Disability and mobility problems increase with age. Assistive devices such as canes, crutches, and walkers can be used to increase a patient's base of support, improve balance, and increase activity and independence, but they are not without significant musculoskeletal and metabolic demands. Most patients with assistive devices have never been instructed on the proper use and often have devices that are inappropriate, damaged, or are of the incorrect height. Selection of a suitable device depends on the patient's strength, endurance, balance, cognitive function, and environmental demands. Canes can help redistribute weight from a lower extremity that is weak or painful, improve stability by increasing the base of support, and provide tactile information about the ground to improve balance. Crutches are useful for patients who need to use their arms for weight bearing and propulsion and not just for balance. Walkers improve stability in those with lower extremity weakness or poor balance and facilitate improved mobility by increasing the patient's base of support and supporting the patient's weight. Walkers require greater attentional demands than canes and make using stairs difficult. The top of a cane or walker should be the same height as the wrist crease when the patient is standing upright with arms relaxed at his or her sides. A cane should be held contralateral to a weak or painful lower extremity and advanced simultaneously with the contralateral leg. Clinicians should routinely evaluate their patients' assistive devices to ensure proper height, fit, and maintenance, and also counsel patients on correct use of the device.
Currently, an estimated 6.1 million community-dwelling adults use mobility devices, including canes, walkers, and crutches, and two-thirds of those persons are older than 65 years.1 With the growing number of older adults in the community and the increasing number of those adults with multiple chronic conditions, disability and the resultant mobility problems are anticipated to become even more widespread.2 Of adults older than 65 years, 10 percent use canes and 4.6 percent use walkers.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Assistive devices can be prescribed to improve balance, reduce pain, and increase mobility and confidence. | C | 3, 4 |
| Because most patients obtain their assistive device without recommendations or instructions from a medical professional, assistive devices should be evaluated routinely for proper fit and use. | C | 7, 9 |
| When only one upper extremity is needed for balance or weight bearing, a cane is preferred. If both upper extremities are needed, crutches or a walker is more appropriate. | C | 10 |
| The correct height of a cane or walker is at the level of the patient's wrist crease, as measured with the patient standing upright with arms relaxed at his or her sides. When holding the device at this height, the patient's elbow is naturally flexed at a 15- to 30-degree angle. | C | 13 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Assistive Devices
Assistive devices can be prescribed to broaden a patient's base of support, improve balance and stability, or redistribute weight from the lower limbs to help alleviate joint pain or compensate for weakness or injury. The goals of assistive device use are to improve independent mobility, reduce disability, delay functional decline, and decrease the burden of care.3,4 Patients using assistive devices have reported improved confidence and feelings of safety, resulting in increased activity levels and independence. There also may be physiologic benefits of assistive device use, including improved cardiorespiratory function, enhanced circulation, and prevention of osteoporosis.3 However, there are insufficient high-quality studies evaluating the impact of specific assistive devices on mobility outcomes and fall prevention.1,5
Assistive devices are not without considerable attentional, neuromotor, and musculoskeletal demands, and even have been associated with falls and injury.3,4,6 Although use of an assistive device may just be a marker of muscle weakness or balance impairment, the assistive device itself may directly increase fall risk. The act of lifting and advancing the device can result in the destabilization of biomechanical forces, and balance may be disrupted by the need to allocate attention to device control.3 Moreover, the device may interfere with limb movements during balance recovery.7 Repetitive stress on upper extremity joints from assistive device use can also cause tendinopathy, osteoarthritis, and carpal tunnel syndrome.3
Most persons are not instructed on the proper use of their cane, and up to 70 percent of canes are faulty, damaged, or the wrong height.1,8 Studies have shown that most patients obtained their assistive device on their own or on the advice of family or friends.7,9 Only about one-third of patients obtained their device through a medical professional, and only 20 percent received education on how to use it.7,9 Problems identified on assessment of assistive devices were that more than one-half were the incorrect height (too high), poor maintenance (including loose rubber caps or hand grips), and poor posture or use (including an incorrect gait pattern, or holding the device on the wrong side).7,9 As a result of the demands of assistive device use and inadequate training, 30 to 50 percent of patients stop using their assistive device soon after receiving it.3 Selection of the appropriate device and education from a medical professional are important to effectively increase mobility and reduce disability.
Canes
Canes can help redistribute weight from a weak or painful lower extremity, improve stability by increasing the base of support, and provide tactile information about the ground to improve balance.1 Canes also have been associated with improved self-reported functional ability and confidence.8 Although several types of canes are available, there is little evidence supporting the use of one type of cane over another.
STANDARD CANES
A standard cane (Figure 1) or straight cane is generally made from wood or aluminum and is inexpensive and lightweight. An aluminum cane has the advantage of an adjustable height. A standard cane can help with balance in a patient who does not need the upper extremity to bear weight.10
Figure 1.
