A 51-year-old man developed a mild fever and several serous vesicles on an erythematous base on his trunk (Figures 1 and 2) three months after having a renal transplant. During the following 10 days, similar lesions developed on his neck, upper arms, lower back, and inner thigh. The patient had the transplant because of end-stage renal disease related to interstitial nephritis. He had received a kidney from his father and was on immunosuppressive therapy.
Figure 1.
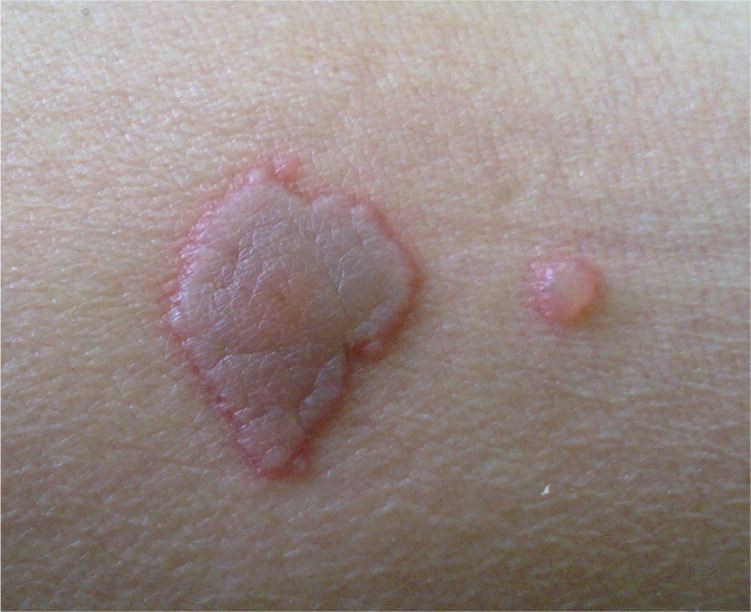
Figure 2.
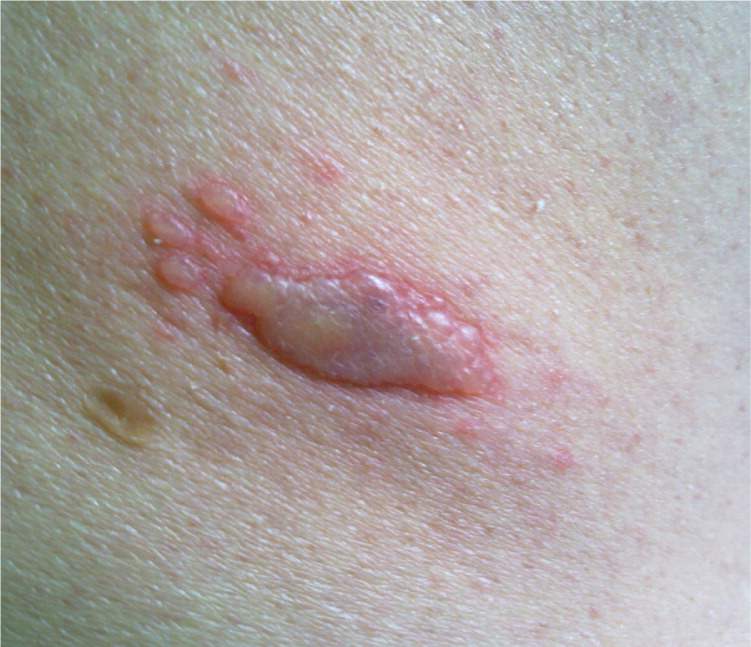
Physical examination was otherwise normal, with no evidence of secondary infection. Complete blood count, liver enzyme level, and serum creatinine level were normal. A Tzanck test from a vesicle showed giant cells and acantholytic cells.
Question
Based on the patient's history, physical examination, and laboratory results, which one of the following is the most likely diagnosis?
