Guideline source: American Academy of Otolaryngology–Head and Neck Surgery
Evidence rating system used? Yes
Literature search described? Yes
Published source: Otolaryngology–Head and Neck Surgery, January 2011
Available at: http://oto.sagepub.com/content/144/1_suppl/S1.long
Endorsed with qualifications by the AAFP, January 2013. https://www.aafp.org/patient-care/clinical-recommendations/all/endorsed.html
More than 530,000 tonsillectomies are performed in children and adolescents in the United States every year because of recurrent throat infections or sleep-disordered breathing. Although tonsillectomy is common and improves patients' quality of life, there are possible risks and practice variations in the care of patients undergoing tonsillectomy.
Recent guidelines from the American Academy of Otolaryngology–Head and Neck Surgery (AAO–HNS) aim to provide physicians with evidence-based guidance on identifying patients one to 18 years of age who would most benefit from the procedure. Table 1 summarizes the Paradise criteria for tonsillectomy used in this guideline, and Table 2 compares AAO–HNS, Italian, and Scottish guidelines.
Table 1. Paradise Criteria for Tonsillectomy

| Criterion | Definition | |
|---|---|---|
| Minimum frequency of sore throat episodes | At least seven episodes in the previous year, at least five episodes in each of the previous two years, or at least three episodes in each of the previous three years | |
| Clinical features | Sore throat plus at least one of the following features qualifies as a counting episode: | |
| Temperature of greater than 100.9°F (38.3°C) | ||
| Cervical adenopathy (tender lymph nodes or lymph node size greater than 2 cm) | ||
| Tonsillar exudate | ||
| Culture positive for group A β-hemolytic streptococcus | ||
| Treatment | Antibiotics administered in the conventional dosage for proved or suspected streptococcal episodes | |
| Documentation | Each episode of throat infection and its qualifying features substantiated by contemporaneous notation in a medical record | |
| If the episodes are not fully documented, subsequent observance by the physician of two episodes of throat infection with patterns of frequency and clinical features consistent with the initial history* | ||
*—Allows for tonsillectomy in patients who meet all but the documentation criterion. A 12-month observation period is usually recommended before consideration of tonsillectomy.
Adapted with permission from Baugh RF, Archer SM, Mitchell RB, et al.; American Academy of Otolaryngology–Head and Neck Surgery Foundation. Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg. 2011;144(1 suppl):S8.
Table 2. Comparison of American, Italian, and Scottish Guidelines for Tonsillectomy in Children and Adolescents
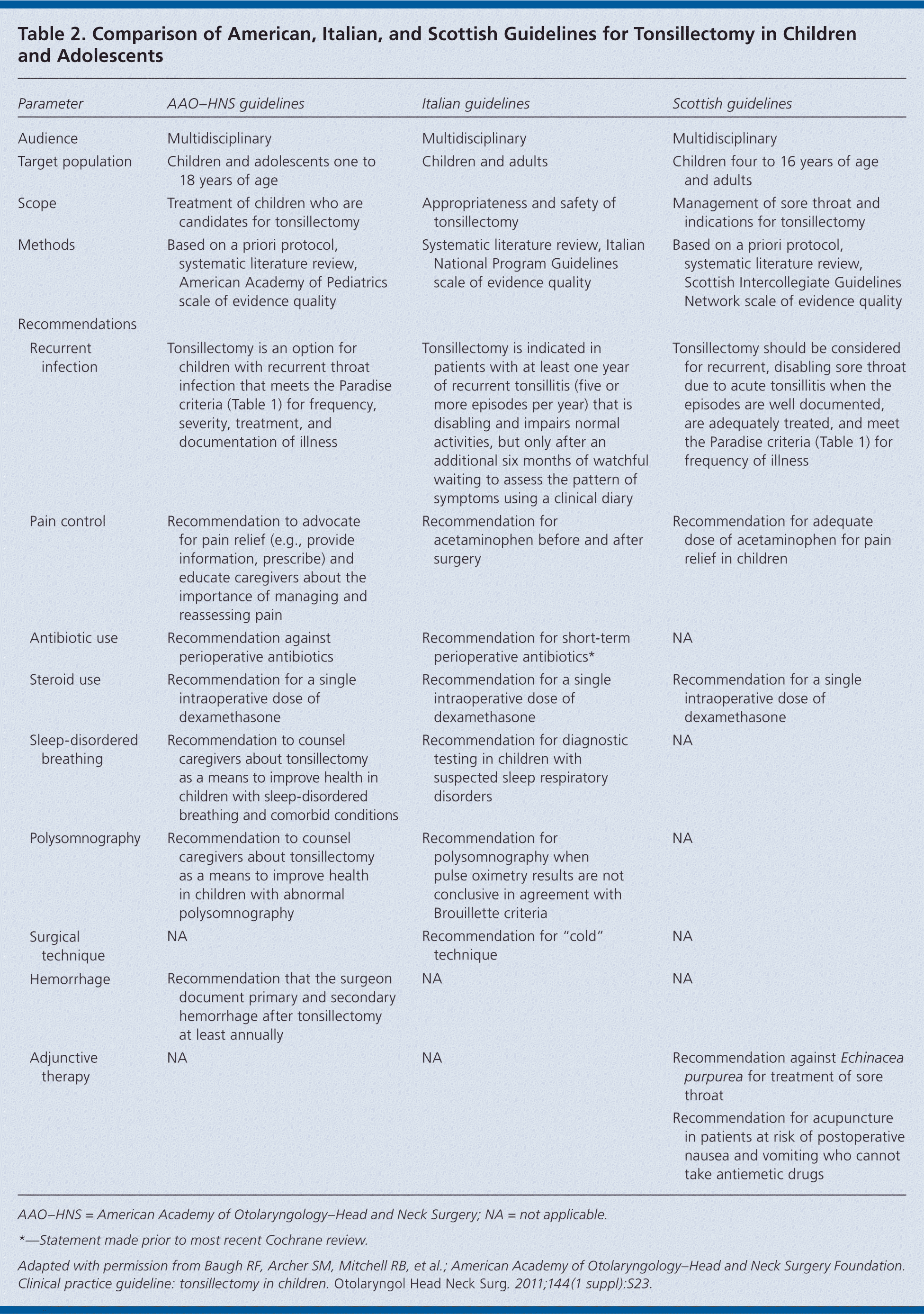
| Parameter | AAO–HNS guidelines | Italian guidelines | Scottish guidelines | |
|---|---|---|---|---|
| Audience | Multidisciplinary | Multidisciplinary | Multidisciplinary | |
| Target population | Children and adolescents one to 18 years of age | Children and adults | Children four to 16 years of age and adults | |