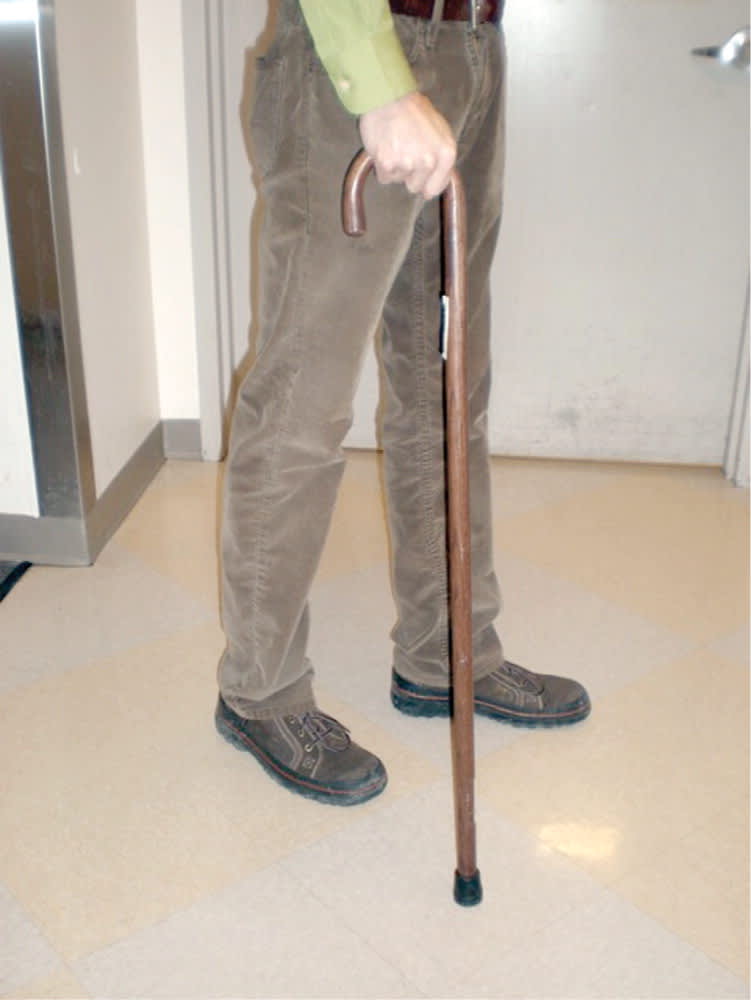
Standard cane.
OFFSET CANES
An offset cane (Figure 2) distributes the patient's weight over the shaft of the cane. An offset cane is appropriate for patients who need the upper extremity to occasionally bear weight, such as those with gait problems caused by pain from knee or hip osteoarthritis.10
Figure 2.
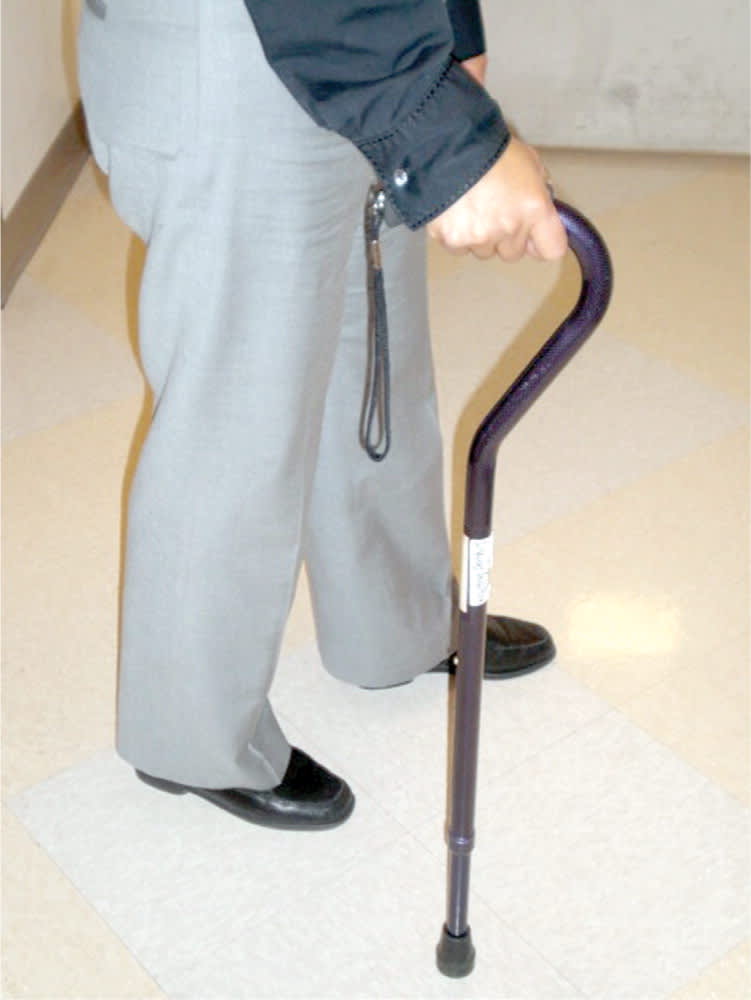
Offset cane. The curved handle helps distribute weight over the cane.
QUADRIPOD CANES
A quadripod cane (Figure 3), commonly referred to as a quad cane, is a four-legged cane that provides a larger base of support extremity. It also can stand freely on its own if the patient needs to use his or her hands, and it can be particularly useful for patients with hemiplegia.11 However, all four points of the cane must be in contact with the ground at the same time for proper use.10
Figure 3.
