Lichen planus is a chronic, inflammatory, autoimmune disease that affects the skin, oral mucosa, genital mucosa, scalp, and nails. Lichen planus lesions are described using the six P's (planar [flat-topped], purple, polygonal, pruritic, papules, plaques). Onset is usually acute, affecting the flexor surfaces of the wrists, forearms, and legs. The lesions are often covered by lacy, reticular, white lines known as Wickham striae. Classic cases of lichen planus may be diagnosed clinically, but a 4-mm punch biopsy is often helpful and is required for more atypical cases. High-potency topical corticosteroids are first-line therapy for all forms of lichen planus, including cutaneous, genital, and mucosal erosive lesions. In addition to clobetasol, topical tacrolimus appears to be an effective treatment for vulvovaginal lichen planus. Topical corticosteroids are also first-line therapy for mucosal erosive lichen planus. Systemic corticosteroids should be considered for severe, widespread lichen planus involving oral, cutaneous, or genital sites. Referral to a dermatologist for systemic therapy with acitretin (an expensive and toxic oral retinoid) or an oral immunosuppressant should be considered for patients with severe lichen planus that does not respond to topical treatment. Lichen planus may resolve spontaneously within one to two years, although recurrences are common. However, lichen planus on mucous membranes may be more persistent and resistant to treatment.
Lichen planus is a chronic, inflammatory, autoimmune disease1 occurring in 0.1 to 4 percent of the general population, most often in perimenopausal women.2 Lichen planus can appear at any age, but most cases occur between 30 and 60 years of age.2
Pathophysiology
Although the exact etiology of lichen planus is unknown, an immune-mediated pathogenesis is recognized.1 A meta-analysis of primarily case-control studies conducted in multiple countries found a statistically significant association between hepatitis C virus (HCV) infection and lichen planus,3 although there is no known explanation for this association. Compared with the control group, patients with lichen planus had a greater prevalence of HCV exposure (odds ratio = 5.4; 95% confidence interval, 3.5 to 8.3), and patients with HCV infection had an increased prevalence of lichen planus (odds ratio = 2.5; 95% confidence interval, 2.0 to 3.1).3 It is appropriate to screen all patients with lichen planus for HCV infection.4 Patients should be asked about HCV risk factors, and liver enzyme and HCV antibody tests should be ordered.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
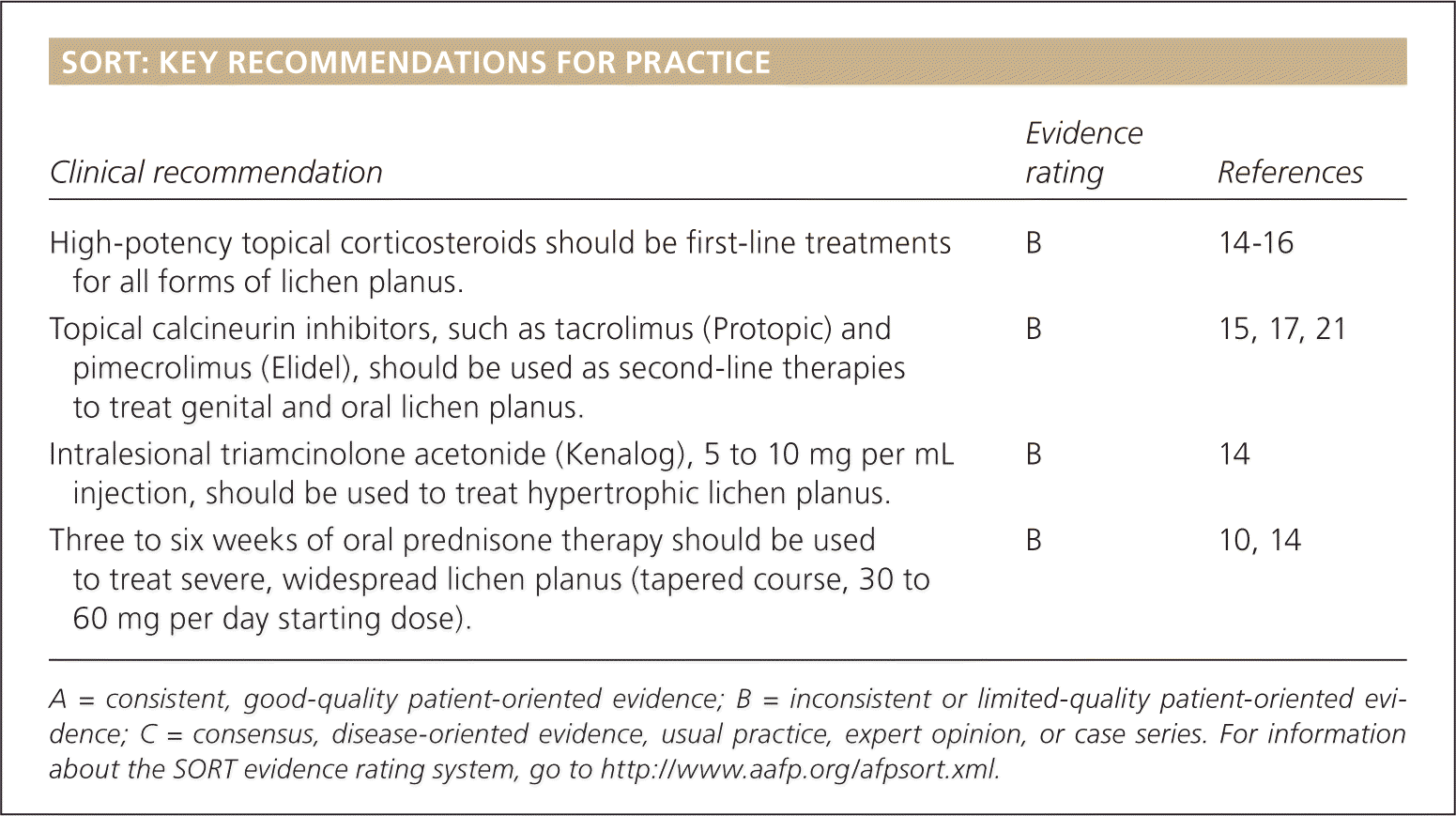
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| High-potency topical corticosteroids should be first-line treatments for all forms of lichen planus. | B | 14–16 |
| Topical calcineurin inhibitors, such as tacrolimus (Protopic) and pimecrolimus (Elidel), should be used as second-line therapies to treat genital and oral lichen planus. | B | 15, 17, 21 |
| Intralesional triamcinolone acetonide (Kenalog), 5 to 10 mg per mL injection, should be used to treat hypertrophic lichen planus. | B | 14 |
| Three to six weeks of oral prednisone therapy should be used to treat severe, widespread lichen planus (tapered course, 30 to 60 mg per day starting dose). | B | 10, 14 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Clinical Presentation
Lichen planus lesions are described using the six P's (Table 1). Onset is usually acute, affecting the flexor surfaces of the wrists (Figure 15 ), forearms, and legs. These lesions are often covered by lacy, reticular, white lines known as Wickham striae (Figure 25 ). The lesions may appear in a linear configuration, following the lines of trauma (Koebner phenomenon; Figure 3). It is common to see post-inflammatory hyperpigmentation as the cutaneous lesions clear, especially in persons with darker skin. Although lichen planus often occurs only on cutaneous surfaces, it may also involve the oral mucosa, genital mucosa, scalp, or nails.6
Table 1. The Six P's to Describe Lichen Planus Lesions

| Planar (flat-topped) |
| Purple |
| Polygonal |
| Pruritic |
| Papules |
| Plaques |
Figure 1.
