Pruritus can be a symptom of a distinct dermatologic condition or of an occult underlying systemic disease. Of the patients referred to a dermatologist for generalized pruritus with no apparent primary cutaneous cause, 14 to 24 percent have a systemic etiology. In the absence of a primary skin lesion, the review of systems should include evaluation for thyroid disorders, lymphoma, kidney and liver diseases, and diabetes mellitus. Findings suggestive of less serious etiologies include younger age, localized symptoms, acute onset, involvement limited to exposed areas, and a clear association with a sick contact or recent travel. Chronic or generalized pruritus, older age, and abnormal physical findings should increase concern for underlying systemic conditions. Initial evaluation for systemic disease includes complete blood count and measurement of thyroid-stimulating hormone, fasting glucose, alkaline phosphatase, bilirubin, creatinine, and blood urea nitrogen. Hodgkin lymphoma is the malignant disease most strongly associated with pruritus, which affects up to 30 percent of patients with the disease. Chest radiography is needed when lymphoma is suspected. A wheal and flare response indicates histamine-induced pruritus in patients with urticaria or an allergic dermatitis. These patients benefit from continuous dosing of a long-acting antihistamine. Second-generation antihistamines, such as cetirizine, loratadine, and fexofenadine, may be more effective because of improved patient compliance.
Pruritus is the subjective sensation of itching. It can become severe enough to interfere with work and restful sleep. Histamine is the primary mediator of itching in many disorders.1 Antihistamines are effective in treating histamine-mediated pruritus, but they may be less effective in patients with diseases that trigger pruritus through mechanisms involving serotonin, leukotrienes, or neuropeptides.1,2
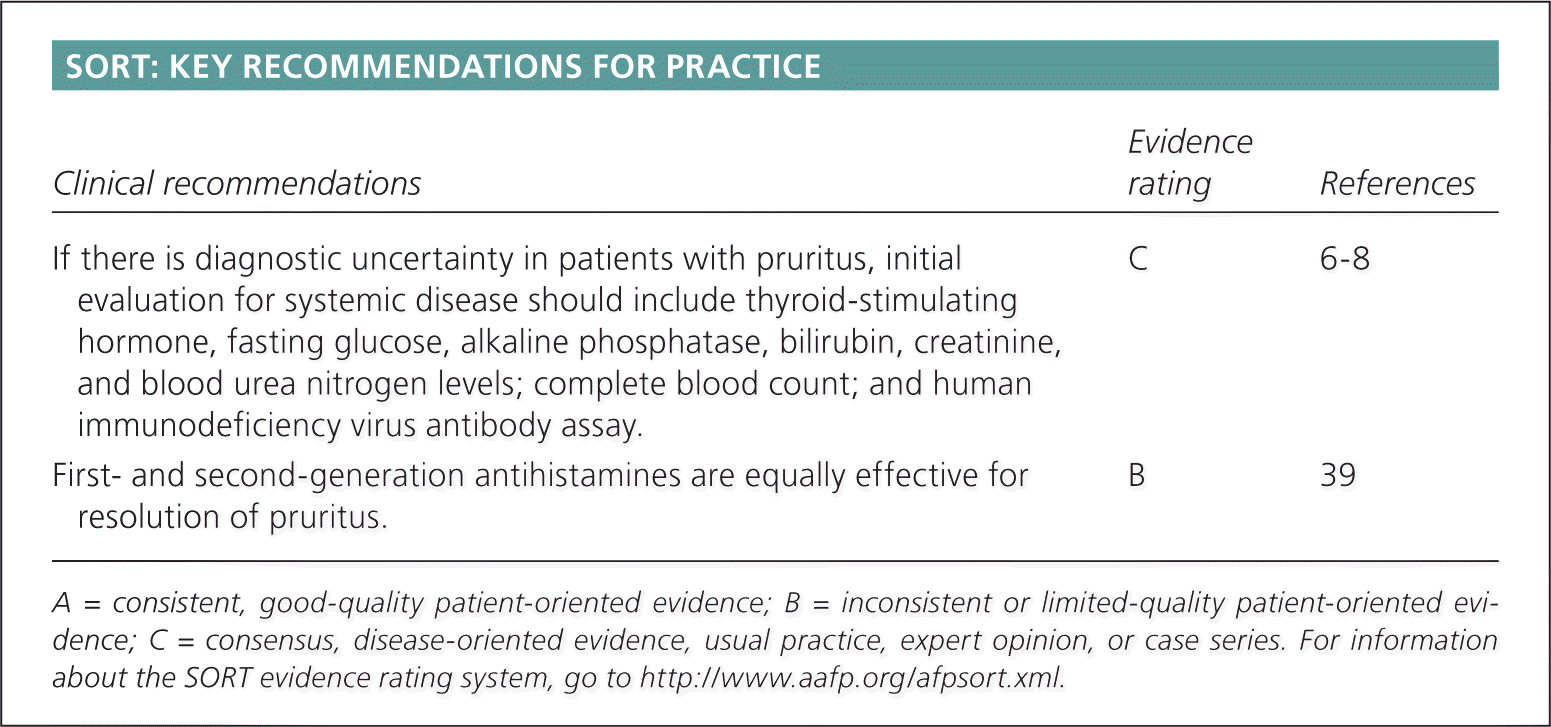
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendations | Evidence rating | References |
|---|---|---|
| If there is diagnostic uncertainty in patients with pruritus, initial evaluation for systemic disease should include thyroid-stimulating hormone, fasting glucose, alkaline phosphatase, bilirubin, creatinine, and blood urea nitrogen levels; complete blood count; and human immunodeficiency virus antibody assay. | C | 6–8 |
| First-and second-generation antihistamines are equally effective for resolution of pruritus. | B | 39 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Evaluation
The initial clinical approach in patients with pruritus includes a history and physical examination to determine if the pruritus is caused by a dermatologic condition or is secondary to an underlying systemic disease. Figure 1 is a diagnostic algorithm for pruritus.
