In 2009, nearly 66 million Americans (three in 10 U.S. households) reported at least one person providing unpaid care as a family caregiver. More adults with chronic conditions and disabilities are living at home than ever before, and family caregivers have an even higher level of responsibility. Caring for loved ones is associated with several benefits, including personal fulfillment. However, caregiving is also associated with physical, psychological, and financial burdens. Primary care physicians can aid in the identification, support, and treatment of caregivers by offering caregiver assessments—interviews directed at identifying high levels of burden—as soon as caregivers are identified. Repeat assessments may be considered when there is a change in the status of caregiver or care recipient. Caregivers should be directed to appropriate resources for support, including national caregiving organizations, local area agencies on aging, Web sites, and respite care. Psychoeducational, skills-training, and therapeutic counseling interventions for caregivers of patients with chronic conditions such as dementia, cancer, stroke, and heart failure have shown small to moderate success in decreasing caregiver burden and increasing caregiver quality of life. Further research is needed to further identify strategies to offset caregiver stress, depression, and poor health outcomes. Additional support and anticipatory guidance for the care recipient and caregiver are particularly helpful during care transitions and at the care recipient's end of life.
A family caregiver is broadly defined as a friend or relative who provides unpaid assistance to a person with a chronic or disabling condition.1 In 2009, nearly 66 million Americans (three in 10 U.S. households) reported at least one person providing unpaid care as a family caregiver.1
Eighty percent of adults requiring long-term care currently live at home or in the community, and unpaid family caregivers provide 90 percent of their care.1,2 These caregivers fill an important role for their families and provide an estimated $375 billion in cost savings nationwide.3 Family caregivers serve as a critical extension of the formal health care system, and supporting family caregivers has recently emerged as a national public health priority.2,4
In the next few decades, the demand for family caregivers is expected to rise by 85 percent.2 This growing demand for caregivers is the result of several factors, including shorter hospital stays, changes in insurance reimbursement, limited hospital discharge planning, an increase in home care technology, and an aging U.S. population. By 2030, one in five adults will be 65 years or older.2
In addition to the growing demand for caregivers, family caregiving has been affected in several important ways over the past five years: caregivers and care recipients are older and have higher levels of disability than in years past; the duration, intensity, and burden of care has increased; the financial cost associated with informal caregiving has risen; and the use of paid formal care has declined significantly.5
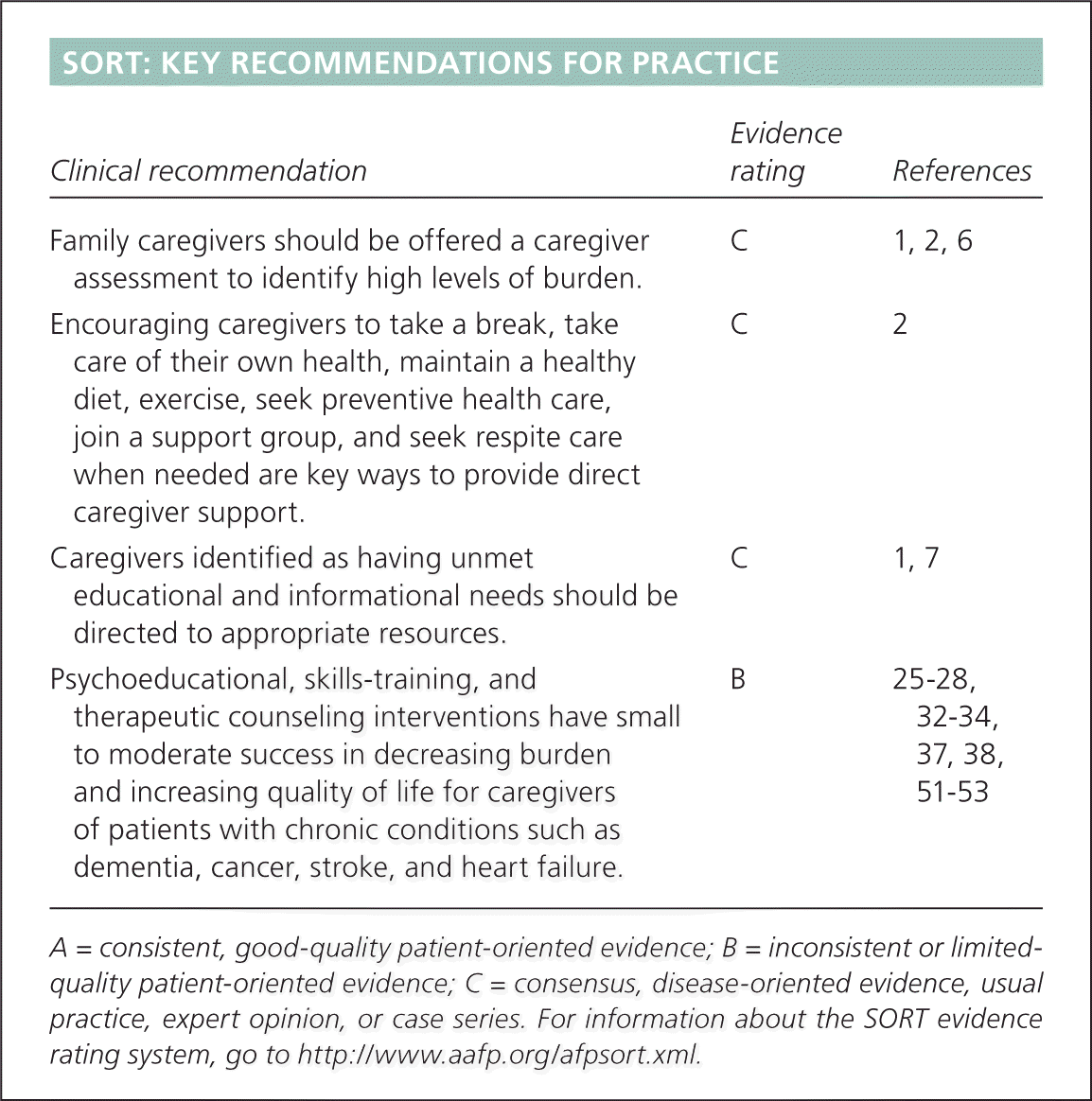
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Family caregivers should be offered a caregiver assessment to identify high levels of burden. | C | 1, 2, 6 |
| Encouraging caregivers to take a break, take care of their own health, maintain a healthy diet, exercise, seek preventive health care, join a support group, and seek respite care when needed are key ways to provide direct caregiver support. | C | 2 |
| Caregivers identified as having unmet educational and informational needs should be directed to appropriate resources. | C | 1, 7 |
| Psychoeducational, skills-training, and therapeutic counseling interventions have small to moderate success in decreasing burden and increasing quality of life for caregivers of patients with chronic conditions such as dementia, cancer, stroke, and heart failure. | B | 25–28, 32–34, 37, 38, 51–53 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Care Recipients and Caregivers