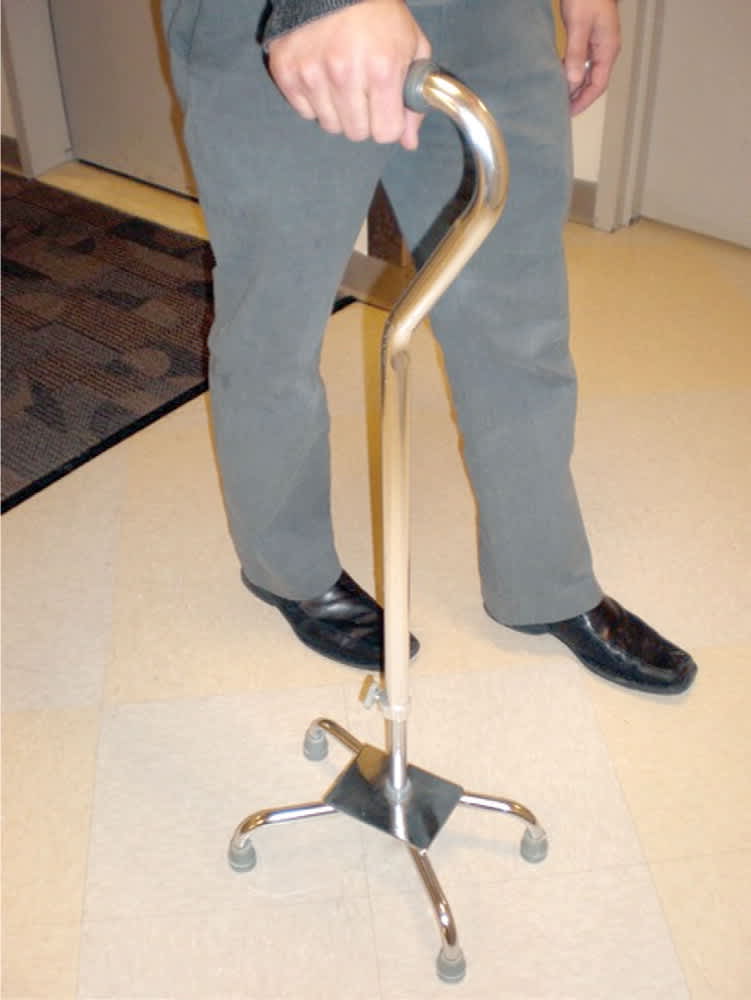
Quadripod cane. These canes have four legs for increased stability.
HANDLES
A standard cane typically has an umbrella handle, which may increase the risk of carpal tunnel syndrome because of pressure on the palm of the hand. A shotgun handle, referred to as such because of its similarity to the butt of a shotgun, is a flat handle more commonly used with offset canes. The shotgun handle distributes pressure across the entire hand from the thenar to hypothenar muscles with less pressure on the palm, decreasing the risk of carpal tunnel syndrome. Special handles with finger and thumb grooves are also available and may prompt patients to use the cane in the correct hand.
Crutches
Crutches are helpful for patients who need to use their arms for weight bearing and propulsion and not just for balance.1 One crutch can provide 80 percent weight-bearing support, and two crutches provide 100 percent weight-bearing support.4 However, crutches require substantial energy expenditure and arm and shoulder strength, making them generally inappropriate for frail older adults.4
AXILLARY CRUTCHES
Axillary crutches (Figure 4) are inexpensive and provide weight-bearing ambulation, but they can be cumbersome and difficult to use.4 If the crutch is incorrectly fit, it can cause nerve compression or axillary artery compression.4
Figure 4.
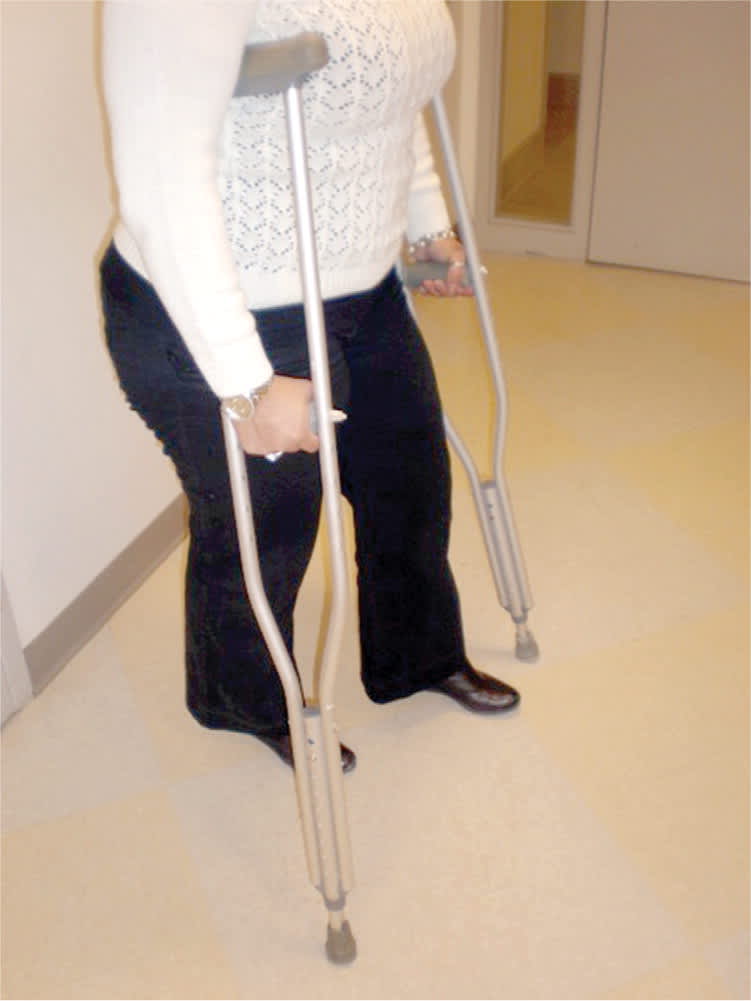
Axillary crutches. The height of the crutches leaves ample space between the crutch and axilla.
