Numerous treatments for nongenital cutaneous warts are available, although no single therapy has been established as completely curative. Watchful waiting is an option for new warts because many resolve spontaneously. However, patients often request treatment because of social stigma or discomfort. Ideally, treatment should be simple and inexpensive with low risk of adverse effects. Salicylic acid has the best evidence to support its effectiveness, but it is slow to work and requires frequent application for up to 12 weeks. Cryotherapy with liquid nitrogen is a favorable option for many patients, with cure rates of 50 to 70 percent after three or four treatments. For recalcitrant warts, Candida or mumps skin antigen can be injected into the wart every three to four weeks for up to three treatments. More expensive treatments for recalcitrant warts are offered in many dermatology offices. Photodynamic therapy with aminolevulinic acid has the best evidence of effectiveness compared with pulsed dye laser, intralesional bleomycin, and surgical removal using curettage or cautery.
Cutaneous warts are benign epidermal proliferations caused by human papillomavirus (HPV) infection. Although there are more than 100 serotypes of HPV, knowing the serotype does not influence the treatment of benign warts.1 Warts vary in appearance, size, shape, and treatment response depending on the type of epithelium affected (Figures 1 through 3). Cutaneous warts can be categorized into six types (Table 1). Warts are spread via person-to-person contact or indirectly by fomites.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Salicylic acid and cryotherapy with liquid nitrogen are first-line treatments for cutaneous warts. | A | 2, 9 |
| Aggressive cryotherapy (10 to 30 seconds) is more effective than less aggressive cryotherapy. | B | 2, 7, 11 |
| Best results of cryotherapy can be achieved when the patient is treated every two or three weeks. There is no therapeutic benefit beyond three months. | B | 17, 27 |
| When using cryotherapy for plantar warts, paring the wart before treatment can increase the clearance rate. | B | 27 |
| Intralesional injection with Candida or mumps skin antigen has moderate effectiveness for treatment of recalcitrant warts in patients with a positive skin antigen pretest. | B | 20, 21 |
| Photodynamic therapy with aminolevulinic acid plus topical salicylic acid is a moderately effective option for treatment of recalcitrant warts. | B | 1, 2, 11, 22 |
| Although preliminary studies were promising, duct tape is not effective for wart treatment. | B | 25, 26 |
| Pulsed dye laser or intralesional injection with bleomycin can be considered for treatment of recalcitrant warts, although the effectiveness is unproven. | B | 2, 11 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Figure 1.
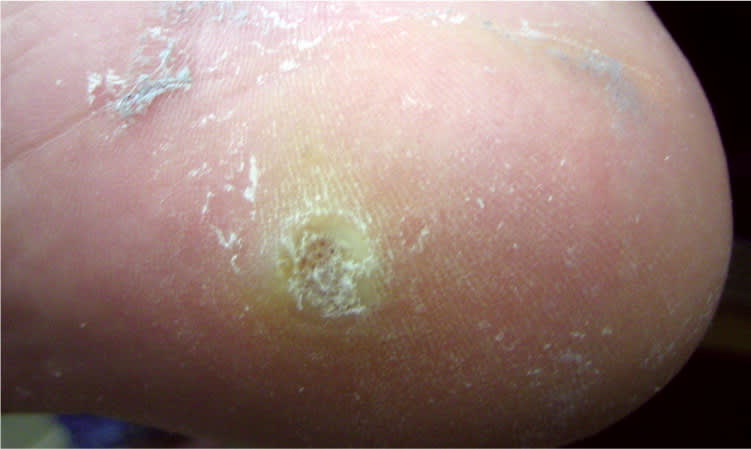
Plantar wart on the foot.
Figure 2.