Figure 1. Diagnosing the Cause of Pruritus
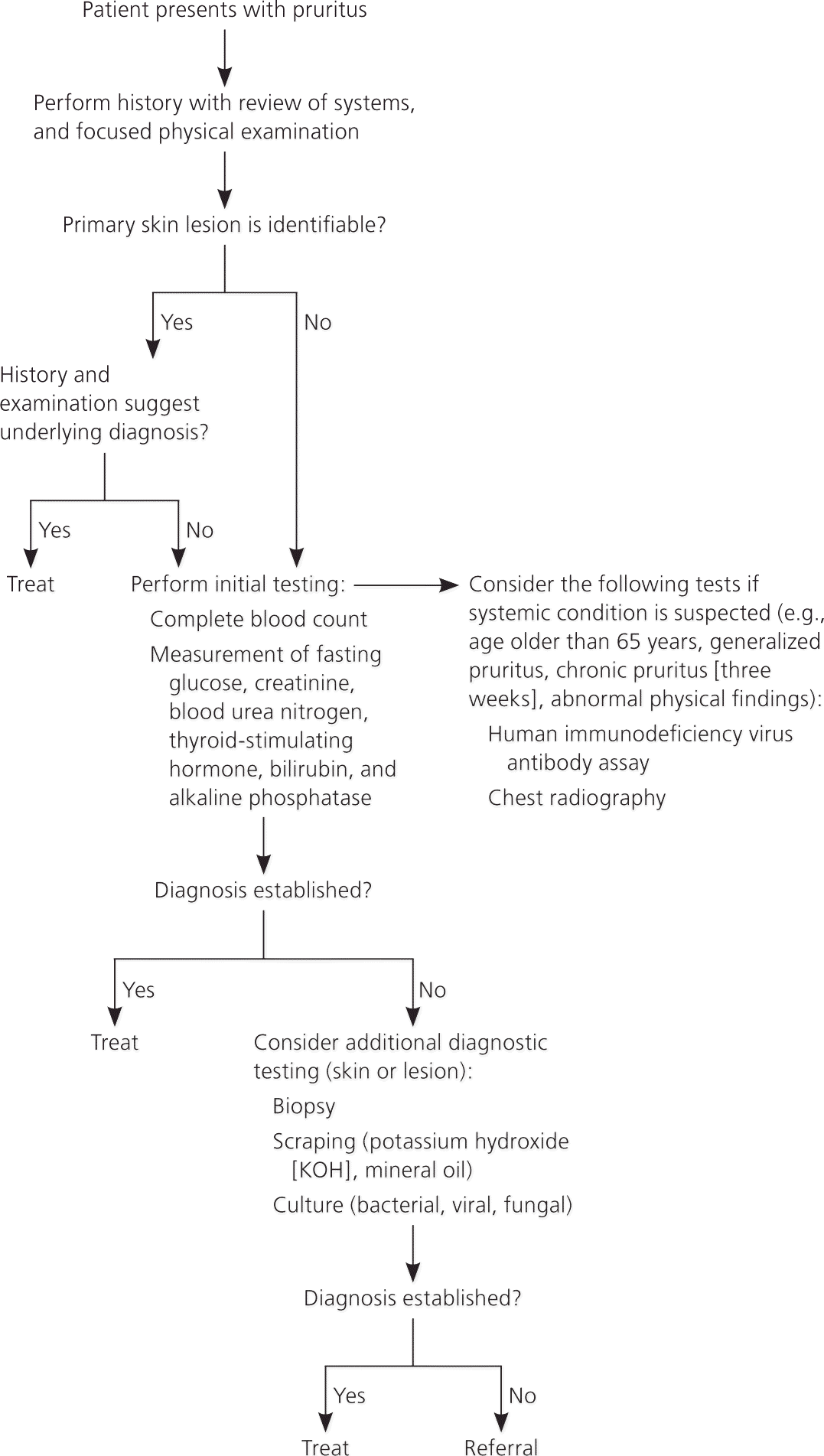
Diagnostic algorithm for pruritus.
