Knee osteoarthritis is a common disabling condition that affects more than one-third of persons older than 65 years. Exercise, weight loss, physical therapy, intra-articular corticosteroid injections, and the use of nonsteroidal anti-inflammatory drugs and braces or heel wedges decrease pain and improve function. Acetaminophen, glucosamine, ginger, S-adenosylmethionine (SAM-e), capsaicin cream, topical nonsteroidal anti-inflammatory drugs, acupuncture, and tai chi may offer some benefit. Tramadol has a poor trade-off between risks and benefits and is not routinely recommended. Opioids are being used more often in patients with moderate to severe pain or diminished quality of life, but patients receiving these drugs must be carefully selected and monitored because of the inherent adverse effects. Intra-articular corticosteroid injections are effective, but evidence for injection of hyaluronic acid is mixed. Arthroscopic surgery has been shown to have no benefit in knee osteoarthritis. Total joint arthroplasty of the knee should be considered when conservative symptomatic management is ineffective.
Osteoarthritis is a degenerative joint disease occurring primarily in older adults. It is characterized by erosion of the articular cartilage, hypertrophy of bone at the margins (i.e., osteophytes), and subchondral sclerosis.1 Arthritis is the leading cause of disability in the United States,2 and osteoarthritis is the most common condition affecting synovial joints.3 Despite its widespread prevalence, however, the precise etiology, pathogenesis, and progression of osteoarthritis are unknown. Several factors may make a person vulnerable to the disease (Table 1).
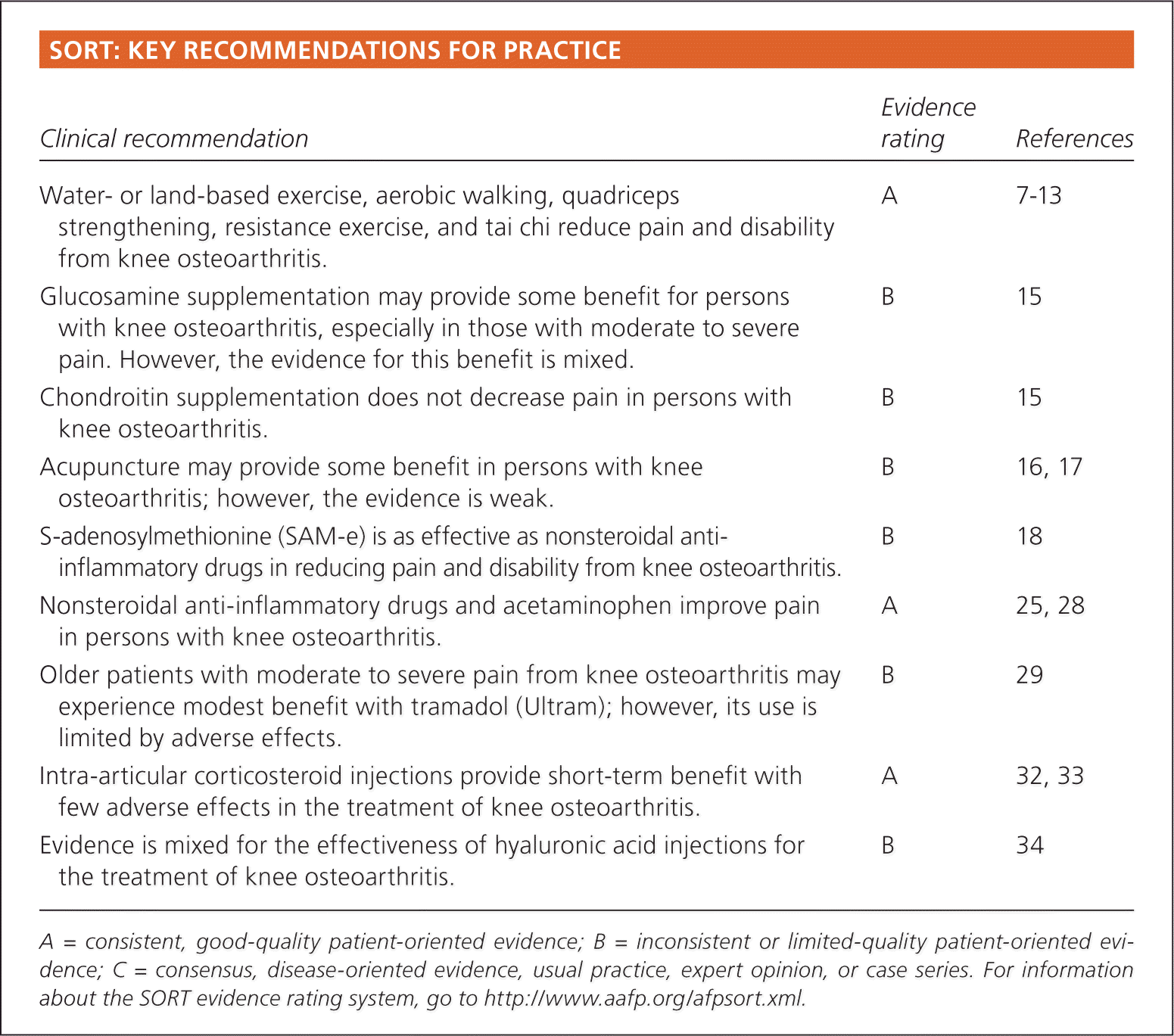
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Water- or land-based exercise, aerobic walking, quadriceps strengthening, resistance exercise, and tai chi reduce pain and disability from knee osteoarthritis. | A | 7–13 |
| Glucosamine supplementation may provide some benefit for persons with knee osteoarthritis, especially in those with moderate to severe pain. However, the evidence for this benefit is mixed. | B | 15 |