FOREARM (LOFSTRAND) CRUTCHES
Forearm crutches (Figure 5) have a cuff around the proximal forearm and distal hand grips, allowing bilateral upper extremity support with occasional weight bearing. This allows the patient's hands to be free without needing to drop the crutch, making it less awkward to use, particularly on stairs.4
Figure 5.
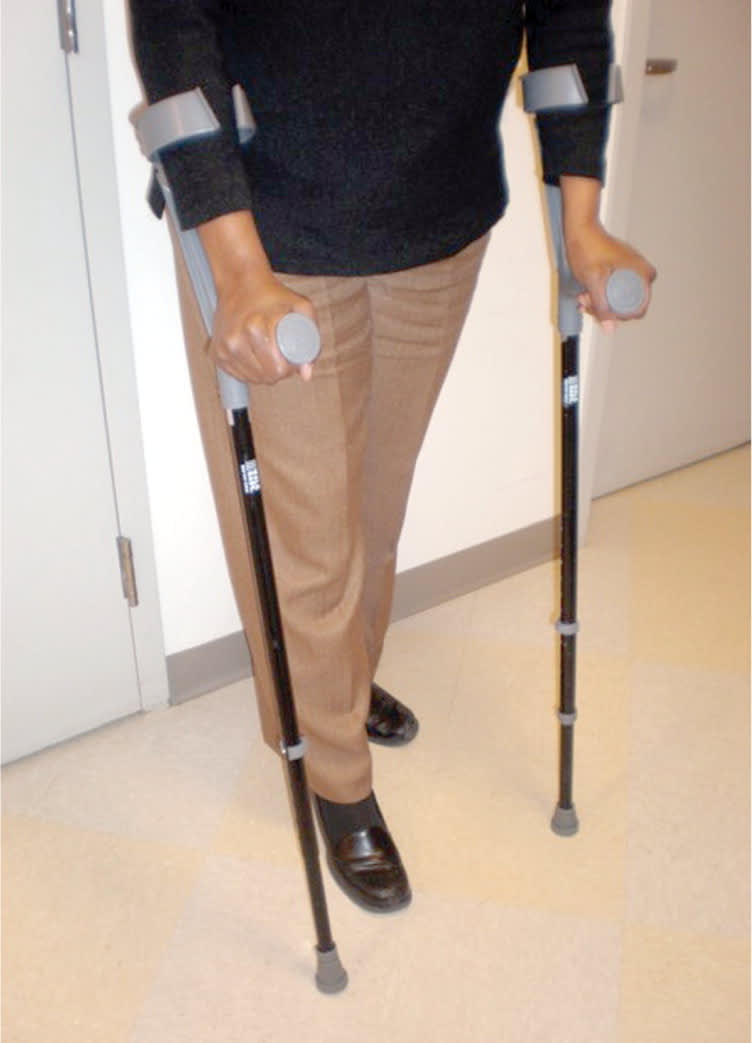
Forearm crutches. These are easier to use on stairs than other types of crutches.
PLATFORM CRUTCHES
Platform crutches provide a horizontal platform for the entire forearm, which is used to bear weight rather than the hand. They can be useful for patients with elbow contractures or with weak or painful hands or wrists.4
Walkers
Walkers improve stability in patients with lower extremity weakness or poor balance, and they facilitate improved mobility by increasing the patient's base of support and supporting the patient's weight.1,4,7 However, walkers can be difficult to maneuver and can result in poor back posture and reduced arm swing.4 Walkers require greater attentional demands than canes, and it is difficult to navigate stairs when using a walker.4
STANDARD WALKERS
A standard walker (Figure 6) is the most stable walker, but it results in a slower gait because the patient must completely lift the walker off the ground with each step.4 This may be useful for patients with cerebellar ataxia, but it may be challenging for frail older patients with decreased upper body strength.6
Figure 6.