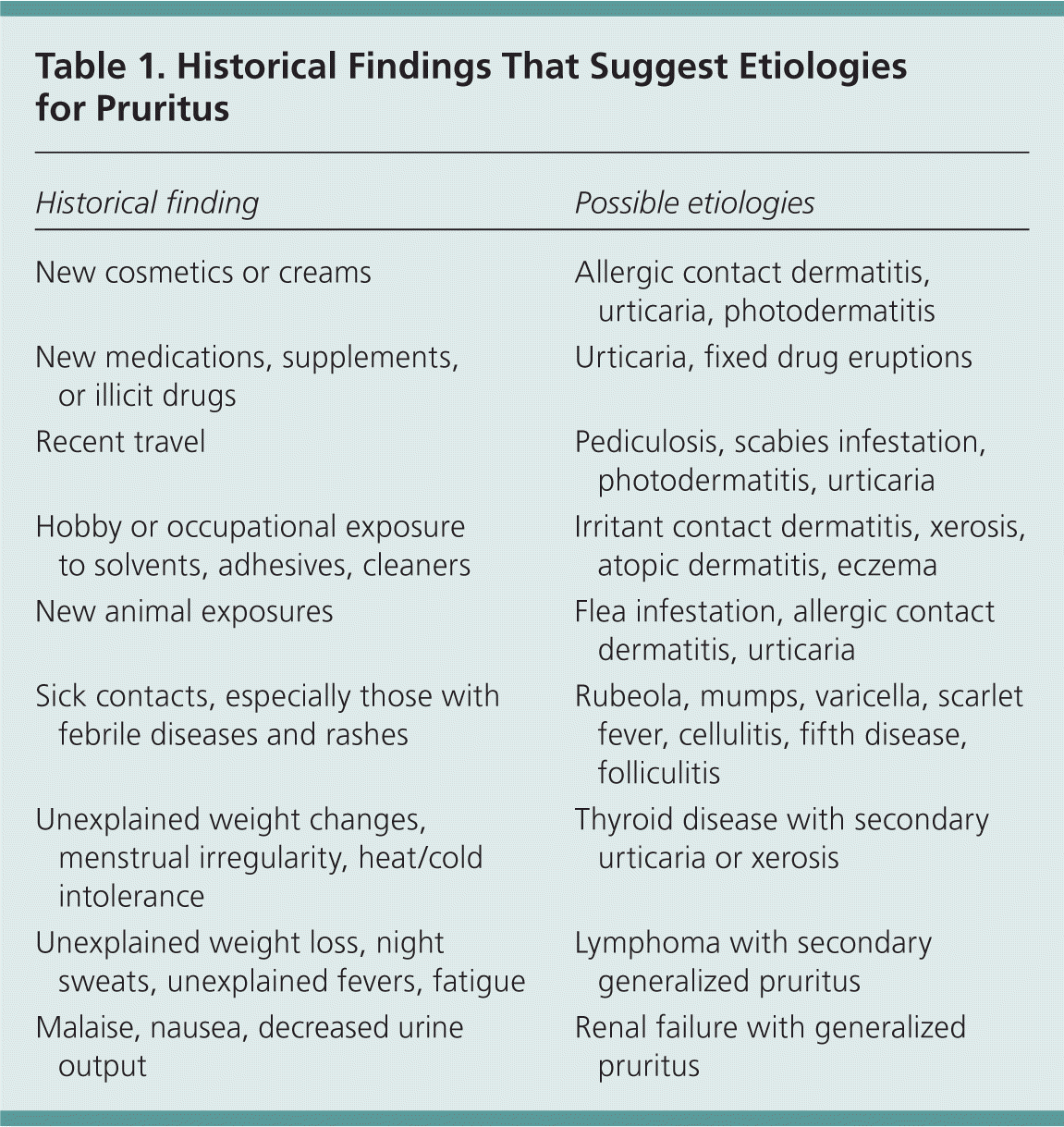
The presence of a primary skin lesion may aim the evaluation toward a dermatologic cause. The history should focus on recent exposures to new topical, oral, or airborne substances that can cause skin lesions. New cosmetics and creams can trigger allergic contact dermatitis, urticaria, and photodermatitis. New drugs (medications, nutritional supplements, illicit drugs) can lead to urticaria or fixed drug eruptions. Travel can expose a person to new foods that can trigger urticaria and to sunlight that can trigger photodermatitis. Travelers are also susceptible to infestations, such as with scabies or lice. Hobbies may expose the skin to solvents and topical agents that can trigger contact dermatitis. Chronic occupational exposure to solvents can dry the skin, causing xerosis and atopic dermatitis or eczema. New animal exposures can lead to flea infestations, allergic cutaneous reactions to dander, and urticaria. Another important finding in the evaluation of patients with pruritus is a recent exposure to sick contacts who have febrile diseases, such as rubeola, mumps, or varicella, or exposure to infectious organisms that can cause rashes, such as parvovirus, Staphylococcus aureus, or Streptococcus species. In the absence of a primary skin lesion, the review of systems should include evaluation for thyroid disorders, lymphoma, kidney and liver diseases, and diabetes mellitus. Table 1 includes historical findings that suggest etiologies for pruritus.