| Chondroitin supplementation does not decrease pain in persons with knee osteoarthritis. | B | 15 |
| Acupuncture may provide some benefit in persons with knee osteoarthritis; however, the evidence is weak. | B | 16, 17 |
| S-adenosylmethionine (SAM-e) is as effective as nonsteroidal anti-inflammatory drugs in reducing pain and disability from knee osteoarthritis. | B | 18 |
| Nonsteroidal anti-inflammatory drugs and acetaminophen improve pain in persons with knee osteoarthritis. | A | 25, 28 |
| Older patients with moderate to severe pain from knee osteoarthritis may experience modest benefit with tramadol (Ultram); however, its use is limited by adverse effects. | B | 29 |
| Intra-articular corticosteroid injections provide short-term benefit with few adverse effects in the treatment of knee osteoarthritis. | A | 32, 33 |
| Evidence is mixed for the effectiveness of hyaluronic acid injections for the treatment of knee osteoarthritis. | B | 34 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Table 1. Common Risk Factors for Knee Osteoarthritis

| Female sex |
| Inflammatory joint disease (e.g., infection, gout, rheumatoid arthritis) |
| No history of osteoporosis |
| Obesity (strongest modifiable risk factor) |
| Occupation requiring repetitive knee bending |
| Older age |
| Previous knee injury (e.g., torn meniscus, intra-articular mechanical damage) |
Osteoarthritis affects 33.6 percent of persons older than 65 years.4 About 80 percent of patients with knee osteoarthritis have some limitation of movement, and 25 percent cannot perform major activities of daily living.4 Approximately 11 percent of adults with knee osteoarthritis need help with personal care.4
Diagnosis of Osteoarthritis
The most common presenting symptom in persons with knee osteoarthritis is pain that is worse with use and better with rest. Other presenting signs and symptoms include stiffness that generally improves after 30 minutes of activity (inactivity gelling), crepitus, swelling, and limp. In advanced cases, patients may present with instability symptoms or genu valgum (knock knee) or varum (bow-leg). Varus deformity is more common than valgus deformity because the medial compartment of the knee is more often involved.