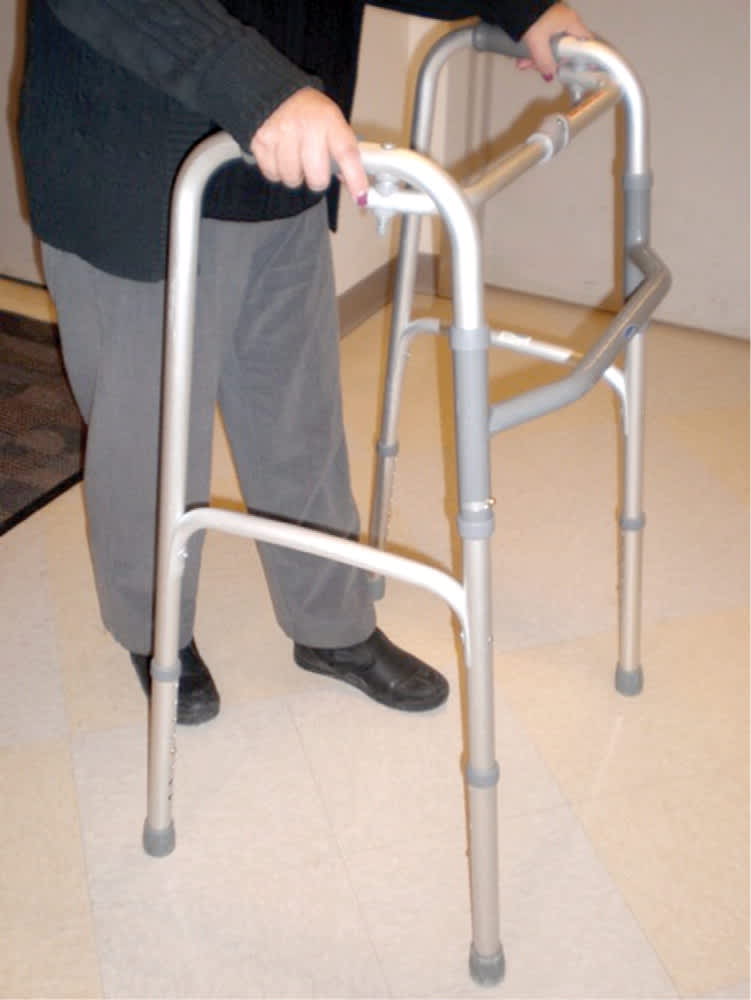
Standard walker. These walkers require lifting when propelling forward.
FRONT-WHEELED WALKERS
A front-wheeled walker (Figure 7), also called a two-wheeled walker, is less stable than a standard walker, but maintains a more normal gait pattern and is better for those who are unable to lift a standard walker.4 In patients with parkinsonism, front-wheeled walkers may reduce freezing compared with standard walkers.12
Figure 7.
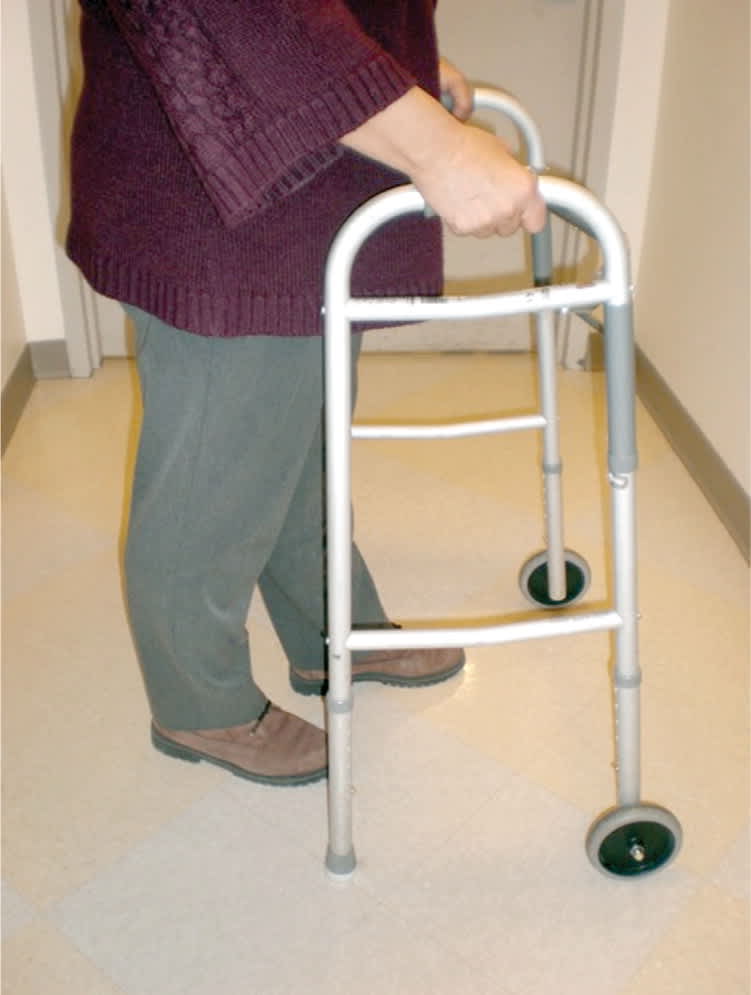
Front-wheeled walker.
FOUR-WHEELED WALKERS
A four-wheeled walker (Figure 8), commonly called a rollator, is useful for higher functioning patients who do not need the walker to bear weight. Although the four-wheeled walker is easier to propel, it is not appropriate for patients with significant balance problems or cognitive impairment because it can roll forward unexpectedly and result in a fall.1,4 Rollators often come with seats and baskets, making them a popular option, but they must be used with caution. The brakes should always be on and the rollator should be against a wall or other solid object before the patient sits. This device can be particularly useful for those with claudication, respiratory disease, or congestive heart failure who often need to stop ambulating and sit down to rest.