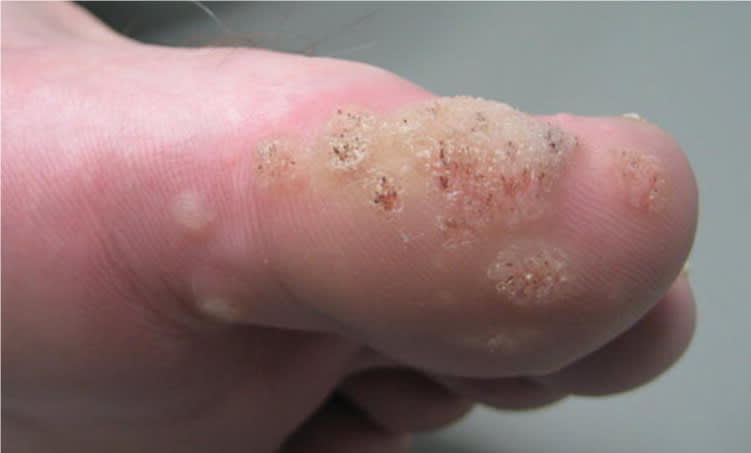
Warts on the first toe.
Figure 3.
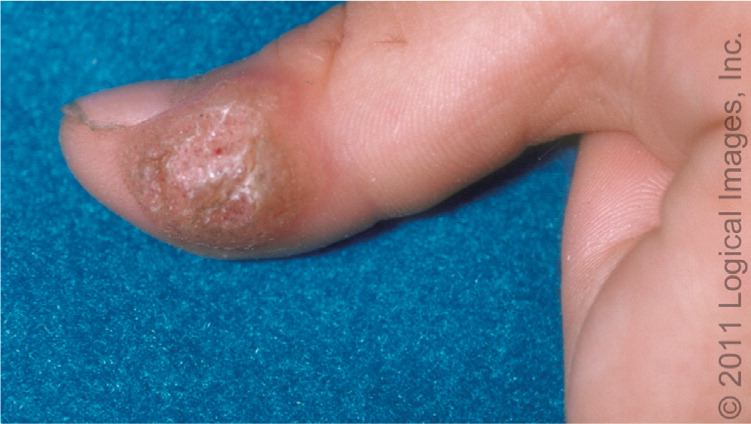
Wart on the thumb of a child.
Copyright © Logical Images
Table 1. Types of Nongenital Cutaneous Warts

| Wart type | Description | Causative HPV serotypes |
|---|---|---|
| Common (verruca vulgaris) | Skin-colored or gray-brown papules, with a rough (hyperkeratotic) surface; most common on the hands; represents 70 percent of nongenital cutaneous warts9 | 1–5, 7, 27, 29 |
| Flat (verruca plana) | Smooth, flat-topped, yellow-brown papules, often located on the face and along scratch marks; common in children, rare in adults | 3, 10, 28, 29 |
| Intermediate | Combination of common and flat warts | 2, 3, 10, 28, 29 |
| Mosaic | Plaque of closely grouped plantar warts | 2 |
| Periungual | Thickened, fissured, cauliflower-like skin around the nail plate | 1, 2, 4, 5, 7, 27, 57 |
| Plantar (verruca plantaris) | Look like thick calluses on the soles of the feet; pinpoint bleeding when the surface is pared away distinguishes it from corns and calluses | 1–4, 27, 29, 57 |
HPV = human papillomavirus.
Nongenital cutaneous warts are common in children, with a peak incidence in the teenage years and a sharp decline thereafter.2 Persons who walk barefoot often are at increased risk of plantar warts,1 meat handlers are at risk of hand warts,3 and nail biters commonly have multiple periungual warts.4 Immunosuppression is another important risk factor. An observational study of immunosuppressed patients at least five years after receiving a renal transplant found that 90 percent of patients had warts.5
Watchful waiting is an option for new warts, because they tend to be self-limited and treatment does not decrease transmissibility of the virus.6 In 17 trials, the average reported cure rate was 30 percent within 10 weeks.7 Observational studies have shown that one-half of cutaneous warts resolve spontaneously within one year, and about two-thirds within two years.8 However, many patients request treatment because of social stigma or discomfort. Ideally, treatment should be simple and inexpensive with low risk of adverse effects.2 Although no single treatment has been established as completely curative, many options are available (Table 2). The effectiveness and safety of these treatments generally have not been assessed in randomized controlled trials (RCTs).9,10 Many non-RCTs have been published on the treatment of cutaneous warts, but should be interpreted with caution because of a significant placebo effect.