| Scope | Treatment of children who are candidates for tonsillectomy | Appropriateness and safety of tonsillectomy | Management of sore throat and indications for tonsillectomy | |
| Methods | Based on a priori protocol, systematic literature review, American Academy of Pediatrics scale of evidence quality | Systematic literature review, Italian National Program Guidelines scale of evidence quality | Based on a priori protocol, systematic literature review, Scottish Intercollegiate Guidelines Network scale of evidence quality | |
| Recommendations | ||||
| Recurrent infection | Tonsillectomy is an option for children with recurrent throat infection that meets the Paradise criteria (Table 1) for frequency, severity, treatment, and documentation of illness | Tonsillectomy is indicated in patients with at least one year of recurrent tonsillitis (five or more episodes per year) that is disabling and impairs normal activities, but only after an additional six months of watchful waiting to assess the pattern of symptoms using a clinical diary | Tonsillectomy should be considered for recurrent, disabling sore throat due to acute tonsillitis when the episodes are well documented, are adequately treated, and meet the Paradise criteria (Table 1) for frequency of illness | |
| Pain control | Recommendation to advocate for pain relief (e.g., provide information, prescribe) and educate caregivers about the importance of managing and reassessing pain | Recommendation for acetaminophen before and after surgery | Recommendation for adequate dose of acetaminophen for pain relief in children | |
| Antibiotic use | Recommendation against perioperative antibiotics | Recommendation for short-term perioperative antibiotics* | NA | |
| Steroid use | Recommendation for a single intraoperative dose of dexamethasone | Recommendation for a single intraoperative dose of dexamethasone | Recommendation for a single intraoperative dose of dexamethasone | |
| Sleep-disordered breathing | Recommendation to counsel caregivers about tonsillectomy as a means to improve health in children with sleep-disordered breathing and comorbid conditions | Recommendation for diagnostic testing in children with suspected sleep respiratory disorders | NA | |
| Polysomnography | Recommendation to counsel caregivers about tonsillectomy as a means to improve health in children with abnormal polysomnography | Recommendation for polysomnography when pulse oximetry results are not conclusive in agreement with Brouillette criteria | NA | |
| Surgical technique | NA | Recommendation for “cold” technique | NA | |
| Hemorrhage | Recommendation that the surgeon document primary and secondary hemorrhage after tonsillectomy at least annually | NA | NA | |
| Adjunctive therapy | NA | NA | Recommendation against Echinacea purpurea for treatment of sore throat | |
| Recommendation for acupuncture in patients at risk of postoperative nausea and vomiting who cannot take antiemetic drugs | ||||
AAO–HNS = American Academy of Otolaryngology–Head and Neck Surgery; NA = not applicable.