Table 1. Historical Findings That Suggest Etiologies for Pruritus
| Historical finding | Possible etiologies |
|---|---|
| New cosmetics or creams | Allergic contact dermatitis, urticaria, photodermatitis |
| New medications, supplements, or illicit drugs | Urticaria, fixed drug eruptions |
| Recent travel | Pediculosis, scabies infestation, photodermatitis, urticaria |
| Hobby or occupational exposure to solvents, adhesives, cleaners | Irritant contact dermatitis, xerosis, atopic dermatitis, eczema |
| New animal exposures | Flea infestation, allergic contact dermatitis, urticaria |
| Sick contacts, especially those with febrile diseases and rashes | Rubeola, mumps, varicella, scarlet fever, cellulitis, fifth disease, folliculitis |
| Unexplained weight changes, menstrual irregularity, heat/cold intolerance | Thyroid disease with secondary urticaria or xerosis |
| Unexplained weight loss, night sweats, unexplained fevers, fatigue | Lymphoma with secondary generalized pruritus |
| Malaise, nausea, decreased urine output | Renal failure with generalized pruritus |
Physical examination should include an evaluation of the liver, spleen, and lymph nodes. Organomegaly increases the likelihood of an underlying systemic disease, such as lymphoma. The skin should also be examined. Finger webs, intertriginous regions, and the genitals should be evaluated for the presence of scabies or lice.
Historical and physical findings that suggest a less serious etiology include younger age, localized symptoms, acute onset, involvement limited to exposed areas, and a clear association with a sick contact or recent travel.3–5 Chronic or generalized pruritus, age older than 65 years, and abnormal physical findings should increase concern for an underlying systemic condition.3–8
If the diagnosis is unclear after the history and physical examination or if initial empiric treatment is ineffective, a limited laboratory evaluation should be performed, including complete blood count and measurement of thyroid-stimulating hormone, fasting glucose, alkaline phosphatase, bilirubin, creatinine, and blood urea nitrogen. 5 If immune suppression or lymphoma is possible, a human immunodeficiency virus antibody assay and chest radiography should also be performed. 5–8 Further diagnostic tests may include biopsy, scraping, or culture of the skin or lesions.