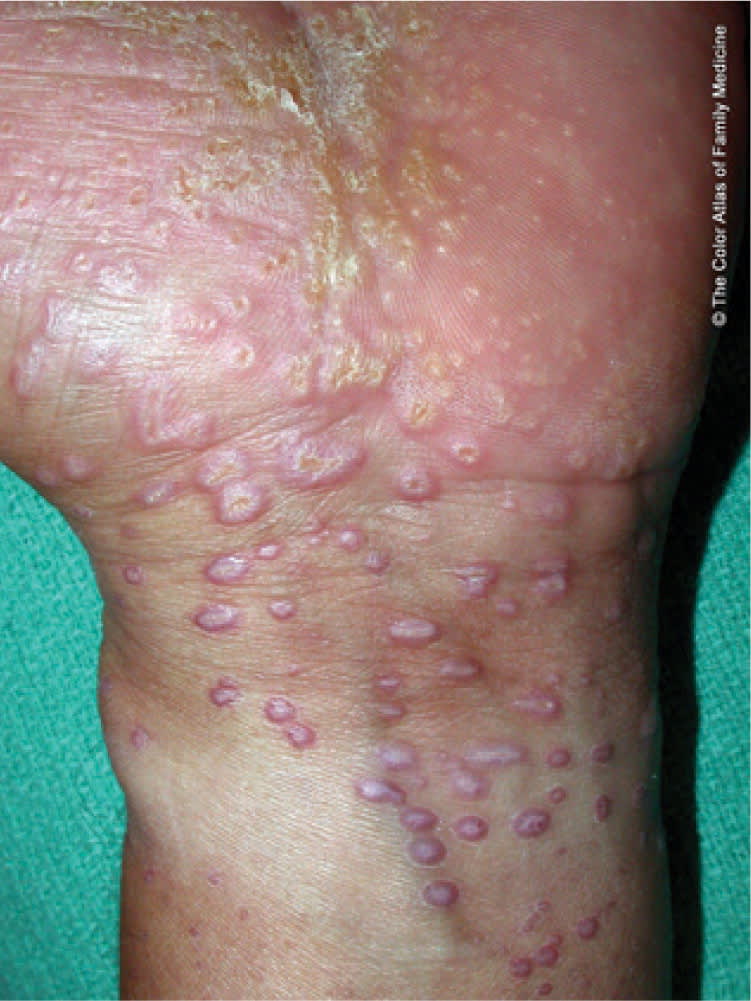
Lichen planus with papules and plaques on the wrist.
Reprinted with permission from Kraft R, Usatine RP. Lichen planus. In: The Color Atlas of Family Medicine. Usatine RP, Smith MA, Chumley H, Mayeaux EJ Jr., Tysinger J, eds. New York, NY: McGraw-Hill; 2009:638.
Figure 2.
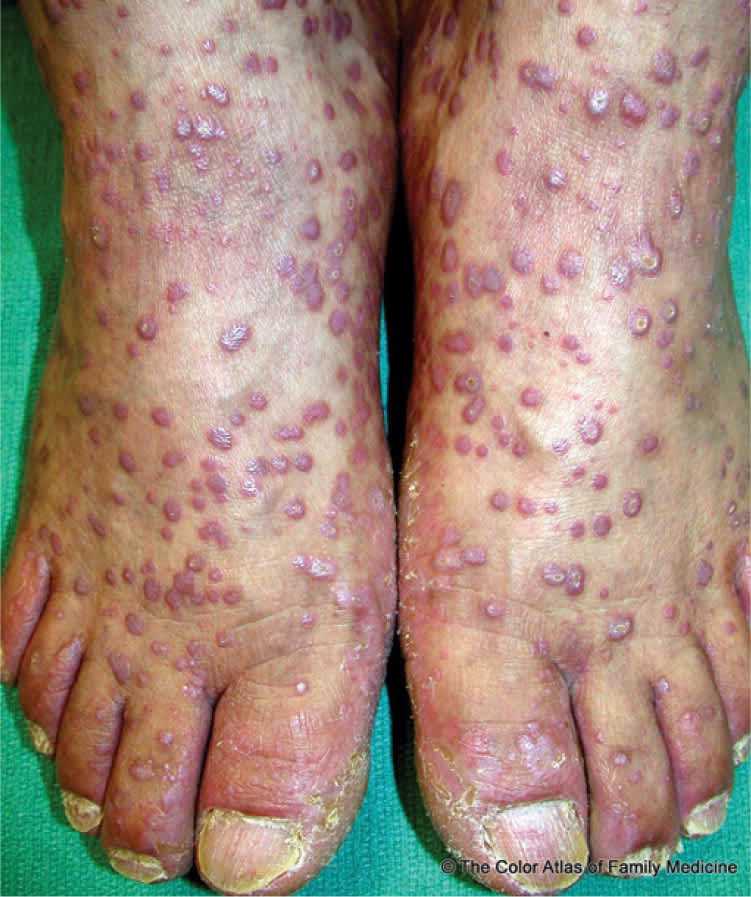
Lichen planus on the feet. The reticular white scale of Wickham striae is visible on some of the plaques.
