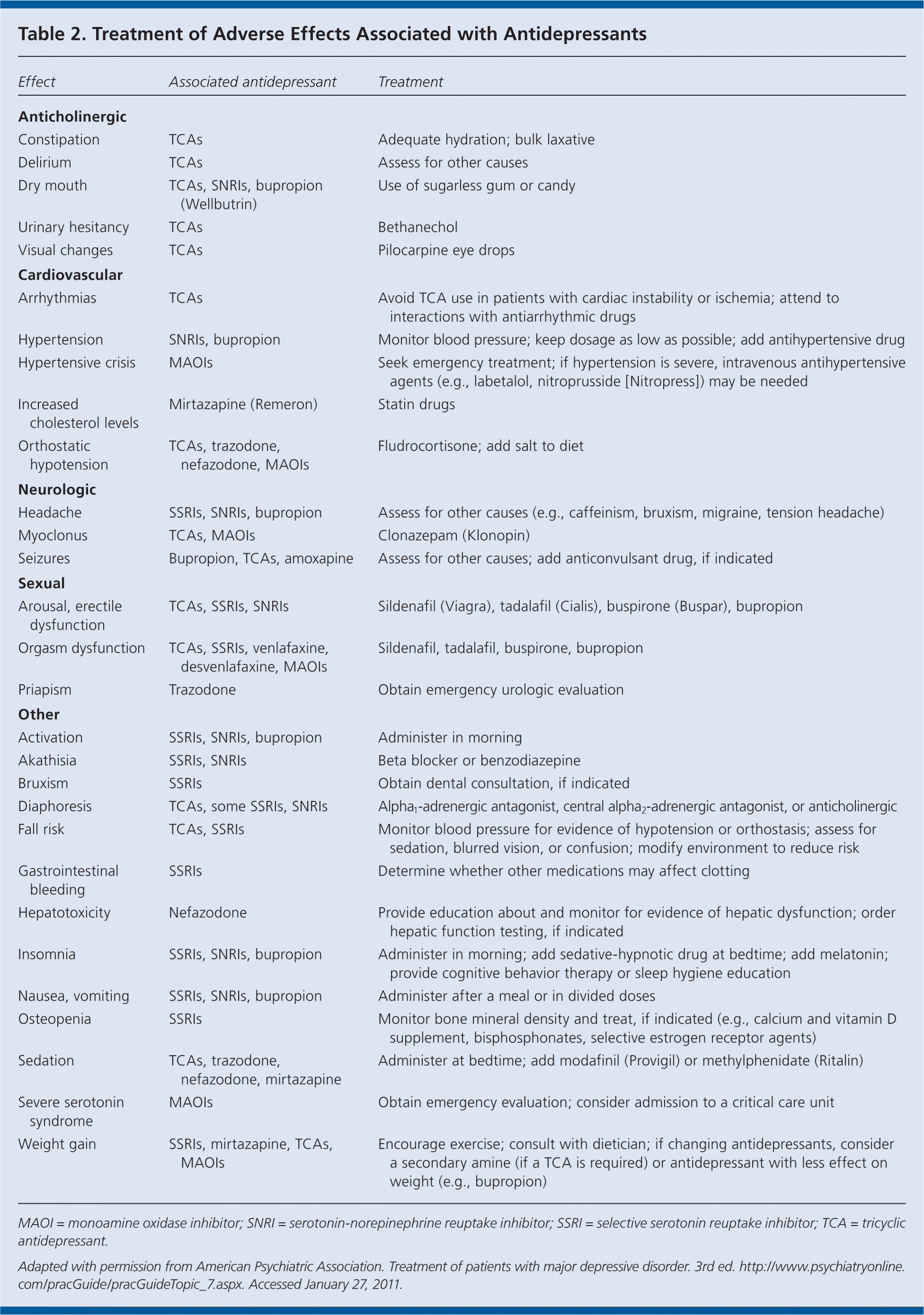
In the continuation phase, management is aimed at preventing relapse. Systematic assessment of symptoms and monitoring for adverse effects of medications (Table 2), adherence to therapy, and functional status are essential. To reduce the risk of relapse, patients in whom pharmacotherapy has been successful should continue treatment at the same dosage for four to nine months. Depression-focused cognitive behavior therapy is also recommended in the continuation phase.
Patients who respond to ECT should continue treatment with medication; a combination of lithium and nortriptyline (Pamelor) is recommended. Alternatively, continuation ECT can be given, especially if medication and psychotherapy have been ineffective.
Maintenance Phase
Patients who have had three or more episodes of major depression or who have chronic major depressive disorder should proceed to the maintenance phase of treatment after completing the continuation phase. Maintenance therapy should also be considered for patients with additional risk factors for recurrence (e.g., residual symptoms, ongoing psychosocial stressors, early age at onset). Additional considerations include patient preference, the type of treatment received, adverse effects, comorbid conditions, frequency and severity of previous depressive episodes (including psychosis and suicide risk), and the persistence of depressive symptoms after recovery. In many patients—particularly those with chronic and recurrent major depressive disorder or co-occurring medical or psychiatric disorders—some form of treatment will be required indefinitely. Because of the risk of recurrence, patients should be monitored at regular intervals during the maintenance phase.
The antidepressant that produced symptom remission during the acute phase should be continued at the full therapeutic dosage. If depression-focused psychotherapy was used during the acute and continuation phases, maintenance therapy should be considered, with less frequent sessions. Maintenance ECT can be considered in patients with depressive episodes that have not responded to medications or depression-focused psychotherapy, but that have responded to ECT.
Discontinuation
Pharmacotherapy should be tapered over the course of at least several weeks. Before discontinuation of active treatment, patients should be counseled about the potential for relapse, and a plan should be established for seeking treatment if symptoms recur. Patients should be monitored for several months after medications are discontinued, and they should receive another course of acute-phase treatment if symptoms recur.