*—Statement made prior to most recent Cochrane review.
Adapted with permission from Baugh RF, Archer SM, Mitchell RB, et al.; American Academy of Otolaryngology–Head and Neck Surgery Foundation. Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg . 2011;144(1 suppl):S23.
Watchful Waiting for Recurrent Throat Infection
Watchful waiting is recommended for patients with recurrent throat infections if they have had fewer than seven episodes in the previous year, fewer than five episodes in each of the previous two years, or fewer than three episodes in each of the previous three years. At least 12 months of observation is recommended before considering tonsillectomy in patients without modifying factors. Observation beyond one year may be considered in patients meeting the Paradise criteria after the child's caregivers are counseled about the risks and benefits of the procedure in less severely affected children. However, prompt treatment is necessary in children with pharyngitis caused by group A β-hemolytic streptococcus.
Recurrent Throat Infection with Documentation
Documentation of recurrent throat infections should be used to help determine the need for tonsillectomy. Documentation for a throat infection includes the presence of a sore throat plus findings from a subjective physician assessment (e.g., fever, pharyngeal or tonsillar erythema, tonsil size, tonsillar exudate, cervical adenopathy, micro-biologic test results). Supportive documentation may include absences from school, spread of infection within the family, and family history of rheumatic heart disease or glomerulonephritis.
Tonsillectomy may be considered in patients with recurrent throat infections if they have had at least seven documented episodes of sore throat in the previous year, at least five documented episodes in each of the previous two years, or at least three documented episodes in each of the previous three years, plus a temperature of greater than 100.9°F (38.3°C), cervical adenopathy, tonsillar exudate, or a positive culture for group A β-hemolytic streptococcus. Evidence suggests that the most severely and frequently affected children have modest improvement with tonsillectomy; however, studies also suggest a notable improvement in quality of life. Caregivers should be advised of the harms and benefits of the procedure before a decision is made. If documentation is lacking, watchful waiting is appropriate while documentation of additional events is completed.
Tonsillectomy for Recurrent Infection with Modifying Factors
Children with recurrent throat infections who do not meet the initial criteria for tonsillectomy should be assessed for modifying factors that may make tonsillectomy favorable (e.g., those leading to risk of significant morbidity).
There are three categories of modifying risk factors. The first category includes exceptions to recognized criteria based on individual features of illness, such as multiple antibiotic allergies. The pattern of illness (e.g., throat episodes are very severe or poorly tolerated by the child) or drug allergies that make antimicrobial therapy difficult may influence the decision to perform a tonsillectomy. The second category includes specific clinical syndromes such as PFAPA (periodic fever, aphthous stomatitis, pharyngitis, and adenitis) or peritonsillar abscess. In these cases, tonsillectomy may be considered based on frequency and severity of illness and the patient's response to treatment. The last category, poorly validated clinical indications, may also influence the decision to perform tonsillectomy. The benefits of tonsillectomy for these conditions (e.g., halitosis, febrile seizures, malocclusion) must be weighed against the risks of surgery.
Tonsillectomy for Sleep-Disordered Breathing
Physicians should ask caregivers of children and adolescents with sleep-disordered breathing and tonsillar hypertrophy about comorbid conditions that could be improved with tonsillectomy. These conditions include growth retardation, poor school performance, enuresis, and behavioral problems.
Although polysomnography is often used to diagnose sleep-disordered breathing in children and adolescents, it is not always necessary. The diagnosis can be made using the history, physical examination, audiotaping or videotaping, pulse oximetry, or limited or full-night polysomnography. Tonsillar and adenoid hypertrophy are the most common causes of sleep-disordered breathing in children. Although studies support inquiring about comorbid conditions that may be improved with tonsillectomy to assist in decision making, there is a lack of randomized controlled trials supporting a recommendation for or against tonsillectomy in patients with these conditions.
Tonsillectomy and Polysomnography
Although polysomnography is not routinely needed in children with sleep-disordered breathing and tonsillar hypertrophy, some children and adolescents presenting for surgical consideration have already received poly-somnography testing. If these test results are abnormal, physicians should counsel caregivers about the benefits of tonsillectomy. Objectively documented sleep-disordered breathing and polysomnography results may warrant tonsillectomy, even without comorbid conditions. However, polysomnography results are broad, and there is no evidence-based cutoff that indicates the need for tonsillectomy.