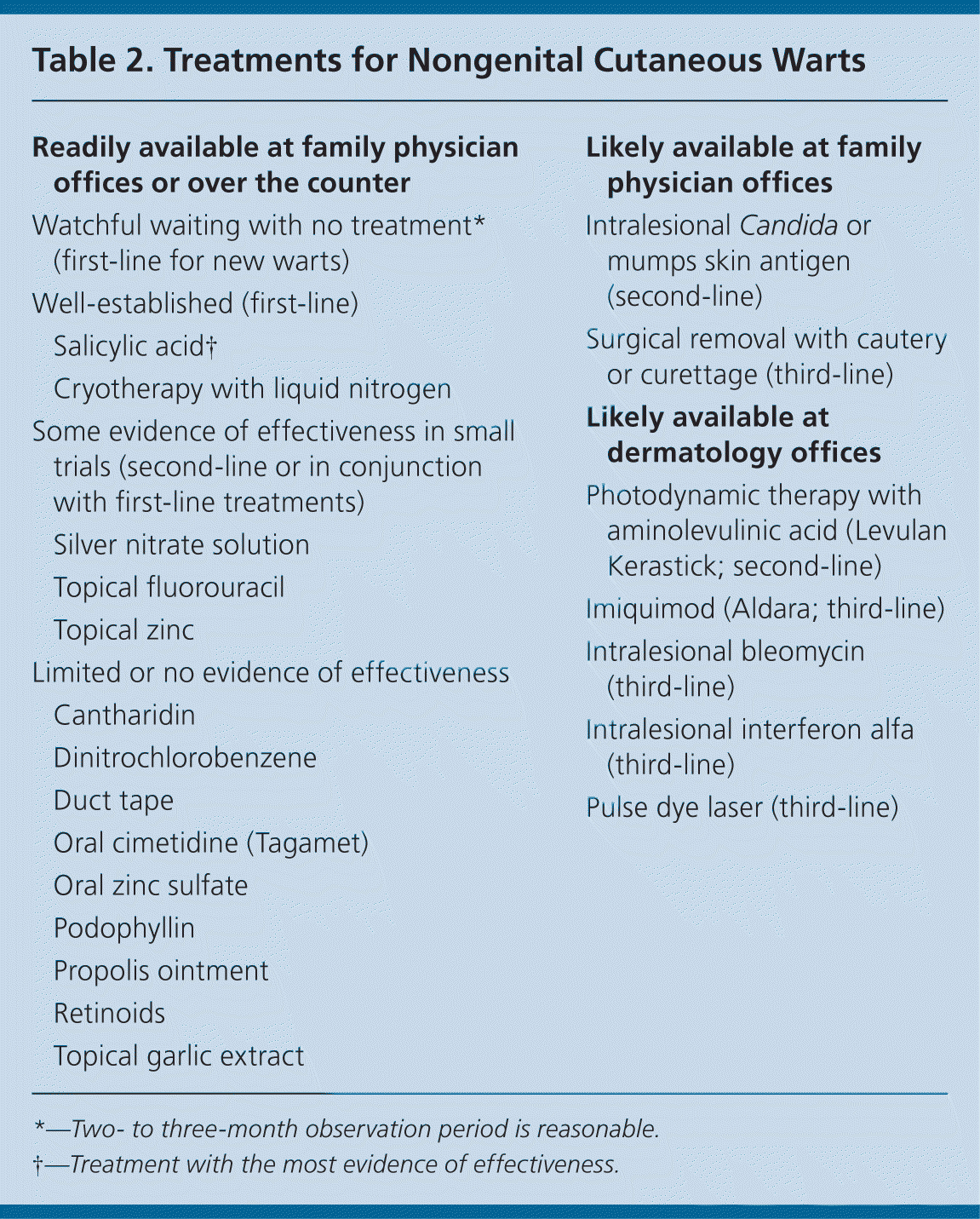
Table 2. Treatments for Nongenital Cutaneous Warts
| Readily available at family physician offices or over the counter | |
| Watchful waiting with no treatment* (first-line for new warts) | |
| Well-established (first-line) | |
| Salicylic acid† | |
| Cryotherapy with liquid nitrogen | |
| Some evidence of effectiveness in small trials (second-line or in conjunction with first-line treatments) | |
| Silver nitrate solution | |
| Topical fluorouracil | |
| Topical zinc | |
| Limited or no evidence of effectiveness | |
| Cantharidin | |
| Dinitrochlorobenzene | |
| Duct tape | |
| Oral cimetidine (Tagamet) | |
| Oral zinc sulfate | |
| Podophyllin | |
| Propolis ointment | |
| Retinoids | |
| Topical garlic extract | |
| Likely available at family physician offices | |
| Intralesional Candida or mumps skin antigen (second-line) | |
| Surgical removal with cautery or curettage (third-line) | |
| Likely available at dermatology offices | |
| Photodynamic therapy with aminolevulinic acid (Levulan Kerastick; second-line) | |
| Imiquimod (Aldara; third-line) | |
| Intralesional bleomycin (third-line) | |
| Intralesional interferon alfa (third-line) | |
| Pulse dye laser (third-line) | |
*—Two- to three-month observation period is reasonable.