Reprinted with permission from Kraft R, Usatine RP. Lichen planus. In: The Color Atlas of Family Medicine. Usatine RP, Smith MA, Chumley H, Mayeaux EJ Jr., Tysinger J, eds. New York, NY: McGraw-Hill; 2009:637.
Figure 3.
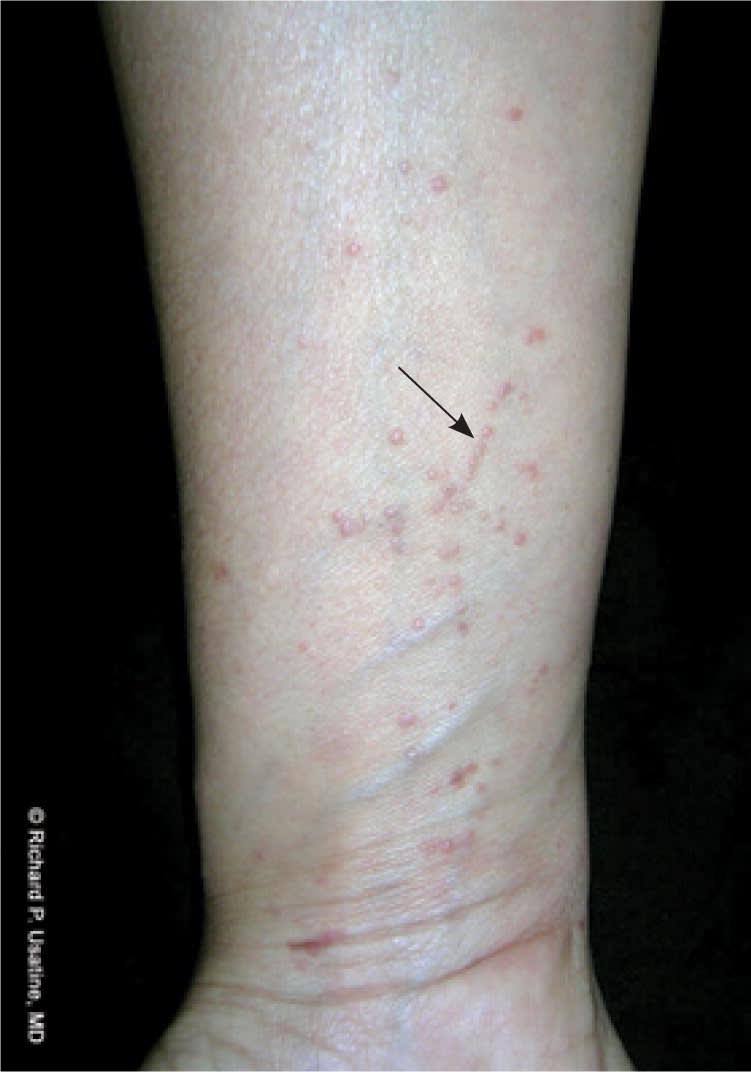
Lichen planus on the wrist showing the Koebner phenomenon (arrow) with linear formations of papules.
Copyright © Richard P. Usatine, MD
Cutaneous lichen planus may present in different forms. Linear lichen planus (Figure 3) manifests as closely aggregated linear lesions on the limbs that may develop the Koebner phenomenon. Annular lichen planus (Figure 4) accounts for approximately 10 percent of lichen planus cases.7 It commonly appears as arcuate groupings of individual papules that develop rings or a peripheral extension of clustered papules with central clearing. In addition to the usual sites of distribution, this form of lichen planus may occur on male genitalia and buccal mucosa.7 Atrophic lichen planus (Figure 5) is a rare form that is characterized by a few well-demarcated white, pink, or bluish papules, patches, or plaques with superficial atrophy. Hypertrophic lichen planus (lichen planus verrucosus; Figure 6) usually occurs on the extremities, especially the ankles, shins, and interphalangeal joints, and it tends to be the most pruritic form.7 It is often chronic with residual scarring and pigmentation when lesions clear. In vesiculobullous lichen planus (Figure 7), vesicles or bullae develop from preexisting lesions on the lower limbs, back, or buttocks, or in the mouth. Erosive/ulcerative lichen planus lesions develop within oral lesions or start as waxy semitranslucent plaques on the soles.8
Figure 4.
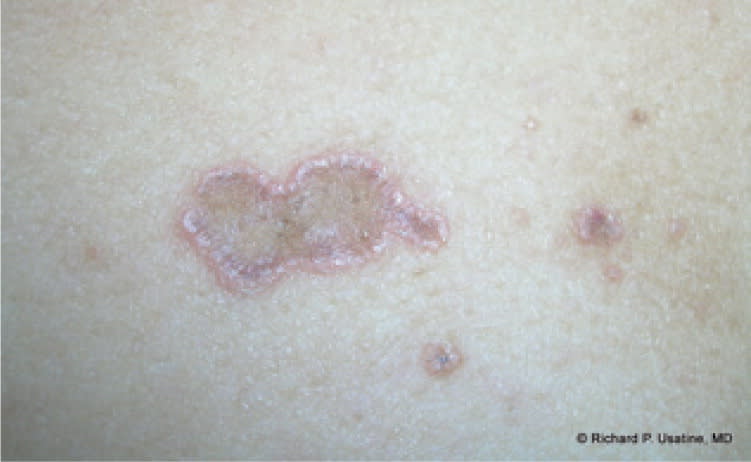
Annular lichen planus on the breast.
Copyright © Richard P. Usatine, MD
Figure 5.