Care recipients are typically female and average 69 years of age. They are older and generally less healthy than in the past year. At least one-half of care recipients rely on their caregivers to help with one or more activities of daily living (e.g., bathing, dressing), and a majority require assistance with four or more instrumental activities of daily living (e.g., managing finances, shopping, taking medications).6 Seventy percent of care recipients have one or more chronic medical conditions.6
Family caregivers are typically women, often the daughter or spouse of the care recipient, and average 49 years of age.6 One-third of family caregivers have provided care for more than five years, and the majority provide 20 to 39 hours of unpaid caregiving each week.6
Caregiver Burden
Caring for loved ones has several benefits, including personal fulfillment and satisfaction from helping to relieve another's suffering.7 However, caregiving is also associated with physical, psychological, and financial burdens for caregivers. Stressors associated with caregiving situations are often persistent, uncontrollable, and unpredictable, with one-third of all caregivers describing a high burden of care.2 Caregivers reporting the highest burden are more likely to be less educated, to live with the care recipient, and to perceive they had no choice in assuming the caregiver role. A majority of caregivers report having less time for family and friends; having increased emotional stress; and neglecting self-care, such as healthy sleep, exercise, and dietary habits.2
HEALTH EFFECTS
One of the greatest risks for caregivers is becoming ill themselves.8 Caregivers have higher rates of insomnia and depression, are at risk of serious illness, and are less likely to engage in preventive health measures. One-half of all caregivers have at least one chronic condition.5,9,10 One in five caregivers describes his or her health as fair or poor, and 17 percent believe that their health has deteriorated as a result of providing care, particularly those who have been providing care for five or more years or who have shifted from light to heavy duty.2 Spousal caregivers reporting high levels of strain have a 23 percent higher Framingham Stroke Risk than their non-caregiver counterparts, as well as increased all-cause mortality (as high as 63 percent in four years).11,12 One-half of caregivers report that the decline in their own health compromises their ability to provide care for the care recipient.2
FINANCIAL BURDEN
Many caregivers adjust their work schedules, take leaves of absence, or reduce work hours as a result of care responsibilities. More than 40 percent of caregivers have an annual household income less than $50,000, yet a majority report spending their own money to take care of the care recipient; in 2007, average out-of-pocket expenses for caregivers was $5,531, representing approximately 10 percent of the caregiver's annual income.2,6 Additional costs include loss of salary and benefits, loss of promotional and training opportunities, and a reduction in retirement savings and Social Security benefits. Female caregivers who provide care for their parents are 2.5 times more likely than non-caregivers to live below the poverty level.5
INADEQUATE PREPARATION
A majority of caregivers (81 percent) feel inadequately trained for the skills that they perform, having never received any formal education in caregiving.5 The top unmet needs of caregivers include keeping care recipients safe at home, managing emotional and physical stress, finding easy activities to do with the recipient, and having enough time for themselves. A majority of caregivers report needing more information about support services (77 percent), and they are most likely to use the Internet (29 percent) or their doctors (28 percent) as primary sources of additional caregiving information.6 Therefore, primary care physicians are uniquely positioned to aid in the identification, support, and treatment of caregivers.