†—Treatment with the most evidence of effectiveness.
Salicylic Acid (Beneficial11)
Salicylic acid is a colorless, crystalline organic acid. The keratolytic agent slowly destroys the HPV-infected epidermis and may cause an immune response from mild irritation.1 Salicylic acid is available over the counter in many different preparations and concentrations. Limited evidence has not shown one preparation or concentration to be superior,2 but salicylic acid 17% is most commonly used. Advantages of salicylic acid over other treatment options include low cost, over-the-counter availability, and minimal adverse effects. It is also the treatment option with the best evidence to support its effectiveness. Combined results from five RCTs showed a 73 percent cure rate with six to 12 weeks of salicylic acid treatment, compared with a 48 percent cure rate with placebo (number needed to treat = 4).2 Combining salicylic acid with cryotherapy may be more effective than either treatment alone (relative risk = 1.24).12,13
Salicylic acid is well tolerated, but the most common adverse effect is minor skin irritation. The therapy should not be used on the face because it can cause hypo- or hyperpigmentation.9 Salicylic acid therapy is slow to take effect and requires frequent application for up to 12 weeks. To achieve high success rates with salicylic acid, the proper technique and length of treatment should be discussed with the patient (Table 3).
Table 3. Common Approach for Salicylic Acid Treatment of Nongenital Cutaneous Warts

| Use any over-the-counter salicylic acid 17% product; salicylic acid is available in numerous preparations and concentrations. |
| Soak the wart area with warm water for five minutes, and gently file down any thick skin with a pumice stone or emery board. |
| Apply salicylic acid product to the wart. |
| Repeat the first two steps daily with liquid or gel preparations, or every other day with the patch. |
| Duct tape may be used to cover the wart after application of salicylic acid liquid. |
| Repeat treatment until the wart has cleared, or for a maximum of 12 weeks. |
| Discontinue treatment if severe redness, pain, or itching occurs in the treated area; mild redness is common. |
| Do not use salicylic acid on the face. |
Cryotherapy (Likely to Be Beneficial11)
Cryotherapy is commonly used in physician offices for treatment of warts and is also available over the counter. Liquid nitrogen is generally used by primary care physicians, and it can freeze the tissue to a temperature of −321°F (−196°C); over-the-counter cryotherapy products freeze the tissue to −94°F (−70°C). Liquid nitrogen can be applied using a cryogun or a cotton swab. A video demonstrating cryotherapy using liquid nitrogen is available at http://www.youtube.com/watch?v=QcbASzrn4ao. Because HPV can survive in liquid nitrogen, cotton swabs and liquid nitrogen should be properly discarded and cryoguns disinfected to avoid spreading the virus to other patients or contaminating the liquid nitrogen reservoirs.14
Most trials comparing cryotherapy with salicylic acid found no difference in effectiveness, with overall cure rates of 50 to 70 percent after three or four treatments.2 However, cryotherapy requires fewer applications than salicylic acid. Usually, liquid nitrogen is applied until a 2-mm white halo forms around the wart.1 Aggressive cryotherapy (10 to 30 seconds) is more effective than less aggressive cryotherapy (52 versus 31 percent clearance rate; number needed to treat = 5; 95% confidence interval, 3 to 15).2,7,11,15 However, aggressive cryotherapy can increase pain and blistering by 45 percent (number needed to harm = 5).2
RCTs show that decreasing the interval between treatments to less than two or three weeks increases reported pain without improvement in wart resolution.2,7,16 Low-quality evidence suggests that paring plantar warts before treatment may be beneficial.17 Two freeze-thaw cycles may improve clearance of plantar warts, but not hand warts.1,17 Cryotherapy should not be continued beyond three months, or a total of four treatments, because no benefit has been documented beyond this point, especially for warts on hands and feet.18
Common adverse effects of cryotherapy include pain; blistering; hypo- or hyperpigmentation, particularly in dark skin; tendon or nerve damage with aggressive therapy; and onychodystrophy following treatment of periungual warts.19 A standardized approach may improve treatment success (Table 4).