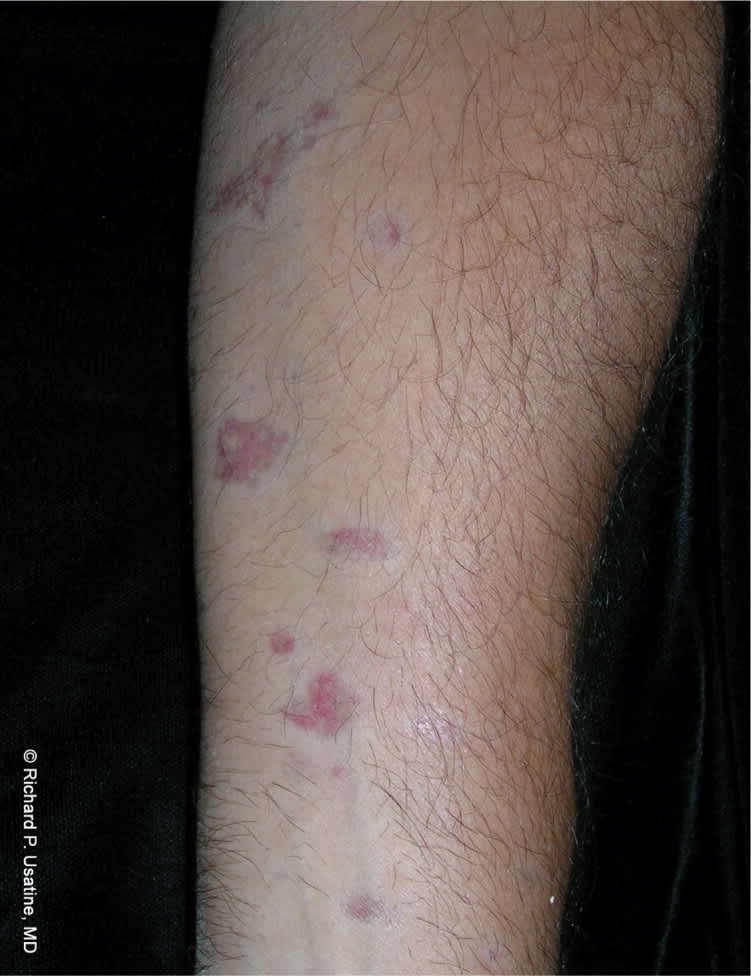
Atrophic lichen planus on the forearm showing multiple colors within the atrophic lesions.
Copyright © Richard P. Usatine, MD
Figure 6.
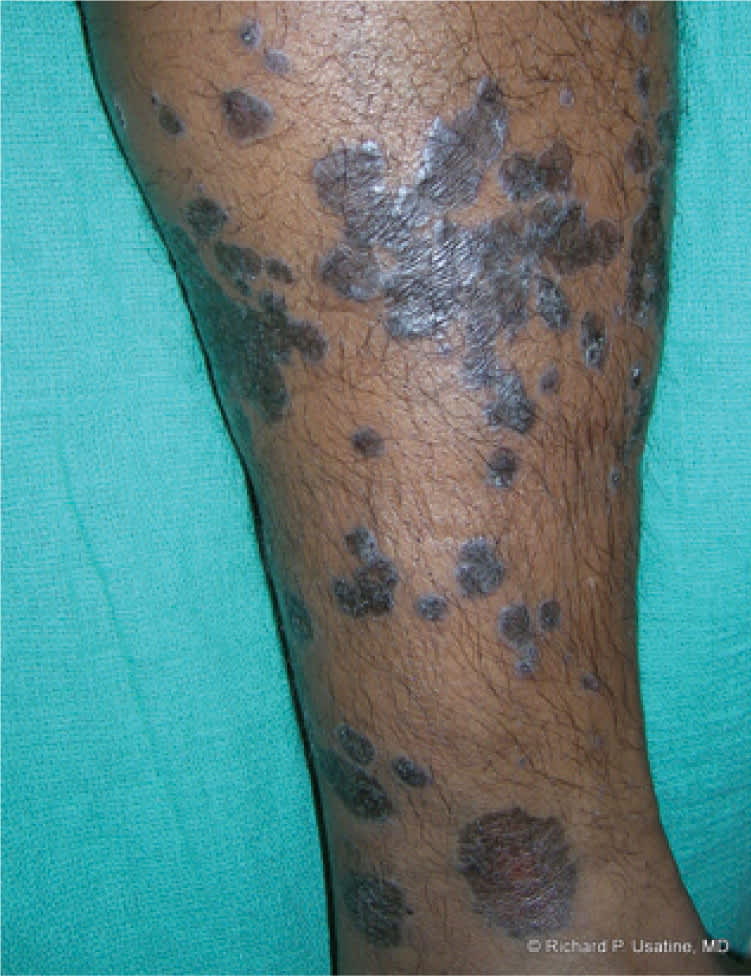
Hypertrophic lichen planus on the leg.
Copyright © Richard P. Usatine, MD
Figure 7.
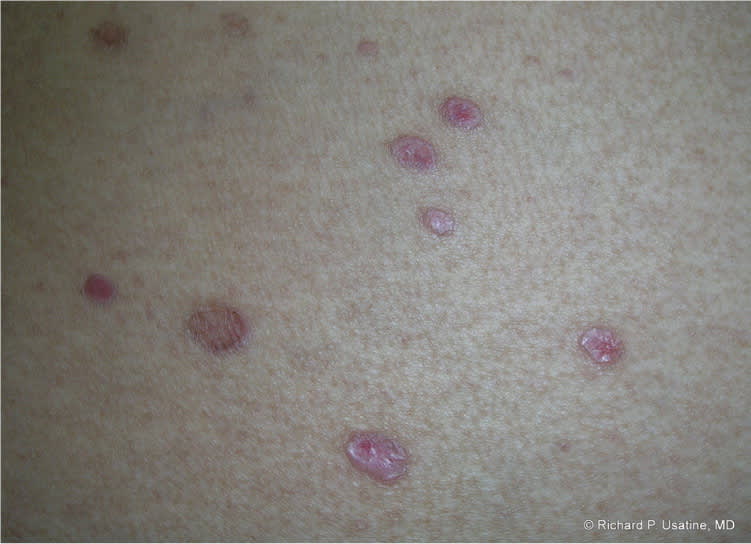
Bullous lichen planus on the buttocks.