Figure 8.
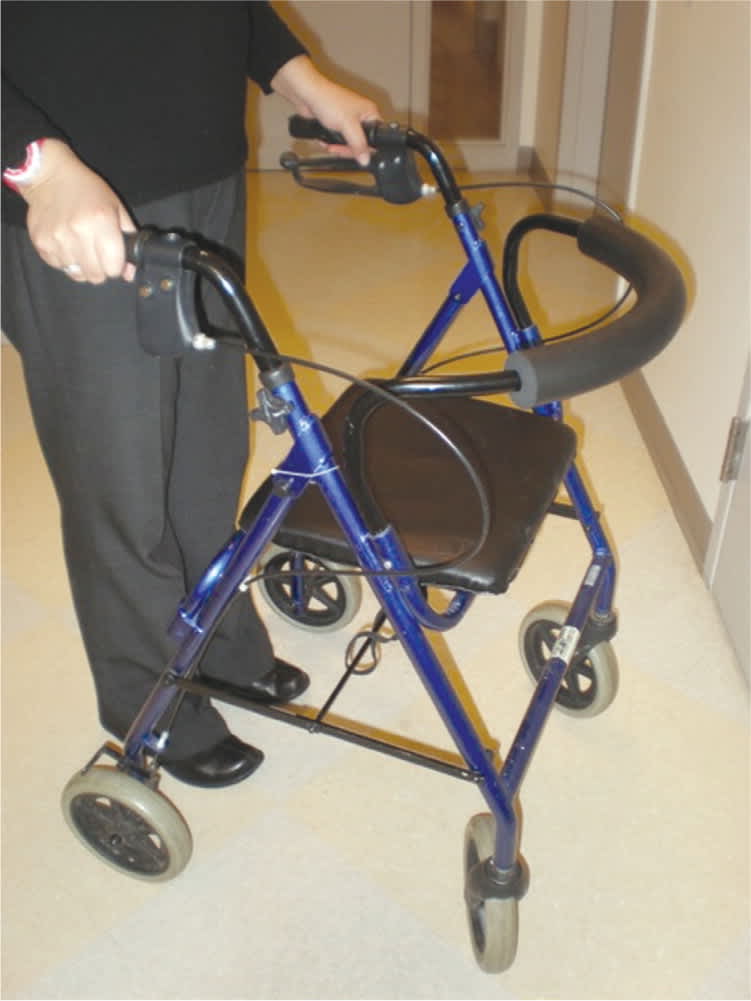
Four-wheeled walker. Although these walkers are easier to use than other types of walkers, they can roll forward unexpectedly and may increase fall risk.
Selecting the Appropriate Device
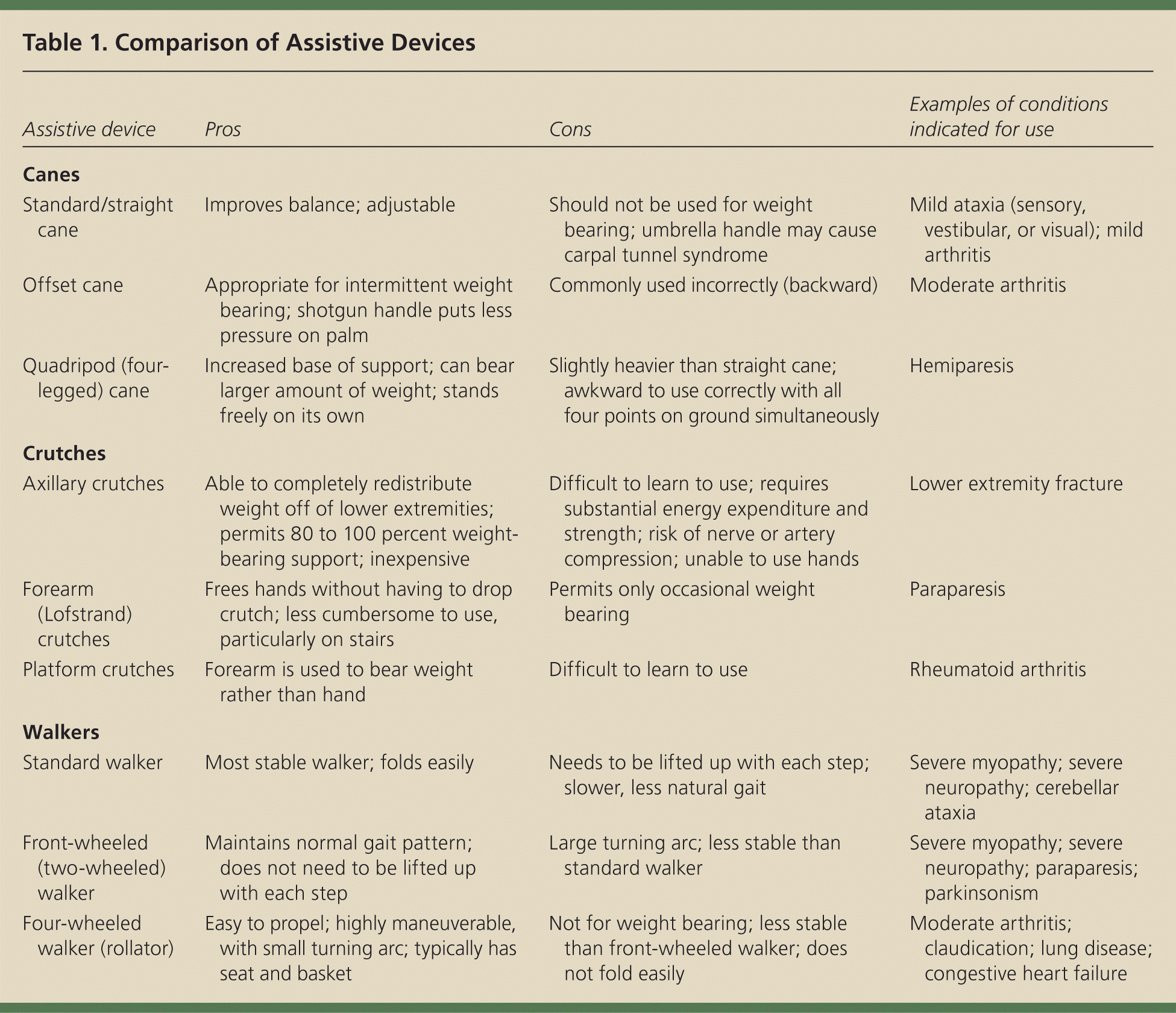
Table 1 highlights the pros and cons of the various devices and lists examples of medical conditions in which each device may be appropriate. Selection of an appropriate device depends on the patient's strength, endurance, vestibular function, cognitive function, vision, and environmental demands.1,4 Figure 9 provides an algorithm for assistive device selection, which is determined by whether the patient needs to use one or both upper extremities to maintain balance or bear weight, and the frequency of this need.10 If the patient requires constant weight bearing, a standard walker may be better because it is more stable. If the patient needs weight-bearing assistance, but not constantly, a front-wheeled walker may suffice. It is important to keep in mind that for some patients who can no longer walk safely or who have severe lower extremity weakness, a wheelchair may be the best option.1
Table 1. Comparison of Assistive Devices
| Assistive device | Pros | Cons | Examples of conditions indicated for use |
|---|---|---|---|
| Canes | |||
| Standard/straight cane | Improves balance; adjustable | Should not be used for weight bearing; umbrella handle may cause carpal tunnel syndrome | Mild ataxia (sensory, vestibular, or visual); mild arthritis |
| Offset cane | Appropriate for intermittent weight bearing; shotgun handle puts less pressure on palm | Commonly used incorrectly (backward) | Moderate arthritis |
| Quadripod (four-legged) cane | Increased base of support; can bear larger amount of weight; stands freely on its own | Slightly heavier than straight cane; awkward to use correctly with all four points on ground simultaneously | Hemiparesis |
| Crutches | |||