Table 4. Suggested Approach for Cryotherapy with Liquid Nitrogen for Treatment of Nongenital Cutaneous Warts

| Pare down dead skin with a sharp blade, especially if treating plantar warts. |
| Apply liquid nitrogen using a cryogun or cotton swab until the wart has a 2-mm white halo for about 10 seconds (five seconds for small warts, 20 seconds for plantar warts). |
| When treating plantar warts, repeat the second step once more after the white halo completely disappears (freeze-thaw-freeze technique). |
| Consider adding salicylic acid between treatments. |
| Cotton swabs and liquid nitrogen should be discarded and cryoguns disinfected after each treatment to avoid spreading the virus. |
| Tell the patient to expect some pain and blistering in the treated area. |
| Repeat every two or three weeks, up to three months or four treatments. |
note: For another approach, go to http://www.youtube.com/watch?v=QcbASzrn4ao.
Candida and Mumps Skin Antigens (Likely to Be Beneficial)
Candida and mumps skin antigens are routinely used to assess a patient's cellular immune system via intradermal injection.20 These products are readily available from medical supply companies. Intralesional injections of the antigens induce a localized, cell-mediated and HPV-specific response that may target the injected wart as well as more distant warts. A single-blinded RCT of 201 patients with recalcitrant warts compared mumps, Candida, or Trichophyton skin antigens alone or plus intralesional interferon alfa with interferon alfa alone or placebo.21 Cure rates were 60 percent in the antigen groups compared with 24 percent in the interferon-only and placebo groups. Complete clearance of warts was reported in 22 percent of patients in the antigen groups compared with 10 percent in the placebo groups.2 Skin antigen treatment is usually well tolerated. Pruritus is the most common adverse effect, although pain, burning, or peeling may also occur. Two cases of pain, edema, and purple discoloration in the distal fingertip developing within 24 hours of Candida skin antigen injection into a subungual wart have been reported. Both cases resolved without sequelae.20 Pretesting patients before treatment should be considered because this modality works only in patients with an immune response to the antigen. Table 5 presents the suggested protocol for intralesional injection of Candida or mumps skin antigens.
Table 5. Suggested Approach for Intralesional Candida or Mumps Skin Antigen for Treatment of Recalcitrant Nongenital Cutaneous Warts

| Use commercial Candida or mumps skin antigen test preparations. |
| Consider pretesting patient with intradermal injection (0.1 mL) in the forearm; continue to third step if antigen response occurs. |
| Administer 0.1- to 0.3-mL injection into the largest wart or split between two warts; maximum amount is 0.3 mL per treatment. |
| Tell patient to expect itching in the area; burning or peeling is possible. |
| May repeat injection every three to four weeks, up to three treatments. |
Photodynamic Therapy with Aminolevulinic Acid (Likely to Be Beneficial11)
Treatment with aminolevulinic acid (Levulan Kerastick) followed by phototoxicity is the mainstay of photodynamic therapy. Aminolevulinic acid is a photosensitizer that acts by inducing photooxidation in the abnormal cells following irradiation with visible light.9 Aminolevulinic acid is usually applied to the wart for three to eight hours, after which the area is exposed to a range of light sources.22 Photodynamic therapy is used to treat many skin diseases, including actinic keratosis, basal cell carcinoma, intraepithelial lesions of the vulva and anus, and genital warts. Two high-quality RCTs including 45 and 67 patients, respectively, with recalcitrant cutaneous warts reported cure rates of 56 to 75 percent with phototherapy plus aminolevulinic acid versus 23 to 42 percent with placebo phototherapy after four months.2 In these RCTs, all warts were treated with a keratolytic agent before phototherapy, and recent guidelines correlate adequate paring with improved phototherapy outcomes.22 Universally reported adverse effects include burning and itching; however, in one trial, 17 percent of patients had severe pain.23 Although photodynamic therapy is likely to be beneficial, it is expensive, is not as readily available to family physicians as other treatments, and is usually administered by dermatologists.