Caregiver Assessment
Caregiver assessment refers to a systematic process of gathering information about a caregiving situation to identify needs, strengths, and resources for the family caregiver. It can be performed by the caregiver's physician, if time permits, or by other health care team members, including a social worker or case manager.7 In 2005, the National Consensus Development Conference for Caregiver Assessment developed a set of guiding principles and practice guidelines, which have been promoted by numerous national organizations and incorporated into the Guided Care model as key components for chronic care delivery.1,5,7,13
According to these guidelines, caregiver assessment is a multidimensional process that should embrace a family-centered perspective and focus on ways to keep the caregiver on the job while promoting health and safety.5 It includes understanding the context in which the caregiver provides care and exploring the caregiver's perception of the care recipient's functional status, as well as the caregiver's values and preferences. Evaluation of caregivers should also include perception of their own well-being, perceived challenges and benefits of caregiving, confidence in their abilities, and the need for additional support systems. The findings from these assessments are used to develop a care plan and to identify appropriate support services.1
A complete assessment can be offered to any person who self-identifies as a caregiver. Because many do not self-identify, it may help to identify assessment candidates by describing caregivers as the care recipient's friends and family who provide assistance.13 Initial assessment may be performed as soon as a caregiver is identified, whereas repeat assessments can be offered as the care recipient's or caregiver's condition changes.1
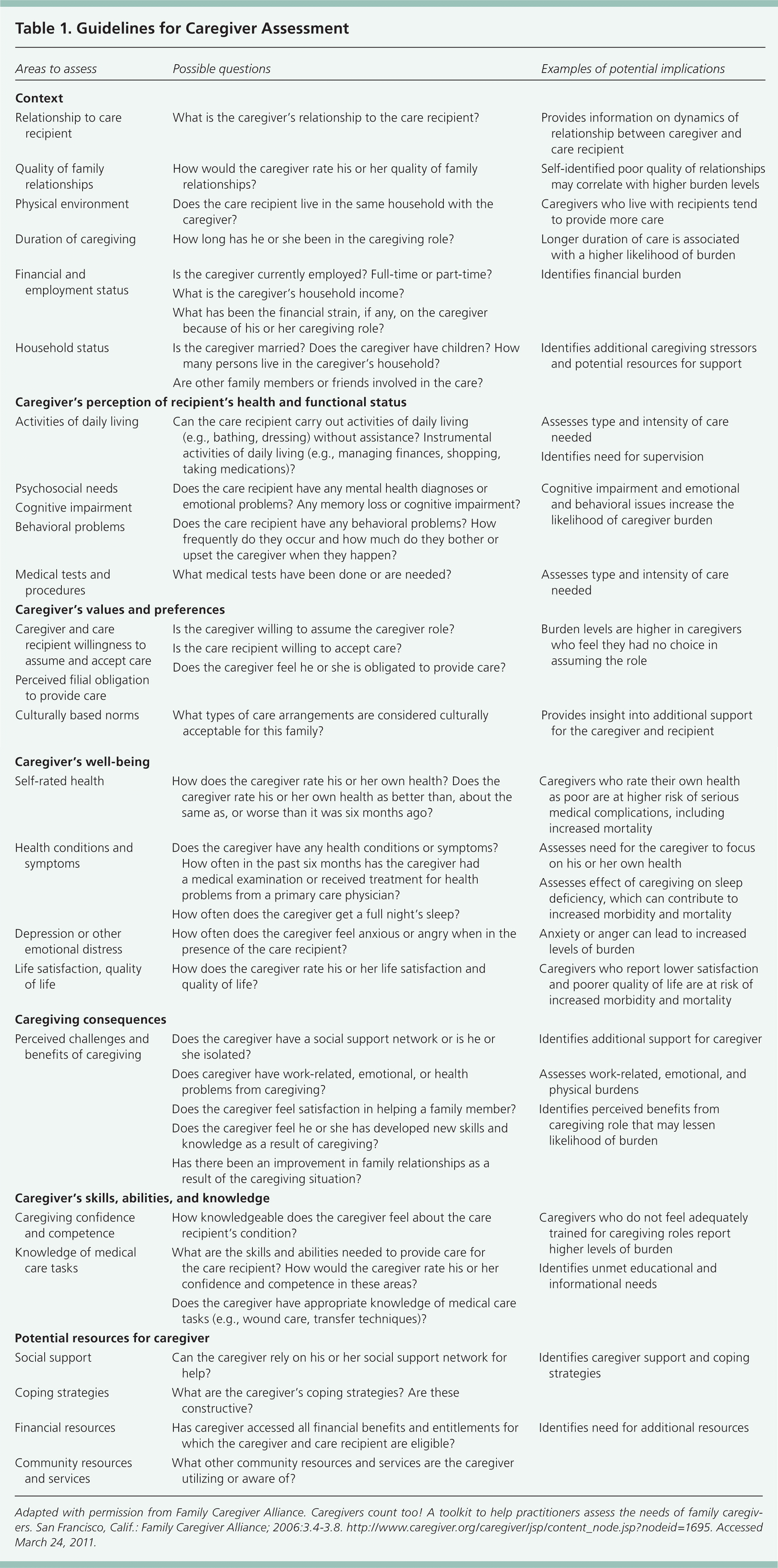
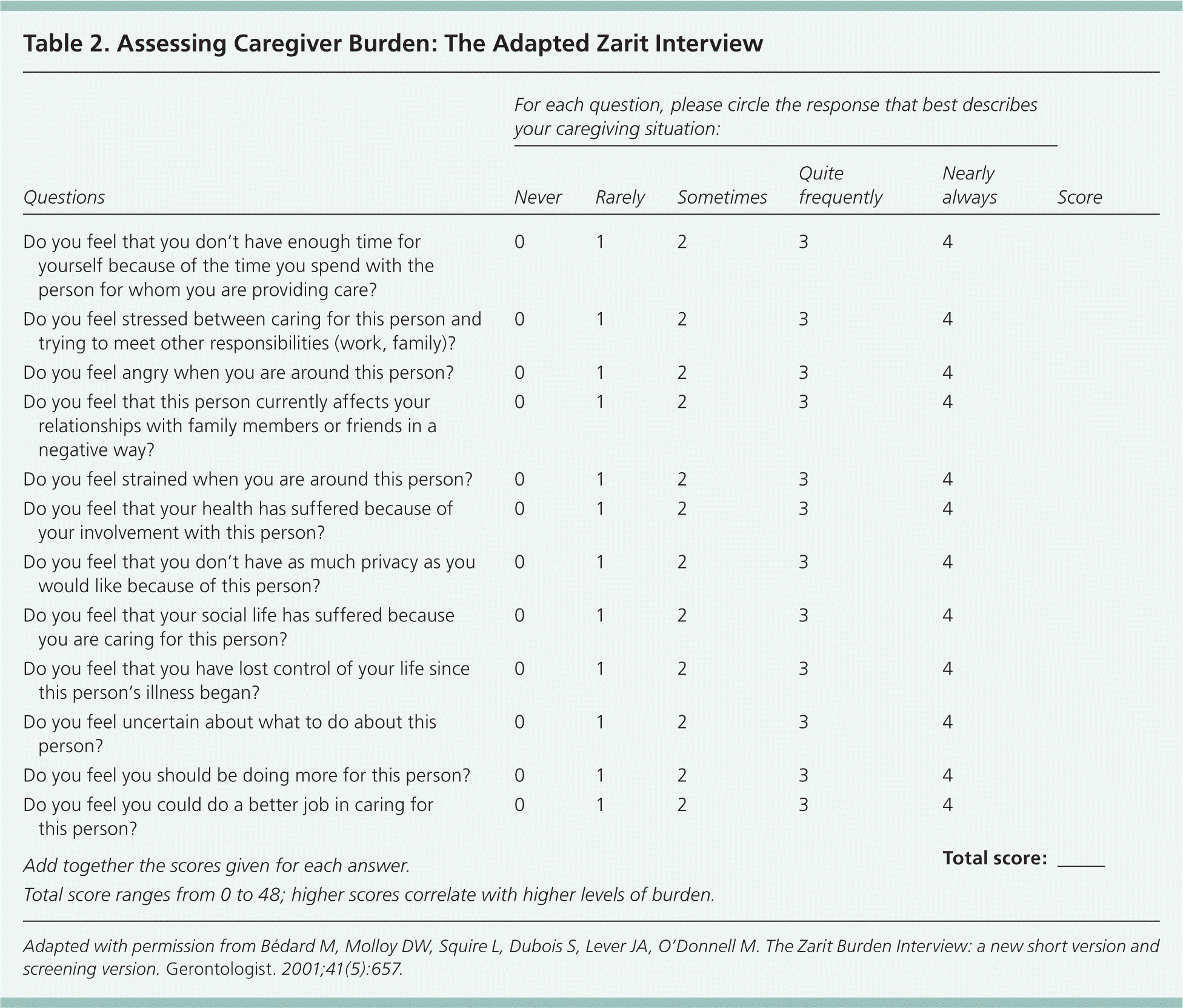
Physicians may only have time to identify caregivers during an office visit and may refer these persons for full assessments. Referrals for assessment may be triggered by a diagnosis of a medical condition associated with high burden for caregiving (e.g., dementia, heart failure, stroke, cancer), change in functional status of a caregiver or care recipient, or care transitions. Table 1 lists practical questions to include in the caregiver assessment.7 Additional practical tools for physicians are available from national organizations, including a toolkit from the Family Caregiver Alliance.7,14–17 A number of well-validated tools to specifically assess caregiver burden are also available, such as the Caregiver Burden Inventory18 and the Adapted Zarit Interview (Table 219 ).18–20
Table 1. Guidelines for Caregiver Assessment
| Areas to assess | Possible questions | Examples of potential implications | ||
|---|---|---|---|---|
| Context | ||||
| Relationship to care recipient | What is the caregiver's relationship to the care recipient? | Provides information on dynamics of relationship between caregiver and care recipient | ||
| Quality of family relationships | How would the caregiver rate his or her quality of family relationships? | Self-identified poor quality of relationships may correlate with higher burden levels | ||