Differential Diagnosis of Pruritus
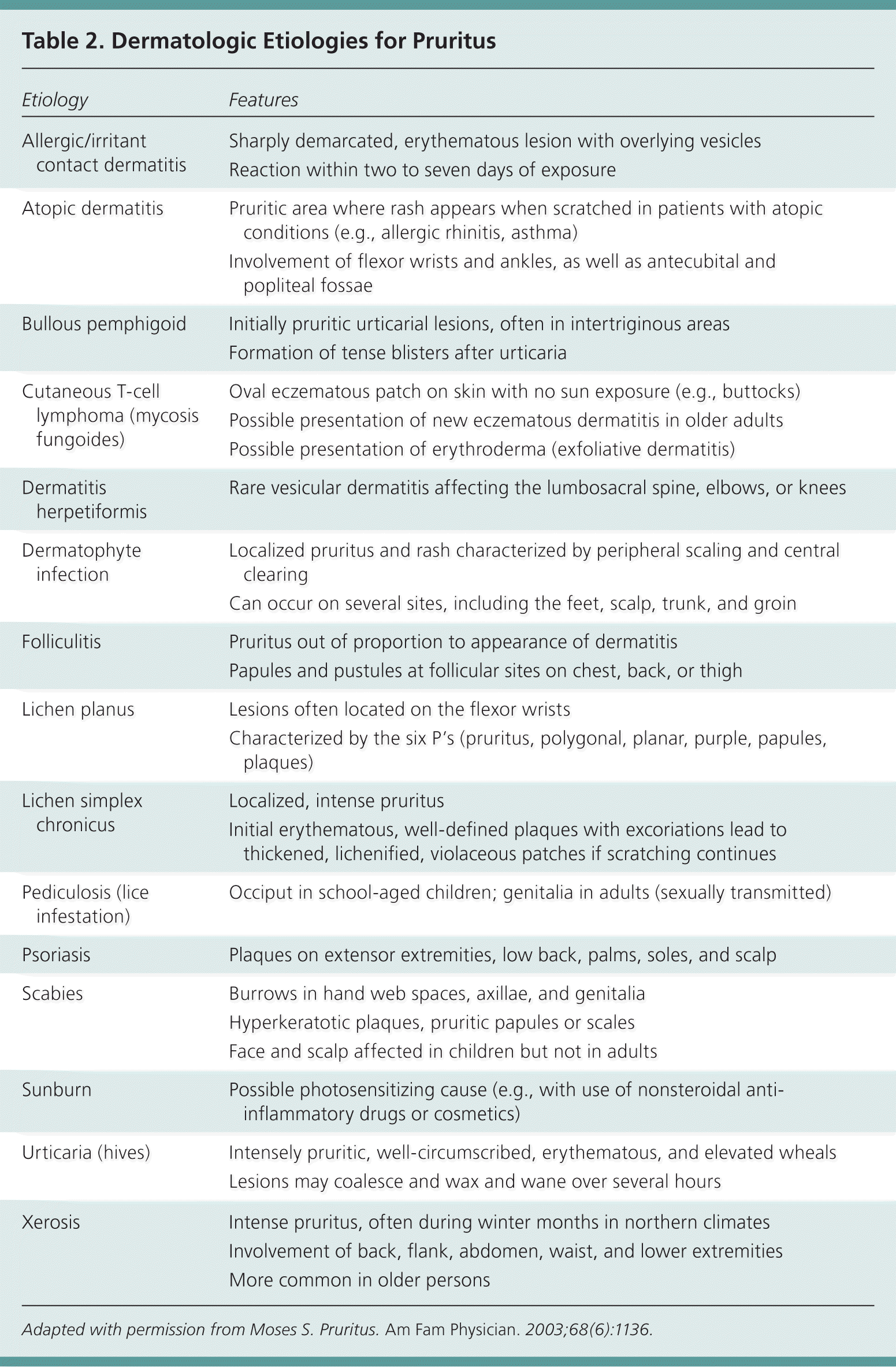
Pruritus can be a symptom of a distinct dermatologic condition (Table 27 ) or of an occult underlying systemic disease (Table 32,3,5,7,9,10 ).
Table 2. Dermatologic Etiologies for Pruritus
| Etiology | Features |
|---|---|
| Allergic/irritant contact dermatitis | Sharply demarcated, erythematous lesion with overlying vesicles |
| Reaction within two to seven days of exposure | |
| Atopic dermatitis | Pruritic area where rash appears when scratched in patients with atopic conditions (e.g., allergic rhinitis, asthma) |
| Involvement of flexor wrists and ankles, as well as antecubital and popliteal fossae | |
| Bullous pemphigoid | Initially pruritic urticarial lesions, often in intertriginous areas |
| Formation of tense blisters after urticaria | |
| Cutaneous T-cell lymphoma (mycosis fungoides) | Oval eczematous patch on skin with no sun exposure (e.g., buttocks) |
| Possible presentation of new eczematous dermatitis in older adults | |
| Possible presentation of erythroderma (exfoliative dermatitis) | |
| Dermatitis herpetiformis | Rare vesicular dermatitis affecting the lumbosacral spine, elbows, or knees |
| Dermatophyte infection | Localized pruritus and rash characterized by peripheral scaling and central clearing |
| Can occur on several sites, including the feet, scalp, trunk, and groin | |
| Folliculitis | Pruritus out of proportion to appearance of dermatitis |
| Papules and pustules at follicular sites on chest, back, or thigh | |
| Lichen planus | Lesions often located on the flexor wrists |
| Characterized by the six P's (pruritus, polygonal, planar, purple, papules, plaques) | |
| Lichen simplex chronicus | Localized, intense pruritus |
| Initial erythematous, well-defined plaques with excoriations lead to thickened, lichenified, violaceous patches if scratching continues | |
| Pediculosis (lice infestation) | Occiput in school-aged children; genitalia in adults (sexually transmitted) |
| Psoriasis | Plaques on extensor extremities, low back, palms, soles, and scalp |
| Scabies | Burrows in hand web spaces, axillae, and genitalia |
| Hyperkeratotic plaques, pruritic papules or scales | |
| Face and scalp affected in children but not in adults | |
| Sunburn | Possible photosensitizing cause (e.g., with use of nonsteroidal anti-inflammatory drugs or cosmetics) |
| Urticaria (hives) | Intensely pruritic, well-circumscribed, erythematous, and elevated wheals |
| Lesions may coalesce and wax and wane over several hours | |
| Xerosis | Intense pruritus, often during winter months in northern climates |
| Involvement of back, flank, abdomen, waist, and lower extremities | |
| More common in older persons |
Adapted with permission from Moses S. Pruritus. Am Fam Physician. 2003;68(6):1136.