Copyright © Richard P. Usatine, MD
Patients with oral lichen planus often have concomitant manifestations in other extraoral sites.1 A study showed that the vulva and vagina were also affected in approximately 25 percent of patients with oral lichen planus; involvement of the nails, scalp, esophagus, or eyes was less common.8 Oral lichen planus lesions are often asymptomatic. However, the condition is occasionally complicated by extensive painful erosions, leading to a considerable decrease in quality of life. Sensitivity to heat and a burning sensation may also occur. Intensive therapy is often required to reduce these complications.9
There are four forms of oral lichen planus: reticular, atrophic, bullous, and erosive.6 The reticular form is most common and manifests as bilateral, asymptomatic Wickham striae on the oral mucosa (Figure 8) or other parts of the mouth, such as the gingiva, tongue, palate, and lips (Figure 95 ). The atrophic form causes atrophic changes with erythema of the oral mucosa. The bullous form manifests as fluid-filled vesicles. The erosive form leads to ulcerated, painful, erythematous areas that may contract secondary infection, such as candidiasis. These ulcerated areas may have Wickham striae and occur in one or multiple sites of the mouth. Erosive lichen planus of the gums resembles desquamative gingivitis. Malignant transformation has been reported in men with oral erosive lichen planus lesions.10
Figure 8.
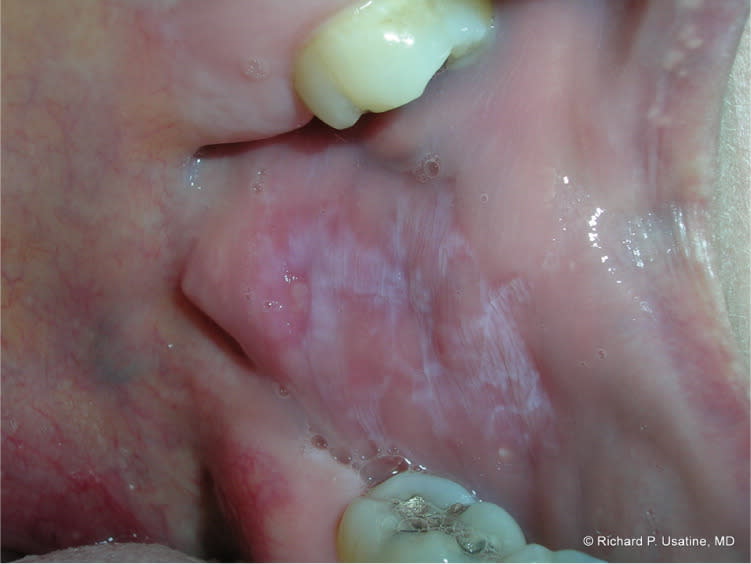
Oral lichen planus with Wickham striae on buccal mucosa.
Copyright © Richard P. Usatine, MD
Figure 9.
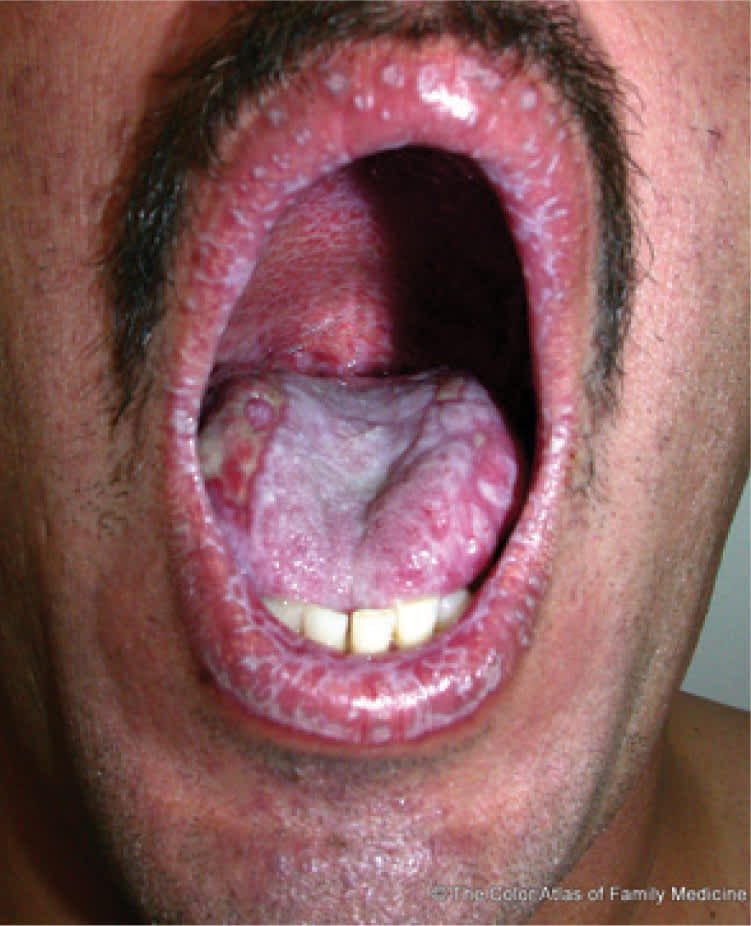
Oral lichen planus with erosions on the lips, tongue, and palate.
Reprinted with permission from Kraft R, Usatine RP. Lichen planus. In: The Color Atlas of Family Medicine. Usatine RP, Smith MA, Chumley H, Mayeaux EJ Jr., Tysinger J, eds. New York, NY: McGraw-Hill; 2009:638.
Lichen planus affecting the genitalia is more common in men. It typically presents on the glans penis and may have an annular pattern (Figure 105 ). Less commonly, linear, white striae similar to the lesions that typically appear on the vulva and vagina occur on the penis and scrotum. Reticular papules or severe erosions may appear on the vulva and become complicated by urethral stenosis. 11,12 Dyspareunia and pruritus are common with vulvar and vaginal lesions.11,12 Two reports show that more than 50 percent of women with oral lichen planus have undiagnosed vulvar lichen planus.11,12
Figure 10.