| Physical environment | Does the care recipient live in the same household with the caregiver? | Caregivers who live with recipients tend to provide more care | ||
| Duration of caregiving | How long has he or she been in the caregiving role? | Longer duration of care is associated with a higher likelihood of burden | ||
| Financial and employment status | Is the caregiver currently employed? Full-time or part-time? | Identifies financial burden | ||
| What is the caregiver's household income? | ||||
| What has been the financial strain, if any, on the caregiver because of his or her caregiving role? | ||||
| Household status | Is the caregiver married? Does the caregiver have children? How many persons live in the caregiver's household? | Identifies additional caregiving stressors and potential resources for support | ||
| Are other family members or friends involved in the care? | ||||
| Caregiver's perception of recipient's health and functional status | ||||
| Activities of daily living | Can the care recipient carry out activities of daily living (e.g., bathing, dressing) without assistance? Instrumental activities of daily living (e.g., managing finances, shopping, taking medications)? | Assesses type and intensity of care needed | ||
| Identifies need for supervision | ||||
| Psychosocial needs Cognitive impairment Behavioral problems | Does the care recipient have any mental health diagnoses or emotional problems? Any memory loss or cognitive impairment? | Cognitive impairment and emotional and behavioral issues increase the likelihood of caregiver burden | ||
| Does the care recipient have any behavioral problems? How frequently do they occur and how much do they bother or upset the caregiver when they happen? | ||||
| Medical tests and procedures | What medical tests have been done or are needed? | Assesses type and intensity of care needed | ||
| Caregiver's values and preferences | ||||
| Caregiver and care recipient willingness to assume and accept care Perceived filial obligation to provide care | Is the caregiver willing to assume the caregiver role? | Burden levels are higher in caregivers who feel they had no choice in assuming the role | ||
| Is the care recipient willing to accept care? | ||||
| Does the caregiver feel he or she is obligated to provide care? | ||||
| Culturally based norms | What types of care arrangements are considered culturally acceptable for this family? | Provides insight into additional support for the caregiver and recipient | ||
| Caregiver's well-being | ||||
| Self-rated health | How does the caregiver rate his or her own health? Does the caregiver rate his or her own health as better than, about the same as, or worse than it was six months ago? | Caregivers who rate their own health as poor are at higher risk of serious medical complications, including increased mortality | ||
| Health conditions and symptoms | Does the caregiver have any health conditions or symptoms? How often in the past six months has the caregiver had a medical examination or received treatment for health problems from a primary care physician? How often does the caregiver get a full night's sleep? | Assesses need for the caregiver to focus on his or her own health Assesses effect of caregiving on sleep deficiency, which can contribute to increased morbidity and mortality | ||