Duct Tape (Unknown Effectiveness11)
Duct tape is a popular remedy for nongenital cutaneous warts, but there is little documented evidence of its effectiveness. One flawed RCT including 61 patients showed positive response to application of duct tape compared with cryotherapy.24 However, two more recent trials showed no effectiveness of duct tape compared with placebo,25,26 although these trials used clear duct tape without rubber instead of the silver-gray duct tape used in the original trial. Because there is insufficient evidence to support the use of duct tape as monotherapy for warts, some experts advise applying it as an adjunct therapy to salicylic acid.
Intralesional Bleomycin (Unknown Effectiveness11)
Bleomycin is a chemotherapeutic agent that inhibits DNA synthesis in cells and viruses.9 It causes acute tissue necrosis that may stimulate an immune response.10 There is no consistent evidence regarding the effectiveness of bleomycin for nongenital cutaneous warts. In five RCTs, cure rates ranged from 16 to 94 percent; one trial even showed higher cure rates in the placebo group.2,7 Adverse effects of bleomycin include pain, swelling, and redness for one week after treatment. Necrosis in the skin may cause scarring, pigment change, or nail damage. Because treatment can lead to significant systemic drug exposure, bleomycin should be avoided in children, pregnant women, and patients with peripheral vascular disease or Raynaud disease.27 Patients are usually referred to a dermatologist for this treatment.
Pulsed Dye Laser (Unknown Effectiveness11)
Pulsed dye laser selectively destroys the dilated capillaries of a wart. One small RCT of 37 patients found no notable difference in wart clearance between pulsed dye laser and placebo at 14 weeks.11 Another trial comparing pulsed dye laser with cryotherapy or cantharidin found no statistically significant difference in cure rates among the three groups.28 Uncontrolled studies have suggested clearance rates between 70 and 90 percent with pulsed dye laser.1 Overall, it appears that plantar warts respond the least to this treatment.28,29 Pulsed dye laser is well tolerated but requires expensive equipment and is usually available only at dermatology offices.
Intralesional Interferon Alfa (Unknown Effectiveness2)
Interferon alfa is a low-molecular-weight glycoprotein produced by cell types that inhibit viral replication and tumor growth. Pooled data from three trials evaluating the effectiveness of interferon alfa for the treatment of cutaneous warts showed no statistically significant advantage over placebo (relative risk = 0.87).2
Imiquimod (Unknown Effectiveness)
Imiquimod (Aldara) is an established therapy for genital and perianal warts. However, no published RCT has evaluated its use for cutaneous warts. Small nonrandomized trials evaluating topical imiquimod 5% for the treatment of recalcitrant warts reported 30 to 80 percent clearance rates.9,30,31 Adverse effects include redness, itching, edema, and erosion.
Surgical Removal by Curettage or Cautery (Unknown Effectiveness11)
Although curettage or cautery is used to remove warts, no RCT has been published. Success rates are reported to be between 65 and 85 percent, but scarring and recurrence occur in up to 30 percent of patients.32–34 Scarring can be particularly problematic on the sole of the foot.
Other Treatments
Many other treatment modalities have been investigated for cutaneous warts, some showing promising effectiveness in small trials (e.g., silver nitrate solution, topical fluorouracil, topical zinc).35–37 Other treatments, such as cantharidin and dinitrochlorobenzene, have little evidence supporting their effectiveness. In addition, oral cimetidine (Tagamet), oral zinc sulfate, podophyllin, propolis ointment, retinoids, and topical garlic extract have poor or inconsistent evidence of their effectiveness and may not differ from placebo.