Table 3. Systemic Etiologies for Pruritus

| Autoimmune |
| Dermatitis herpetiformis |
| Dermatomyositis |
| Linear immunoglobulin A disease |
| Sjögren syndrome |
| Hematologic |
| Hemochromatosis |
| Iron deficiency anemia |
| Mastocytosis |
| Plasma cell dyscrasias |
| Polycythemia vera |
| Hepatobiliary |
| Biliary cirrhosis |
| Chronic pancreatitis with obstruction of biliary tracts |
| Drug-induced cholestasis |
| Hepatitis, particularly hepatitis C |
| Sclerosing cholangitis |
| Infectious disease |
| AIDS |
| Infectious hepatitis |
| Parasitic disease (giardiasis, onchocerciasis, schistosomiasis, ascariasis) |
| Prion disease |
| Malignancy |
| Leukemia |
| Lymphoma |
| Multiple myeloma |
| Solid tumors with paraneoplastic syndrome |
| Metabolic and endocrine |
| Carcinoid syndrome |
| Chronic renal disease |
| Diabetes mellitus |
| Hyper/hypothyroidism |
| Hyperparathyroidism |
| Neurologic |
| Cerebral abscess |
| Cerebral tumor |
| Multiple sclerosis |
| Stroke |
| Other |
| Drug ingestion |
| Eating disorders with rapid weight loss |
| Neuropsychiatric disorders |
| Pregnancy |
COMMON DERMATOLOGIC CAUSES
Atopic Dermatitis. Atopic dermatitis is characterized by pruritus. It is generally defined as a chronic, relapsing inflammatory skin disease that often occurs in patients with a personal or family history of asthma or allergic rhinitis. 11 In contrast to other dermatologic disorders, atopic dermatitis often lacks a primary skin lesion. Usually only the secondary cutaneous findings of excoriation, weeping, lichenification, and pigment changes are apparent.2
Contact Dermatitis. Contact dermatitis is a rash caused by direct skin exposure to a substance. It is one of the most common skin disorders, with a lifetime prevalence of 30 percent. 12 Often intensely pruritic, the dermatitis can be induced by an allergen or more commonly by an irritant. Irritant contact dermatitis represents the most common cause of occupational skin diseases in industrial countries.13
Dermatophytes. Dermatophyte infections cause localized pruritus and a rash characterized by peripheral scaling and central clearing. Tinea pedis (athlete's foot) usually occurs between the toes with dry, cracking skin and white areas of maceration. Tinea infections can occur at several other sites, including the scalp, trunk, and groin.
Lice. Pediculosis is marked by pruritus caused by a delayed hypersensitivity reaction to the saliva of the louse. A magnifying lens is often necessary to see the lice or eggs, usually at the base of hair shafts. Body lice are typically found in patients with poor hygiene, whereas pubic lice are sexually transmitted.14
Lichen Simplex Chronicus. Lichen simplex chronicus is a localized disorder characterized by pruritus that leads to thickened, lichenified, violaceous patches. These patches are intensely pruritic, which causes the patient to continue to scratch, perpetuating the cycle. Early lesions manifest as erythematous, well-defined plaques with excoriations. Lesions continue to thicken if the itch-scratch-itch cycle is not broken with appropriate treatment.15
Psoriasis. Up to 80 percent of patients with psoriasis report pruritus that is cyclical, with nocturnal exacerbations that interrupt sleep. Pruritus is often more generalized and not restricted to areas of psoriatic plaques.16
Scabies. The classic feature of scabies is pruritus, which is caused by deposition of mite eggs in the epidermal layer of skin. The pruritus is often severe and worsens at night.