| Depression or other emotional distress | How often does the caregiver feel anxious or angry when in the presence of the care recipient? | Anxiety or anger can lead to increased levels of burden | ||
| Life satisfaction, quality of life | How does the caregiver rate his or her life satisfaction and quality of life? | Caregivers who report lower satisfaction and poorer quality of life are at risk of increased morbidity and mortality | ||
| Caregiving consequences | ||||
| Perceived challenges and benefits of caregiving | Does the caregiver have a social support network or is he or she isolated? | Identifies additional support for caregiver | ||
| Does caregiver have work-related, emotional, or health problems from caregiving? | Assesses work-related, emotional, and physical burdens | |||
| Does the caregiver feel satisfaction in helping a family member? | Identifies perceived benefits from caregiving role that may lessen likelihood of burden | |||
| Does the caregiver feel he or she has developed new skills and knowledge as a result of caregiving? | ||||
| Has there been an improvement in family relationships as a result of the caregiving situation? | ||||
| Caregiver's skills, abilities, and knowledge | ||||
| Caregiving confidence and competence | How knowledgeable does the caregiver feel about the care recipient's condition? | Caregivers who do not feel adequately trained for caregiving roles report higher levels of burden Identifies unmet educational and informational needs | ||
| Knowledge of medical care tasks | What are the skills and abilities needed to provide care for the care recipient? How would the caregiver rate his or her confidence and competence in these areas? | |||
| Does the caregiver have appropriate knowledge of medical care tasks (e.g., wound care, transfer techniques)? | ||||
| Potential resources for caregiver | ||||
| Social support | Can the caregiver rely on his or her social support network for help? | Identifies caregiver support and coping strategies | ||
| Coping strategies | What are the caregiver's coping strategies? Are these constructive? | |||
| Financial resources | Has caregiver accessed all financial benefits and entitlements for which the caregiver and care recipient are eligible? | Identifies need for additional resources | ||
| Community resources and services | What other community resources and services are the caregiver utilizing or aware of? | |||
Adapted with permission from Family Caregiver Alliance. Caregivers count too! A toolkit to help practitioners assess the needs of family caregivers. San Francisco, Calif.: Family Caregiver Alliance; 2006:3.4–3.8. http://www.caregiver.org/caregiver/jsp/content_node.jsp?nodeid=1695. Accessed March 24, 2011.
Table 2. Assessing Caregiver Burden: The Adapted Zarit Interview
| Questions | For each question, please circle the response that best describes your caregiving situation: | |||||
|---|---|---|---|---|---|---|
| Never | Rarely | Sometimes | Quite frequently | Nearly always | Score | |