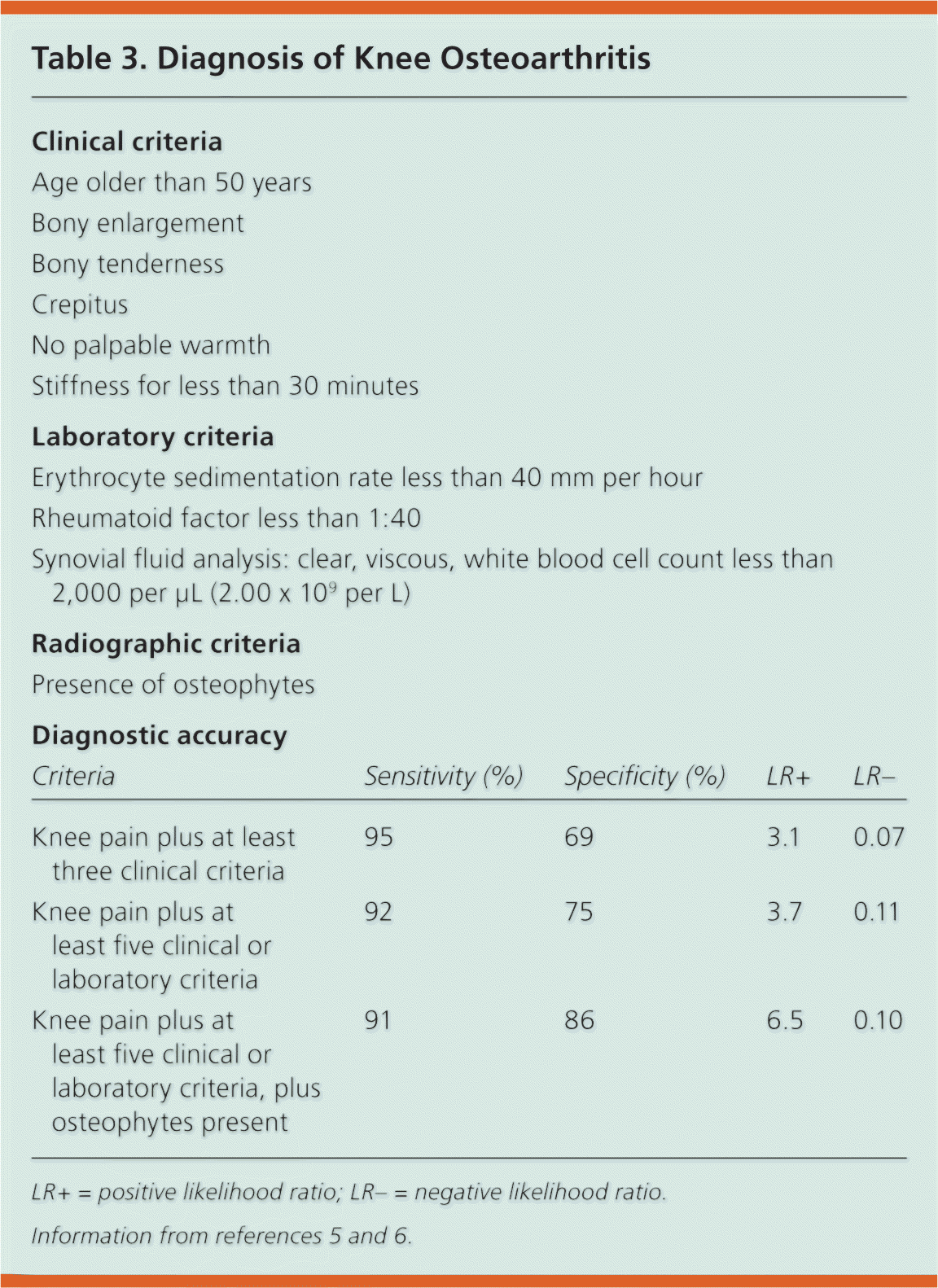
The differential diagnosis of chronic knee pain is given in Table 2. The criteria for diagnosing knee osteoarthritis are based on the presence of knee pain plus at least three of the six clinical characteristics listed in Table 3.5,6 The addition of laboratory and radiographic criteria enchances the diagnostic accuracy; however, these tests are not necessary for all patients. In most patients, the history, physical examination, and radiography are all that is needed.
Table 2. Differential Diagnosis of Knee Pain

| Conditions involving soft tissue of knee |
| Bursitis |
| Iliotibial band syndrome |
| Ligamentous instability (medial and lateral collateral ligaments) |
| Meniscal pathology |
| Other forms of arthritis |
| Gout and pseudogout |
| Rheumatoid arthritis |
| Septic arthritis |
| Referred pain |
| Neuropathy |
| Radiculopathy |
| Other |
| Avascular necrosis |
| Patellofemoral pain syndrome |
| Tumor |
Table 3. Diagnosis of Knee Osteoarthritis
| Clinical criteria | ||||
| Age older than 50 years | ||||
| Bony enlargement | ||||
| Bony tenderness | ||||
| Crepitus | ||||
| No palpable warmth | ||||
| Stiffness for less than 30 minutes | ||||
| Laboratory criteria | ||||
| Erythrocyte sedimentation rate less than 40 mm per hour | ||||
| Rheumatoid factor less than 1:40 | ||||
| Synovial fluid analysis: clear, viscous, white blood cell count less than 2,000 per μL (2.00 × 109 per L) | ||||
| Radiographic criteria | ||||
| Presence of osteophytes | ||||
| Diagnostic accuracy | ||||
| Criteria | Sensitivity (%) | Specificity (%) | LR+ | LR– |
| Knee pain plus at least three clinical criteria | 95 | 69 | 3.1 | 0.07 |
| Knee pain plus at least five clinical or laboratory criteria | 92 | 75 | 3.7 | 0.11 |
| Knee pain plus at least five clinical or laboratory criteria, plus osteophytes present | 91 | 86 | 6.5 | 0.10 |
LR+ = positive likelihood ratio; LR– = negative likelihood ratio.