| Axillary crutches | Able to completely redistribute weight off of lower extremities; permits 80 to 100 percent weight-bearing support; inexpensive | Difficult to learn to use; requires substantial energy expenditure and strength; risk of nerve or artery compression; unable to use hands | Lower extremity fracture |
| Forearm (Lofstrand) crutches | Frees hands without having to drop crutch; less cumbersome to use, particularly on stairs | Permits only occasional weight bearing | Paraparesis |
| Platform crutches | Forearm is used to bear weight rather than hand | Difficult to learn to use | Rheumatoid arthritis |
| Walkers | |||
| Standard walker | Most stable walker; folds easily | Needs to be lifted up with each step; slower, less natural gait | Severe myopathy; severe neuropathy; cerebellar ataxia |
| Front-wheeled (two-wheeled) walker | Maintains normal gait pattern; does not need to be lifted up with each step | Large turning arc; less stable than standard walker | Severe myopathy; severe neuropathy; paraparesis; parkinsonism |
| Four-wheeled walker (rollator) | Easy to propel; highly maneuverable, with small turning arc; typically has seat and basket | Not for weight bearing; less stable than front-wheeled walker; does not fold easily | Moderate arthritis; claudication; lung disease; congestive heart failure |
Figure 9. Geriatric Assistive Device Selection
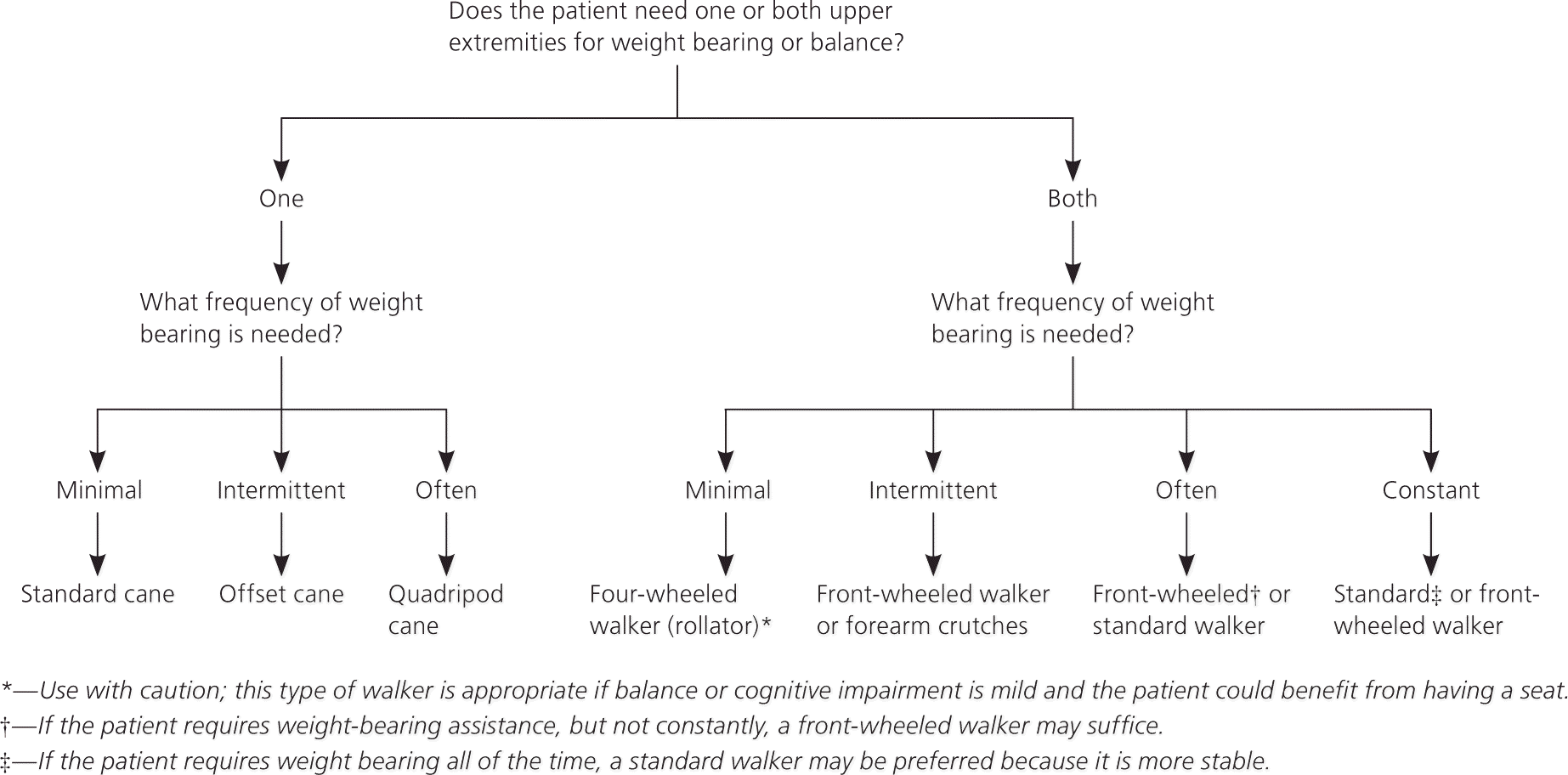
Algorithm for assistive device selection.
Instruction to Patients
CORRECT HEIGHT AND FIT
The correct height of a cane or walker is at the level of the patient's wrist crease, which is measured with the patient standing upright with arms relaxed at his or her sides. When holding the device at this height, the patient's elbow is naturally flexed at a 15- to 30-degree angle.13 The correct height for axillary crutches should be the distance from 1.6 to 2 inches (4 to 5 cm) below the axilla to the floor, 2 inches lateral and 5.9 inches (15 cm) anterior to the foot. The handle position should be where the elbow is in 30 degrees of flexion.4 Forearm crutches are also used with the elbow flexed 15 to 30 degrees, and