| Do you feel that you don't have enough time for yourself because of the time you spend with the person for whom you are providing care? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel stressed between caring for this person and trying to meet other responsibilities (work, family)? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel angry when you are around this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel that this person currently affects your relationships with family members or friends in a negative way? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel strained when you are around this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel that your health has suffered because of your involvement with this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel that you don't have as much privacy as you would like because of this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel that your social life has suffered because you are caring for this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel that you have lost control of your life since this person's illness began? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel uncertain about what to do about this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel you should be doing more for this person? | 0 | 1 | 2 | 3 | 4 | |
| Do you feel you could do a better job in caring for this person? | 0 | 1 | 2 | 3 | 4 | |
| Add together the scores given for each answer. | Total score:____ | |||||
| Total score ranges from 0 to 48; higher scores correlate with higher levels of burden. | ||||||
Adapted with permission from Bédard M, Molloy DW, Squire L, Dubois S, Lever JA, O'Donnell M. The Zarit Burden Interview: a new short version and screening version. Gerontologist. 2001;41(5):657.
Office-based assessment of the patient-caregiver dyad can provide unique ethical and communication challenges. While attempting to preserve patient autonomy and privacy, the physician also needs to validate the caregiver's role as a member of the care team and help to resolve potential conflicts between the needs and rights of the care recipient and those of the caregiver.2 It is important to maintain communication and coordination among the care recipient, caregiver, and care agencies.
Supporting Caregivers
Encouraging caregivers to take breaks, take care of their own health, maintain a healthy diet, exercise, seek preventive health care, join a support group, and locate respite care when needed are key ways to provide direct caregiver support.2 Physicians can also identify coping strategies, such as praying (73 percent), talking with friends and family (61 percent), and obtaining additional information from books or Web sites (44 percent).7 Caregivers identified as having unmet educational and informational needs should be directed to appropriate resources, such as national caregiving organizations, Web sites for additional training, and respite care services.1,7 Practical online resource locators (e.g., Eldercare Locator, Family Care Navigator) and online toolkits, such as a planning guide from the AARP,21 can be easily accessed and provided during an office visit.21–23 Table 3 provides a list of caregiver resources available online.