A. Cytomegalovirus.
B. Epstein-Barr virus.
C. Herpes simplex virus.
D. Herpes zoster.
E. Varicella-zoster virus.
Discussion
The answer is E: varicella-zoster virus infection. Patients with a primary infection typically present with fever, constitutional symptoms, and a vesicular, pruritic, widely disseminated rash that primarily involves the trunk and face.1 In patients who have had an organ transplant, symptoms usually resolve without complication. In rare cases, however, primary varicella leads to more severe disease and visceral invasion.1
Complications of varicella can be life threatening and include hepatitis, pancreatitis, pneumonitis, and encephalitis.1 Definitive laboratory testing, including polymerase chain reaction assays, direct fluorescent antibody testing on skin scrapings, viral culture, and serology, can be used for atypical cases of varicella and should be used routinely for suspected disseminated or visceral disease.1,2 Test results positive for immunoglobulin G and immunoglobulin M indicate a recent infection with varicella-zoster virus. Patients who develop primary varicella, or disseminated or organ-invasive disease following a transplant should be treated with intravenous acyclovir (Zovirax).1–3
The cutaneous manifestations of cytomegalovirus infection in organ transplant recipients are nonspecific. Cutaneous lesions may include ulcers, morbilliform rash, petechiae, purpuric eruptions, necrotic papules, and vesiculobullous eruptions.2
Epstein-Barr virus infection can cause a diffuse maculopapular and morbilliform rash. The lesions are vesicular, erythematous, and purpuric and may be accompanied by fever, pharyngitis, and lymphadenopathy.2
Organ transplant recipients with herpes simplex virus infection typically present with mucocutaneous lesions of the oropharynx. The herpetic vesicles break down to form shallow, grouped erosions and ulcers. In patients with immunosuppression, these ulcers may become large, confluent, chronic, granulating, and slow healing.1,2
Herpes zoster appears as a painful vesicular rash in a dermatomal distribution. Patients with herpes zoster who are immunocompromised may develop disseminated skin lesions that can mimic primary varicella during periods of prominent immunosuppression. All patients with previous varicella infection or vaccination are at risk of herpes zoster.2
Summary Table
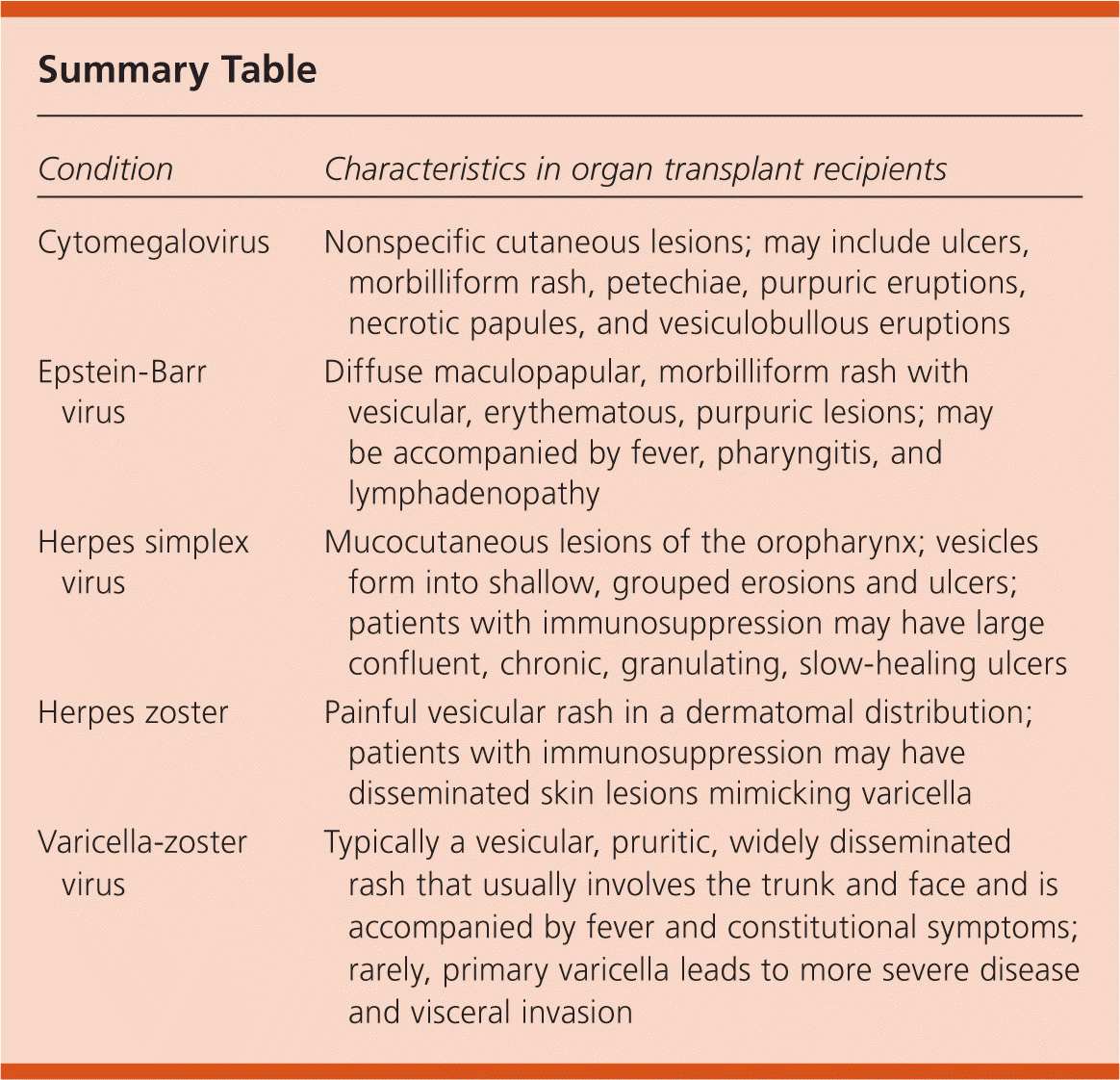
| Condition | Characteristics in organ transplant recipients |
|---|---|
| Cytomegalovirus | Nonspecific cutaneous lesions; may include ulcers, morbilliform rash, petechiae, purpuric eruptions, necrotic papules, and vesiculobullous eruptions |
| Epstein-Barr virus | Diffuse maculopapular, morbilliform rash with vesicular, erythematous, purpuric lesions; may be accompanied by fever, pharyngitis, and lymphadenopathy |
| Herpes simplex virus | Mucocutaneous lesions of the oropharynx; vesicles form into shallow, grouped erosions and ulcers; patients with immunosuppression may have large confluent, chronic, granulating, slow-healing ulcers |
| Herpes zoster | Painful vesicular rash in a dermatomal distribution; patients with immunosuppression may have disseminated skin lesions mimicking varicella |
| Varicella-zoster virus | Typically a vesicular, pruritic, widely disseminated rash that usually involves the trunk and face and is accompanied by fever and constitutional symptoms; rarely, primary varicella leads to more severe disease and visceral invasion |