the forearm cuff should be 1 to 1.6 inches (2.5 to 4 cm) below the olecranon when the distal end of the crutch is placed 2 inches lateral and 6 inches (15.2 cm) anterior to the foot.4 For platform crutches, the proper height is determined by having the patient stand with the elbow flexed at 90 degrees and measuring the length from the forearm to the ground.4
PROPER USE
A cane should be held contralateral to a weak or painful lower extremity and advanced simultaneously with the contralateral leg. When using a walker, both feet should stay between the posterior legs or wheels. With a cane or walker, posture should be upright without forward or lateral leaning. Patients should take their time when turning and should not lift the device off the ground while doing so.7 When navigating stairs, patients with a unilateral lower extremity impairment should advance the unimpaired extremity first when going up stairs and advance the impaired extremity first when going down stairs. One way for patients to remember this is the phrase, “Up with the good and down with the bad.” A video about how to use a cane is available online at http://www.youtube.com/watch?v=fRn8ZZJMzno.
MONITORING
All patients should be observed using their device. Medical professionals should routinely assess whether the device is appropriate and evaluate cane and walker maintenance, including checking proper height and condition of legs, wheels, tips, and hand grips.7 Patients who have gait or balance disorders, a new disability, or difficulty using their assistive device can benefit from a referral to a physical therapist.1
Data Sources: A PubMed search was completed in Clinical Queries using the following key terms: assistive devices, canes, crutches, and walkers. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, Bandolier, Clinical Evidence, the Cochrane database, Database of Abstracts of Reviews of Effects, the Institute for Clinical Systems Improvement, the National Guideline Clearinghouse database, and UpToDate. Search date: December 10, 2010.