Table 3. Online Resources for Caregivers

| Caregiving | |
| AARP: http://www.aarp.org/families/caregiving | |
| American Red Cross Family Caregiver Program: http://www.redcross.org/ | |
| American Society on Aging: http://www.asaging.org/caregiving_resources.cfm | |
| Caring Today magazine: http://www.caringtoday.com | |
| Empower Online, Mather LifeWays Institute on Aging: http://matherlifeways.com/re_ptc.asp | |
| Family Caregiver Alliance: http://www.caregiver.org | |
| National Alliance for Caregiving: http://www.caregiving.org | |
| National Family Caregivers Association: http://www.nfcacares.org | |
| National Family Caregiver Support Program, Administration on Aging: http://www.aoa.gov/aoaroot/aoa_programs/hcltc/caregiver | |
| National Institute on Aging: http://www.niapublications.org | |
| Next Step in Care, United Hospital Fund: http://www.nextstepincare.org | |
| Rosalynn Carter Institute for Caregiving: http://rci.gsw.edu | |
| Disease-specific caregiving | |
| Cancer | |
| American Cancer Society: http://www.cancer.org/Treatment/Caregivers | |
| CancerCare: http://www.cancercare.org/get_help/special_progs/caregivers.php | |
| National Cancer Institute: http://www.cancer.gov/cancertopics/coping/familyfriends | |
| Dementia | |
| Alzheimer's Association: http://www.alz.org/living_with_alzheimers_caring_for_alzheimers.asp | |
| Alzheimer's Disease Education and Referral Center, National Institute on Aging: http://www.nia.nih.gov/Alzheimers/Caregiving/ | |
| Heart failure | |
| American Heart Association: http://www.heart.org/HEARTORG/Caregiver/Caregiver_UCM_001103_SubHomePage.jsp | |
| Heart Failure Society of America: http://www.hfsa.org/ | |
| Stroke | |
| American Heart Association and American Stroke Association: http://www.strokeassociation.org/ | |
| National Institute of Neurological Disorders and Stroke: http://www.ninds.nih.gov | |
| National Stroke Association: http://www.stroke.org/site/PageServer?pagename=care | |
| Resource locators | |
| Eldercare Locator, Administration on Aging: http://www.eldercare.gov | |
| Family Care Navigator, Family Caregiver Alliance: http://www.caregiver.org/caregiver/jsp/fcn_content_node.jsp?nodeid=2083 | |
| Paying for Senior Care: http://www.payingforseniorcare.com | |
| Respite care | |
| ARCH National Respite Network: http://www.archrespite.org | |
| Family Caregiver Alliance Camps for Caring: http://www.caregiver.org/caregiver/jsp/content_node.jsp?nodeid=2427 | |
| Training and education | |
| AssistGuide Information Services, AGIS Caregiver Kit: http://www.agis.com/caregiverkit | |
| Family Caregiver Alliance workshops, classes, and retreats: http://www.caregiver.org/caregiver/jsp/content_node.jsp?nodeid=2432 | |
| National Registry of Evidence-based Programs and Practices, New York University Caregiver Intervention: http://www.nrepp.samhsa.gov/ViewIntervention.aspx?id=74 | |
| Powerful Tools for Caregivers, Legacy Health: http://www.legacyhealth.org/body.cfm?id=690 | |
| Prepare to Care: A Planning Guide for Families, AARP Foundation: http://assets.aarp.org/www.aarp.org_/articles/foundation/aa66r2_care.pdf | |
CAREGIVER INTERVENTIONS AND INNOVATIONS
Evidence suggests that when patients and caregivers are treated as a dyad, outcomes for both are improved.24 Recent research has identified a number of successful models of caregiver interventions. These interventions come in a variety of formats, from universal, community-based interventions to illness-specific, individualized interventions.5 In a meta-analysis of 78 caregiver interventions targeting caregivers of older adults, psychoeducational and psychotherapeutic interventions had the most consistent effects on all outcome measures.25 Studies about caregivers of persons with dementia and other chronic illnesses have demonstrated significant effect sizes from caregiver interventions.25–27 A 2010 meta-analysis that included 29 randomized controlled trials (RCTs) of interventions designed to support caregivers of patients with cancer found that psychoeducational, skills-training, and therapeutic counseling interventions reduced caregiver burden and increased caregiver self-efficacy, quality of life, and coping skills with small to moderate effect sizes.28 However, these interventions did not reduce caregiver depression.
Caregiver care is improved by offering innovations in self-management, decision support, information systems, and delivery redesign. One important advance in caregiving is the increased use of high-tech home health care, Web-based technology, and assistive technology. Nearly one-half of caregivers use some form of technology to improve the quality of the care they provide.5 Examples of new tools include Internet-based solutions such as the Comprehensive Health Enhancement Support System and Link2Care, which have resulted in increased delivery of information to family caregivers, decreased depression, and increased sense of social support.29,30 Other tools include home telemedicine, telehealth, and disease-state monitoring systems, which can transmit data on health status to base stations. Devices such as automatic medication dispensers, vibrating alarm watches, scooters, and lifting systems can also relieve caregiver burden and improve the safety of the care recipient at home.
Special Caregiving Scenarios
CANCER
Because of changes in the health care system and insurance reimbursement, much of cancer care is now provided at home.31 More than 50 percent of caregivers of persons with cancer provide care for patients with metastatic disease or severe comorbidities who are undergoing treatment, yet these caregivers receive little formal training, information, or support.31 Family caregivers of patients with cancer report high levels of depression, often higher than their care recipients.32 Information for these caregivers is available online through national organizations (Table 3).