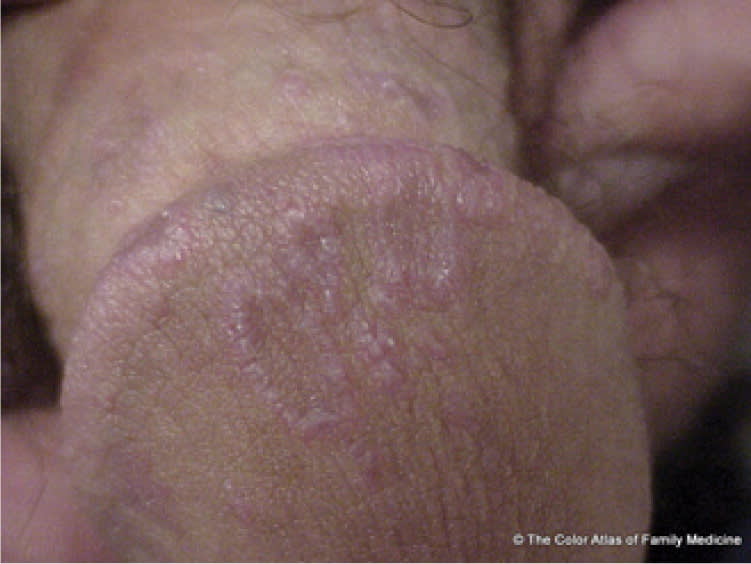
Lichen planus on the penis showing a lacy, white, annular pattern.
Reprinted with permission from Kraft R, Usatine RP. Lichen planus. In: The Color Atlas of Family Medicine. Usatine RP, Smith MA, Chumley H, Mayeaux EJ Jr., Tysinger J, eds. New York, NY: McGraw-Hill; 2009:639.
Approximately 10 percent of patients with lichen planus present with scalp and nail variants. Scalp lesions (lichen planopilaris) are violaceous, scaly, pruritic papules that can progress to scarring alopecia if untreated13 (Figure 11). Nail involvement is characterized by irregular, longitudinal grooving and ridging of the nail plate; thinning of the nail plate; nail pterygium (i.e., cuticular overgrowth); shedding of the nail plate with atrophy of the nail bed; subungual keratosis; longitudinal erythronychia or melanonychia; and subungual hyperpigmentation.7
Figure 11.
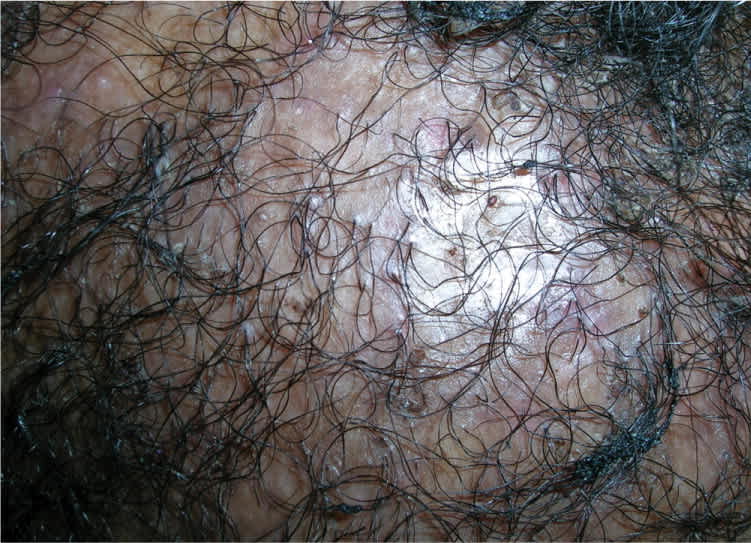
Lichen planopilaris causing hair loss with visible dark dots from follicular plugging.
Copyright © Richard P. Usatine, MD
Diagnosis
Lichen planus can be diagnosed clinically in classic cases, although biopsy is often helpful to confirm the diagnosis and is required for more atypical presentations. A 4-mm punch biopsy should be adequate on the skin or in the mouth. The histology shows a characteristic “saw-tooth” pattern of epidermal hyperplasia; hyperparakeratosis with thickening of the granular cell layer; and vacuolar alteration of the basal layer of the epidermis, with an intense infiltration (mainly T cells) at the dermal-epidermal junction. A 4-mm punch biopsy of perilesional skin for direct immunofluorescence may be added to the workup when bullous lesions, pemphigus, or bullous pemphigoid is present. Tables 2 and 3 present the differential diagnosis of cutaneous and oral lichen planus.
Table 2. Differential Diagnosis of Cutaneous Lichen Planus
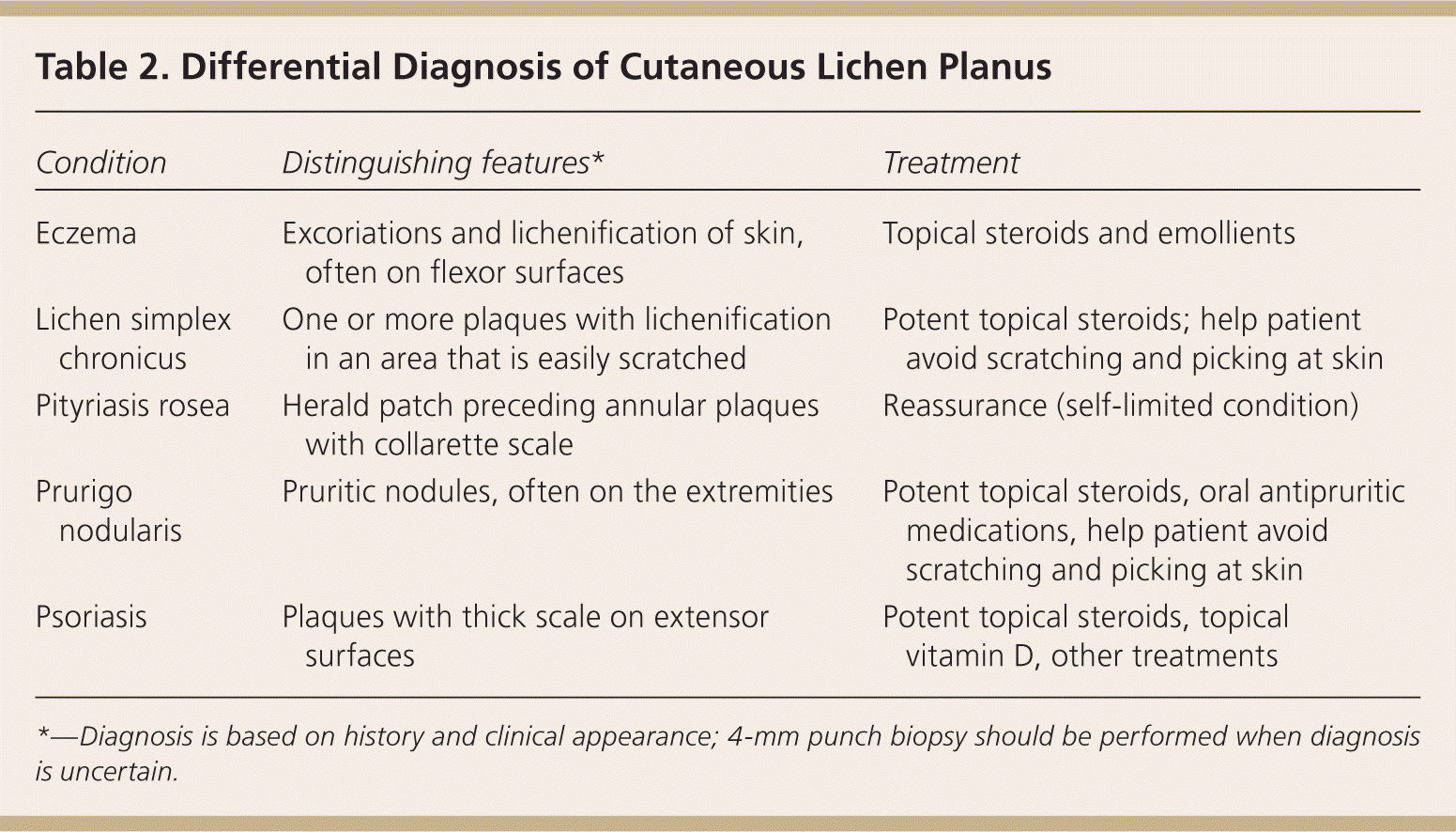
| Condition | Distinguishing features* | Treatment |
|---|---|---|
| Eczema | Excoriations and lichenification of skin, often on flexor surfaces | Topical steroids and emollients |
| Lichen simplex chronicus | One or more plaques with lichenification in an area that is easily scratched | Potent topical steroids; help patient avoid scratching and picking at skin |
| Pityriasis rosea | Herald patch preceding annular plaques with collarette scale | Reassurance (self-limited condition) |
| Prurigo nodularis | Pruritic nodules, often on the extremities | Potent topical steroids, oral antipruritic medications, help patient avoid scratching and picking at skin |
| Psoriasis | Plaques with thick scale on extensor surfaces | Potent topical steroids, topical vitamin D, other treatments |
*—Diagnosis is based on history and clinical appearance; 4-mm punch biopsy should be performed when diagnosis is uncertain.
Table 3. Differential Diagnosis of Oral Lichen Planus

| Condition | Distinguishing features | Diagnostic method | Treatment |
|---|---|---|---|
| Bite trauma | White area on buccal mucosa where the teeth occlude | Clinical appearance | Reassurance |