Treatment
PHYSICAL MODALITIES AND EXERCISE
Physical modalities for the treatment of knee pain in patients with osteoarthritis include physical therapy, exercise, weight loss, and the use of braces or heel wedges. A review of physical therapy interventions for patients with knee osteoarthritis concluded that exercise and weight loss reduce pain and improve physical function.7 Exercise should be prescribed as a treatment for knee osteoarthritis. High- and low-intensity aerobic exercises are equally effective in improving functional status, gait, pain, and aerobic capacity in persons with knee osteoarthritis8; water-based and land-based exercises reduce knee pain and physical disability9,10; and aerobic walking, quadriceps strengthening, and resistance exercise reduce pain and disability.11,12 A small randomized controlled trial (RCT) showed that performing tai chi three times per week for 12 weeks decreased pain and improved physical functioning in older women with knee osteoarthritis.13 Any activity that worsens knee pain should be discontinued.
The use of braces and heel wedges may also be effective for treatment of knee osteoarthritis. There is some evidence that the use of a lateral heel wedge decreases the use of nonsteroidal anti-inflammatory drugs (NSAIDs).14 Similar evidence suggests that a brace and lateral wedge insole may have a small beneficial effect.14 Braces and heel wedges can be customized and purchased at stores specializing in orthotics.
COMPLEMENTARY AND ALTERNATIVE MEDICINE
Many complementary and alternative medicine treatments have been used to treat knee osteoarthritis, with variable success. Glucosamine and chondroitin supplements have been marketed since the 1990s as disease-modifying options. A double-blind RCT showed little benefit from the use of glucosamine combined with chondroitin in participants with mild knee osteoarthritis.15 However, a greater benefit was noted in persons with moderate to severe pain. Glucosamine is safe, but the benefit is variable. Chondroitin does not decrease pain from osteoarthritis of the knee or hip.15
The benefit of acupuncture is not clear. A meta-analysis did not demonstrate any clinically relevant improvement in pain or function scores with acupuncture compared with sham acupuncture.16 However, in the short term (six weeks) and in the long term (six months), patients who received either acupuncture or sham acupuncture felt better than those who received usual care. Another study showed that six months of treatment with traditional Chinese acupuncture decreased pain scores and increased functionality an average of 40 percent compared with sham acupuncture or no treatment.17
Supplementation with S-adenosylmethionine (SAM-e), ginger (Zingiber officinale), or turmeric (Curcuma longa) has also been promoted as treatment for osteoarthritis. A meta-analysis of RCTs found that SAM-e is as effective as NSAIDs in reducing pain and disability, and has a better safety profile.18 Ginger may provide some clinical benefit in patients with knee osteoarthritis; patients who took 255 mg of ginger extract twice daily had a reduction in pain (63 percent compared with 50 percent in the placebo group).19 Turmeric historically has been used to treat arthritis pain, but no clinical trials have shown it to be effective.20
PHARMACOLOGIC TREATMENT
Pharmacologic treatments can be categorized as topical, oral, or intra-articular. The use of topical therapies avoids many of the adverse effects associated with systemic medications. A review of placebo- controlled trials of capsaicin cream 0.025% (Zostrix) concluded that it was statistically more effective than placebo, but less effective than topical NSAIDs.21 A meta-analysis of RCTs compared topical NSAIDs with placebo or oral NSAIDs in patients with knee osteoarthritis.22 Topical NSAIDs were superior to placebo in relieving pain, but only for the first two weeks of treatment. Topical NSAIDs were less effective than oral NSAIDs, even in the first week of treatment.