In a 2006 RCT of 354 family caregivers of persons with advanced cancer, a coping-skills intervention led to significantly improved quality of life and decreased caregiver burden.33 A 2010 meta-analysis of 29 RCTs assessed psychoeducational, skills-training, and therapeutic counseling interventions in caregivers of persons with cancer, and results showed small to medium effects in decreasing cancer burden and increasing coping skills, self-efficacy, and quality of life.28 Given the high level of responsibility and the generally low level of training for these unpaid caregivers, additional research is needed to implement these evidence-based interventions.32,34
DEMENTIA
More than 25 percent of caregivers provide care for someone with cognitive impairment.35 Caregiving for a person with dementia is associated with high levels of strain caused by associated behavioral disturbances, intense physical needs, and need for constant vigilance. High strain has been identified as a predictor of long-term care placement.35,36 Therefore, physicians need to identify these caregivers early and provide appropriate support. Fact sheets from the Family Caregiver Alliance are free, easy to download, and provide practical guidance to caregivers on topics such as understanding dementia behaviors, finding community care options, controlling frustration, and maintaining self-care (http://www.caregiver.org/caregiver/jsp/publications.jsp?nodeid=345).
Evidence supporting interventions that target caregivers of persons with dementia has become more robust in the past decade.37,38 Examples of effective interventions in RCTs directed at these caregivers include the Tailored Activity Program, Resources for Enhancing Alzheimer's Caregiver Health, and the Adult Day Services Plus program.39–46 A 2006 meta-analysis of 127 RCTs with interventions targeting caregivers of persons with dementia demonstrated a small to medium effect on caregiver burden, depression, well-being, and coping skills.38 Psychoeducational interventions that involve active participation of caregivers demonstrate the broadest effects on caregiving domains, and multicomponent interventions reduce the risk of institutionalization.37,38
HEART FAILURE
Caregivers of patients with heart failure report similar problems as those caring for patients with other chronic illnesses.47 However, patients with heart failure often have frequent exacerbations requiring hospitalization, which can increase caregiver strain. These caregivers report that the most burdensome aspects of care are enforcing dietary restriction and adherence, as well as monitoring for signs and symptoms of heart failure.47,48 A growing number of multidisciplinary team interventions that target patient and caregiver education and include technologic innovations such as home telemonitoring are effective in decreasing hospital readmissions and caregiver burden; however, many of these programs are not yet widely available.
STROKE
Advances in stroke care have decreased the rate of severe disabilities among stroke survivors, allowing more stroke survivors to live at home. However, these patients often require significant assistance with activities of daily living and instrumental activities of daily living. The prevalence of caregiver burden ranges from 25 to 54 percent.49 Physical care activities, particularly assistance with toileting, mood disturbances, and memory deficits, cause significant emotional stress in caregivers of stroke survivors.50 However, caregiver interventions providing education, emotional support, and access to services have been nonsignificant or have shown only modest effects on caregiver burden.51,52 A 2010 systematic review of 117 studies of longitudinal family stroke care found that caregiver stress, depression, and health measures did not change significantly across the selected cross-sectional studies.53 Given the higher stress levels associated with care-recipient depression and anxiety, interventions to target these comorbidities as part of post-stroke caregiving are still needed.
TRANSITIONS IN CARE
Many caregivers experience a decrease in depression symptoms after the death of a care recipient, perhaps marking the end of the care recipient's suffering. The placement of a care recipient into a long-term care facility is not associated with positive effects and may be accompanied by an increase in caregiver anxiety.54 To ease these care transitions, primary care physicians can provide anticipatory guidance, assistance with advance care planning, and appropriate resources for respite, long-term, and end-of-life care.41,46,55,56
Public Policy
Providing optimal care for the care recipient and caregiver mandates an understanding of financial reimbursement strategies for caregivers. In 2000, the Older Americans Act passed the National Family Caregiver Support Program, the first federally funded program to formally recognize caregivers. However, in 2009, the program received only $154 million in federal funding, approximately one-twentieth of 1 percent of the value of caregiver contributions.2 Additional funding for caregiver services is available from the Family Medical Leave Act, the Department of Veterans Affairs programs, the Centers for Medicare and Medicaid Services' home and community-based care programs, Program of All-inclusive Care for the Elderly, respite care, and selected adult day care services. Fifteen states now have Cash and Counseling programs in which Medicaid beneficiaries with a disability can receive cash vouchers to pay family members who provide caregiving.5 Despite these new programs, caregiver funding remains insufficient and varies among states.
Accommodations in the workplace, including flexible scheduling and telecommuting, are important ways that employers can respond to caregivers' needs. New strategies of financial reimbursement for providing caregiver support in the office also need to be implemented and may be a part of health care reform via the patient-centered medical home. Obtaining additional funding for caregiving resources is an urgent national public health issue.