| Leukoplakia | White adherent patch or plaque on oral mucosa that does not rub off | Punch or shave biopsy | Surgical excision or cryotherapy with liquid nitrogen |
| Thrush | White adherent patch or plaque on oral mucosa that rubs off | Clinical appearance and potassium hydroxide (KOH) preparation | Antifungal suspension or troches |
Treatment
CUTANEOUS LICHEN PLANUS
Cutaneous lichen planus may resolve spontaneously within one to two years, although lichen planus affecting mucous membranes may be more persistent and resistant to treatment. Recurrences are common, even with treatment. Table 4 summarizes the treatment of nongenital cutaneous lichen planus lesions. High-potency topical corticosteroids are first-line therapy for cutaneous lichen planus.14–16 Oral antihistamines (e.g., hydroxyzine [Vistaril]) may be used to control pruritus. Hypertrophic lesions are treated with intralesional triamcinolone acetonide (Kenalog), 5 to 10 mg per mL injection (0.5 to 1 mL per 2-cm lesion).14
Table 4. Treatment of Nongenital Cutaneous Lichen Planus Lesions
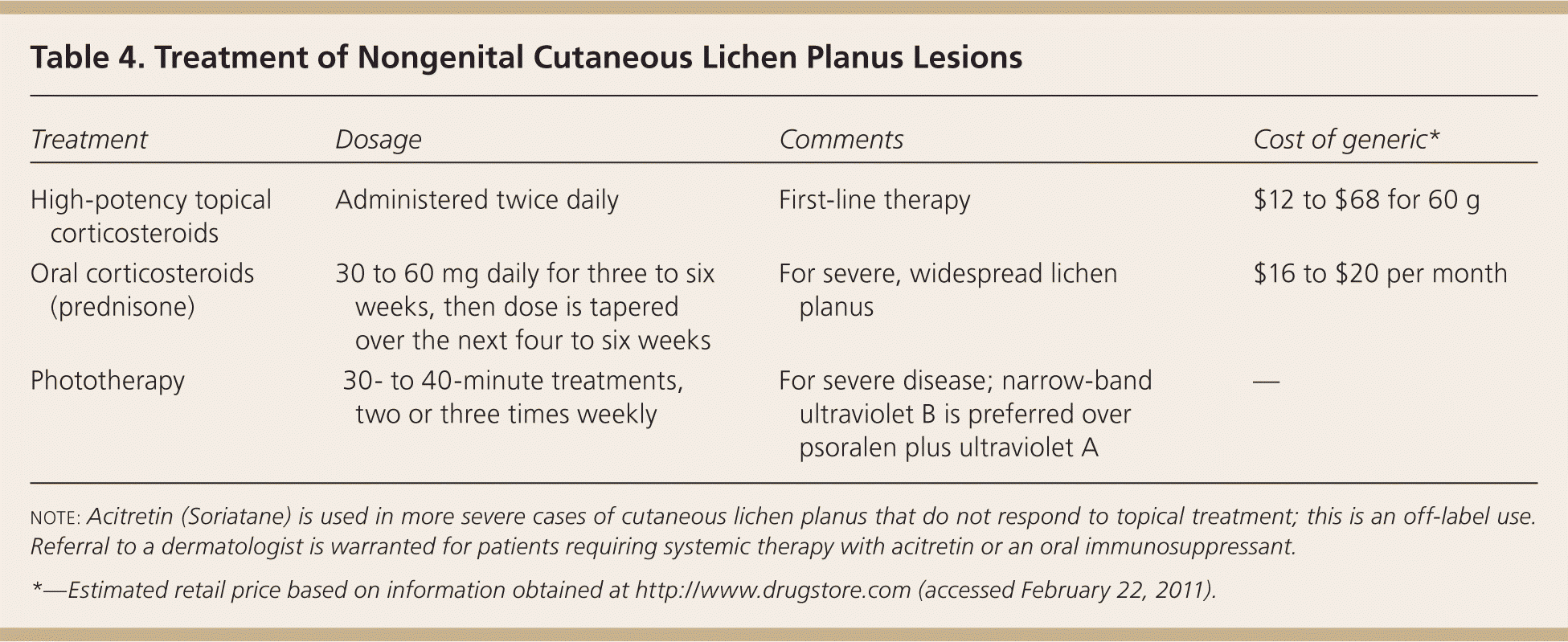
| Treatment | Dosage | Comments | Cost of generic* |
|---|---|---|---|
| High-potency topical corticosteroids | Administered twice daily | First-line therapy | $12 to $68 for 60 g |
| Oral corticosteroids (prednisone) | 30 to 60 mg daily for three to six weeks, then dose is tapered over the next four to six weeks | For severe, widespread lichen planus | $16 to $20 per month |
| Phototherapy | 30- to 40-minute treatments, two or three times weekly | For severe disease; narrow-band ultraviolet B is preferred over psoralen plus ultraviolet A | — |
note: Acitretin (Soriatane) is used in more severe cases of cutaneous lichen planus that do not respond to topical treatment; this is an off-label use. Referral to a dermatologist is warranted for patients requiring systemic therapy with acitretin or an oral immunosuppressant.
*—Estimated retail price based on information obtained at http://www.drugstore.com (accessed February 22, 2011).
Acitretin (Soriatane) is an expensive and toxic oral retinoid that is used in more severe cases of cutaneous lichen planus that do not respond to topical treatment.14 Acitretin is a strong teratogen that remains in the body for at least three months after the last dose; therefore, women who may become pregnant are not candidates for the therapy. Acitretin is not approved by the U.S. Food and Drug Administration (FDA) for the treatment of lichen planus, and the label includes an FDA boxed warning recommending that it be used only by physicians with experience treating severe psoriasis, prescribing oral retinoids, and handling teratogenic medications. Referral to a dermatologist is warranted for patients with severe lichen planus requiring systemic therapy with acitretin or an oral immunosuppressant.