The primary lesion is a small, erythematous papule that is often excoriated. A thin, reddish-brown line, or burrow, 2 to 15 mm long in intertriginous regions is more pathognomic. However, burrows are often absent or obscured by excoriation or secondary infection. 17
Urticaria. Urticaria, or hives, is a common disorder that affects up to 25 percent of the population.18 The usual lesion is an intensely pruritic, well-circumscribed, erythematous, elevated wheal. Individual lesions may coalesce and wax and wane over several hours.19 Histamine is the primary mediator for most types of urticaria, although other immunohistochemicals may play an important role in more chronic cases.18
Xerosis. Xerosis is the most common cause of pruritus in the absence of an identifiable skin lesion. It is characterized by dry, scaly skin, usually on the lower extremities and in axillary creases, and most often occurs in the winter months. Associated factors include older age, frequent bathing, use of hot water when bathing, and exposure to high ambient temperatures with relatively low humidity.20
COMMON SYSTEMIC CAUSES
Pruritus in the absence of a primary dermatologic etiology may be indicative of a serious underlying systemic disease. 4 Studies have shown that 14 to 24 percent of patients presenting to a dermatologist's office with pruritus and no primary dermatologic cause have a systemic condition. 4,9,21–24 However, pruritus is often overemphasized as an early manifestation of cancer.4,21
Chronic Renal Disease. More than 50 percent of patients with chronic renal disease and up to 80 percent of patients on dialysis have pruritus.2 The pruritus is often generalized, but may be localized to the back.25
Liver Disease. Pruritus caused by impaired bile secretion is a common symptom in several forms of liver disease. It can be generalized, but is typically worse on the palms and soles. Associated conditions include primary biliary cirrhosis, sclerosing cholangitis, viral hepatitis, drug-induced cholestasis, and other causes of obstructive jaundice. Biliary obstruction leads to pruritus in these disorders, but there is little correlation between serum bilirubin level and severity of pruritus.26
Malignancy. The possibility of an underlying malignant disease should be considered in patients with generalized pruritus of unknown cause. Among malignant diseases, Hodgkin lymphoma has the strongest association with pruritus, which occurs in up to 30 percent of patients with the disease.10 Pruritus can precede the clinical presentation of lymphoma by up to five years and is often the presenting symptom.5 Pruritus has been reported as a paraneoplastic manifestation in patients with nasopharynx, prostate, stomach, breast, brain, uterine, or colon cancer.5,27
Peripheral or Central Nervous System. Pruritus can also arise from diseases or disorders of the peripheral or central nervous system, such as multiple sclerosis, neuropathy, and nerve compression or irritation (e.g., notalgia paresthetica, brachioradial pruritus).28
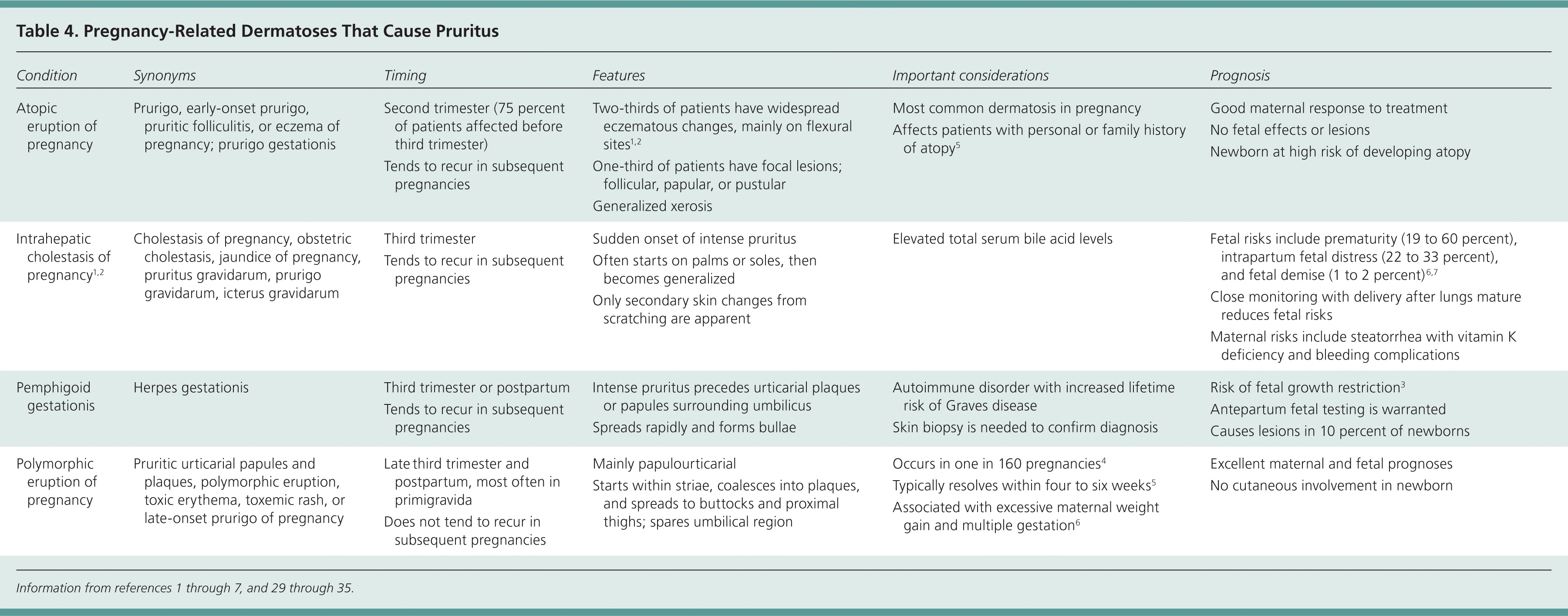
