A 62-year-old white man presented with blistering of the skin on his lower extremity. The rash began two weeks prior on the anterior surface of his right ankle and did not improve with a one-week course of ciprofloxacin (Cipro). A similar rash subsequently developed on the lateral surface of his right thigh. He denied any foreign travel, trauma, or insect bites. He had a history of hypothyroidism, for which he took levothyroxine. He had no known medication allergies. He worked as a truck driver and had no pets. The patient did not have fever, gastrointestinal symptoms, or joint pain. Apart from the skin changes and swelling of the leg, the review of systems was unremarkable.
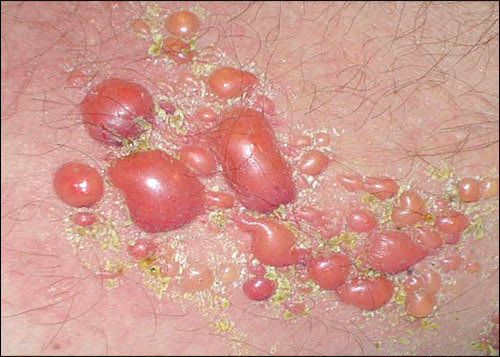
Physical examination revealed large, confluent, erythematous patches with clusters of clear and hemorrhagic vesicles, bullae, and sporadic ulcerations over the right lateral leg and anterior ankle (see accompanying figure). There was no mucosal involvement or inguinal lymphadenopathy. The rash was pruritic, but there was no pain or numbness. The examination was negative for Nikolsky sign (i.e., epidermal detachment from minimal pressure applied to normal skin adjacent to the lesion).
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Bullous pemphigoid.
B. Dermatitis herpetiformis.
C. Erythema multiforme.
D. Pemphigus vulgaris.
E. Porphyria cutanea tarda.
Discussion
The correct answer is A: bullous pemphigoid. The autoimmune condition is characterized by tense bullae on normal or erythematous skin.1 Typical age of onset is between 60 and 80 years; however, cases of juvenile bullous pemphigoid occur. Incidence of the disease increases with age.1,2 Patients may present with pruritus or urticaria with bullous formation occurring over weeks to months.3 Fluid contained in the bullae may be clear, or hemorrhagic if the base is bleeding. Rupture of the bullae results in erosions and crusting.1 Skin involvement can be localized, with lesions confined to the lower extremities, abdomen, and forearms; or generalized, with a widespread distribution of bullae.1,2 Mucosal involvement occurs in 10 to 25 percent of affected patients.3
The diagnosis is based on histologic examination, which reveals separation of the epidermis and dermis. Direct immunofluorescence testing shows deposition of immunoglobulin G autoantibodies targeting two hemidesmosomal proteins on the basement membrane of the epidermis.1,3 Serum antibody titers for the two antigens may also be performed. Prednisone, alone or in combination with a steroid-sparing agent, is the cornerstone of treatment. 2,3 Topical corticosteroids may be sufficient for mild cases. The prognosis is good for most patients. 2
Dermatitis herpetiformis is an autoimmune condition typified by clusters of erythematous papules, excoriations, and vesicles that arise as a consequence of gluten sensitivity. The lesions are extremely pruritic and tend to be distributed symmetrically along extensor surfaces.2,4 Dermatitis herpetiformis is associated with celiac sprue, but it can occur with other autoimmune disorders and malignancies. Most patients are between 20 and 40 years of age, but the condition may occur at any age.2,4
Erythema multiforme is an acute type IV hypersensitivity reaction to certain medications, herpes simplex virus or mycoplasma infection, and other triggers. 5,6 It is a self-limited condition characterized by macules, papules, and “target” lesions that may contain a small bulla or vesicle.5 The rash begins on the distal extremities and spreads proximally. 6 The skin lesions are usually symmetric, and there is minimal involvement of mucous membranes. Diagnosis is based largely on history and clinical presentation. 5
Pemphigus vulgaris is an autoimmune disease that affects the skin and mucous membranes. The predominant skin lesions are flaccid blisters. The blisters are located on the head, trunk, and intertriginous areas, and onset is typically between 40 and 60 years of age. Pemphigus vulgaris is associated with Nikolsky sign and has a mortality rate of 5 to 15 percent.2,7 It is associated with other autoimmune diseases, including myasthenia gravis and thymoma. 2
Porphyria cutanea tarda results from a deficiency in a heme-synthesizing enzyme. Blistering of the skin occurs on sun-exposed areas, especially the hands and forearms, and occasionally the face. Patients may also exhibit hypertrichosis of the forehead and cheeks, skin hyperpigmentation, and urine discoloration. Risk factors for the disease include hepatitis C, hemochromatosis, and alcoholism. 8
Summary Table
| Condition | Characteristics |
|---|---|
| Bullous pemphigoid | Tense bullae with clear or hemorrhagic fluid; may begin as urticaria or pruritus with bullous formation over weeks to months; mucosal involvement rare; Nikolsky sign absent; onset typically between 60 and 80 years of age |
| Dermatitis herpetiformis | Clusters of pruritic and erythematous papules, excoriations, or vesicles symmetrically distributed on extensor surfaces; associated with celiac sprue; onset typically between 20 and 40 years of age |
| Erythema multiforme | Acute type IV hypersensitivity reaction characterized by macules, papules, and “target” lesions; begins on distal extremities and spreads proximally; minimal involvement of mucous membranes |
| Pemphigus vulgaris | Flaccid blisters located on head, trunk, and intertriginous areas; mucosal involvement; Nikolsky sign present; onset typically between 40 and 60 years of age |
| Porphyria cutanea tarda | Blistering of the skin occurring on sun-exposed areas; may exhibit hypertrichosis of the forehead and cheeks, hyperpigmentation, and urine discoloration; associated with hepatitis C, hemochromatosis, and alcoholism |