For genital lichen planus lesions, triamcinolone ointment (Triderm) is a good firstline agent. Topical tacrolimus (Protopic) and clobetasol (Temovate) appear to be effective treatments for vulvovaginal erosive lichen planus.17 Aloe vera gel has been deemed a safe and effective treatment for patients with vulvar lichen planus.18 Topical lidocaine (Xylocaine) may be used as needed for pain relief, and a water-based lubricant may be used to prevent pain during intercourse.
The scarring alopecia of lichen planopilaris is difficult to reverse. A case series showed that topical high-potency corticosteroids and intralesional corticosteroids are commonly used.13
ORAL LICHEN PLANUS
Various treatments have been employed to treat symptomatic oral lichen planus, but complete resolution is difficult to achieve.19 Table 5 summarizes treatment options for oral lichen planus. Topical corticosteroids are first-line therapy.14–16 High-potency topical steroids are the most effective, with response rates up to 75 percent compared with placebo.20 Topical corticosteroids are also first-line therapy for mucosal erosive lichen planus.14 High-potency corticosteroids applied to the oral mucosa do not appear to cause significant adrenal suppression, even with relatively long-term use. Systemic corticosteroids, such as oral prednisone, should be considered only for severe, widespread oral lichen planus and for lichen planus involving other mucocutaneous sites.10,14
Table 5. Treatment of Oral Lichen Planus

| Treatment | Comments | Cost of generic (brand)* | ||
|---|---|---|---|---|
| High-potency topical corticosteroids† | First-line therapy | Clobetasol 0.05% ointment: | ||
| Clobetasol (Temovate) Fluocinonide | $30 ($205) for 60 g | |||
| Fluocinonide 0.05% | ||||
| Gel: $38 for 60 g (NA) | ||||
| Ointment: $34 for 60 g (NA) | ||||
| Topical calcineurin inhibitors† | For cases unresponsive to topical corticosteroids | Pimecrolimus 1% cream: | ||
| Pimecrolimus (Elidel) Tacrolimus (Protopic) | NA ($203 for 60 g) | |||
| Tacrolimus 0.1% ointment: | ||||
| NA ($243 for 60 g) | ||||
| Oral corticosteroids (prednisone)‡ | For severe, widespread lichen planus | $16 to $20 per month (NA) | ||
NA = not available.
*—Estimated retail price based on information obtained at http://www.drugstore.com (accessed February 22, 2011). Generic price listed first; brand price listed in parentheses.
†—Applied twice daily.
‡—30 to 60 mg daily for three to six weeks, then tapered over the next four to six weeks.
Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus (Elidel), are second-line therapies for oral lichen planus. 15,21 A comparative study showed that topical tacrolimus is as effective as the high-potency corticosteroid clobetasol in the treatment of oral lichen planus.15,21 A randomized controlled trial revealed that pimecrolimus 1% cream effectively treats erosive oral lichen planus with long-lasting therapeutic effects.22
In a randomized controlled trial, aloe vera gel was significantly more effective than placebo in the clinical and symptomatologic improvement of oral lichen planus.23 If topical corticosteroids are ineffective, carbon-dioxide laser evaporation can lead to long-term remission of symptoms, and may be appropriate as first-line therapy in patients with painful oral lichen planus.24