Pregnancy. Pregnancy-related dermatoses (Table 41–7,29–35 ) represent a heterogeneous group of pruritic inflammatory skin diseases related to pregnancy or the postpartum period. Some dermatoses cause only intense pruritus and skin lesions (e.g., polymorphic eruption of pregnancy, atopic eruption of pregnancy), but others can cause significant fetal risks, including prematurity, growth restriction, fetal distress, and intrauterine fetal demise (e.g., intrahepatic cholestasis of pregnancy, pemphigoid gestationis).29–37 Early recognition, precise diagnosis, and prompt treatment are essential for improving maternal and fetal prognosis.
Table 4. Pregnancy-Related Dermatoses That Cause Pruritus
| Condition | Synonyms | Timing | Features | Important considerations | Prognosis |
|---|---|---|---|---|---|
| Atopic eruption of pregnancy | Prurigo, early-onset prurigo, pruritic folliculitis, or eczema of pregnancy; prurigo gestationis | Second trimester (75 percent of patients affected before third trimester) |
|
| |
| Tends to recur in subsequent pregnancies | |||||
| Intrahepatic cholestasis of pregnancy1,2 | Cholestasis of pregnancy, obstetric cholestasis, jaundice of pregnancy, pruritus gravidarum, prurigo gravidarum, icterus gravidarum | Third trimester |
|
| |
| Tends to recur in subsequent pregnancies | |||||
| Pemphigoid gestationis | Herpes gestationis | Third trimester or postpartum |
|
|
|
| Tends to recur in subsequent pregnancies | |||||
| Polymorphic eruption of pregnancy | Pruritic urticarial papules and plaques, polymorphic eruption, toxic erythema, toxemic rash, or late-onset prurigo of pregnancy | Late third trimester and postpartum, most often in primigravida |
|
| |
| Does not tend to recur in subsequent pregnancies |
Psychiatric Illness. Psychiatric illness can cause pruritus and is diagnosed through exclusion. Neurotic excoriations are scattered, linear, crusted lines that may occur anywhere on the body within reach of the patient, although they are most often confined to the extremities. They are associated with obsessive-compulsive disorder, depression, and delusions of parasitosis.38
Treatment
A wheal and flare response is a marker of histamine-induced pruritus in patients with urticaria or an allergic dermatitis. These patients benefit from continuous dosing of long-acting antihistamines. First-and second-generation antihistamines are equally effective for resolution of pruritus.39 However, second-generation antihistamines (e.g., cetirizine [Zyrtec], loratadine [Claritin], fexofenadine [Allegra]) cause fewer adverse effects, leading to improved patient compliance.2,40 Concurrent administration of histamine H1 and H2 blockers increases therapeutic effectiveness.2
Most patients with pruritus benefit from several basic measures to lessen drying of skin, which can increase symptoms. Bathing should be limited to short, cool showers with soap applied only to intertriginous or oily skin areas. A mild moisturizing cream should be applied immediately after bathing. The patient's home should be humidified to at least 40 percent, especially during dry, cold winter months. Contact irritants, such as wool, fiberglass, and detergents, irritate most skin and can exacerbate symptoms, particularly in persons with sensitivity to these agents.2,3,5,41,42
The conditions that can lead to pruritus are extensive. Distinguishing between pruritus with a specific dermatologic cause and pruritus that is a manifestation of a systemic disease can facilitate efficient diagnosis and treatment, leading to a rapid resolution of symptoms for most patients. Treatment options for specific etiologies of pruritus are beyond the scope of this article.