Many oral medications are available for managing pain from knee osteoarthritis. Acetaminophen is the preferred drug in guidelines from the American College of Rheumatology.23 It is more effective than placebo in the treatment of osteoarthritis pain.24 Liver toxicity is extremely rare, although caution should be used in patients who consume alcohol daily. Patients taking 3 to 4 g of acetaminophen per day should have regular monitoring of kidney and liver function. NSAIDs are slightly superior to acetaminophen for improving knee and hip pain in patients with osteoarthritis, especially in those with moderate to severe pain.25 There is no difference in clinical effectiveness among NSAIDs.25
Cyclooxygenase-2 (COX-2) inhibitors may have a role in the treatment of osteoarthritis. Celecoxib (Celebrex) is the only prototype COX-2 inhibitor available because rofecoxib and valdecoxib have been withdrawn from the market because of adverse cardiovascular effects. However, celecoxib is also associated with an increased incidence of myocardial infarction and stroke.26 A systematic review showed that although the use of celecoxib results in similar symptom control as other NSAIDs and does not reduce the risk of serious adverse gastrointestinal effects, patients may be less likely to stop taking celecoxib because of gastrointestinal effects.27,28 Although there is no increased risk of adverse effects with the use of COX-2 inhibitors for treatment of osteoarthritis compared with other NSAIDs, there also may not be much benefit.
Opioids also may have a beneficial role in the treatment of knee osteoarthritis. Guidelines from the American College of Rheumatology support the use of opioid therapy when other treatments have been ineffective or are inappropriate.23 Tramadol (Ultram), with or without acetaminophen, decreases pain intensity, relieves symptoms, and improves function.29 Tramadol increases the risk of seizure, especially in patients who drink alcohol. A recent guideline from the American Geriatrics Society recommends that all older patients with moderate to severe pain or diminished quality of life be considered for opioid therapy.30 The risks of NSAID use in older patients, including increased cardiovascular risk and gastrointestinal toxicity, may exceed the potential for addiction in these patients. However, propoxyphene, which was taken off the market in November 2010, should be avoided because it is no more effective than acetaminophen and is associated with more adverse effects.31
INTRA-ARTICULAR INJECTIONS
Intra-articular corticosteroid injections may provide short-term symptomatic relief in patients with knee osteoarthritis, with low risk of adverse effects. A systematic review of 28 clinical trials found a significant short-term reduction in pain and improvement in patient self-assessment with intra-articular corticosteroid injection compared with placebo injection32; however, good evidence of long-term benefit is lacking. The precise mechanism of action is unknown, but corticosteroids are presumed to inhibit accumulation of inflammatory cell lines, reduce prostaglandin synthesis, inhibit leukocyte secretion from synovial cells, and decrease interleukin secretion by the synovium. A typical dose for knee injections is 40 mg of triamcinolone acetonide (Kenalog), with a number needed to treat of two or three.33
Intra-articular hyaluronic acid injections (e.g., Synvisc, Euflexxa) for osteoarthritis are minimally effective. Despite being promoted as potential disease-modifying agents, no study has demonstrated that these drugs alter the disease course. Synovial fluid is an ultrafiltrate of plasma modified by the addition of hyaluronic acid, which is produced by the synovium. In persons with osteoarthritis, the hyaluronic acid is decreased and compromised. Exogenous supplementation of intra-articular hyaluronic acid is thought to support and restore the elastoviscous properties of synovial fluid. However, a meta-analysis showed that studies demonstrating benefit from intra-articular hyaluronic acid injections were poorly designed or industry sponsored, whereas other studies demonstrated no clinically significant improvement in function.34
SURGERY
Arthroscopic surgery is not an appropriate treatment for knee osteoarthritis unless there is evidence of loose bodies or mechanical symptoms such as locking, giving way, or catching. Two well-designed RCTs of arthroscopic surgery for treatment of knee osteoarthritis showed no benefit.35,36
Total knee replacement should be considered as a last resort. According to the American Academy of Orthopedic Surgeons, the main indication for total knee arthroplasty is relief of pain associated with knee osteoarthritis if nonsurgical treatment has been ineffective. The complication rate of total knee replacement is 5.4 percent of patients and 7.6 percent of knees.37
Data Sources: A Medline search was performed, which included meta-analyses, randomized controlled trials, clinical trials, and systematic reviews. Also searched were the Cochrane Database of Systematic Reviews, UpToDate, the Centers for Disease Control and Prevention, and DynaMed. Search period: November 18, 2009, to September 1, 2010.

